|
|
| (20 intermediate revisions by 7 users not shown) |
| Line 1: |
Line 1: |
| | __NOTOC__ |
| '''For patient information click [[Megaloblastic anemia (patient information)|here]]''' | | '''For patient information click [[Megaloblastic anemia (patient information)|here]]''' |
|
| |
|
| Line 5: |
Line 6: |
| Image = Megaloblastic anemia.jpg | | | Image = Megaloblastic anemia.jpg | |
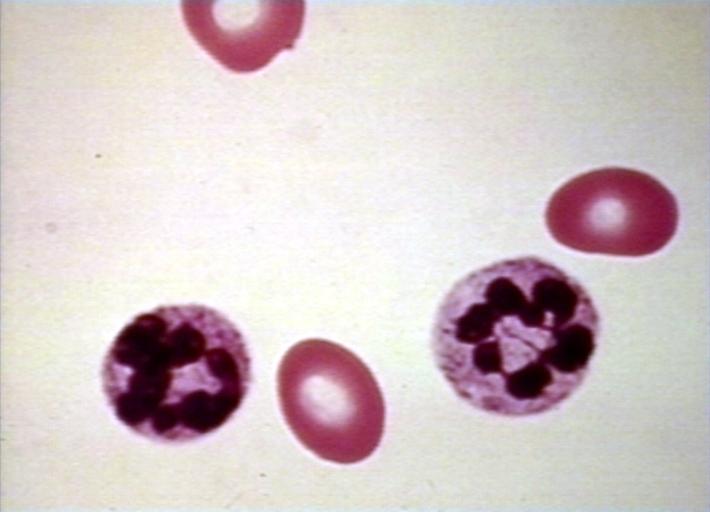
| Caption = Megaloblastic anemia blood smear | | | Caption = Megaloblastic anemia blood smear | |
| DiseasesDB = 29507 | | | DiseasesDB = | |
| ICD10 = {{ICD10|D|51|1|d|50}}, {{ICD10|D|52|0|d|50}}, {{ICD10|D|53|1|d|50}} | | | ICD10 = {{ICD10|D|51|1|d|50}}, {{ICD10|D|52|0|d|50}}, {{ICD10|D|53|1|d|50}} | |
| ICD9 = {{ICD9|281}} | | | ICD9 = {{ICD9|281}} | |
| Line 14: |
Line 15: |
| }} | | }} |
| {{Macrocytic anemia}} | | {{Macrocytic anemia}} |
| {{CMG}}; '''Associate Editor-In-Chief:''' {{CZ}} | | {{CMG}} {{shyam}}; '''Associate Editor-In-Chief:''' {{OK}}, {{ADS}}, {{CZ}} |
|
| |
|
| ==[[Macrocytic anemia overview|Overview]]== | | ==[[Macrocytic anemia overview|Overview]]== |
| Line 37: |
Line 38: |
|
| |
|
| ==Diagnosis== | | ==Diagnosis== |
| ==[[Macrocytic anemia history and symptoms|History and Symptoms]]==
| | [[Macrocytic anemia diagnostic study of choice|Diagnostic Study of Choice]] | [[Macrocytic anemia history and symptoms|History and Symptoms]] | [[Macrocytic anemia physical examination|Physical Examination]] | [[Macrocytic anemia laboratory findings|Laboratory Findings]] | [[Macrocytic anemia electrocardiogram|Electrocardiogram]] | [[Macrocytic anemia x-ray|X-ray]] | [[Macrocytic anemia echocardiography and ultrasound|Echocardiography and Ultrasound]] | [[Macrocytic anemia ct|CT]] | [[Macrocytic anemia mri|MRI]] | [[Macrocytic anemia other imaging findings|Other Imaging Findings]] | [[Macrocytic anemia other diagnostic studies|Other Diagnostic Studies]] |
| | |
| ==[[Macrocytic anemia physical examination|Physical Examination]]==
| |
| | |
| ==[[Macrocytic anemia laboratory findings|Laboratory Findings]]==
| |
| | |
| ==[[Macrocytic anemia electrocardiogram|Electrocardiogram]]==
| |
| | |
| ==[[Macrocytic anemia chest x ray|Chest X Ray]]==
| |
| | |
| ==[[Macrocytic anemia CT|CT]]==
| |
| | |
| ==[[Macrocytic anemia MRI|MRI]]==
| |
| | |
| ==[[Macrocytic anemia echocardiography or ultrasound|Echocardiography or Ultrasound]]==
| |
| | |
| ==[[Macrocytic anemia other imaging findings|Other Imaging Findings]]==
| |
| | |
| ==[[Macrocytic anemia other diagnostic studies|Other Diagnostic Studies]]==
| |
| | |
| ==Treatment== | | ==Treatment== |
| | | [[Macrocytic anemia medical therapy|Medical Therapy]] | [[Macrocytic anemia surgery|Surgery]] | [[Macrocytic anemia primary prevention|Primary Prevention]] | [[Macrocytic anemia secondary prevention|Secondary Prevention]] | [[Macrocytic anemia cost-effectiveness of therapy|Cost-Effectiveness of Therapy]] | [[Macrocytic anemia future or investigational therapies|Future or Investigational Therapies]] |
| ==[[Macrocytic anemia medical therapy|Medical Therapy]]==
| |
| | |
| ==[[Macrocytic anemia surgery|Surgery]]==
| |
| | |
| ==[[Macrocytic anemia primary prevention|Primary Prevention]]==
| |
| | |
| ==[[Macrocytic anemia secondary prevention|Secondary Prevention]]==
| |
| | |
| ==[[Macrocytic anemia cost-effectiveness of therapy|Cost-Effectiveness of Therapy]]==
| |
| | |
| ==[[Macrocytic anemia future or investigational therapies|Future or Investigational Therapies]]==
| |
|
| |
|
| ==Case Studies== | | ==Case Studies== |
| | :[[Macrocytic anemia case study one|Case #1]] |
|
| |
|
| ==[[Macrocytic anemia case study one|Case #1]]==
| |
|
| |
| ==Classification==
| |
| ===Megaloblastic anemias (DNA replication disorders)===
| |
| * Commonest cause of macrocytic anemia.
| |
| * In [[megaloblastic anemia]]s cells are larger because they cannot produce DNA quickly enough to divide at the right time as they grow, and thus grow too large before division.
| |
| * Causes for the DNA synthetic problem range from lack of certain vitamins needed to produce DNA (notably [[folate]] and [[B12]]), to poisons or inhibitors of DNA replication, such as some kinds of antiviral drugs and chemotherapeutic agents.
| |
| * The pathognomonic findings of megaloblastic anemia are: megaloblasts in [[bone marrow]], ovalocytes in the (peripheral) blood smear, and hypersegmented [[neutrophils]].
| |
|
| |
| ===Non megaloblastic macrocytic anemias===
| |
| * Non megaloblastic macrocytic anemias, are disorders associated with increased red cell membrane surface area
| |
| * It is commonly associated with pathologies of the liver and spleen which produce [[codocyte]]s or "target cells" which have a central collection of hemoglobin surrounded by a pallor (a thin area) then followed by a thicker collection of hemoglobin at the rim of the cell.
| |
|
| |
| ===Alcohol===
| |
| * Round macrocytes which are not codocytes are produced in chronic alcoholism (which produces a mild macrocytosis even in the absence of vitamin deficiency), apparently as a direct toxic effect of alcohol specifically on the bone marrow.
| |
|
| |
| ===Association with rapid red cell turnover and reticulocytosis===
| |
| Mild macrocytocis is a common finding associated with rapid blood restoration or production, since in general, "fresh" or newly-produced red cells ([[reticulocytes]]) are larger than the mean (average) size, due to slow shrinkage of normal cells over a normal red cell circulating lifetime. Thus, [[chronic obstructive pulmonary disease]] (COPD), in which which red cells are rapidly produced in response to low oxygen levels in the blood, often produces mild macrocytosis. Also, rapid blood replacement from the marrow after a traumatic blood loss, or rapid red blood cell turnover from rapid hemolysis, also often produces mild macrocytosis in the associated anemia. ==Diagnosis==
| |
|
| |
| ===History and Symptoms===
| |
|
| |
| *The major manifestations of Folate or B12 deficiency are related to the anemia and gastrointestinal dysfunction. Only B12 deficiency causes neurologic dysfunction. Constitutional symptoms related to anemia such as fatigue, dyspnea, lightheadedess, and anorexia occur. High output cardiac failure and angina are also consequences.
| |
|
| |
|
| Symptoms mostly related to GI mucosal abnormalities. Tend to be worse in folate rather than B12 deficiency. [[Diarrhea]], [[cheilosis]] and [[glossitis]] can be noted.
| |
|
| |
|
| *The classic picture of B12 deficiency is subacute combined degeneration of the dorsal columns. Specific for B12 deficiency, the patient will present with a broad based gait, ataxic, irritable, forgetful with numbness or paresthesias. Rhomberg and Babinski’s can be noted. Dementia may progress to frank “Megaloblastic Madness”. Remember, hematological abnormalities can occur without neurologic manifestations in B12 deficiency.
| |
|
| |
|
| ===Hematological findings===
| |
| MCV is often >110. Hct can often be as low as 15. Elevated LDH and bilirubin are seen since dyserythopoesis leads to destruction of >90% of RBC precursors. Hypersegmentation of PMNs is quite sensitive (>5% with 5 or more lobes or >1% with 6 lobes). Reticulocyte, WBC and platelets are low to normal. In one series of patients with B12 deficiency, 64% had a MCV greater than 100, and only 29% had anemia.
| |
| In general the [[blood film]] can point towards vitamin deficiency:
| |
| *Decreased [[red blood cell]] (RBC) count and [[hemoglobin]] levels
| |
| *Increased [[mean corpuscular volume]] (MCV >95 fl often >110) and [[mean corpuscular hemoglobin]] (MCH)
| |
| *The [[reticulocyte]] count is normal
| |
| *The [[platelet]] count may be reduced.
| |
| *[[Neutrophil granulocyte]]s may show multisegmented nuclei ("senile neutrophil"). This is thought to be due to decreased production and a compensatory prolonged lifespan for circulating neutrophils.
| |
| *[[Anisocytosis]] (increased variation in RBC size) and [[poikilocytosis]] (abnormally shaped RBCs).
| |
| *Macrocytes (larger than normal RBCs) are present.
| |
| *Ovalocytes (oval shaped RBCs) are present.
| |
| *[[Bone marrow]] (not normally checked in a patient suspected of megaloblastic anemia) shows megaloblastic [[hyperplasia]].
| |
| *[[Howell-Jolly body|Howell-Jolly bodies]] (chromosomal remnant) also present.
| |
|
| |
|
| '''Blood chemistries will also show:'''
| |
| *Increased homocysteine and methylmalonic acid in B12 deficiency
| |
| *Increased homocysteine in folate defiency
| |
| <div align="left">
| |
| <gallery heights="175" widths="175">
| |
| Image:Peripheral blood in megaloblastic anemia 0001.jpg|Peripheral blood in megaloblastic anemia
| |
| Image:Howell-Jolly bodies 0001.jpg|Howell-Jolly bodies
| |
| Image:Howell-Jolly bodies and erythroblast.jpg|Howell-Jolly bodies and erythroblast
| |
| </gallery>
| |
| </div>
| |
|
| |
|
| ===Analysis===
| |
| The [[Schilling test]] was performed in the past to determine the nature of the vitamin B12 deficiency, but due to the lack of available radioactive B12, it is now largely a historical artifact. Vitamin B{{ssub|12}} is a necessary prosthetic group to the enzyme [[methylmalonyl-coenzyme A mutase]]. B{{ssub|12}} deficiency leads to dysfunction of this enzyme and a buildup of its substrate, [[methylmalonic acid]], the elevated level of which can be detected in the urine and blood. Since the level of methylmalonic acid is not elevated in folic acid deficiency, this test provides a one tool in differentiating the two. However, since the test for elevated methylmalonic acid is not specific enough, the gold standard for the diagnosis of B12 deficiency is a low blood level of B12. Unlike the Shilling test, which often included B12 with intrinsic factor, a low level of blood B12 gives no indication as to the etiology of the low B12, which may result from a number of mechanisms.
| |
|
| |
|
| ==Treatment==
| |
| * Folate is administered 1mg QD. Higher doses may be required in malabsorptive syndromes. It is empirically given to those with SCD and those on HD.
| |
| * B12 must be given as a load then maintenance. Most advocate 1000 mcg IM Qweek x4 then 100mcg/month.
| |
| * LDH falls in 2 days. Hypokalemia requiring replacement can occur in the acute phase as new cells are being generated rapidly.
| |
| * A reticulocytosis begins in 3-5 days and peaks in 10 days. The HCT will rise within 10days. If it does not, suspect another disorder. Hypersegmented PMNs disappear in 10-14 days.
| |
| * Neurologic abnormalities may take up to 6 months to resolve if ever. The longer the disease has been present, the worse is the prognosis for recovery.
| |
| * Persons with PA have a 2x risk of gastric CA (in some studies). Screen for occult blood.
| |
|
| |
|
| [[el:Μακροκυτταρική αναιμία]]
| |
| [[sq:Anemi makrocitike]]
| |
| {{WikiDoc Help Menu}}
| |
| {{WikiDoc Sources}}
| |
|
| |
|
| ==References==
| |
| {{Reflist|2}}
| |
| [[es:Anemia megaloblástica]]
| |
| [[gl:Anemia megaloblástica]]
| |
| [[he:אנמיה מגלובלסטית]]
| |
| [[it:Anemia megaloblastica]]
| |
| [[pl:Niedokrwistość megaloblastyczna]]
| |
| [[pt:Anemia megaloblástica]]
| |
| [[ru:Пернициозная анемия]]
| |
| [[sl:Megaloblastna anemija]]
| |
| [[sr:Мегалобластна анемија]]
| |
| [[tr:Megaloblastik anemi]]
| |
|
| |
|
| {{WikiDoc Help Menu}} | | {{WikiDoc Help Menu}} |