Conjunctivitis pathophysiology: Difference between revisions
No edit summary |
No edit summary |
||
| Line 34: | Line 34: | ||
Development of allergic conjunctivitis is the result of [[type 1 hypersensitivity]]. | Development of allergic conjunctivitis is the result of [[type 1 hypersensitivity]]. | ||
Following exposure to environmental [[allergens]] in sensitized individual, the cross-linking of [[IgE]] at the [[mast cell]] membrane level results in subsequent cell [[degranulation]] and secretion of [[histamine]],[loukotriene]], and [[prostaglandin]]. The principal effects of these products are [[vasodilation]] and smooth-muscle contraction. | Following exposure to environmental [[allergens]] in sensitized individual, the cross-linking of [[IgE]] at the [[mast cell]] membrane level results in subsequent cell [[degranulation]] and secretion of [[histamine]],[loukotriene]], and [[prostaglandin]]. The principal effects of these products are [[vasodilation]] and smooth-muscle contraction. | ||
Common airborne antigens involve in the [[pathogenesis]] of [[allergic conjunctivitis]] include [[pollen]], grass, and weeds.<ref name="pmid19134019">{{cite journal| author=Malling HJ, Montagut A, Melac M, Patriarca G, Panzner P, Seberova E et al.| title=Efficacy and safety of 5-grass pollen sublingual immunotherapy tablets in patients with different clinical profiles of allergic rhinoconjunctivitis. | journal=Clin Exp Allergy | year= 2009 | volume= 39 | issue= 3 | pages= 387-93 | pmid=19134019 | doi=10.1111/j.1365-2222.2008.03152.x | pmc=4233960 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=19134019 }} </ref><ref name="pmid17967188">{{cite journal| author=Kämpe M, Stålenheim G, Janson C, Stolt I, Carlson M| title=Systemic and local eosinophil inflammation during the birch pollen season in allergic patients with predominant rhinitis or asthma. | journal=Clin Mol Allergy | year= 2007 | volume= 5 | issue= | pages= 4 | pmid=17967188 | doi=10.1186/1476-7961-5-4 | pmc=2174506 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=17967188 }} </ref> | |||
Combination of type 1 and type 4 hypersensitivity reactions may be responsible for '''giant papillary conjunctivitis'''. Also, prolonged mechanical irritation to the [[superior tarsal muscle|superior tarsal]] conjunctiva of the upper lid from [[foreign bodies]] may also be a contributing factor in giant papillary conjunctivitis.<ref name="pmid7886881">{{cite journal| author=Donshik PC| title=Giant papillary conjunctivitis. | journal=Trans Am Ophthalmol Soc | year= 1994 | volume= 92 | issue= | pages= 687-744 | pmid=7886881 | doi= | pmc=1298525 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=7886881 }} </ref><ref name="pmid10703125">{{cite journal| author=Donshik PC, Porazinski AD| title=Giant papillary conjunctivitis in frequent-replacement contact lens wearers: a retrospective study. | journal=Trans Am Ophthalmol Soc | year= 1999 | volume= 97 | issue= | pages= 205-16; discussion 216-20 | pmid=10703125 | doi= | pmc=1298261 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=10703125 }} </ref> | Combination of type 1 and type 4 hypersensitivity reactions may be responsible for '''giant papillary conjunctivitis'''. Also, prolonged mechanical irritation to the [[superior tarsal muscle|superior tarsal]] conjunctiva of the upper lid from [[foreign bodies]] may also be a contributing factor in giant papillary conjunctivitis.<ref name="pmid7886881">{{cite journal| author=Donshik PC| title=Giant papillary conjunctivitis. | journal=Trans Am Ophthalmol Soc | year= 1994 | volume= 92 | issue= | pages= 687-744 | pmid=7886881 | doi= | pmc=1298525 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=7886881 }} </ref><ref name="pmid10703125">{{cite journal| author=Donshik PC, Porazinski AD| title=Giant papillary conjunctivitis in frequent-replacement contact lens wearers: a retrospective study. | journal=Trans Am Ophthalmol Soc | year= 1999 | volume= 97 | issue= | pages= 205-16; discussion 216-20 | pmid=10703125 | doi= | pmc=1298261 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=10703125 }} </ref> | ||
| Line 45: | Line 45: | ||
* [[Anxiety disorder]] | * [[Anxiety disorder]] | ||
* [[Depression]] | * [[Depression]] | ||
The exact pathogenesis of the keratoconjunctivitis sicca associated [[Sjögren's syndrome]] is not fully understood. It is thought that keratoconjunctivitis sicca associated [[Sjögren's syndrome]] is the result of [[lymphosytic infiltration]] and malfunction of the [[lacrimal glands]]. | |||
This lymphasitic infiltration ([[CD4+ T cells]] and [[B cells]]) may result in [[lacrimal gland]] dysfunction and reduced [[tear]] production (Mediated by [[apopitosis]]). | |||
====Superior Limbic Keratoconjunctivitis==== | ====Superior Limbic Keratoconjunctivitis==== | ||
[[Superior limbic keratoconjunctivitis|Superior limbic keratoconjunctivitis (SLK)]] is disease characterized by [[inflammation]] of the upper palpebral and superior [[bulbar conjunctiva]] | [[Superior limbic keratoconjunctivitis|Superior limbic keratoconjunctivitis (SLK)]] is disease characterized by [[inflammation]] of the upper palpebral and superior [[bulbar conjunctiva]]. | ||
The exact pathogenesis of superior limbic keratoconjunctivitis is not fully understood, a mechanical [[hypothesis]] seems most attractive. It is thought that mechanical trauma from tight upper lids or loose redundant conjunctiva | The exact pathogenesis of superior limbic keratoconjunctivitis is not fully understood, a mechanical [[hypothesis]] seems most attractive. It is thought that mechanical trauma from tight upper lids or loose redundant conjunctiva can lead to the disruption of normal [[epithelium]]. Also association between [[thyroid]] abnormalities ([[Graves ophthalmopathy]]) and superior limbic keratoconjunctivitis has been reported.<ref name="pmid2695351">{{cite journal| author=Nelson JD| title=Superior limbic keratoconjunctivitis (SLK). | journal=Eye (Lond) | year= 1989 | volume= 3 ( Pt 2) | issue= | pages= 180-9 | pmid=2695351 | doi=10.1038/eye.1989.26 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=2695351 }} </ref><ref name="pmid25792798">{{cite journal| author=Chelala E, El Rami H, Dirani A, Fakhoury H, Fadlallah A| title=Extensive superior limbic keratoconjunctivitis in Graves' disease: case report and mini-review of the literature. | journal=Clin Ophthalmol | year= 2015 | volume= 9 | issue= | pages= 467-8 | pmid=25792798 | doi=10.2147/OPTH.S79561 | pmc=4362972 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=25792798 }} </ref><ref name=Superior_limbic_keratoconjunctivitis > American Academy of Ophthalmology (2015) http://eyewiki.aao.org/Superior_limbic_keratoconjunctivitis Accessed on June 27, 2016 </ref> | ||
===Gross Pathology=== | ===Gross Pathology=== | ||
| Line 63: | Line 57: | ||
*Pseudomembrane formation | *Pseudomembrane formation | ||
*[[Chemosis]] | *[[Chemosis]] | ||
*Eyelid | *Eyelid edema | ||
*[[Conjunctival hemorrhage]] (specific for Acute hemorrhagic conjunctivitis) | *[[Conjunctival hemorrhage]] (specific for Acute hemorrhagic conjunctivitis) | ||
Revision as of 19:40, 28 July 2016
|
Conjunctivitis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Conjunctivitis pathophysiology On the Web |
|
American Roentgen Ray Society Images of Conjunctivitis pathophysiology |
|
Risk calculators and risk factors for Conjunctivitis pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [5]; Associate Editor(s)-in-Chief: Sara Mehrsefat, M.D. [6]
Overview
Conjunctivitis is defined as inflammation of bulbar and/or palpebral conjunctiva. Conjunctivitis has many etiologies, but the majority of cases can be caused by allergies or infection. Infective conjunctivitis is an infection of the conjunctiva either caused by viruses or bacteria. Airborne antigens may be involved in the pathogenesis of allergic conjunctivitis. Common airborne antigens include pollen, grass, and weeds. Keratoconjunctivitis sicca (dry eye syndrome) is a multifactorial disease and associated with different medical conditions.[1][2]
Pathophysiology
Pathogenesis
Infective Conjunctivitis
Infective conjunctivitis is an infection of the conjunctiva either caused by viruses or bacteria. Any change in the host defense, or in the species of normal flora of the eye can lead to clinical infection and conjunctivitis. Ocular conjunctival surfaces are usually colonized by different organisms such as adenoviruses, Staphylococcus aureus, Haemophilus influenzae, and Streptococcus pneumoniae.
Change in the normal flora may occur by:[3]
- External contamination
- Contact lens wear
- Swimming
Infective conjunctivitis is usually spread by:[1][2]
- Direct contact with the infected person’s eye drainage or drainage from the person’s cough, sneeze, or runny nose
- Contact with the infected person’s fingers, hands or objects (eye makeup applicators, towels, shared eye medications)
- Adjacent infectious sites (rubbing of the eyes)
Neonatal Conjunctivitis
Neonatal conjunctivitis is occurring in a newborn during the first month of life, and often known as ophthalmia neonatorum. Neonatal conjunctivitis is mainly caused by sexually transmitted diseases agents such as Chlamydia trachomatis, Neisseria gonorrhoeae, and Herpes simplex virus (HSV). Chlamydia trachomatis is the most common cause of ophthalmia neonatorum in the developed countries because of higher prevalence of chlamydia as a sexually transmitted disease. The recognized routes of transmission of the organisms to the newborns include:[4]
- Infected birth canal during vaginal birth
- Transmembrane transmission of the infection
- Transplacental transmission of the infection
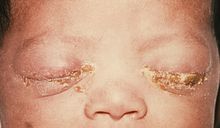
On gross pathology, It is characterized by eyelids edema, erythema of the palpebral conjunctiva, and purulent eye discharge. On a gram stained of conjunctival smear, one or more polymorph nuclear per oil immersion field may be detected. Additionally, neonatal conjunctivitis may caused by irritation. it is generally secondary to the instillation of silver nitrate drops for ocular prophylaxis.[5]
Allergic Conjunctivitis
Development of allergic conjunctivitis is the result of type 1 hypersensitivity. Following exposure to environmental allergens in sensitized individual, the cross-linking of IgE at the mast cell membrane level results in subsequent cell degranulation and secretion of histamine,[loukotriene]], and prostaglandin. The principal effects of these products are vasodilation and smooth-muscle contraction. Common airborne antigens involve in the pathogenesis of allergic conjunctivitis include pollen, grass, and weeds.[6][7]
Combination of type 1 and type 4 hypersensitivity reactions may be responsible for giant papillary conjunctivitis. Also, prolonged mechanical irritation to the superior tarsal conjunctiva of the upper lid from foreign bodies may also be a contributing factor in giant papillary conjunctivitis.[8][9]
Keratoconjunctivitis Sicca
Keratoconjunctivitis sicca (dry eye syndrome) is a multifactorial disease and associated with different medical conditions such as:[10][11]
- Sjögren's syndrome
- Ocular surface disease
- Ocular allergy
- Dysfunction of the lacrimal gland with reduced tear production and mucin deficiency
- Anxiety disorder
- Depression
The exact pathogenesis of the keratoconjunctivitis sicca associated Sjögren's syndrome is not fully understood. It is thought that keratoconjunctivitis sicca associated Sjögren's syndrome is the result of lymphosytic infiltration and malfunction of the lacrimal glands. This lymphasitic infiltration (CD4+ T cells and B cells) may result in lacrimal gland dysfunction and reduced tear production (Mediated by apopitosis).
Superior Limbic Keratoconjunctivitis
Superior limbic keratoconjunctivitis (SLK) is disease characterized by inflammation of the upper palpebral and superior bulbar conjunctiva. The exact pathogenesis of superior limbic keratoconjunctivitis is not fully understood, a mechanical hypothesis seems most attractive. It is thought that mechanical trauma from tight upper lids or loose redundant conjunctiva can lead to the disruption of normal epithelium. Also association between thyroid abnormalities (Graves ophthalmopathy) and superior limbic keratoconjunctivitis has been reported.[12][13][14]
Gross Pathology
On gross pathology, the following are characteristic findings of conjunctivitis:[15]
- Conjunctival injection
- Mucopurulent discharge or non-purulent discharge
- Pseudomembrane formation
- Chemosis
- Eyelid edema
- Conjunctival hemorrhage (specific for Acute hemorrhagic conjunctivitis)
Microscopic histopathological analysis
On microscopic histopathological analysis, the following are characteristic findings of conjunctivitis:[16]
- Mild spongiotic reaction pattern (low power view of the histology)
- Stromal infiltration by polymorphonuclear, leukocytes, plasma cells, mastocytes, and lymphocyte
- Eosinophils (allergic conjunctivitis)
- Numerous neutrophils (bacterial conjunctivitis)
- Hyperplastic with increase numbers of plasma cell (chronic conjunctivitis)
- epithelial cells Keratinization of the superior limbus (Superior limbic keratoconjunctivitis (SLK))
- Dyskeratosis (Superior limbic keratoconjunctivitis (SLK))
Images
The following are gross and microscopic images associated with conjunctivitis.
-
Viral conjunctivitis[17]
-
Acute hemorrhagic conjunctivitis[18]
-
Neonatal conjunctivitis<ref> Centers for Disease Control and Prevention's Public Health Image
-
Chlamydial conjunctivitis (Day 5-14)[19]
References
- ↑ 1.0 1.1 Azari AA, Barney NP (2013). "Conjunctivitis: a systematic review of diagnosis and treatment". JAMA. 310 (16): 1721–9. doi:10.1001/jama.2013.280318. PMC 4049531. PMID 24150468.
- ↑ 2.0 2.1 Kyei S, Koffuor GA, Ramkissoon P, Abokyi S, Owusu-Afriyie O, Wiredu EA (2015). "Possible Mechanism of Action of the Antiallergic Effect of an Aqueous Extract of Heliotropium indicum L. in Ovalbumin-Induced Allergic Conjunctivitis". J Allergy (Cairo). 2015: 245370. doi:10.1155/2015/245370. PMC 4657065. PMID 26681960.
- ↑ Everitt H, Kumar S, Little P (2003). "A qualitative study of patients' perceptions of acute infective conjunctivitis". Br J Gen Pract. 53 (486): 36–41. PMC 1314490. PMID 12564275.
- ↑ Treadwell P (1994). "Sexually transmitted diseases in neonates and infants". Semin Dermatol. 13 (4): 256–61. PMID 7848819.
- ↑ Mallika P, Asok T, Faisal H, Aziz S, Tan A, Intan G (2008). "Neonatal conjunctivitis - a review". Malays Fam Physician. 3 (2): 77–81. PMC 4170304. PMID 25606121.
- ↑ Malling HJ, Montagut A, Melac M, Patriarca G, Panzner P, Seberova E; et al. (2009). "Efficacy and safety of 5-grass pollen sublingual immunotherapy tablets in patients with different clinical profiles of allergic rhinoconjunctivitis". Clin Exp Allergy. 39 (3): 387–93. doi:10.1111/j.1365-2222.2008.03152.x. PMC 4233960. PMID 19134019.
- ↑ Kämpe M, Stålenheim G, Janson C, Stolt I, Carlson M (2007). "Systemic and local eosinophil inflammation during the birch pollen season in allergic patients with predominant rhinitis or asthma". Clin Mol Allergy. 5: 4. doi:10.1186/1476-7961-5-4. PMC 2174506. PMID 17967188.
- ↑ Donshik PC (1994). "Giant papillary conjunctivitis". Trans Am Ophthalmol Soc. 92: 687–744. PMC 1298525. PMID 7886881.
- ↑ Donshik PC, Porazinski AD (1999). "Giant papillary conjunctivitis in frequent-replacement contact lens wearers: a retrospective study". Trans Am Ophthalmol Soc. 97: 205–16, discussion 216-20. PMC 1298261. PMID 10703125.
- ↑ Sivaraman KR, Jivrajka RV, Soin K, Bouchard CS, Movahedan A, Shorter E; et al. (2016). "Superior Limbic Keratoconjunctivitis-like Inflammation in Patients with Chronic Graft-Versus-Host Disease". Ocul Surf. doi:10.1016/j.jtos.2016.04.003. PMID 27179980.
- ↑ Messmer EM (2015). "The pathophysiology, diagnosis, and treatment of dry eye disease". Dtsch Arztebl Int. 112 (5): 71–81, quiz 82. doi:10.3238/arztebl.2015.0071. PMC 4335585. PMID 25686388.
- ↑ Nelson JD (1989). "Superior limbic keratoconjunctivitis (SLK)". Eye (Lond). 3 ( Pt 2): 180–9. doi:10.1038/eye.1989.26. PMID 2695351.
- ↑ Chelala E, El Rami H, Dirani A, Fakhoury H, Fadlallah A (2015). "Extensive superior limbic keratoconjunctivitis in Graves' disease: case report and mini-review of the literature". Clin Ophthalmol. 9: 467–8. doi:10.2147/OPTH.S79561. PMC 4362972. PMID 25792798.
- ↑ American Academy of Ophthalmology (2015) http://eyewiki.aao.org/Superior_limbic_keratoconjunctivitis Accessed on June 27, 2016
- ↑ National Eye Institute (2015) [1] Accessed on June 24, 2016
- ↑ DermNet NZ (2015)[2] Accessed on June 26, 2016
- ↑ Image Courtesy of Joyhil09 [3]
- ↑ Image Courtesy of James Heilman [4]
- ↑ http://picasaweb.google.com/mcmumbi/USMLEIIImages
![Viral conjunctivitis[17]](/images/e/ee/An_eye_with_viral_conjunctivitis.jpg)
![Chlamydial conjunctivitis (Day 5-14)[19]](/images/3/39/Chlamydial_conjunctivitis.jpg)