Hepatitis B pathophysiology: Difference between revisions
No edit summary |
No edit summary |
||
| Line 14: | Line 14: | ||
During HBV infection, the host [[immune response]] causes both hepatocellular damage and viral clearance. While the innate immune response does not play a significant role in these processes, the adaptive immune response, particularly virus-specific [[cytotoxic T lymphocytes]] (CTLs), contributes to nearly all of the liver injury associated with HBV infection. By killing infected cells and by producing antiviral [[cytokine]]s capable of purging HBV from viable hepatocytes, CTLs also eliminate the virus.<ref name=Iannacone_2006>{{cite journal | author=Iannacone M. ''et al'' | title=Pathogenetic and antiviral immune responses against hepatitis B virus | journal=[http://www.futuremedicine.com/doi/abs/10.2217/17460794.1.2.189 Future Virology] | year=2006 | pages=189-196 | volume=1 | issue=2 | During HBV infection, the host [[immune response]] causes both hepatocellular damage and viral clearance. While the innate immune response does not play a significant role in these processes, the adaptive immune response, particularly virus-specific [[cytotoxic T lymphocytes]] (CTLs), contributes to nearly all of the liver injury associated with HBV infection. By killing infected cells and by producing antiviral [[cytokine]]s capable of purging HBV from viable hepatocytes, CTLs also eliminate the virus.<ref name=Iannacone_2006>{{cite journal | author=Iannacone M. ''et al'' | title=Pathogenetic and antiviral immune responses against hepatitis B virus | journal=[http://www.futuremedicine.com/doi/abs/10.2217/17460794.1.2.189 Future Virology] | year=2006 | pages=189-196 | volume=1 | issue=2 | ||
==References== | ==References== | ||
{{ | {{reflist|2}} | ||
[[Category:Needs overview]] | [[Category:Needs overview]] | ||
Revision as of 16:26, 18 December 2012
|
Hepatitis B |
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Hepatitis B pathophysiology On the Web |
|
American Roentgen Ray Society Images of Hepatitis B pathophysiology |
|
Risk calculators and risk factors for Hepatitis B pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Pathophysiology
Transmission
Transmission results from exposure to infectious blood or body fluids containing blood. Possible forms of transmission include (but are not limited to) unprotected sexual contact, blood transfusions, re-use of contaminated needles and syringes, and vertical transmission from mother to child during childbirth. Without intervention, a mother who is positive for the hepatitis B surface antigen confers a 20% risk of passing the infection to her offspring at the time of birth. This risk is as high as 90% if the mother is also positive for the hepatitis B e antigen. HBV can also be transmitted between family members within households, possibly by contact of nonintact skin or mucous membrane with secretions or saliva containing HBV.[1]
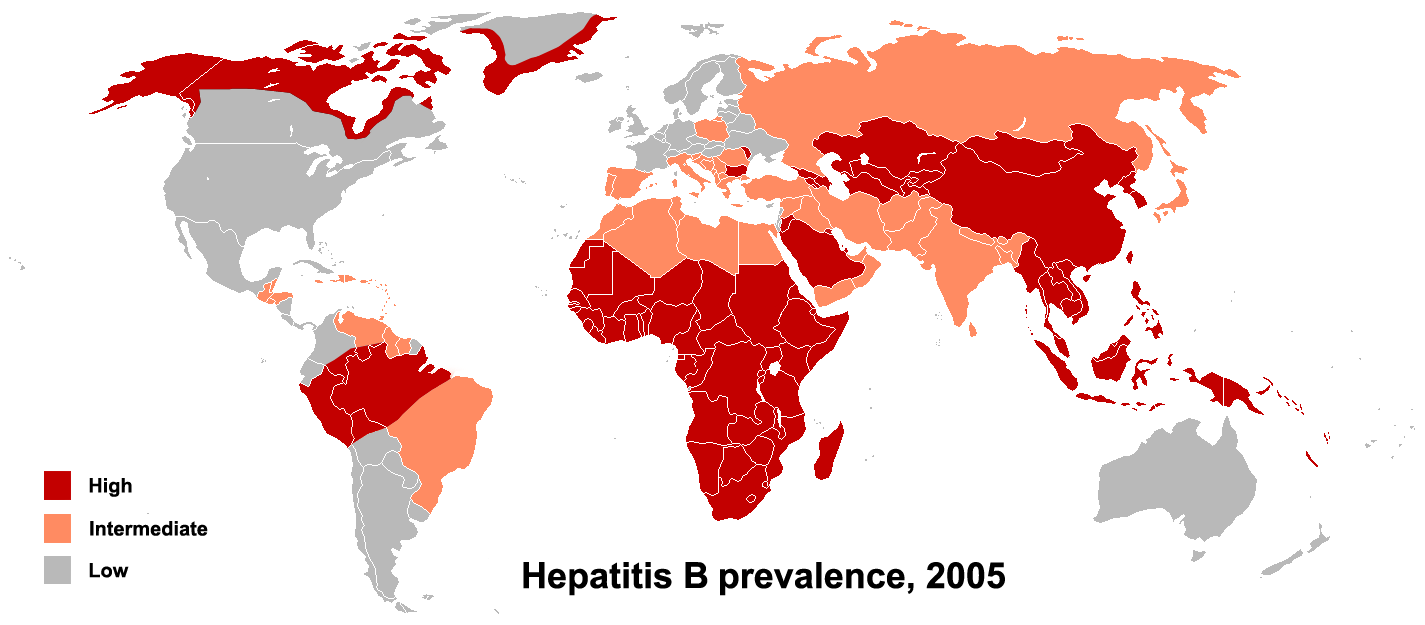
The primary method of transmission reflects the prevalence of chronic HBV infection in a given area. In low prevalence areas such as the continental United States and Western Europe, where less than 2% of the population is chronically infected, injection drug abuse and unprotected sex are the primary methods, although other factors may be important.[2] In moderate prevalence areas, which include Eastern Europe, Russia, and Japan, where 2-7% of the population is chronically infected, the disease is predominantly spread among children. In high prevalence areas such as China and South East Asia, transmission during childbirth is most common, although in other areas of high endemicity such as Africa, transmission during childhood is also a significant factor.[3] The prevalence of chronic HBV infection in areas of high endemicity is at least 8%.
Roughly 16-40% of unimmunized sexual partners of individuals with hepatitis B will be infected through sexual contact. The risk of transmission is closely related to the rate of viral replication in the infected individual at the time of exposure.
Immunopathogenesis
During HBV infection, the host immune response causes both hepatocellular damage and viral clearance. While the innate immune response does not play a significant role in these processes, the adaptive immune response, particularly virus-specific cytotoxic T lymphocytes (CTLs), contributes to nearly all of the liver injury associated with HBV infection. By killing infected cells and by producing antiviral cytokines capable of purging HBV from viable hepatocytes, CTLs also eliminate the virus.<ref name=Iannacone_2006>{{cite journal | author=Iannacone M. et al | title=Pathogenetic and antiviral immune responses against hepatitis B virus | journal=Future Virology | year=2006 | pages=189-196 | volume=1 | issue=2
References
- ↑ Petersen NJ, Barrett DH, Bond WW, Berquist KR, Favero MS, Bender TR, Maynard JE (1976). "Hepatitis B surface antigen in saliva, impetiginous lesions, and the environment in two remote Alaskan villages". Appl. Environ. Microbiol. 32 (4): 572–574. PMID 791124.
- ↑ Redd JT, Baumbach J, Kohn W; et al. (2007). "Patient-to-patient transmission of hepatitis B virus associated with oral surgery" (PDF). J Infect Dis. 195 (9): 1311&ndash, 4.
- ↑ Alter MJ (2003). "Epidemiology and prevention of hepatitis B". Semin. Liver Dis. 23 (1): 39–46. doi:10.1055/s-2003-37583. PMID 12616449.