Sandbox/AIRSG
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alejandro Lemor, M.D. [2]
Overview
Aortic insufficiency (AI) refers to the retrograde or backward flow of blood from the aorta into the left ventricle during diastole.[1][2][3][4] Aortic insufficiency can be an acute or chronic illnes and both differ in the causes and management. The most common causes of acute AI are aortic dissection and infective endocarditis and the preffered treatment in both cases surgical intervention. The most common cause of chronic AI is bicuspid aortic valve and the treatment will depend on the stage of the disease in which the patient is. Acute AI is a life-threatening condition and must be recognized and treated promptly.
Causes
Life Threatening Causes
Life-threatening causes include conditions which may result in death or permanent disability within 24 hours if left untreated.
Common Causes
- Bicuspid aortic valve
- Senile or degenerative calcific aortic valve disease[5]
- Hypertension
- Idiopthic dialation of the aorta
- Myxomatous degeneration
- Rheumatic fever
Click here for the complete list of causes.
FIRE: Focused Initial Rapid Evaluation
A Focused Initial Rapid Evaluation (FIRE) should be performed to identify patients in need of immediate intervention. The algorithm below is based on the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease.[6][7]
Boxes in red signify that an urgent management is needed.
Identify cardinal findings that increase the pretest probability of acute aortic regurgitation ❑
❑ ❑ | |||||||||||||||||||||||||||||||||||||||||||
Does the patient have any of the following findings that require urgent management? ❑ Tachycardia | |||||||||||||||||||||||||||||||||||||||||||
Diagnosis
A complete diagnostic approach should be carried out after a focused initial rapid evaluation is conducted and following initiation of any urgent intervention.[6][7]
Abbreviations: BP: blood pressure; CXR: chest X-ray; ECG: electrocardiogram; LV: left ventricle
Characterize the symptoms: Acute ❑ Dyspnea on exertion ❑ Orthopnea ❑ Paroxysmal nocturnal dyspnea ❑ Palpitations ❑ Chest pain | |||||||||||||||||||||||||||||||||||||||||
Inquire about past medical history: ❑ Previously healthy ❑ Cardiac disease: ❑ Rheumatic fever ❑ Pulmonary disease | |||||||||||||||||||||||||||||||||||||||||
Examine the patient: Vitals Cardiovascular examination
❑ Cardiac auscultation
❑ Search for other signs suggestive of aortic insufficiency
Respiratory examination | |||||||||||||||||||||||||||||||||||||||||
Order imaging studies:
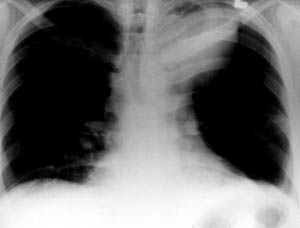
❑ ECG
❑ TTE
| |||||||||||||||||||||||||||||||||||||||||
Acute ❑ ❑ | Chronic ❑ ❑ | ||||||||||||||||||||||||||||||||||||||||
| Continue with the treatment of acute aortic insufficiency | Interpret the results from TTE | ||||||||||||||||||||||||||||||||||||||||
❑ ❑ | Mild to moderate (Stage B) ❑ ❑ | Asymptomatic severe (Stage C) ❑ ❑ | Symptomatic severe (Stage D) ❑ ❑ | ||||||||||||||||||||||||||||||||||||||
Treatment
Treatment of Acute Aortic Insufficiency
Shown below is an algorithm for the treatment of acute aortic insufficiency according to the 2014 AHA/ACC Guidelines on the management of valvular heart disease.[1][2][3][4]
Treatment ❑ The use of nitroprusside and inotropic agents (such as: dopamine and dobutamine) help reduce the LV end-diastolic pressure before surgery | |||||||||||||||||||||||||||||||||||||||||||||||
Mild or moderate | Severe | Urgent surgical intervention ❑ Aortic valve replacement | |||||||||||||||||||||||||||||||||||||||||||||
Antibiotic treatment A complete list of pathogen specific antibiotics regimens with appropriate dosages and duration of treatment is available here | |||||||||||||||||||||||||||||||||||||||||||||||
Chronic Aortic Insufficiency
Shown below is an algorithm summarizing the treatment approach to chronic aortic insufficiency (AI) according to the 2008 and 2014 AHA/ACC guidelines on the managenent of valvular heart disease.[1][2][3][4]
Do's
❑
Don'ts
❑ Do not use beta blockers in AI of causes other than AD as it will block the compensation tachycardia. ❑ Do not use intra-aortic baloon counterpulsation in severe acute AI as it will increase the aortic diastolic pressure and the regurgitant volume.
References
- ↑ 1.0 1.1 1.2 Connolly HM, Crary JL, McGoon MD; et al. (1997). "Valvular heart disease associated with fenfluramine-phentermine". N. Engl. J. Med. 337 (9): 581–8. doi:10.1056/NEJM199708283370901. PMID 9271479.
- ↑ 2.0 2.1 2.2 Weissman NJ (2001). "Appetite suppressants and valvular heart disease". Am. J. Med. Sci. 321 (4): 285–91. doi:10.1097/00000441-200104000-00008. PMID 11307869.
- ↑ 3.0 3.1 3.2 Schade R, Andersohn F, Suissa S, Haverkamp W, Garbe E (2007). "Dopamine agonists and the risk of cardiac-valve regurgitation". N. Engl. J. Med. 356 (1): 29–38. doi:10.1056/NEJMoa062222. PMID 17202453.
- ↑ 4.0 4.1 4.2 Zanettini R, Antonini A, Gatto G, Gentile R, Tesei S, Pezzoli G (2007). "Valvular heart disease and the use of dopamine agonists for Parkinson's disease". N. Engl. J. Med. 356 (1): 39–46. doi:10.1056/NEJMoa054830. PMID 17202454.
- ↑ Nishimura, RA. (2002). "Cardiology patient pages. Aortic valve disease". Circulation. 106 (7): 770–2. PMID 12176943. Unknown parameter
|month=ignored (help) - ↑ 6.0 6.1 "2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary". Retrieved 4 March 2014.
- ↑ 7.0 7.1 Bonow, R. O.; Carabello, B. A.; Chatterjee, K.; de Leon, A. C.; Faxon, D. P.; Freed, M. D.; Gaasch, W. H.; Lytle, B. W.; Nishimura, R. A.; O'Gara, P. T.; O'Rourke, R. A.; Otto, C. M.; Shah, P. M.; Shanewise, J. S. (2008). "2008 Focused Update Incorporated Into the ACC/AHA 2006 Guidelines for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): Endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons". Circulation. 118 (15): e523–e661. doi:10.1161/CIRCULATIONAHA.108.190748. ISSN 0009-7322.
- ↑ Williams BR, Steinberg JP (2006). "Images in clinical medicine. Müller's sign". The New England Journal of Medicine. 355 (3): e3. doi:10.1056/NEJMicm050642. PMID 16855259. Retrieved 2012-04-15. Unknown parameter
|month=ignored (help)