Ranolazine
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sophia Saad, Associate Editor - WikiDoc [2]; Anusha Vege, M.B.B.S. [3]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Ranolazine is an Anti-anginal that is FDA approved for the treatment of treatment of chronic angina.. Common adverse reactions include constipation, nausea , dizziness, headache.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Chronic Angina
- Dosing Information
- initial dosage: 500 mg PO bid
- maximum dosage: 1000 mg PO bid (based on clinical symptoms)s
Dose modification
- Dosing information
- Maximum dosage: 500 mg PO bid in patients on moderate CYP3A inhibitors such as diltiazem, verapamil, and erythromycin.
- Use of Ranexa with strong CYP3A inhibitors is contraindicated.
- Use of P-gp inhibitors, such as cyclosporine, may increase exposure to Ranexa. Titrate Ranexa based on clinical response.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information about Off-Label Guideline-Supported Use of Ranolazine in adult patients.
Non–Guideline-Supported Use
There is limited information about the non–guideline-supported off-label use.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
FDA Package Insert for Ranolazine contains no information regarding FDA-labeled indications and dosage information.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information about Off-Label Guideline-Supported Use of Ranolazine in pediatric patients.
Non–Guideline-Supported Use
There is limited information about Off-Label Non–Guideline-Supported Use of Ranolazine in pediatric patients.
Contraindications
Ranexa is contraindicated in patients:
- Taking strong inhibitors of CYP3A.
- Taking inducers of CYP3A.
- With liver cirrhosis.
Warnings
QT Interval Prolongation
Ranolazine blocks IKr and prolongs the QTc interval in a dose-related manner. Clinical experience in an acute coronary syndrome population did not show an increased risk of proarrhythmia or sudden death. However, there is little experience with high doses (> 1000 mg twice daily) or exposure, other QT-prolonging drugs, potassium channel variants resulting in a long QT interval, in patients with a family history of (or congenital) long QT syndrome, or in patients with known acquired QT interval prolongation.
Renal Failure
Acute renal failure has been observed in some patients with severe renal impairment (creatinine clearance [CrCL] < 30 mL/min) while taking Ranexa. If acute renal failure develops (e.g., marked increase in serum creatinine associated with an increase in blood urea nitrogen [BUN]), discontinue Ranexa and treat appropriately. Monitor renal function after initiation and periodically in patients with moderate to severe renal impairment (CrCL < 60 mL/min) for increases in serum creatinine accompanied by an increase in BUN.
Adverse Reactions
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. A total of 2,018 patients with chronic angina were treated with ranolazine in controlled clinical trials. Of the patients treated with Ranexa, 1,026 were enrolled in three double-blind, placebo-controlled, randomized studies (CARISA, ERICA, MARISA) of up to 12 weeks' duration. In addition, upon study completion, 1,251 patients received treatment with Ranexa in open-label, long-term studies; 1,227 patients were exposed to Ranexa for more than 1 year, 613 patients for more than 2 years, 531 patients for more than 3 years, and 326 patients for more than 4 years. At recommended doses, about 6% of patients discontinued treatment with Ranexa because of an adverse event in controlled studies in angina patients compared to about 3% on placebo. The most common adverse events that led to discontinuation more frequently on Ranexa than placebo were dizziness (1.3% versus 0.1%), nausea (1% versus 0%), asthenia, constipation, and headache (each about 0.5% versus 0%). Doses above 1000 mg twice daily are poorly tolerated. In controlled clinical trials of angina patients, the most frequently reported treatment-emergent adverse reactions (> 4% and more common on Ranexa than on placebo) were dizziness(6.2%), headache (5.5%), constipation(4.5%), and nausea (4.4%). Dizziness may be dose-related. In open-label, long-term treatment studies, a similar adverse reaction profile was observed. The following additional adverse reactions occurred at an incidence of 0.5 to 4.0% in patients treated with Ranexa and were more frequent than the incidence observed in placebo-treated patients:
- Cardiac Disorders – bradycardia, palpitations
- Ear and Labyrinth Disorders – tinnitus, vertigo
- Eye Disorders – blurred vision
- Gastrointestinal Disorders – abdominal pain, dry mouth, vomiting, dyspepsia
- General Disorders and Administrative Site Adverse Events – asthenia, peripheral edema
- Metabolism and Nutrition Disorders – anorexia
- Nervous System Disorders – syncope (vasovagal)
- Psychiatric Disorders – confusional state
- Renal and Urinary Disorders – hematuria
- Respiratory, Thoracic, and Mediastinal Disorders – dyspnea
- Skin and Subcutaneous Tissue Disorders – hyperhidrosis
- Vascular Disorders – hypotension, orthostatic hypotension
- Other (< 0.5%) but potentially medically important adverse reactions observed more frequently with Ranexa than placebo treatment in all controlled studies included: angioedema, renal failure, eosinophilia, chromaturia, blood urea increased, hypoesthesia, paresthesia, tremor, pulmonary fibrosis, thrombocytopenia, leukopenia, and pancytopenia.
A large clinical trial in acute coronary syndrome patients was unsuccessful in demonstrating a benefit for Ranexa, but there was no apparent proarrhythmic effect in these high-risk patients.
Laboratory Abnormalities
Ranexa produces small reductions in hemoglobin A1c. Ranexa is not a treatment for diabetes. Ranexa produces elevations of serum creatinine by 0.1 mg/dL, regardless of previous renal function, likely because of inhibition of creatinine's tubular secretion. In general, the elevation has a rapid onset, shows no signs of progression during long-term therapy, is reversible after discontinuation of Ranexa, and is not accompanied by changes in BUN. In healthy volunteers, Ranexa 1000 mg twice daily had no effect upon the glomerular filtration rate. More marked and progressive increases in serum creatinine, associated with increases in BUN or potassium, indicating acute renal failure, have been reported after initiation of Ranexa in patients with severe renal impairment.
Postmarketing Experience
The following adverse reactions have been identified during postapproval use of Ranexa. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure:
- Nervous System Disorders : Tremor, paresthesia, abnormal coordination, and other serious neurologic adverse events have been reported to occur, sometimes concurrently, in patients taking ranolazine. The onset of events was often associated with an increase in ranolazine dose or exposure. Many patients reported symptom resolution following drug discontinuation or dose decrease.
- Psychiatric Disorders – hallucination
- Renal and Urinary Disorders – dysuria, urinary retention
- Skin and Subcutaneous Tissue Disorders – angioedema, pruritus, rash
Drug Interactions
Effects of Other Drugs on Ranolazine
- Strong CYP3A Inhibitors
- Do not use Ranexa with strong CYP3A inhibitors, including ketoconazole, itraconazole, clarithromycin, nefazodone, nelfinavir, ritonavir, indinavir, and saquinavir.
- Moderate CYP3A Inhibitors
- Limit the dose of Ranexa to 500 mg twice daily in patients on moderate CYP3A inhibitors, including diltiazem, verapamil, erythromycin, fluconazole, and grapefruit juice or grapefruit-containing products.
- P-gp Inhibitors
- Concomitant use of Ranexa and P-gp inhibitors, such as cyclosporine, may result in increases in ranolazine concentrations. Titrate Ranexa based on clinical response in patients concomitantly treated with predominant P-gp inhibitors such as cyclosporine.
- CYP3A Inducers
- Do not use Ranexa with CYP3A inducers such as rifampin, rifabutin, rifapentine, phenobarbital, phenytoin, carbamazepine, and St. John's wort.
Effects of Ranolazine on Other Drugs
- Drugs Metabolized by CYP3A
- Limit the dose of simvastatin in patients on any dose of Ranexa to 20 mg once daily, when ranolazine is co-administered. Dose adjustment of other sensitive CYP3A substrates (e.g., lovastatin) and CYP3A substrates with a narrow therapeutic range (e.g., cyclosporine, tacrolimus, sirolimus ) may be required as Ranexa may increase plasma concentrations of these drugs.
- Drugs Transported by P-gp
- Drugs Metabolized by CYP2D6
- The exposure to CYP2D6 substrates, such as tricyclic antidepressants and antipsychotics, may be increased during co-administration with Ranexa, and lower doses of these drugs may be required.
- Drugs Transported by OCT2
- In subjects with type 2 diabetes mellitus, concomitant use of Ranexa 1000 mg twice daily and metformin results in increased plasma levels of metformin. When Ranexa 1000 mg twice daily is co-administered with metformin, metformin dose should not exceed 1700 mg/day. Monitor blood glucose levels and risks associated with high exposures of metformin. Metformin exposure was not significantly increased when given with Ranexa 500 mg twice daily.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): C
In animal studies, ranolazine at exposures 1.5 (rabbit) to 2 (rat) times the usual human exposure caused maternal toxicity and misshapen sternebrae and reduced ossification in offspring. These doses in rats and rabbits were associated with an increased maternal mortality rate. There are no adequate well-controlled studies in pregnant women. Ranexa should be used during pregnancy only when the potential benefit to the patient justifies the potential risk to the fetus.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Ranolazine in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Ranolazine during labor and delivery.
Nursing Mothers
It is not known whether ranolazine is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions from ranolazine in nursing infants, decide whether to discontinue nursing or to discontinue Ranexa, taking into account the importance of the drug to the mother.
Pediatric Use
Safety and effectiveness have not been established in pediatric patients.
Geriatic Use
Of the chronic angina patients treated with Ranexa in controlled studies, 496 (48%) were ≥ 65 years of age, and 114 (11%) were ≥ 75 years of age. No overall differences in efficacy were observed between older and younger patients. There were no differences in safety for patients ≥ 65 years compared to younger patients, but patients ≥ 75 years of age on Ranexa, compared to placebo, had a higher incidence of adverse events, serious adverse events, and drug discontinuations due to adverse events. In general, dose selection for an elderly patient should usually start at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease, or other drug therapy.
Gender
There is no FDA guidance on the use of Ranolazine with respect to specific gender populations.
Race
There is no FDA guidance on the use of Ranolazine with respect to specific racial populations.
Renal Impairment
A pharmacokinetic study of Ranexa in subjects with severe renal impairment (CrCL < 30 mL/min) was stopped when 2 of 4 subjects developed acute renal failure after receiving Ranexa 500 mg twice daily for 5 days (lead-in phase) followed by 1000 mg twice a day (1 dose in one subject and 11 doses in the other). Increases in creatinine, BUN, and potassium were observed in 3 subjects during the 500 mg lead-in phase. One subject required hemodialysis, while the other 2 subjects improved upon drug discontinuation. Monitor renal function periodically in patients with moderate to severe renal impairment. Discontinue Ranexa if acute renal failure develops. In a separate study, Cmax was increased between 40% and 50% in patients with mild, moderate or severe renal impairment compared to patients with no renal impairment, suggesting a similar increase in exposure in patients with renal failure independent of the degree of impairment. The pharmacokinetics of ranolazine has not been assessed in patients on dialysis.
Hepatic Impairment
Ranexa is contraindicated in patients with liver cirrhosis. In a study of cirrhotic patients, the Cmax of ranolazine was increased 30% in cirrhotic patients with mild (Child-Pugh Class A) hepatic impairment, but increased 80% in cirrhotic patients with moderate (Child-Pugh Class B) hepatic impairment compared to patients without hepatic impairment. This increase was not enough to account for the 3-fold increase in QT prolongation seen in cirrhotic patients with mild to moderate hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Ranolazine in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Ranolazine in patients who are immunocompromised.
Use in Patients with Heart Failure
Heart failure (NYHA Class I to IV) had no significant effect on ranolazine pharmacokinetics. Ranexa had minimal effects on heart rate and blood pressure in patients with angina and heart failure NYHA Class I to IV. No dose adjustment of Ranexa is required in patients with heart failure.
Use in Patients with Diabetes Mellitus
A population pharmacokinetic evaluation of data from angina patients and healthy subjects showed no effect of diabetes on ranolazine pharmacokinetics. No dose adjustment is required in patients with diabetes. Ranexa produces small reductions in HbA1c in patients with diabetes, the clinical significance of which is unknown. Ranexa should not be considered a treatment for diabetes.
Administration and Monitoring
Administration
Dosing Information
Initiate Ranexa dosing at 500 mg twice daily and increase to 1000 mg twice daily, as needed, based on clinical symptoms. Take Ranexa with or without meals. Swallow Ranexa tablets whole; do not crush, break, or chew. The maximum recommended daily dose of Ranexa is 1000 mg twice daily. If a dose of Ranexa is missed, take the prescribed dose at the next scheduled time; do not double the next dose.
Dose Modification
Dose adjustments may be needed when Ranexa is taken in combination with certain other drugs. Limit the maximum dose of Ranexa to 500 mg twice daily in patients on moderate CYP3A inhibitors such as diltiazem, verapamil, and erythromycin. Use of Ranexa with strong CYP3A inhibitors is contraindicated. Use of P-gp inhibitors, such as cyclosporine, may increase exposure to Ranexa. Titrate Ranexa based on clinical response.
Monitoring
- Monitor renal function after initiation and periodically in patients with moderate to severe renal impairment (CrCL < 60 mL/min) for increases in serum creatinine accompanied by an increase in BUN.
- Monitor blood glucose levels and risks associated with high exposures of metformin.
- Monitor renal function periodically in patients with moderate to severe renal impairment.
- In addition to general supportive measures, continuous ECG monitoring may be warranted in the event of overdose.
IV Compatibility
FDA Package Insert for Ranolazine contains no information regarding IV Compatibility.
Overdosage
High oral doses of ranolazine produce dose-related increases in dizziness, nausea, and vomiting. High intravenous exposure also produces diplopia, paresthesia, confusion, and syncope. In addition to general supportive measures, continuous ECG monitoring may be warranted in the event of overdose. Severe tremor, unsteady gait/incoordination, dysphasia, and hallucinations have been reported in cases of overdose with Ranexa. Since ranolazine is about 62% bound to plasma proteins, hemodialysis is unlikely to be effective in clearing ranolazine.
Pharmacology
Mechanism of Action
The mechanism of action of ranolazine's antianginal effects has not been determined. Ranolazine has anti-ischemic and antianginal effects that do not depend upon reductions in heart rate or blood pressure. It does not affect the rate-pressure product, a measure of myocardial work, at maximal exercise. Ranolazine at therapeutic levels can inhibit the cardiac late sodium current (INa). However, the relationship of this inhibition to angina symptoms is uncertain. The QT prolongation effect of ranolazine on the surface electrocardiogram is the result of inhibition of IKr, which prolongs the ventricular action potential.
Structure
Ranexa (ranolazine) is available as a film-coated, non-scored, extended-release tablet for oral administration. Ranolazine is a racemic mixture, chemically described as 1-piperazineacetamide, N-(2,6-dimethylphenyl)-4-[2-hydroxy-3-(2-methoxyphenoxy)propyl]-, (±)-. It has an empirical formula of C24H33N3O4, a molecular weight of 427.54 g/mole, and the following structural formula:
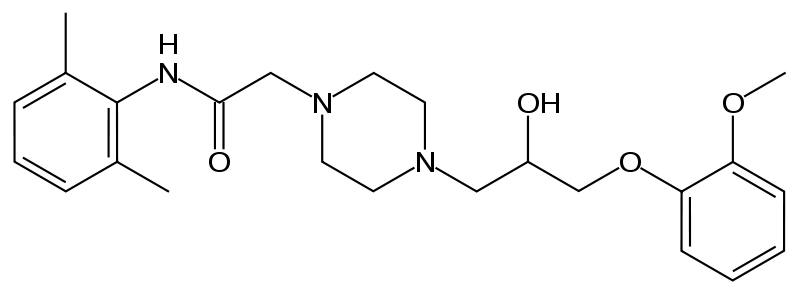
Ranolazine is a white to off-white solid. Ranolazine is soluble in dichloromethane and methanol; sparingly soluble in tetrahydrofuran, ethanol, acetonitrile, and acetone; slightly soluble in ethyl acetate, isopropanol, toluene, and ethyl ether; and very slightly soluble in water. Ranexa tablets contain 500 mg or 1000 mg of ranolazine and the following inactive ingredients: carnauba wax, hypromellose, magnesium stearate, methacrylic acid copolymer (Type C), microcrystalline cellulose, polyethylene glycol, sodium hydroxide, and titanium dioxide. Additional inactive ingredients for the 500 mg tablet include polyvinyl alcohol, talc, Iron Oxide Yellow, and Iron Oxide Red; additional inactive ingredients for the 1000 mg tablet include lactose monohydrate, triacetin, and Iron Oxide Yellow.
Pharmacodynamics
Hemodynamic Effects
Patients with chronic angina treated with Ranexa in controlled clinical studies had minimal changes in mean heart rate (< 2 bpm) and systolic blood pressure (< 3 mm Hg). Similar results were observed in subgroups of patients with CHF NYHA Class I or II, diabetes, or reactive airway disease, and in elderly patients.
Electrocardiographic Effects
Dose and plasma concentration-related increases in the QTc interval, reductions in T wave amplitude, and, in some cases, notched T waves, have been observed in patients treated with Ranexa. These effects are believed to be caused by ranolazine and not by its metabolites. The relationship between the change in QTc and ranolazine plasma concentrations is linear, with a slope of about 2.6 msec/1000 ng/mL, through exposures corresponding to doses several-fold higher than the maximum recommended dose of 1000 mg twice daily. The variable blood levels attained after a given dose of ranolazine give a wide range of effects on QTc. At Tmax following repeat dosing at 1000 mg twice daily, the mean change in QTc is about 6 msec, but in the 5% of the population with the highest plasma concentrations, the prolongation of QTc is at least 15 msec. In cirrhotic subjects with mild or moderate hepatic impairment, the relationship between plasma level of ranolazine and QTc is much steeper. Age, weight, gender, race, heart rate, congestive heart failure, diabetes, and renal impairment did not alter the slope of the QTc-concentration relationship of ranolazine. No proarrhythmic effects were observed on 7-day Holter recordings in 3,162 acute coronary syndrome patients treated with Ranexa. There was a significantly lower incidence of arrhythmias (ventricular tachycardia, bradycardia, supraventricular tachycardia, and new atrial fibrillation) in patients treated with Ranexa (80%) versus placebo (87%), including ventricular tachycardia ≥ 3 beats (52% versus 61%). However, this difference in arrhythmias did not lead to a reduction in mortality, a reduction in arrhythmia hospitalization, or a reduction in arrhythmia symptoms.
Pharmacokinetics
Ranolazine is extensively metabolized in the gut and liver and its absorption is highly variable. For example, at a dose of 1000 mg twice daily, the mean steady-state Cmax was 2600 ng/mL with 95% confidence limits of 400 and 6100 ng/mL. The pharmacokinetics of the (+) R- and (-) S-enantiomers of ranolazine are similar in healthy volunteers. The apparent terminal half-life of ranolazine is 7 hours. Steady state is generally achieved within 3 days of twice-daily dosing with Ranexa. At steady state over the dose range of 500 to 1000 mg twice daily, Cmax and AUC0–τ increase slightly more than proportionally to dose, 2.2- and 2.4-fold, respectively. With twice-daily dosing, the trough:peak ratio of the ranolazine plasma concentration is 0.3 to 0.6. The pharmacokinetics of ranolazine is unaffected by age, gender, or food.
Absorption and Distribution
After oral administration of Ranexa, peak plasma concentrations of ranolazine are reached between 2 and 5 hours. After oral administration of 14C-ranolazine as a solution, 73% of the dose is systemically available as ranolazine or metabolites. The bioavailability of ranolazine from Ranexa tablets relative to that from a solution of ranolazine is 76%. Because ranolazine is a substrate of P-gp, inhibitors of P-gp may increase the absorption of ranolazine. Food (high-fat breakfast) has no important effect on the Cmax and AUC of ranolazine. Therefore, Ranexa may be taken without regard to meals. Over the concentration range of 0.25 to 10 µg/mL, ranolazine is approximately 62% bound to human plasma proteins.
Metabolism and Excretion
Ranolazine is metabolized mainly by CYP3A and, to a lesser extent, by CYP2D6. Following a single oral dose of ranolazine solution, approximately 75% of the dose is excreted in urine and 25% in feces. Ranolazine is metabolized rapidly and extensively in the liver and intestine; less than 5% is excreted unchanged in urine and feces. The pharmacologic activity of the metabolites has not been well characterized. After dosing to steady state with 500 mg to 1500 mg twice daily, the four most abundant metabolites in plasma have AUC values ranging from about 5 to 33% that of ranolazine, and display apparent half-lives ranging from 6 to 22 hours.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
Ranolazine tested negative for genotoxic potential in the following assays: Ames bacterial mutation assay, Saccharomyces assay for mitotic gene conversion, chromosomal aberrations assay in Chinese hamster ovary (CHO) cells, mammalian CHO/HGPRT gene mutation assay, and mouse and rat bone marrow micronucleus assays. There was no evidence of carcinogenic potential in mice or rats. The highest oral doses used in the carcinogenicity studies were 150 mg/kg/day for 21 months in rats (900 mg/m2/day) and 50 mg/kg/day for 24 months in mice (150 mg/m2/day). These maximally tolerated doses are 0.8 and 0.1 times, respectively, the maximum recommended human dose (MRHD) of 2 grams on a surface area basis. A published study reported that ranolazine promoted tumor formation and progression to malignancy when given to transgenic APC (min/+) mice at a dose of 30 mg/kg twice daily. The clinical significance of this finding is unclear.
Reproductive Toxicology Studies
Animal reproduction studies with ranolazine were conducted in rats and rabbits. There was an increased incidence of misshapen sternebrae and reduced ossification of pelvic and cranial bones in fetuses of pregnant rats dosed at 400 mg/kg/day (2 times the MRHD on a surface area basis). Reduced ossification of sternebrae was observed in fetuses of pregnant rabbits dosed at 150 mg/kg/day (1.5 times the MRHD on a surface area basis). These doses in rats and rabbits were associated with an increased maternal mortality rate.
Clinical Studies
Chronic Stable Angina
CARISA (Combination Assessment of Ranolazine In Stable Angina) was a study in 823 chronic angina patients randomized to receive 12 weeks of treatment with twice-daily Ranexa 750 mg, 1000 mg, or placebo, who also continued on daily doses of atenolol 50 mg, amlodipine 5 mg, or diltiazem CD 180 mg. Sublingual nitrates were used in this study as needed. In this trial, statistically significant (p < 0.05) increases in modified Bruce treadmill exercise duration and time to angina were observed for each Ranexa dose versus placebo, at both trough (12 hours after dosing) and peak (4 hours after dosing) plasma levels, with minimal effects on blood pressure and heart rate. The changes versus placebo in exercise parameters are presented in Table 1. Exercise treadmill results showed no increase in effect on exercise at the 1000 mg dose compared to the 750 mg dose.

The effects of Ranexa on angina frequency and nitroglycerin use are shown in Table 2.

Tolerance to Ranexa did not develop after 12 weeks of therapy. Rebound increases in angina, as measured by exercise duration, have not been observed following abrupt discontinuation of Ranexa. Ranexa has been evaluated in patients with chronic angina who remained symptomatic despite treatment with the maximum dose of an antianginal agent. In the ERICA (Efficacy of Ranolazine In Chronic Angina) trial, 565 patients were randomized to receive an initial dose of Ranexa 500 mg twice daily or placebo for 1 week, followed by 6 weeks of treatment with Ranexa 1000 mg twice daily or placebo, in addition to concomitant treatment with amlodipine 10 mg once daily. In addition, 45% of the study population also received long-acting nitrates. Sublingual nitrates were used as needed to treat angina episodes. Results are shown in Table 3. Statistically significant decreases in angina attack frequency (p = 0.028) and nitroglycerin use (p = 0.014) were observed with Ranexa compared to placebo. These treatment effects appeared consistent across age and use of long-acting nitrates.

Gender
Effects on angina frequency and exercise tolerance were considerably smaller in women than in men. In CARISA, the improvement in Exercise Tolerance Test (ETT) in females was about 33% of that in males at the 1000 mg twice-daily dose level. In ERICA, where the primary endpoint was angina attack frequency, the mean reduction in weekly angina attacks was 0.3 for females and 1.3 for males.
Race
There were insufficient numbers of non-Caucasian patients to allow for analyses of efficacy or safety by racial subgroup. 14.2 Lack of Benefit in Acute Coronary Syndrome In a large (n = 6,560) placebo-controlled trial (MERLIN-TIMI 36) in patients with acute coronary syndrome, there was no benefit shown on outcome measures. However, the study is somewhat reassuring regarding proarrhythmic risks, as ventricular arrhythmias were less common on ranolazine and there was no difference between Ranexa and placebo in the risk of all-cause mortality (relative risk ranolazine:placebo 0.99 with an upper 95% confidence limit of 1.22).
How Supplied
Ranexa is supplied as film-coated, oblong-shaped, extended-release tablets in the following strengths:
- 500 mg tablets are light orange, with GSI500 on one side
- 1000 mg tablets are pale yellow, with GSI1000 on one side
Ranexa (ranolazine) extended-release tablets are available in:

Storage
Store Ranexa tablets at 25°C (77°F) with excursions permitted to 15° to 30°C (59° to 86°F).
Images
Drug Images
{{#ask: Page Name::Ranolazine |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Ranolazine |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
To ensure safe and effective use of Ranexa, the following information and instructions should be communicated to the patient when appropriate. Patients should be advised:
- that Ranexa will not abate an acute angina episode
- to inform their physician of any other medications when taken concurrently with Ranexa, including over-the-counter medications
- that Ranexa may produce changes in the electrocardiogram (QTc interval prolongation)
- to inform their physician of any personal or family history of QTc prolongation, congenital long QT syndrome, or if they are receiving drugs that prolong the QTc interval such as Class Ia (e.g., quinidine) or Class III (e.g., dofetilide, sotalol, amiodarone) antiarrhythmic agents, erythromycin, and certain antipsychotics (e.g., thioridazine, ziprasidone)
- to inform their physician if they have impaired renal function before or while taking Ranexa
- that patients with severe renal impairment may be at risk of renal failure while on Ranexa
- that Ranexa should not be used in patients who are receiving drugs that are strong CYP3A inhibitors (e.g., ketoconazole, clarithromycin, nefazodone, ritonavir)
- that initiation of treatment with Ranexa should be avoided during administration of inducers of CYP3A (e.g., rifampin, rifabutin, rifapentine, barbiturates, carbamazepine, phenytoin, St. John's wort)
- to inform their physician if they are receiving drugs that are moderate CYP3A inhibitors (e.g., diltiazem, verapamil, erythromycin)
- to inform their physician if they are receiving P-gp inhibitors (e.g., cyclosporine)
- that grapefruit juice or grapefruit products should be limited when taking Ranexa
- that Ranexa should not be used in patients with liver cirrhosis
- that doses of Ranexa higher than 1000 mg twice daily should not be used
- that if a dose is missed, the usual dose should be taken at the next scheduled time. The next dose should not be doubled
- that Ranexa may be taken with or without meals
- that Ranexa tablets should be swallowed whole and not crushed, broken, or chewed
- to contact their physician if they experience fainting spells while taking Ranexa
- that Ranexa may cause dizziness and lightheadedness; therefore, patients should know how they react to this drug before they operate an automobile, or machinery, or engage in activities requiring mental alertness or coordination
Precautions with Alcohol
Alcohol-Ranolazine interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
Ranexa
Look-Alike Drug Names
There is limited information about the Look-Alike Drug Names.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Page Name=Ranolazine |Pill Name=Ranolazine 1000 mg NDC 61958-1004.jpg |Drug Name=Ranolazine |Pill Ingred=carnauba wax, hypromelloses, magnesium stearate, methacrylic acid - ethyl acrylate copolymer (1:1) type a, cellulose, microcrystalline, sodium hydroxide, polyvinyl alcohol, titanium dioxide, polyethylene glycol 3350, talc, ferric oxide yellow, ferric oxide red, water|+sep=; |Pill Imprint=Ranolazine 1000 mg NDC 61958-1004.jpg |Pill Dosage=1000 mg |Pill Color=Yellow|+sep=; |Pill Shape=Oval |Pill Size (mm)=21.00 |Pill Scoring=1 |Pill Image= |Drug Author=Gilead Sciences, Inc. |NDC=61958-1004
}}
{{#subobject:
|Page Name=Ranolazine |Pill Name=Ranolazine 500 mg NDC 61958-1003.jpg |Drug Name=Ranolazine |Pill Ingred=carnauba wax, hypromelloses, magnesium stearate, methacrylic acid - ethyl acrylate copolymer (1:1) type a, cellulose, microcrystalline, sodium hydroxide, polyvinyl alcohol, titanium dioxide, polyethylene glycol 3350, talc, ferric oxide yellow, ferric oxide red, water|+sep=; |Pill Imprint=GSI500 |Pill Dosage=500 mg |Pill Color=Orange|+sep=; |Pill Shape=Round |Pill Size (mm)=17.00 |Pill Scoring=1 |Pill Image= |Drug Author=Gilead Sciences, Inc. |NDC=61958-1003
}}
{{#subobject:
|Label Page=Ranolazine |Label Name=Ranolazine_label_01.jpg
}}
{{#subobject:
|Label Page=Ranolazine |Label Name=Ranolazine_label_02.jpg
}}
{{#subobject:
|Label Page=Ranolazine |Label Name=Ranolazine_panel_01.jpg
}}
{{#subobject:
|Label Page=Ranolazine |Label Name=Ranolazine_panel_02.jpg
}}