Trazodone
{{DrugProjectFormSinglePage |authorTag=Chetan Lokhande, M.B.B.S [1] |genericName=Trazodone |aOrAn=a |drugClass=5-HT2 Antagonists |indication=depression |hasBlackBoxWarning=Yes |adverseReactions=gastrointestinal: constipation (7% to 8% ), diarrhea (up to 9% ), nausea (21% ), vomiting (at least 1% ), xerostomia (14% to 33.8% ),musculoskeletal: backache (5% ) neurologic: confusion (up to 5.7% ), dizziness (25% ), headache (9.9% to 33% ), insomnia (6.4% to 9.9% ), somnolence (23.9% to 46% ), ophthalmic: blurred vision (5% to 14.7% ), psychiatric: dream disorder (up to 5.1% ), feeling nervous (6.4% to 14.8% ), other: fatigue (5.7% to 15% ) |blackBoxWarningTitle=Warning: Suicidality And Antidepressant Drugs |blackBoxWarningBody= Increased risk of suicidal thinking and behavior in children, adolescents and young adults taking antidepressants for major depressive disorder (MDD) and other psychiatric disorders. Trazodone is not approved for use in pediatric patients |fdaLIADAdult=* Depression
- Immediate-release tablets, initial 150 mg/day orally in divided doses; may increase dosage by 50 mg/day every 3 to 4 days; MAX, 400 mg/day for outpatients and 600 mg/day for inpatients.
- Extended-release tablets, initial 150 mg Orally once daily in the evening, preferably at bedtime; may increase by 75 mg once daily every 3 days; MAX, 375 mg/day; dose may be gradually reduced once adequate response achieved.
|offLabelAdultGuideSupport=* Insomnia
- 50 to 100 mg orally, 1 hour prior to bedtime has been used in clinical trials.
|offLabelAdultNoGuideSupport=There is limited information about Off-Label Non–Guideline-Supported Use of Trazodone in adult patients. |fdaLIADPed=There is limited information about FDA-labeled indications and dosage information of Trazodone in pediatric patients. |offLabelPedGuideSupport=There is limited information about Off-Label Guideline-Supported Use of Trazodone in pediatric patients. |offLabelPedNoGuideSupport=There is limited information about Off-Label Non–Guideline-Supported Use of Trazodone in pediatric patients. |contraindications=None |warnings=====Clinical Worsening and Suicide Risk====
- Patients with major depressive disorder (MDD), both adult and pediatric, may experience worsening of their depression and/or the emergence of suicidal ideation and behavior (suicidality) or unusual changes in behavior, whether or not they are taking antidepressant medications, and this risk may persist until significant remission occurs. Suicide is a known risk of depression and certain other psychiatric disorders and these disorders themselves are the strongest predictors of suicide. There has been a long standing concern, however, that antidepressants may have a role in inducing worsening of depression and the emergence of suicidality in certain patients during the early phases of treatment. Pooled analyses of short- term placebo-controlled trials of antidepressant drugs (SSRIs and others) showed that these drugs increase the risk of suicidal thinking and behavior (suicidality) in children, adolescents, and young adults (ages 18 – 24) with MDD and other psychiatric disorders. Short-term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond age 24; there was a reduction with antidepressants compared to placebo in adults aged 65 and older.
- The pooled analyses of placebo-controlled trials in children and adolescents with MDD, obsessive compulsive disorder (OCD), or other psychiatric disorders included a total of 24 short-term trials of 9 antidepressant drugs in over 4,400 patients. The pooled analyses of placebo-controlled trials in adults with MDD or other psychiatric disorders included a total of 295 short-term trials (median duration of 2 months) of 11 antidepressant drugs in over 77,000 patients. There was considerable variation in risk of suicidality among drugs, but a tendency toward an increase in the younger patients for almost all drugs studied. There were differences in absolute risk of suicidality across the different indications, with the highest incidence in MDD. The risk differences (drug vs. placebo), however, were relatively stable within age strata and across indications. These risk differences (drug-placebo difference in the number of cases of suicidality per 1,000 patients treated) are provided in Table
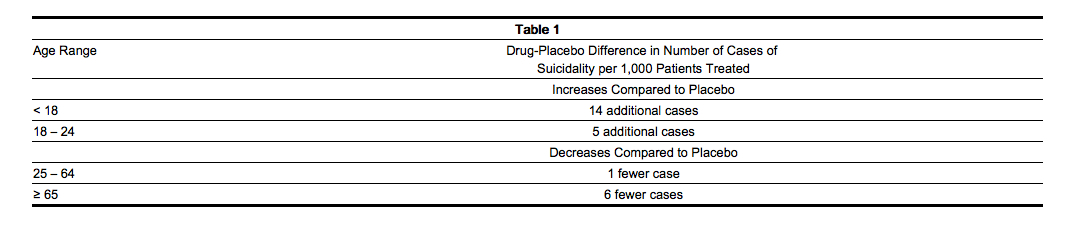
- No suicides occurred in any of the pediatric trials. There were suicides in the adult trials, but the number was not sufficient to reach any conclusion about drug effect on suicide.
- It is unknown whether the suicidality risk extends to longer-term use, i.e., beyond several months. However, there is substantial evidence from placebo-controlled maintenance trials in adults with depression that the use of antidepressants can delay the recurrence of depression.
- All patients being treated with antidepressants for any indication should be monitored appropriately and observed closely for clinical worsening, suicidality, and unusual changes in behavior, especially during the initial few months of a course of drug therapy, or at times of dose changes, either increases or decreases.
- The following symptoms, anxiety, agitation, panic attacks, insomnia, irritability, hostility, aggressiveness, impulsivity, akathisia (psychomotor restlessness), hypomania, and mania, have been reported in adult and pediatric patients being treated with antidepressants for major depressive disorder as well as for other indications, both psychiatric and nonpsychiatric. Although a causal link between the emergence of such symptoms and either the worsening of depression and/or the emergence of suicidal impulses has not been established, there is concern that such symptoms may represent precursors to emerging suicidality.
- Consideration should be given to changing the therapeutic regimen, including possibly discontinuing the medication, in patients whose depression is persistently worse, or who are experiencing emergent suicidality or symptoms that might be precursors to worsening depression or suicidality, especially if these symptoms are severe, abrupt in onset, or were not part of the patient's presenting symptoms.
- Families and caregivers of patients being treated with antidepressants for major depressive disorder or other indications, both psychiatric and nonpsychiatric, should be alerted about the need to monitor patients for the emergence of agitation, irritability, unusual changes in behavior, and the other symptoms described above, as well as the emergence of suicidality, and to report such symptoms immediately to health care providers. Such monitoring should include daily observation by families and caregivers. Prescriptions for trazodone should be written for the smallest quantity of tablets consistent with good patient management, in order to reduce the risk of overdose.
Serotonin Syndrome or Neuroleptic Malignant Syndrome (NMS)-like Reactions
- The development of a potentially life-threatening serotonin syndrome or neuroleptic malignant syndrome (NMS)-like reactions have been reported with antidepressants alone and may occur with trazodone treatment, but particularly with concomitant use of other serotoninergic drugs (includingSSRIs, SNRIs and triptans) and with drugs that impair metabolism of serotonin (including monoamine oxidase inhibitors [MAOIs]), or with antipsychotics or other dopamine antagonists. Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, and hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination) and/or gastrointestinal symptoms (e.g., nausea, vomiting, and diarrhea). Serotonin syndrome, in its most severe form, can resemble neuroleptic malignant syndrome, which includes hyperthermia, muscle rigidity, autonomic instability with possible rapid fluctuation of vital signs, and mental status changes.
- Treatment with trazodone hydrochloride tablets and any concomitant serotonergic or antidopaminergic agents, including antipsychotics, should be discontinued immediately if the above reactions occur and supportive symptomatic treatment should be initiated.
- Trazodone hydrochloride tablets should not be used within 14 days of an MAOI [see Warnings and Precautions and Drug Interactions].
- If concomitant treatment with trazodone hydrochloride tablets and an SSRI, SNRI or a 5- hydroxytryptamine receptor agonist (triptan) is clinically warranted, careful observation of the patient is advised, particularly during treatment initiation and dose increases.
- The concomitant use of trazodone hydrochloride tablets with serotonin precursors (such as tryptophan) is not recommended.
Screening Patients for Bipolar Disorder and Monitoring for Mania/Hypomania
- A major depressive episode may be the initial presentation of bipolar disorder. It is generally believed (though not established in controlled trials) that treating such an episode with an antidepressant alone may increase the likelihood of precipitation of a mixed/manic episode in patients at risk for bipolar disorder. Whether any of the symptoms described for clinical worsening and suicide risk represent such a conversion is unknown. However, prior to initiating treatment with an antidepressant, patients with depressive symptoms should be adequately screened to determine if they are at risk for bipolar disorder; such screening should include a detailed psychiatric history, including a family history of suicide, bipolar disorder, and depression. It should be noted that trazodone hydrochloride tablets is not approved for use in treating bipolar depression.
QT Prolongation and Risk of Sudden Death
- Trazodone is known to prolong the QT/QTc interval. Some drugs that prolong the QT/QTc interval can cause Torsades de Pointes with sudden, unexplained death. The relationship of QT prolongation is clearest for larger increases (20 msec and greater), but it is possible that smaller QT/QTc prolongations may also increase risk, especially in susceptible individuals, such as those with hypokalemia, hypomagnesemia, or a genetic predisposition to prolonged QT/QTc.
- Although Torsades de Pointes has not been observed with the use of trazodone hydrochloride tablets at recommended doses in premarketing trials, experience is too limited to rule out an increased risk. However, there have been postmarketing reports of Torsades de Pointes with the immediate-release form of trazodone (in the presence of multiple confounding factors), even at doses of 100 mg per day or less.
Use in Patients with Heart Disease
- Trazodone hydrochloride is not recommended for use during the initial recovery phase of myocardial infarction.
- Caution should be used when administering trazodone hydrochloride tablets to patients with cardiac disease and such patients should be closely monitored, since antidepressant drugs (including trazodone hydrochloride) may cause cardiac arrhythmias.
- QT prolongation has been reported with trazodone therapy [see Warnings and Precautions]. Clinical studies in patients with pre-existing cardiac disease indicate that trazodone hydrochloride may be arrhythmogenic in some patients in that population. Arrhythmias identified include isolated PVCs, ventricular couplets, tachycardia with syncope, and Torsades de Pointes. Postmarketing events have been reported at doses of 100 mg or less with the immediate-release form of trazodone.
- Concomitant administration of drugs that prolong the QT interval or that are inhibitors of CYP3A4 may increase the risk of cardiac arrhythmia.
Orthostatic Hypotension and Syncope
- Hypotension, including orthostatic hypotension and syncope has been reported in patients receiving trazodone hydrochloride. Concomitant use with an antihypertensive may require a reduction in the dose of the antihypertensive drug.
Abnormal Bleeding
- Postmarketing data have shown an association between use of drugs that interfere with serotonin reuptake and the occurrence of gastrointestinal (GI) bleeding. While no association between trazodone and bleeding events, in particular GI bleeding, was shown, patients should be cautioned about potential risk of bleeding associated with the concomitant use of trazodone and NSAIDs, aspirin, or other drugs that affect coagulation or bleeding. Other bleeding events related to SSRIs and SNRIs have ranged from ecchymosis, hematoma, epistaxis, and petechiae to life-threatening hemorrhages.
Interaction with MAOIs
- In patients receiving serotonergic drugs in combination with a monoamine oxidase inhibitor (MAOI), there have been reports of serious, sometimes fatal reactions including hyperthermia, rigidity, myoclonus, autonomic instability with rapid fluctuation in vital signs, and mental status changes that include extreme agitation progressing to delirium and coma. These reactions have also been reported in patients who have recently discontinued antidepressant treatment and have been started on an MAOI. Some cases presented with features resembling neuroleptic malignant syndrome. Furthermore, limited animal data on the effects of combined use of serotonergic antidepressants and MAOIs suggest that these drugs may act synergistically to elevate blood pressure and evoke behavioral excitation. Therefore, it is recommended that trazodone hydrochloride tablets should not be used in combination with an MAOI or within 14 days of discontinuing treatment with an MAOI. Similarly, at least 14 days should be allowed after stopping trazodone hydrochloride tablets before starting an MAOI.
Priapism
- Rare cases of priapism (painful erections greater than 6 hours in duration) were reported in men receiving trazodone. Priapism, if not treated promptly, can result in irreversible damage to the erectile tissue. Men who have an erection lasting greater than 6 hours, whether painful or not, should immediately discontinue the drug and seek emergency medical attention [see Adverse Reactions and Overdosage].
- Trazodone should be used with caution in men who have conditions that might predispose them to priapism (e.g., sickle cell anemia, multiple myeloma, or leukemia), or in men with anatomical deformation of the penis (e.g., angulation, cavernosal fibrosis, or Peyronie's disease).
Hyponatremia
- Hyponatremia may occur as a result of treatment with antidepressants. In many cases, this hyponatremia appears to be the result of the syndrome of inappropriate antidiuretic hormone secretion (SIADH). Cases with serum sodium lower than 110 mmol/L have been reported. Elderly patients may be at greater risk of developing hyponatremia with antidepressants. Also, patients taking diuretics or who are otherwise volume-depleted can be at greater risk. Discontinuation of trazodone hydrochloride tablets should be considered in patients with symptomatic hyponatremia and appropriate medical intervention should be instituted.
- Signs and symptoms of hyponatremia include headache, difficulty concentrating, memory impairment, confusion, weakness, and unsteadiness, which can lead to falls. Signs and symptoms associated with more severe and/or acute cases have included hallucination, syncope, seizure, coma, respiratory arrest, and death.
Potential for Cognitive and Motor Impairment
- Trazodone hydrochloride tablets may cause somnolence or sedation and may impair the mental and/or physical ability required for the performance of potentially hazardous tasks. Patients should be cautioned about operating hazardous machinery, including automobiles, until they are reasonably certain that the drug treatment does not affect them adversely.
Discontinuation Symptoms
- Withdrawal symptoms including anxiety, agitation and sleep disturbances, have been reported with trazodone. Clinical experience suggests that the dose should be gradually reduced before complete discontinuation of the treatment.
|clinicalTrials=* The following serious adverse reactions are described elsewhere in the labeling:
- Clinical Worsening and Suicide Risk [see Boxed Warning and Warnings and Precautions]
- Serotonin Syndrome or NMS-like Reactions [see Warnings and Precautions]
- QT Prolongation and Risk of Sudden Death [see Warnings and Precautions]
- Orthostatic Hypotension [see Warnings and Precautions]
- Abnormal bleeding events [see Warnings and Precautions]
- Priapism [see Warnings and Precautions]
- Hyponatremia [see Warnings and Precautions]
- Cognitive and Motor Impairment [see Warnings and Precautions]
- Discontinuation symptoms [see Warnings and Precautions]
- The most common adverse reactions (reported in ≥5% and at twice the rate of placebo) are: Somnolence/sedation, dizziness, constipation, vision blurred.
- Table 2 presents the summary of adverse events (AEs) leading to discontinuation of trazodone hydrochloride tablets treatment with an incidence of at least 1% and at least twice that for placebo.
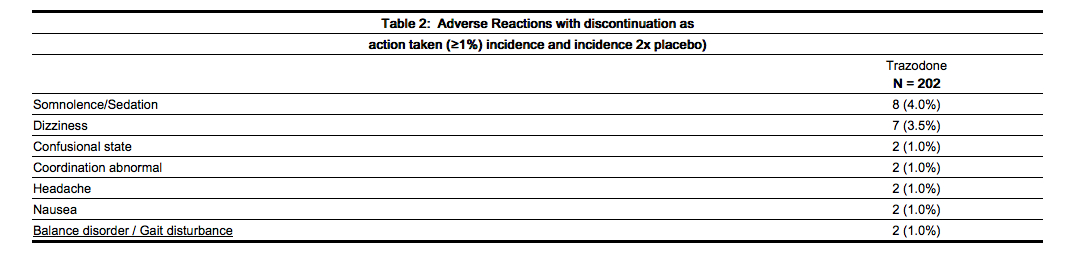
- The table below is presented solely to indicate the relative frequency of adverse events reported in representative controlled clinical studies conducted to evaluate the safety and efficacy of trazodone hydrochloride.
- The figures cited cannot be used to predict concisely the incidence of untoward events in the course of usual medical practice where patient characteristics and other factors often differ from those which prevailed in the clinical trials. These incidence figures, also, cannot be compared with those obtained from other clinical studies involving related drug products and placebo as each group of drug trials is conducted under a different set of conditions.
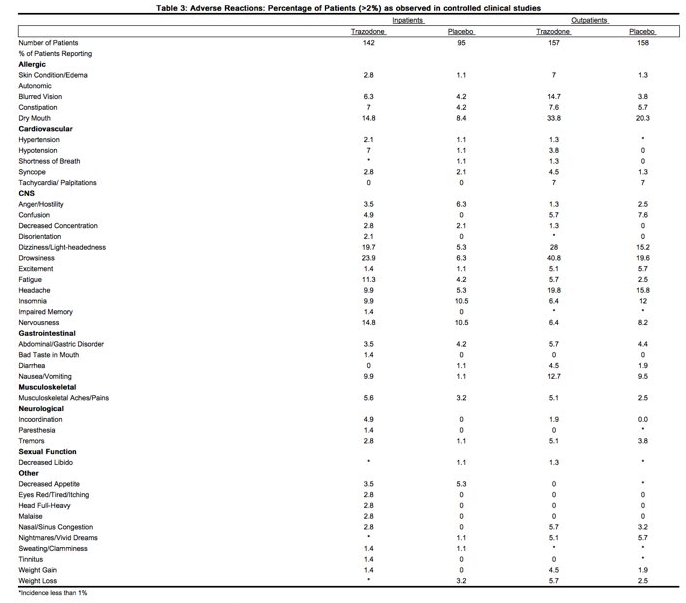
- Occasional sinus bradycardia has occurred in long-term studies.
- In addition to the relatively common (i.e., greater than 1%) untoward events enumerated above, the following adverse events have been reported to occur in association with the use of trazodone hydrochloride in the controlled clinical studies: akathisia, allergic reaction, anemia, chest pain, delayed urine flow, early menses, flatulence, hallucinations/delusions, hematuria, hyper-salivation, hypomania, impaired speech, impotence, increased appetite, increased libido, increased urinary frequency, missed periods, muscle twitches, numbness, and retrograde ejaculation.
|postmarketing=* Spontaneous reports regarding trazodone hydrochloride received from postmarketing experience include the following: abnormal dreams, agitation, alopecia, anxiety, aphasia, apnea, ataxia, breast enlargement or engorgement, cardiospasm, cerebrovascular accident, chills, cholestasis, clitorism, congestive heart failure, diplopia, edema, extrapyramidal symptoms, grand mal seizures, hallucinations, hemolytic anemia, hirsutism, hyperbilirubinemia, increased amylase, increased salivation, insomnia, leukocytosis, leukonychia, jaundice, lactation, liver enzyme alterations, methemoglobinemia, nausea/vomiting (most frequently), paresthesia, paranoid reaction, priapism [see Warnings and Precautions and Patient Counseling Information], pruritus, psoriasis, psychosis, rash, stupor, inappropriate ADH syndrome, tardive dyskinesia, unexplained death, urinary incontinence, urinary retention, urticaria, vasodilation, vertigo, and weakness.
- Cardiovascular system effects which have been reported include the following: conduction block, orthostatic hypotension and syncope, palpitations, bradycardia, atrial fibrillation, myocardial infarction, cardiac arrest, arrhythmia, ventricular ectopic activity, including ventricular tachycardia and QT prolongation. In postmarketing surveillance, prolonged QT interval, Torsades de Pointes, and ventricular tachycardia have been reported with the immediate-release form of trazodone at doses of 100 mg per day or less [see Warnings and Precautions ].
|drugInteractions=* MAOs
- MAOIs should not be used within 14 days of trazodone [see Warnings and Precautions].
- Central Nervous System (CNS) Depressants
- Trazodone may enhance the response to alcohol, barbiturates, and other CNS depressants.
- Cytochrome P450 3A4 Inhibitors
- In vitro drug metabolism studies suggest that there is a potential for drug interactions when trazodone is given with cytochrome P450 3A4 (CYP3A4) inhibitors. The effect of short-term administration of ritonavir (200 mg twice daily, 4 doses) on the pharmacokinetics of a single dose of trazodone (50 mg) has been studied in 10 healthy subjects. The Cmax of trazodone increased by 34%, the AUC increased 2.4-fold, the half-life increased by 2.2-fold, and the clearance decreased by 52%. Adverse effects including nausea, hypotension, and syncope were observed when ritonavir and trazodone were co-administered. It is likely that ketoconazole, indinavir, and other CYP3A4 inhibitors such as itraconazole may lead to substantial increases in trazodone plasma concentrations with the potential for adverse effects. If trazodone is used with a potent CYP3A4 inhibitor, the risk of cardiac arrhythmia may be increased [see Warnings and Precautions] and a lower dose of trazodone should be considered.
- Cytochrome P450 Inducers (e.g., carbamazepine)
- Carbamazepine induces CYP3A4. Following co-administration of carbamazepine 400 mg per day with trazodone 100 mg to 300 mg daily, carbamazepine reduced plasma concentrations of trazodone and m- chlorophenlypiperazine (an active metabolite) by 76% and 60% respectively, compared to pre- carbamazepine values. Patients should be closely monitored to see if there is a need for an increased dose of trazodone when taking both drugs.
- Digoxin and Phenytoin
- Increased serum digoxin or phenytoin levels have been reported in patients receiving trazodone concurrently with either of these drugs. Monitor serum levels and adjust dosages as needed.
- Serotonergic Drugs
- Based on the mechanism of action of trazodone and the potential for serotonin syndrome, caution is advised when trazodone is co-administered with other drugs that may affect the neurotransmitter systems [see Warnings and Precautions].
- NSAIDs, Aspirin, or Other Drugs Affecting Coagulation or Bleeding
- Due to a possible association between serotonin modulating drugs and gastrointestinal bleeding, patients should be monitored for and cautioned about the potential risk of bleeding associated with the concomitant use of trazodone and NSAIDs, aspirin, or other drugs that affect coagulation or bleeding [see Warnings and Precautions]
- Warfarin
- There have been reports of altered (either increased or decreased) prothrombin times in taking both warfarin and trazodone.
|FDAPregCat=C |useInPregnancyFDA=Trazodone hydrochloride has been shown to cause increased fetal resorption and other adverse effects on the fetus in two studies using the rat when given at dose levels approximately 30 – 50 times the proposed maximum human dose. There was also an increase in congenital anomalies in one of three rabbit studies at approximately 15 – 50 times the maximum human dose. There are no adequate and well-controlled studies in pregnant women. Trazodone hydrochloride should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. |useInNursing=Trazodone and/or its metabolites have been found in the milk of lactating rats, suggesting that the drug may be secreted in human milk. Caution should be exercised when Trazodone is administered to a nursing woman. |useInPed=Safety and effectiveness in the pediatric population have not been established [see Boxed Warning and Warnings and Precautions ]. Trazodone hydrochloride should not be used in children or adolescents. |useInGeri=* Reported clinical literature and experience with trazodone has not identified differences in responses between elderly and younger patients. However, as experience in the elderly with trazodone hydrochloride is limited, it should be used with caution in geriatric patients.
- Antidepressants have been associated with cases of clinically significant hyponatremia in elderly patients who may be at greater risk for this adverse reaction [see Warnings and Precautions ].
|useInRenalImpair=Trazodone has not been studied in patients with renal impairment. Trazodone should be used with caution in this population. |useInHepaticImpair=Trazodone has not been studied in patients with hepatic impairment. Trazodone should be used with caution in this population. |overdose=* Human Experience
- Death from overdose has occurred in patients ingesting trazodone and other CNS depressant drugs concurrently (alcohol; alcohol and chloral hydrate and diazepam; amobarbital; chlordiazepoxide; or meprobamate).
- The most severe reactions reported to have occurred with overdose of trazodone alone have been priapism, respiratory arrest, seizures, and ECG changes, including QT prolongation. The reactions reported most frequently have been drowsiness and vomiting. Overdosage may cause an increase in incidence or severity of any of the reported adverse reactions.
- Management of Overdose
- There is no specific antidote for trazodone hydrochloride overdose.
- Treatment should consist of those general measures employed in the management of overdosage with any drug effective in the treatment of major depressive disorder.
- Ensure an adequate airway, oxygenation and ventilation. Monitor cardiac rhythm and vital signs.
- General supportive and symptomatic measures are also recommended. Induction of emesis is not recommended. Gastric lavage with a large bore orogastric tube with appropriate airway protection, if needed, may be indicated if performed soon after ingestion, or in symptomatic patients. Activated charcoal should be administered. Forced diuresis may be useful in facilitating elimination of the drug.
- In managing overdosage, consider the possibility of multiple drug involvement. The physician should consider contacting a poison control center for additional information on the treatment of any overdose.
|drugBox={{Drugbox2 | verifiedrevid = 457287206 | IUPAC_name = 2-{3-[4-(3-chlorophenyl)piperazin-1-yl]propyl}[1,2,4]triazolo[4,3-a]pyridin-3(2H)-one | image = Trazodoneimage1.png | width = 250 | image2 = Trazodone image 2.png | width2 = 250
| tradename = Desyrel, Molipaxin, Oleptro, Trazorel, Trittico | Drugs.com = Monograph | MedlinePlus = a681038 | pregnancy_US = C | legal_US = Rx-only | legal_UK = POM | legal_AU = S4 | routes_of_administration = Oral
| bioavailability = 65% (Oral)[1]
| metabolism = Hepatic (CYP3A4)[1]
| elimination_half-life = 7 hours (immediate-release),
10 hours (extended-release)[1]
| excretion = 21% faeces,
70-75% urine[1]
| CASNo_Ref =
| CAS_number_Ref =
| CAS_number = 19794-93-5
| ATC_prefix = N06
| ATC_suffix = AX05
| PubChem = 5533
| IUPHAR_ligand = 213
| DrugBank_Ref =
| DrugBank = DB00656
| ChemSpiderID_Ref =
| ChemSpiderID = 5332
| UNII_Ref =
| UNII = YBK48BXK30
| KEGG_Ref =
| KEGG = D08626
| ChEBI_Ref =
| ChEBI = 9654
| ChEMBL_Ref =
| ChEMBL = 621
| C=19 | H=22 | Cl=1 | N=5 | O=1
| molecular_weight = 371.864 g/mol
| smiles = Clc4cccc(N3CCN(CCCN1/N=C2/C=C\C=C/N2C1=O)CC3)c4
| InChI = 1/C19H22ClN5O/c20-16-5-3-6-17(15-16)23-13-11-22(12-14-23)8-4-10-25-19(26)24-9-2-1-7-18(24)21-25/h1-3,5-7,9,15H,4,8,10-14H2
| InChIKey = PHLBKPHSAVXXEF-UHFFFAOYAD
| StdInChI_Ref =
| StdInChI = 1S/C19H22ClN5O/c20-16-5-3-6-17(15-16)23-13-11-22(12-14-23)8-4-10-25-19(26)24-9-2-1-7-18(24)21-25/h1-3,5-7,9,15H,4,8,10-14H2
| StdInChIKey_Ref =
| StdInChIKey = PHLBKPHSAVXXEF-UHFFFAOYSA-N
}}
|mechAction=The mechanism of trazodone's antidepressant action is not fully understood, but is thought to be related to its potentiation of serotonergic activity in the CNS.
|structure=Trazodone hydrochloride is a triazolopyridine. It is a white, odorless crystalline powder which is freely soluble in water.
Chemical Name: 2-[3-[4-(3-chlorophenyl)-1-piperazinyl]propyl]-1,2,4-triazolo[4,3-a]pyridin-3(2H)-one hydrochloride
Structural Formula:
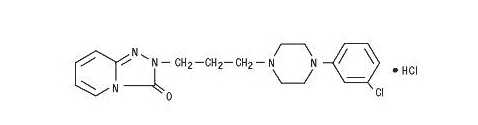
Molecular Formula: C19H22ClN5O HCl
Molecular Weight: 408.32
Each tablet, for oral administration, contains 50 mg, 100 mg, 150 mg or 300 mg of trazodone hydrochloride, USP. In addition, each tablet contains the following inactive ingredients: colloidal silicon dioxide, magnesium stearate, microcrystalline cellulose, pregelatinized starch, sodium lauryl sulfate, and sodium starch glycolate. |PD=Preclinical studies have shown that trazodone selectively inhibits neuronal reuptake of serotonin and acts as an antagonist at 5-HT-2A/2C serotonin receptors.
Trazodone is not a monoamine oxidase inhibitor and, unlike amphetamine-type drugs, does not stimulate the central nervous system.
Trazodone antagonizes alpha 1-adrenergic receptors, a property which may be associated with postural hypotension. |PK=* Absorption
- In humans, trazodone hydrochloride is well absorbed after oral administration without selective localization in any tissue. When trazodone hydrochloride is taken shortly after ingestion of food, there may be an increase in the amount of drug absorbed, a decrease in maximum concentration and a lengthening in the time to maximum concentration. Peak plasma levels occur approximately one hour after dosing when trazodone hydrochloride is taken on an empty stomach or 2 hours after dosing when taken with food.
- Metabolism
- In vitro studies in human liver microsomes show that trazodone is metabolized, via oxidative cleavage, to an active metabolite, m-chlorophenylpiperazine (mCPP) by CYP3A4. Other metabolic pathways that may be involved in the metabolism of trazodone have not been well characterized. Trazodone is extensively metabolized; less than 1% of an oral dose is excreted unchanged in the urine.
- Elimination
- In some patients trazodone may accumulate in the plasma
- Protein Binding
- Trazodone is 89 to 95% protein bound in vitro at concentrations attained with therapeutic doses in humans.
|nonClinToxic=* Carcinogenesis, Mutagenesis, Impairment of Fertility
- No drug- or dose-related occurrence of carcinogenesis was evident in rats receiving trazodone in daily oral doses up to 300 mg/kg for 18 months.
|clinicalStudies=The efficacy and safety of trazodone hydrochloride was established from both inpatient and outpatient trials of the trazodone immediate release formulation in the treatment of major depressive disorder. |howSupplied=Trazodone Hydrochloride Tablets, USP 50 mg are available for oral administration as white to off white, round, biconvex, uncoated tablets debossed with "13" bisect "30" on one side and plain on other side.
Bottles of 30 NDC 13668-330-30
Bottles of 100 NDC 13668-330-01
Bottles of 500 NDC 13668-330-05
Bottles of 1000 NDC 13668-330-10
100 Unit dose Tablets NDC 13668-330-74
Trazodone Hydrochloride Tablets, USP 100 mg are available for oral administration as white to off white, round, biconvex, uncoated tablets debossed with "13" bisect "31" on one side and plain on other side.
Bottles of 30 NDC 13668-331-30
Bottles of 100 NDC 13668-331-01
Bottles of 500 NDC 13668-331-05
Bottles of 1000 NDC 13668-331-10
100 Unit dose Tablets NDC 13668-331-74
Trazodone Hydrochloride Tablets, USP 150 mg are available for oral administration as white to off white, oval, flat faced beveled edge uncoated tablets with a full bisect and two partial trisects. Debossed "13" bisect "32" on one side and "50 50 50" on other side.
Bottles of 30 NDC 13668-332-30
Bottles of 100 NDC 13668-332-01
Bottles of 500 NDC 13668-332-05
Bottles of 1000 NDC 13668-332-10
100 Unit dose Tablets NDC 13668-332-74
Directions for using the correct score when breaking the tablet, please refer to the following:

|storage=Store at 20° to 25°C (68° to 77°F), excursions permitted to 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature].
Dispense in a tight, light-resistant container as defined in the USP using a child-resistant closure. |fdaPatientInfo=* Trazodone Hydrochloride Tablets, USP
- Read the Medication Guide that comes with trazodone hydrochloride tablets before you start taking it and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or treatment. Talk to your healthcare provider or pharmacist if there is something you do not understand or you want to learn about trazodone hydrochloride tablets.
What is the most important information I should know about trazodone hydrochloride?
- Antidepressant medicines, depression or other serious mental illnesses, and suicidal thoughts or actions: Talk to your healthcare provider about:
- All risks and benefits of treatment with antidepressant medicines
- All treatment choices for depression or other serious mental illnesses
- Antidepressant medicines may increase suicidal thoughts or actions in some children, teenagers, and young adults within the first few months of treatment.
- Depression and other serious mental illnesses are the most important causes of suicidal thoughts and actions. Some people may have a higher risk of having suicidal thoughts or actions. These include people who have or have a family history of bipolar illness (also called manic- depressive illness) or suicidal thoughts or actions.
How can I watch for and try to prevent suicidal thoughts and actions?
- Pay close attention to any changes, especially sudden changes in mood, behaviors, thoughts, or feelings. This is very important when an antidepressant medicine is started or when the dose is changed.
- Call your healthcare provider right away to report new or sudden changes in mood, behavior, thoughts or feelings.
- Keep all follow-up visits with your healthcare provider as scheduled. Call your healthcare provider between visits as needed, especially if you are worried about symptoms.
- Call a healthcare provider right away if you have any of the following symptoms, especially if they are new, worse, or worry you:
- Thoughts about suicide or dying
- Attempts to commit suicide
- New or worse depression
- New or worse anxiety
- Feeling very agitated or restless
- Panic attacks
- Trouble sleeping (insomnia)
- New or worse irritability
- Acting aggressive, being angry or violent
- Acting on dangerous impulses
- An extreme increase in activity and talking (mania)
- Other unusual changes in behavior or mood
What else do I need to know about antidepressant medicines?
- Never stop an antidepressant medicine without first talking to a healthcare provider. Stopping an antidepressant medicine suddenly can cause other symptoms.
- Antidepressants are medicines used to treat depression and other illnesses. It is important to discuss all the risks of treating depression and also the risks of not treating it. You should discuss all treatment choices with your healthcare provider, not just the use of antidepressants.
- Antidepressant medicines have other side effects. Talk to your healthcare provider about the side effects of your medicines.
- Antidepressant medicines can interact with other medicines. Know all of the medicines that you take. Keep a list of all medicines to show your healthcare provider. Do not start new medicines without first checking with your healthcare provider.
- Trazodone hydrochloride tablets are not approved for use in children. Talk to your healthcare provider for more information.
=What are trazodone hydrochloride tablets?
- Trazodone hydrochloride tablets are a prescription medicine used to treat major depressive disorder in adults.
- What should I tell my healthcare provider before taking trazodone hydrochloride tablets?
- Before you take trazodone hydrochloride tablets tell your healthcare provider if you:
- Have heart problems, including QT prolongation or a family history of it
- Have ever had a heart attack
- Have bipolar disorder
- Have liver or kidney problems
- Have other serious medical conditions
- Are pregnant or plan to become pregnant. Trazodone hydrochloride tablets may harm your unborn baby. Talk to your healthcare provider if you are pregnant or plan to become pregnant.
- Are breastfeeding or plan to breastfeed. It is not known if trazodone hydrochloride tablets passes into your breast milk. You and your healthcare provider should decide if you will take trazodone hydrochloride tablets or breastfeed.
- Have taken a Monoamine Oxidase Inhibitor (MAOI) or if you have stopped taking an MAOI in the last 2 weeks.
- Tell your healthcare provider about all the medicines you take, including prescription and non-prescription medicines, vitamins, and herbal supplements.
- Using trazodone hydrochloride tablets with certain other medicines can affect each other causing serious side effects.
- Know the medicines you take. Keep a list of them and show it to your healthcare provider and pharmacist when you get a new medicine.
How should I take trazodone hydrochloride tablets?
- Take trazodone hydrochloride tablets exactly as your healthcare provider tells you.
- Trazodone hydrochloride tablets should be taken shortly after a meal or light snack.
- If you feel drowsy after taking trazodone hydrochloride tablets, talk to your healthcare provider. Your healthcare provider may change your dose or the time of day you take your trazodone hydrochloride tablets.
- Do not stop taking trazodone hydrochloride tablets without talking to your healthcare provider.
- Trazodone hydrochloride tablets should be swallowed whole or broken in half along the score line. Do not chew or crush trazodone hydrochloride tablets. Tell your healthcare provider if you cannot swallow trazodone either whole or as a half tablet.
- If you take too much trazodone hydrochloride, call your doctor or go to the nearest emergency room right away.
What should I avoid while taking trazodone hydrochloride tablets?
- Do not drive, operate heavy machinery, or do other dangerous activities until you know how trazodone hydrochloride tablets affects you. Trazodone hydrochloride tablets can slow your thinking and motor skills.
- Do not drink alcohol or take other medicines that make you sleepy or dizzy while taking trazodone hydrochloride tablets until you talk with your healthcare provider. Trazodone hydrochloride tablets may make your sleepiness or dizziness worse if you take it with alcohol or other medicines that cause sleepiness or dizziness.
What are the possible side effects of trazodone hydrochloride tablets?
- Trazodone hydrochloride tablets can cause serious side effects or death. See "What is the most important information I should know about trazodone hydrochloride tablets?"
- Serious side effects include:
- Serotonin syndrome. Symptoms of serotonin syndrome include: agitation, hallucinations, problems with coordination, fast heartbeat, tight muscles, trouble walking, nausea, vomiting, diarrhea.
- Feeling high or in a very good mood, then becoming irritable, or having too much energy, feeling like you have to keep talking or do not sleep (Mania).
- Irregular or fast heartbeat or faint (QT prolongation).
- Low blood pressure. You feel dizzy or faint when you change positions (go from sitting to standing).
- Unusual bruising or bleeding.
- Erection lasting for more than 6 hours (Priapism).
- Low sodium in your blood (Hyponatremia). Symptoms of hyponatremia include: headache, feeling weak, feeling confused, trouble concentrating, memory problems and feeling unsteady when you walk.
- Withdrawal symptoms. Symptoms of withdrawal can include anxiety, agitation, and sleep problems. Do not stop taking trazodone hydrochloride tablets without talking to your healthcare provider.
- Get medical help right away, if you have any of the symptoms listed above.
- The most common side effects of trazodone hydrochloride tablets include:
- Sleepiness
- Dizziness
- Constipation
- Blurry vision
- Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
- These are not all the possible side effects of trazodone hydrochloride tablets. For more information, ask your healthcare provider or pharmacist.
- Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800- FDA-1088.
How should I store trazodone hydrochloride tablets?
- Store trazodone hydrochloride tablets between between 68°F to 77°F (20° C to 25°C).
- Keep in tight container
- Keep out of the light
- Safely throw away medicine that is out of date or no longer needed.
- Keep trazodone hydrochloride tablets and all medicines out of the reach of children.
General information about the safe and effective use of trazodone hydrochloride tablets
- Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use trazodone hydrochloride tablets for a condition for which it was not prescribed. Do not give trazodone hydrochloride tablets to other people, even if they have the same symptoms that you have. It may harm them.
- This Medication Guide summarizes the most important information about trazodone hydrochloride tablets. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about trazodone hydrochloride tablets that is written for health professionals.
- For more information go to www.torrentpharma.com or call 1-800-FDA-1088
What are the ingredients in trazodone hydrochloride tablets?
- Active ingredient: trazodone hydrochloride, USP
- Inactive ingredients: colloidal silicon dioxide, magnesium stearate, microcrystalline cellulose, pregelatinized starch, sodium lauryl sulfate, and sodium starch glycolate.
- This Medication Guide has been approved by the U.S. Food and Drug Administration.
|alcohol=Alcohol-Trazodone interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication. }} {{#subobject:
|Label Page=Trazodone |Label Name=Trazodone label.png
}}