Triclabendazole
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Zach Leibowitz [2]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Triclabendazole is an anthelmintic that is FDA approved for the treatment of fascioliasis in patients 6 years of age and older. Common adverse reactions include abdominal pain, hyperhidrosis, nausea, decreased appetite, headache, urticaria, diarrhea, vomiting, musculoskeletal chest pain, and pruritus.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Triclabendazole is indicated for the treatment of fascioliasis in adult patients. The recommended dose of EGATEN is 2 doses of 10 mg/kg given 12 hours apart in patients 6 years of age and older.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding triclabendazole Off-Label Guideline-Supported Use and Dosage (Adult) in the drug label.
Non–Guideline-Supported Use
There is limited information regarding triclabendazole Off-Label Non-Guideline-Supported Use and Dosage (Adult) in the drug label.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Triclabendazole is indicated for the treatment of fascioliasis in pediatric patients of 6 years of age and older. The recommended dose of EGATEN is 2 doses of 10 mg/kg given 12 hours apart in patients 6 years of age and older.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding triclabendazole Off-Label Guideline-Supported Use and Dosage (Pediatric) in the drug label.
Non–Guideline-Supported Use
There is limited information regarding triclabendazole Off-Label Non-Guideline-Supported Use and Dosage (Pediatric) in the drug label.
Contraindications
- Triclabendazole is contraindicated in patients with known hypersensitivity to triclabendazole and/or to other benzimidazole derivatives or to any of the excipients in triclabendazole.
Warnings
QT Prolongation
- Transient prolongation of the mean QTc interval was noted on the electrocardiographic recordings in dogs. Monitor ECG in patients with a history of prolongation of the QTc interval or a history of symptoms compatible with a long QT interval or when triclabendazole is used in patients who receive drugs that prolong the QT interval.
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in clinical trials of another drug and may not reflect the rates observed in clinical practice.
- The safety of triclabendazole was evaluated in 208 adult and pediatric patients 5 years of age and older who participated in 6 clinical trials for the treatment of fascioliasis and received 10 mg/kg or 20 mg/kg of triclabendazole; of these, 6 patients failed the 10 mg/kg dose and were retreated with 20 mg/kg. The 10 mg/kg dosing regimen is not approved. In these trials, 186 patients received a single dose of 10 mg/kg and 28 patients received a dose of 20 mg/kg as two divided doses. Pooled data for adverse reactions reported in more than 2% of the patients in these clinical trials for the 10 mg/kg and 20 mg/kg dosing regimens are presented in Table 1.
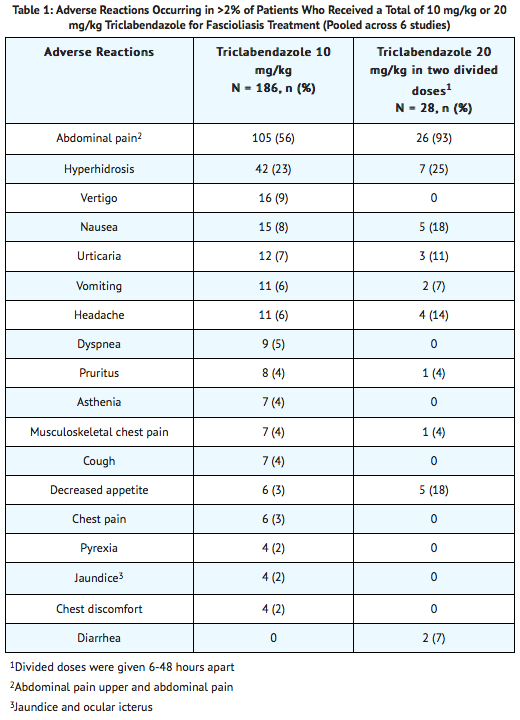
- Adverse reactions reported in less than or equal to 2% of patients who received a total of 10 mg/kg of triclabendazole were constipation, biliary colic, arthralgia, back pain, spinal pain, and chromaturia. Some adverse reactions associated with triclabendazole treatment in fascioliasis, e.g. abdominal pain, biliary colic, and jaundice, could be secondary to the infection and may be more frequent and/or severe in patients with a heavy worm burden.
- The safety profile of triclabendazole 20 mg/kg in divided doses in a non-hepatic parasitic infection (N = 104) was generally similar to the safety profile in fascioliasis, except for a lower incidence of post-treatment abdominal pain.
Liver Enzyme Elevations
- In clinical studies, up to one third of patients had liver enzyme elevations at baseline, which generally improved post-treatment. Of those with normal liver enzyme values at baseline, 6.8%, 4.5%, 4.2% and 3% of patients had post-treatment elevations in bilirubin, aspartate aminotransferase (AST), alkaline phosphatase (ALP) and alanine aminotransferase (ALT), respectively. Transient increases in liver enzymes and total bilirubin in fascioliasis patients receiving triclabendazole are reported in the literature.
Postmarketing Experience
- Resistance to triclabendazole has been reported outside the United States
Drug Interactions
Effect of triclabendazole on CYP2C19 Substrates
- No specific clinical drug interaction studies have been conducted for triclabendazole. However, in vitro data suggest the potential for increased plasma concentrations of CYP2C19 substrates with concomitant use of triclabendazole. The potential elevation in concentrations of concomitantly used CYP2C19 substrates is expected to be transient based on the short elimination half-life and short treatment duration of triclabendazole.
- For those CYP2C19 substrate drugs that require therapeutic monitoring of systemic drug exposures, if the plasma concentrations of the CYP2C19 substrates are elevated during administration of triclabendazole, re-check the plasma concentration of the CYP2C19 substrates after cessation of triclabendazole therapy.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): Risk Summary
- There are no available data on triclabendazole use in pregnant women to inform a drug-associated risk of major birth defects, miscarriage or adverse maternal or fetal outcomes. Reproductive studies in animals (rat and rabbits) have not shown a risk of increased fetal abnormalities with exposure to triclabendazole during organogenesis at doses approximately 0.3 to 1.6 times the maximum recommended human dose (MRHD) of 20 mg/kg based on body surface area comparison.
- The estimated background risk of major birth defects and miscarriage for the indicated population are unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2%-4% and 15%-20%, respectively.
Animal Data
- Embryo-fetal developmental toxicity studies revealed no malformations in rats and rabbits at doses up to 200 mg/kg/day and 20 mg/kg/day, respectively (approximately 1.6 times and 0.3 times the MRHD based on body surface area comparison, respectively). The animals were treated orally during organogenesis, starting on Day 6 of the pregnancy until Day 15 in rats and Day 18 in rabbits. Maternal toxicity was noted at doses greater than or equal to 100 mg/kg/day in rats and 10 mg/kg/day in rabbits, which was associated with lower fetus weights and delayed ossification. These findings were considered indicative of delayed physiological growth that was secondary to maternal toxicity. No increase in malformation or other abnormalities was observed at any dose level in either species.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Triclabendazole in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Triclabendazole during labor and delivery.
Nursing Mothers
- There are no data on the presence of triclabendazole in human milk, the effects on the breastfed infant, or the effects on milk production. Published animal data indicate that triclabendazole is detected in goat milk when administered as a single dose to one lactating animal. When a drug is present in animal milk, it is likely that the drug will be present in human milk. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for triclabendazole and any potential adverse effects on the breastfed infant from triclabendazole or from the underlying maternal condition.
Pediatric Use
- Safety and effectiveness of triclabendazole has been established in pediatric patients aged 6 years and older.
- Safety and effectiveness of triclabendazole in pediatric patients below the age of 6 years have not been established.
Geriatic Use
- Clinical studies of triclabendazole did not include sufficient numbers of patients aged 65 and over to determine whether the elderly respond differently from younger patients. In general, dose selection for an elderly patient should be cautious, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Gender
There is no FDA guidance on the use of Triclabendazole with respect to specific gender populations.
Race
There is no FDA guidance on the use of Triclabendazole with respect to specific racial populations.
Renal Impairment
- Triclabendazole has not been studied in patients with renal impairment.
Hepatic Impairment
- Triclabendazole has not been studied in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Triclabendazole in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Triclabendazole in patients who are immunocompromised.
Administration and Monitoring
Administration
- The recommended dose of triclabendazole is 2 doses of 10 mg/kg given 12 hours apart in patients 6 years of age and older. The 250 mg tablets are functionally scored and divisible into two equal halves of 125 mg. If the dosage cannot be adjusted exactly, round the dose upwards.
- Take triclabendazole orally with food. Triclabendazole tablets can be swallowed whole or divided in half and taken with water or crushed and administered with applesauce. The crushed tablet mixed with applesauce is stable for up to 4 hours.
Monitoring
There is limited information regarding Triclabendazole Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Triclabendazole and IV administrations.
Overdosage
- The reported symptom of overdosage following ingestion of approximately 54 mg/kg of triclabendazole (approximately 2.7 times the recommended dose) was nausea. The patient recovered following osmotic diuresis.
Pharmacology
| |
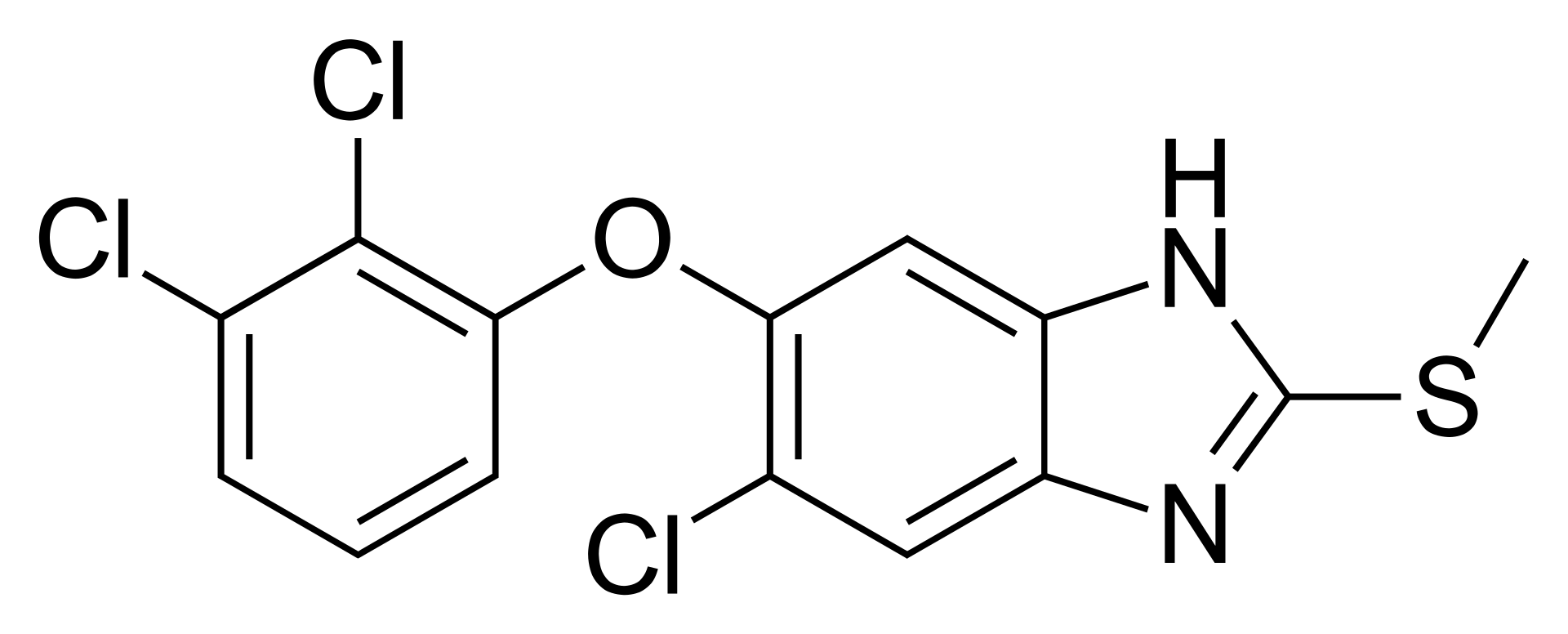
Triclabendazole
| |
| Systematic (IUPAC) name | |
| 5-Chloro-6-(2,3-dichlorophenoxy)-2-(methylthio)-1H-benzimidazole | |
| Identifiers | |
| CAS number | |
| ATC code | P02 Template:ATCvet |
| PubChem | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | 359.658 |
| SMILES | & |
| Physical data | |
| Melt. point | 175–176 °C (347–349 °F) |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | Oxidation to sulfone and sulfoxide metabolites |
| Half life | 22–24 hs |
| Excretion | Feces (>95%), urine (2%), milk (<1%) |
| Therapeutic considerations | |
| Pregnancy cat. |
? |
| Legal status | |
| Routes | by mouth |
Mechanism of Action
- Triclabendazole is an anthelmintic against Fasciola species.
Structure

Pharmacodynamics
- Triclabendazole exposure-response relationships and the time course of pharmacodynamics response are unknown.
Pharmacokinetics
- After oral administration of a single dose of 10 mg/kg triclabendazole with a 560-kcal meal to patients with fascioliasis, mean peak plasma concentrations (Cmax) for triclabendazole, the sulfoxide and sulfone metabolites were 1.16, 38.6, and 2.29 μmol/L, respectively. The area under the curve (AUC) for triclabendazole, the sulfoxide and sulfone metabolites were 5.72, 386, and 30.5 μmol∙h/L, respectively.
Absorption
- Following oral administration of a single dose of triclabendazole at 10 mg/kg with a 560-kcal meal to patients with fascioliasis, the median Tmax for the parent compound and the sulfoxide metabolite was 3 to 4 hours.
Effect of Food
- Cmax and AUC of triclabendazole and sulfoxide metabolite increased approximately 3-fold and 2-fold respectively when triclabendazole was administered as a single dose at 10 mg/kg with a meal containing a total of approximately 560 kcal (consisting of 2 cups of sweetened white coffee, a roll with cheese, and a roll with butter and jam). In addition, the sulfoxide metabolite Tmax increased from 2 hours in the fasted state to 4 hours in the fed state.
Distribution
- The apparent volume of distribution (Vd) of the sulfoxide metabolite in fed patients is approximately 1 L/kg.
- Protein-binding of triclabendazole, sulfoxide metabolite and sulfone metabolite in human plasma was 96.7%, 98.4% and 98.8% respectively.
Elimination
- The plasma elimination half-life (t1/2) of triclabendazole, the sulfoxide and sulfone metabolites in humans is approximately 8, 14, and 11 hours, respectively.
Metabolism
- Based on in vitro studies, triclabendazole is primarily metabolized by CYP1A2 (approximately 64%) into its active sulfoxide metabolite and to a lesser extent by CYP2C9, CYP2C19, CYP2D6, CYP3A, and FMO. This sulfoxide metabolite is further metabolized primarily by CYP2C9 to the active sulfone metabolite and to a lesser extent by CYP1A1, CYP1A2, CYP1B1, CYP2C19, CYP2D6 and CYP3A4, in vitro.
Excretion
- No excretion data is available in humans. However, in animals, the drug is largely excreted via the biliary tract in the feces (90%), together with the sulfoxide and sulfone metabolite. Less than 10% of an oral dose is excreted in the urine.
Specific Populations
- The pharmacokinetics of triclabendazole were not studied in patients with renal or hepatic impairment.
Pediatric Patients
- No dedicated pediatric pharmacokinetic studies were conducted. However, in one pharmacokinetic study of 20 patients, 7 children (ages 9 to 15 years) were dosed with triclabendazole 10 mg/kg single dose. AUC values of triclabendazole sulfoxide were 20% lower in these pediatric patients in the fed state than in the 13 patients above 15 years of age, but the difference was not statistically significant.
Drug Interaction Studies
- Clinical drug interaction studies have not been conducted for triclabendazole.
In Vitro Studies
- Triclabendazole and its sulfoxide and sulfone metabolites have the potential to inhibit CYP1A2, CYP2A6, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP2D6, and CYP3A at clinically relevant plasma concentrations, with the highest potential of inhibition on CYP2C19. No in vitro studies were conducted to assess the ability of triclabendazole and its metabolites to induce CYP enzymes. No in vitro studies were conducted to assess the ability of triclabendazole and its metabolites to induce or inhibit transporters.
Microbiology
Mechanism of Action
- The mechanism by which triclabendazole exhibits its effect against Fasciola species is not fully elucidated. Studies in vitro and/or in infected animals suggest that triclabendazole and its active metabolites (sulfoxide and sulfone) are absorbed by the tegument of the immature and mature worms, leading to a decrease of the resting membrane potential, inhibition of tubulin function as well as protein and enzyme synthesis. These metabolic disturbances are associated with inhibition of motility, disruption of the surface as well as ultrastructure that includes inhibition of spermatogenesis and vitelline cells.
Antimicrobial Activity
- Triclabendazole and its metabolites are active against the immature and mature worms of Fasciola hepatica and Fasciola gigantic.
Resistance
- Studies in vitro and in vivo as well as case reports suggest a potential for development of resistance to triclabendazole.
- The mechanism of resistance may be multifactorial that include changes in drug uptake/efflux mechanisms, the target molecules, and altered drug metabolism. The clinical significance of triclabendazole resistance in humans is not established.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
Mutagenesis
- No genotoxic potential was noted for triclabendazole tested in a battery of 6 genotoxicity in vitro and in vivo assays which include a bacterial reverse mutation assay, chromosome aberration assays, and a micronucleus assay.
Impairment of Fertility
- No drug-related effects on reproductive performance, mating ratios or fertility indices have been noted in a 2-generation reproductive and developmental toxicity study in rats. The animals were treated with up to 75 ppm triclabendazole via diet, amounting to a mean daily intake of 7.3 mg/kg/day (approximately 0.1 times the MRHD based on body surface area comparison) for a period of 110 days, which included a 12-day mating period beginning on Day 62 of dosing and continuing until the offspring were weaned.
Animal Toxicology and/or Pharmacology
- Dietary administration of triclabendazole at a dose of 39 mg/kg/day (1.1-times the MRHD based on body surface area comparison) was associated with a transient increase in the QT and QTc intervals on weeks 5 and 9 in some dogs in a 13-week study resulting in QT (QTc) intervals of 212-227 (318-338) msec in the 39 mg/kg dose group (adjusted) compared to 190-193 (280-297) msec in controls. At Week 13, no statistically significant differences were noted between the treatment and control groups.
- Additionally, when dogs were administered triclabendazole at a single dose of 40 or 100 mg/kg (1.1 or 2.7 times the MRHD based on body surface area comparison), increase in QTc intervals was observed resulting in QTc intervals of 217-247 msec compared to a normal (historical control) of 193-231 msec. However, plasma levels of the sulfone metabolite in dogs (which is thought to mediate QTc prolongation) was about 100-500 times the plasma level of the sulfone metabolite measured in human plasma.
- In the 13-week study in beagle dogs, slight anemia accompanied by minimal increases in reticulocyte and nucleated red cell counts were observed at 39 mg/kg/day (1.1 times the MRHD based on body surface area comparison) predominantly at week 9 of dosing.
Clinical Studies
- An open label, randomized trial, conducted in Vietnam compared the efficacy of triclabendazole (two 10 mg/kg doses given 12 hours apart with food) to oral artesunate (4 mg/kg, given once daily for 10 days). One hundred patients (age range: 9-74 years) with acute symptomatic fascioliasis were randomized, 50 in each treatment group. At 3 months after treatment, 92% and 76% (difference 16%; 95% CI [1.7, 30.8], p = 0.035) of patients in the triclabendazole and artesunate arms respectively, reported no clinical symptoms.
- The clinical development program of triclabendazole for the treatment of fascioliasis included 6 non-randomized, open label studies performed in Cuba, Bolivia, Peru, Chile, and Iran in a total of 245 adult and pediatric patients with stool-confirmed fascioliasis. All studies were similar in design. The studied triclabendazole doses ranged from 5 mg/kg to 20 mg/kg administered on Days 1-3. Cure was defined as absence of Fasciola eggs in the stool based on the Kato-Katz method at Day 60 in patients who were positive at baseline. Across these studies, there was a finding of a dose response. Specifically, the Day 60 cure rate was highest (95.5%; 95% CI [77%, 100%]) for the 20 mg/kg dose, which was given in 2 divided doses, followed by cure rates of 88% (95% CI [64%, 99%]), 80% (95% CI [73%, 86%]), and 50% (95% CI [27%, 73%]) in the 15 mg/kg, 10 mg/kg, and 5 mg/kg dose groups, respectively. The 5 mg/kg, 10 mg/kg, and 15 mg/kg dosing regimens are not approved [see Dosage and Administration (2)]. These rates were significantly higher than that estimated from patients receiving an inadequate, non-triclabendazole treatment in a separate study (22%; 95% CI [9.8, 38.2]).
How Supplied
- Triclabendazole tablets are supplied as pale red, speckled, capsule shaped, biconvex tablets, with imprint “EG EG” on one side and functionally scored on both sides. Each tablet contains 250 mg of triclabendazole. Triclabendazole tablets are available as:
- Blister packs of 4 tablets
Storage
Store in the original container. Store below 30°C (86°F).
Images
Drug Images
{{#ask: Page Name::Triclabendazole |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel

{{#ask: Label Page::Triclabendazole |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
Important Administration Instructions
- Advise patients that triclabendazole should be taken orally with food. The tablets can be swallowed whole or divided in half and taken with water, or crushed and administered with applesauce. The crushed tablet mixed with applesauce is stable for up to 4 hours.
QT Prolongation
- Advise patients with a history of prolongation of the QTc interval or a history of symptoms compatible with a long QT interval or when triclabendazole is used in patients who receive drugs that prolong the QT interval that their ECGs will need to be monitored.
Precautions with Alcohol
Alcohol-Triclabendazole interaction has not been established. Talk to your doctor regarding the effects of taking alcohol with this medication.
Brand Names
Look-Alike Drug Names
There is limited information regarding Triclabendazole Look-Alike Drug Names in the drug label.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.