Ocrelizumab
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Yashasvi Aryaputra[2];
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Ocrelizumab is a CD20-directed cytolytic antibody that is FDA approved for the treatment of relapsing or primary progressive forms of multiple sclerosis. Common adverse reactions include upper respiratory tract infections, infusion reactions, skin infections, and lower respiratory tract infections.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Indications:
- Ocrelizumab is indicated for the treatment of adult patients with relapsing or primary progressive forms of multiple sclerosis.
Recommended Dosage and Dose Administration
- Administer Ocrelizumab under the close supervision of an experienced healthcare professional with access to appropriate medical support to manage severe reactions such as serious infusion reactions.
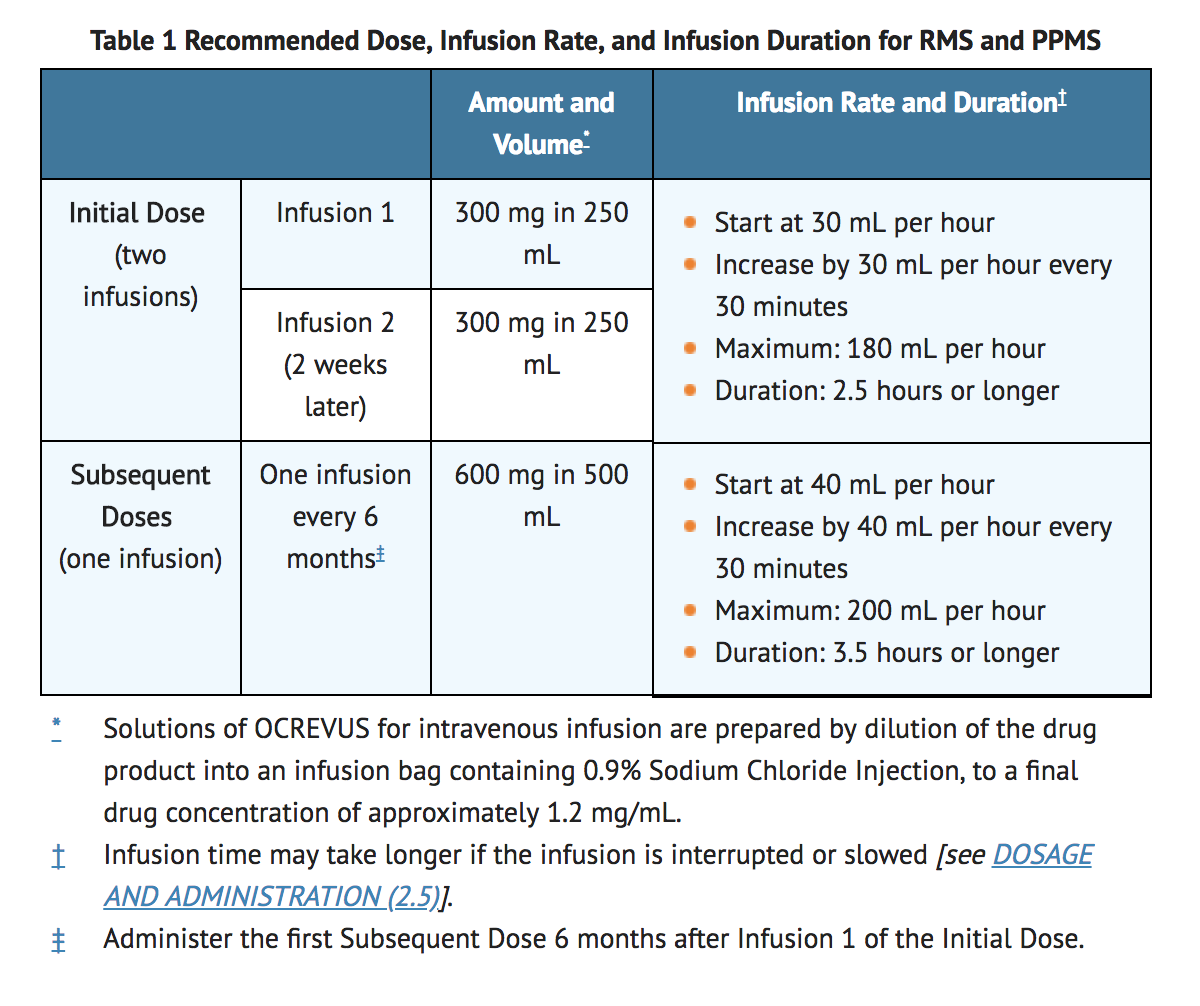
- Initial dose: 300 mg intravenous infusion, followed two weeks later by a second 300 mg intravenous infusion.
- Subsequent doses: single 600 mg intravenous infusion every 6 months.
- Observe the patient for at least one hour after the completion of the infusion.
Delayed or Missed Doses
- If a planned infusion of Ocrelizumab is missed, administer Ocrelizumab as soon as possible; do not wait until the next scheduled dose. Reset the dose schedule to administer the next sequential dose 6 months after the missed dose is administered. Doses of Ocrelizumab must be separated by at least 5 months.
Dose Modifications Because of Infusion Reactions
- Dose modifications in response to infusion reactions depends on the severity.
Life-threatening Infusion Reactions
- Immediately stop and permanently discontinue Ocrelizumab if there are signs of a life-threatening or disabling infusion reaction. Provide appropriate supportive treatment.
Severe Infusion Reactions
- Immediately interrupt the infusion and administer appropriate supportive treatment, as necessary. Restart the infusion only after all symptoms have resolved. When restarting, begin at half of the infusion rate at the time of onset of the infusion reaction. If this rate is tolerated, increase the rate as described in TABLE 1. This change in rate will increase the total duration of the infusion but not the total dose.
Mild to Moderate Infusion Reactions
- Reduce the infusion rate to half the rate at the onset of the infusion reaction and maintain the reduced rate for at least 30 minutes. If this rate is tolerated, increase the rate as described in TABLE 1. This change in rate will increase the total duration of the infusion but not the total dose.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Ocrelizumab Off-Label Guideline-Supported Use and Dosage (Adult) in the drug label.
Non–Guideline-Supported Use
There is limited information regarding Ocrelizumab Off-Label Non-Guideline-Supported Use and Dosage (Adult) in the drug label.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding Ocrelizumab FDA-Labeled Indications and Dosage (Pediatric) in the drug label.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Ocrelizumab Off-Label Guideline-Supported Use and Dosage (Pediatric) in the drug label.
Non–Guideline-Supported Use
There is limited information regarding Ocrelizumab Off-Label Non-Guideline-Supported Use and Dosage (Pediatric) in the drug label.
Contraindications
- Ocrelizumab is contraindicated in patients with:
- Active HBV infection.
- A history of life-threatening infusion reaction to Ocrelizumab.
Warnings
Infusion Reactions
- Ocrelizumab can cause infusion reactions, which can include pruritus, rash, urticaria, erythema, bronchospasm, throat irritation, oropharyngeal pain, dyspnea, pharyngeal or laryngeal edema, flushing, hypotension, pyrexia, fatigue, headache, dizziness, nausea, and tachycardia. In multiple sclerosis (MS) clinical trials, the incidence of infusion reactions in Ocrelizumab-treated patients [who received methylprednisolone (or an equivalent steroid) and possibly other pre-medication to reduce the risk of infusion reactions prior to each infusion] was 34 to 40%, with the highest incidence with the first infusion. There were no fatal infusion reactions, but 0.3% of Ocrelizumab-treated MS patients experienced infusion reactions that were serious, some requiring hospitalization.
- Observe patients treated with Ocrelizumab for infusion reactions during the infusion and for at least one hour after completion of the infusion. Inform patients that infusion reactions can occur up to 24 hours after the infusion.
Reducing the Risk of Infusion Reactions and Managing Infusion Reactions
- Administer pre-medication (e.g., methylprednisolone or an equivalent corticosteroid, and an antihistamine) to reduce the frequency and severity of infusion reactions. The addition of an antipyretic (e.g., acetaminophen) may also be considered.
- Management recommendations for infusion reactions depend on the type and severity of the reaction. For life-threatening infusion reactions, immediately and permanently stop Ocrelizumab and administer appropriate supportive treatment. For less severe infusion reactions, management may involve temporarily stopping the infusion, reducing the infusion rate, and/or administering symptomatic treatment.
Infections
- A higher proportion of Ocrelizumab-treated patients experienced infections compared to patients taking REBIF or placebo. In RMS trials, 58% of Ocrelizumab-treated patients experienced one or more infections compared to 52% of REBIF-treated patients. In the PPMS trial, 70% of Ocrelizumab-treated patients experienced one or more infections compared to 68% of patients on placebo. Ocrelizumab increased the risk for upper respiratory tract infections, lower respiratory tract infections, skin infections, and herpes-related infections. Ocrelizumab was not associated with an increased risk of serious infections in MS patients. Delay Ocrelizumab administration in patients with an active infection until the infection is resolved.
Respiratory Tract Infections
- A higher proportion of Ocrelizumab-treated patients experienced respiratory tract infections compared to patients taking REBIF or placebo. In RMS trials, 40% of Ocrelizumab-treated patients experienced upper respiratory tract infections compared to 33% of REBIF-treated patients, and 8% of Ocrelizumab-treated patients experienced lower respiratory tract infections compared to 5% of REBIF-treated patients. In the PPMS trial, 49% of Ocrelizumab-treated patients experienced upper respiratory tract infections compared to 43% of patients on placebo and 10% of Ocrelizumab-treated patients experienced lower respiratory tract infections compared to 9% of patients on placebo. The infections were predominantly mild to moderate and consisted mostly of upper respiratory tract infections and bronchitis.
Herpes
- In active-controlled (RMS) clinical trials, herpes infections were reported more frequently in Ocrelizumab-treated patients than in REBIF-treated patients, including herpes zoster (2.1% vs. 1.0%), herpes simplex (0.7% vs. 0.1%), oral herpes (3.0% vs. 2.2%), genital herpes (0.1% vs. 0%), and herpes virus infection (0.1% vs. 0%). Infections were predominantly mild to moderate in severity. There were no reports of disseminated herpes.
- In the placebo-controlled (PPMS) clinical trial, oral herpes was reported more frequently in the Ocrelizumab-treated patients than in the patients on placebo (2.7% vs 0.8%).
Progressive Multifocal Leukoencephalopathy (PML)
- PML is an opportunistic viral infection of the brain caused by the John Cunningham (JC) virus that typically only occurs in patients who are immunocompromised, and that usually leads to death or severe disability. Although no cases of PML were identified in Ocrelizumab clinical trials, JC virus infection resulting in PML has been observed in patients treated with other anti-CD20 antibodies and other MS therapies and has been associated with some risk factors (e.g., immunocompromised patients, polytherapy with immunosuppressants). At the first sign or symptom suggestive of PML, withhold Ocrelizumab and perform an appropriate diagnostic evaluation. MRI findings may be apparent before clinical signs or symptoms. Typical symptoms associated with PML are diverse, progress over days to weeks, and include progressive weakness on one side of the body or clumsiness of limbs, disturbance of vision, and changes in thinking, memory, and orientation leading to confusion and personality changes.
Hepatitis B Virus (HBV) Reactivation
- There were no reports of hepatitis B reactivation in MS patients treated with Ocrelizumab. Fulminant hepatitis, hepatic failure, and death caused by HBV reactivation have occurred in patients treated with other anti-CD20 antibodies. Perform HBV screening in all patients before initiation of treatment with Ocrelizumab. Do not administer Ocrelizumab to patients with active HBV confirmed by positive results for HBsAg and anti-HB tests. For patients who are negative for surface antigen [HBsAg] and positive for HB core antibody [HBcAb+] or are carriers of HBV [HBsAg+], consult liver disease experts before starting and during treatment.
Possible Increased Risk of Immunosuppressant Effects with Other Immunosuppressants
- When initiating Ocrelizumab after an immunosuppressive therapy or initiating an immunosuppressive therapy after Ocrelizumab, consider the potential for increased immunosuppressive effects. Ocrelizumab has not been studied in combination with other MS therapies.
Vaccinations
- Administer all immunizations according to immunization guidelines at least 6 weeks prior to initiation of Ocrelizumab.
- The safety of immunization with live or live-attenuated vaccines following Ocrelizumab therapy has not been studied, and vaccination with live-attenuated or live vaccines is not recommended during treatment and until B-cell repletion.
- No data are available on the effects of live or non-live vaccination in patients receiving Ocrelizumab.
Malignancies
- An increased risk of malignancy with Ocrelizumab may exist. In controlled trials, malignancies, including breast cancer, occurred more frequently in Ocrelizumab-treated patients. Breast cancer occurred in 6 of 781 females treated with Ocrelizumab and none of 668 females treated with REBIF or placebo. Patients should follow standard breast cancer screening guidelines.
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reactions rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
- The safety of Ocrelizumab has been evaluated in 1311 patients across MS clinical studies, which included 825 patients in active-controlled clinical trials in patients with relapsing forms of MS (RMS) and 486 patients in a placebo-controlled study in patients with primary progressive MS (PPMS).
Adverse Reactions in Patients with Relapsing Forms of MS
- In active-controlled clinical trials (Study 1 and Study 2), 825 patients with RMS received Ocrelizumab 600 mg intravenously every 24 weeks (initial treatment was given as two separate 300 mg infusions at Weeks 0 and 2). The overall exposure in the 96-week controlled treatment periods was 1448 patient-years.
- The most common adverse reactions in RMS trials (incidence ≥ 10%) were upper respiratory tract infections and infusion reactions. TABLE 2 summarizes the adverse reactions that occurred in RMS trials (Study 1 and Study 2).
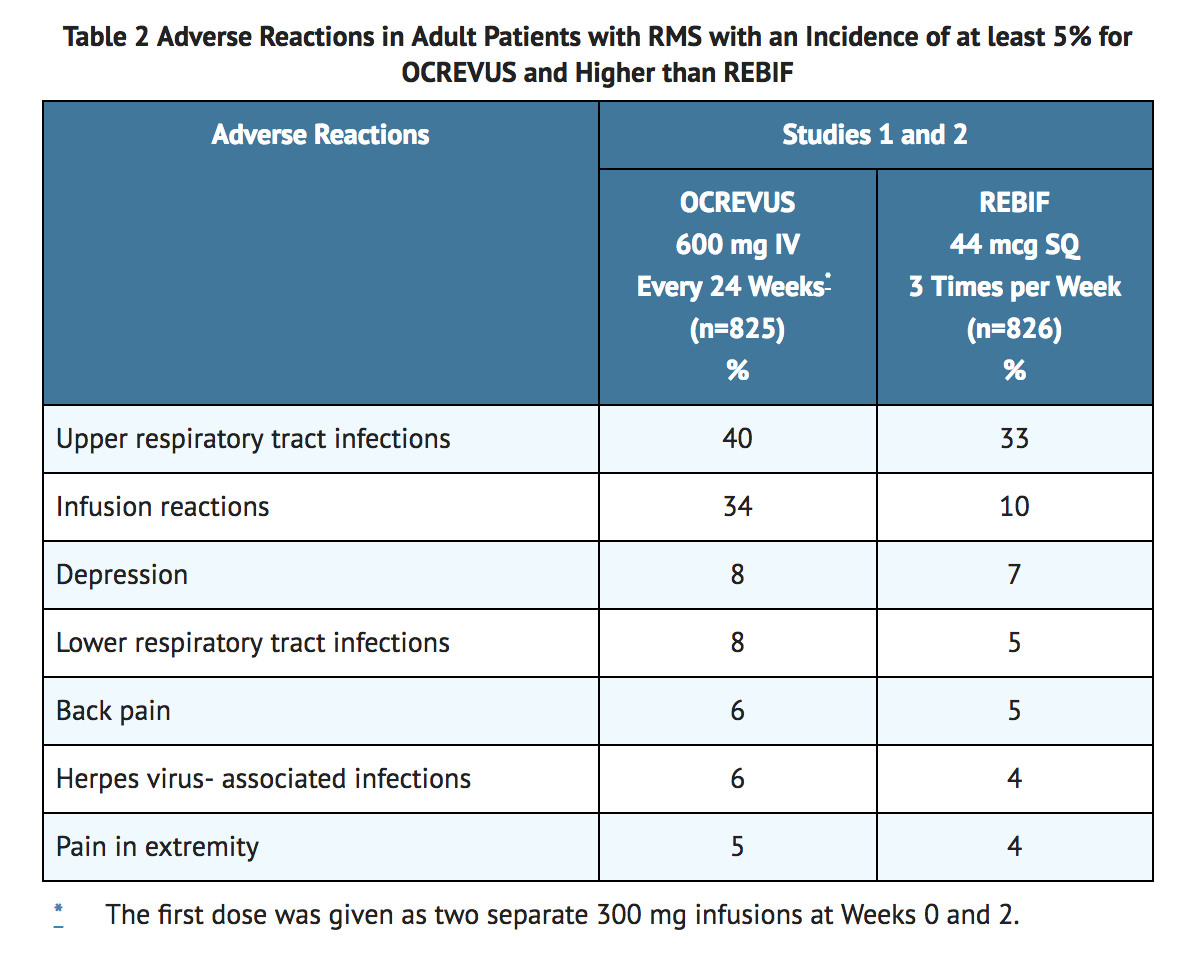
Adverse Reactions in Patients with Primary Progressive MS
- In a placebo-controlled clinical trial (Study 3), a total of 486 patients with PPMS received one course of Ocrelizumab (600 mg of Ocrelizumab administered as two 300 mg infusions two weeks apart) given intravenously every 24 weeks and 239 patients received placebo intravenously. The overall exposure in the controlled treatment period was 1416 patient-years, with median treatment duration of 3 years.
- The most common adverse reactions in the PPMS trial (incidence ≥ 10%) were upper respiratory tract infections, infusion reactions, skin infections, and lower respiratory tract infections. TABLE 3 summarizes the adverse reactions that occurred in the PPMS trial (Study 3).
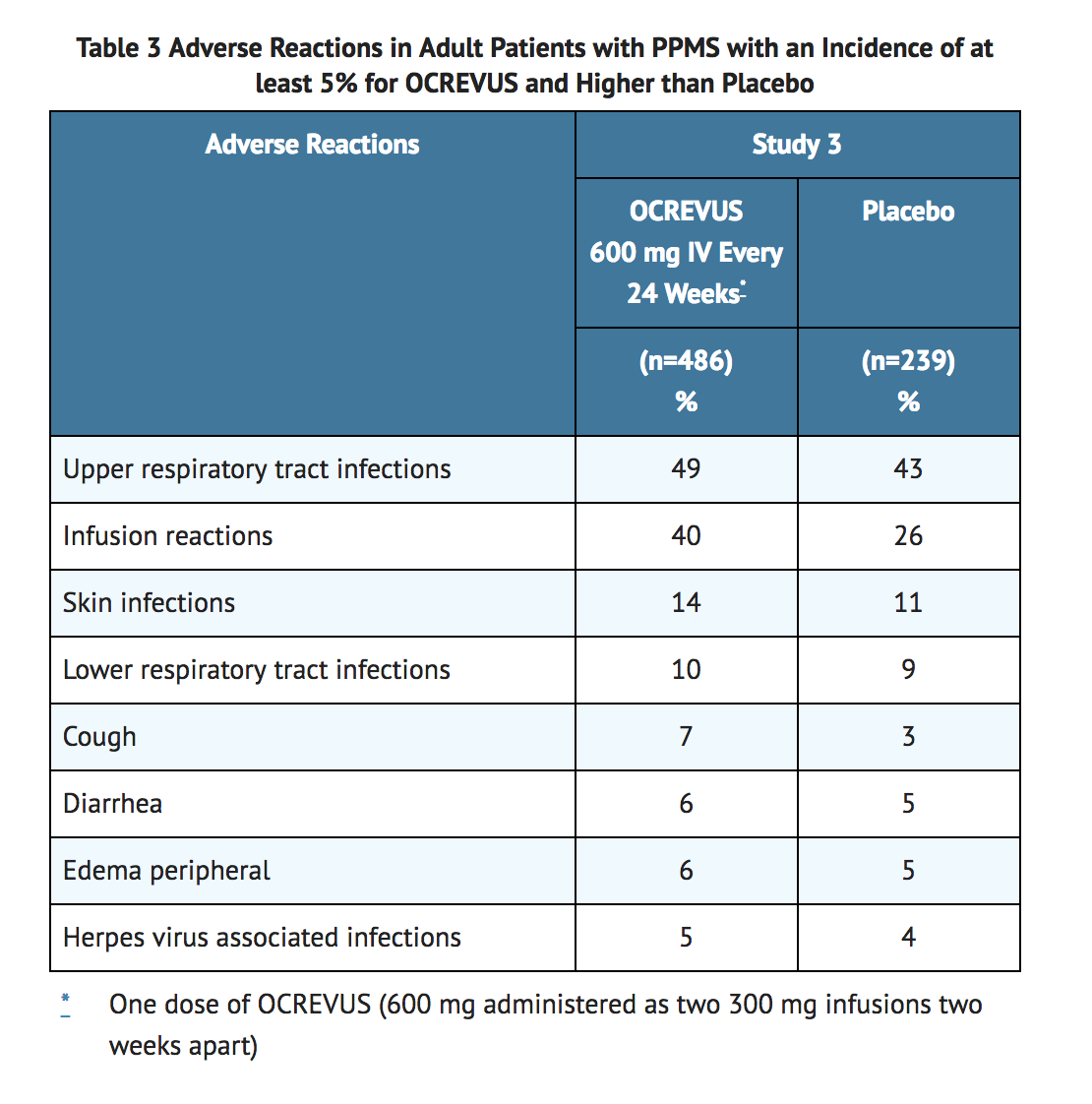
Laboratory Abnormalities
Decreased Immunoglobulins
- Ocrelizumab decreased total immunoglobulins with the greatest decline seen in IgM levels. In MS clinical trials, there was no apparent association between immunoglobulin decrease and risk for serious infections.
- In the active-controlled (RMS) trials (Study 1 and Study 2), the proportion of patients at baseline reporting IgG, IgA, and IgM below the lower limit of normal (LLN) in Ocrelizumab-treated patients was 0.5%, 1.5%, and 0.1%, respectively. Following treatment, the proportion of Ocrelizumab-treated patients reporting IgG, IgA, and IgM below the LLN at 96 weeks was 1.5%, 2.4%, and 16.5%, respectively.
- In the placebo-controlled (PPMS) trial (Study 3), the proportion of patients at baseline reporting IgG, IgA, and IgM below the LLN in Ocrelizumab-treated patients was 0.0%, 0.2%, and 0.2%, respectively. Following treatment, the proportion of Ocrelizumab-treated patients reporting IgG, IgA, and IgM below the LLN at 120 weeks was 1.1%, 0.5%, and 15.5%, respectively.
Decreased Neutrophil Levels
- In the PPMS clinical trial (Study 3), decreased neutrophil counts occurred in 13% of Ocrelizumab-treated patients compared to 10% in placebo patients. The majority of the decreased neutrophil counts were only observed once for a given patient treated with Ocrelizumab and were between LLN - 1.5 × 109/L and 1.0 × 109/L. Overall, 1% of the patients in the Ocrelizumab group had neutrophil counts less than 1.0 × 109/L and these were not associated with an infection.
Immunogenicity
- As with all therapeutic proteins, there is potential for immunogenicity. Immunogenicity data are highly dependent on the sensitivity and specificity of the test methods used. Additionally, the observed incidence of a positive result in a test method may be influenced by several factors, including sample handling, timing of sample collection, drug interference, concomitant medication, and the underlying disease. Therefore, comparison of the incidence of antibodies to Ocrelizumab with the incidence of antibodies to other products may be misleading.
- Patients in MS trials (Study 1, Study 2, and Study 3) were tested at multiple time points (baseline and every 6 months post-treatment for the duration of the trial) for anti-drug antibodies (ADAs). Out of 1311 patients treated with Ocrelizumab, 12 (~1%) tested positive for ADAs, of which 2 patients tested positive for neutralizing antibodies. These data are not adequate to assess the impact of ADAs on the safety and efficacy of Ocrelizumab.
Postmarketing Experience
There is limited information regarding Ocrelizumab Postmarketing Experience in the drug label.
Drug Interactions
- Immunosuppressive or Immune-Modulating Therapies
Immunosuppressive or Immune-Modulating Therapies
- The concomitant use of Ocrelizumab and other immune-modulating or immunosuppressive therapies, including immunosuppressant doses of corticosteroids, is expected to increase the risk of immunosuppression. Consider the risk of additive immune system effects when coadministering immunosuppressive therapies with Ocrelizumab. When switching from drugs with prolonged immune effects, such as daclizumab, fingolimod, natalizumab, teriflunomide, or mitoxantrone, consider the duration and mode of action of these drugs because of additive immunosuppressive effects when initiating Ocrelizumab.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): Risk Summary
- There are no adequate data on the developmental risk associated with use of Ocrelizumab in pregnant women. There are no data on B-cell levels in human neonates following maternal exposure to Ocrelizumab. However, transient peripheral B-cell depletion and lymphocytopenia have been reported in infants born to mothers exposed to other anti-CD20 antibodies during pregnancy. Ocrelizumab is a humanized monoclonal antibody of an immunoglobulin G1 subtype and immunoglobulins are known to cross the placental barrier. Following administration of Ocrelizumab to pregnant monkeys at doses similar to or greater than those used clinically, increased perinatal mortality, depletion of B-cell populations, renal, bone marrow, and testicular toxicity were observed in the offspring in the absence of maternal toxicity.
- In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively. The background risk of major birth defects and miscarriage for the indicated population is unknown.
Data (Animal)
- Following intravenous administration of Ocrelizumab to monkeys during organogenesis (loading doses of 15 or 75 mg/kg on gestation days 20, 21, and 22, followed by weekly doses of 20 or 100 mg/kg), depletion of B-lymphocytes in lymphoid tissue (spleen and lymph nodes) was observed in fetuses at both doses.
- Intravenous administration of Ocrelizumab (three daily loading doses of 15 or 75 mg/kg, followed by weekly doses of 20 or 100 mg/kg) to pregnant monkeys throughout the period of organogenesis and continuing through the neonatal period resulted in perinatal deaths (some associated with bacterial infections), renal toxicity (glomerulopathy and inflammation), lymphoid follicle formation in the bone marrow, and severe decreases in circulating B-lymphocytes in neonates. The cause of the neonatal deaths is uncertain; however, both affected neonates were found to have bacterial infections. Reduced testicular weight was observed in neonates at the high dose.
- A no-effect dose for adverse developmental effects was not identified; the doses tested in monkey are 2 and 10 times the recommended human dose of 600 mg, on a mg/kg basis.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Ocrelizumab in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Ocrelizumab during labor and delivery.
Nursing Mothers
Risk Summary
- There are no data on the presence of Ocrelizumab in human milk, the effects on the breastfed infant, or the effects of the drug on milk production. Ocrelizumab was excreted in the milk of Ocrelizumab-treated monkeys. Human IgG is excreted in human milk, and the potential for absorption of Ocrelizumab to lead to B-cell depletion in the infant is unknown. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for Ocrelizumab and any potential adverse effects on the breastfed infant from Ocrelizumab or from the underlying maternal condition.
Pediatric Use
- Safety and effectiveness of Ocrelizumab in pediatric patients have not been established.
Geriatic Use
- Clinical studies of Ocrelizumab did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects.
Gender
There is no FDA guidance on the use of Ocrelizumab with respect to specific gender populations.
Race
There is no FDA guidance on the use of Ocrelizumab with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Ocrelizumab in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Ocrelizumab in patients with hepatic impairment.
Females of Reproductive Potential and Males
Contraception
- Women of childbearing potential should use contraception while receiving Ocrelizumab and for 6 months after the last infusion of Ocrelizumab.
Immunocompromised Patients
There is no FDA guidance one the use of Ocrelizumab in patients who are immunocompromised.
Administration and Monitoring
Administration
Intravenous
- Solution in vial is clear or slightly opalescent, and colorless to pale brown; do not use if discolored.
- Do not shake vial.
- 300 mg dose: Withdraw 10 mL from vial and further dilute in 250 mL of NS to final concentration of about 1.2 mg/mL.
- 600 mg dose: Withdraw 20 mL from 2 vials and further dilute in 500 mL of NS to final concentration of about 1.2 mg/mL.
- Only dilute in NS; do not dilute with any other diluent.
- May use polyvinyl chloride (PCV) or polyolefin (PO) infusion bags and IV administration sets.
- Diluted solution should be used immediately or stored for up to 8 hours at a room temperature not exceeding 25 degrees C (77 degrees F) or for up to 24 hours if stored in the refrigerator at 2 to 8 degrees C (36 to 46 degrees F). Storage time includes infusion time.
- Prior to administration, bring infusion bag to room temperature.
- Administer diluted solution via a dedicated line with a 0.2 or 0.22 micron in-line filter.
- 300 mg dose: Begin infusion rate at 30 mL/hr and increase by 30 mL/hr every 30 minutes, as tolerated, to MAX 180 mL/hr for a duration of 2.5 hours or longer. Observe patient for at least 1 hour after infusion completion.
- 600 mg dose: Begin infusion rate at 40 mL/hr and increase by 40 mL/hr every 30 minutes, as tolerated, to MAX 200 mL/hr for a duration of 3.5 hours or longer. Observe patient for at least 1 hour after infusion completion.
- If infusion cannot be completed the same day, discard remaining solution.
- Missed dose: Give as soon as possible; do not wait until the next scheduled dose. Reset the dose schedule to administer the next sequential dose 6 months after the missed dose; doses must be separated by at least 5 months.
Monitoring
- Reductions in the rates of relapse and disability progression are indicative of efficacy.
- Hepatitis B virus screening: Prior to initiation.
- Signs and symptoms of active infection: Prior to every infusion.
- Signs and symptoms of infusion reactions: During infusion and for at least 1 hour after completion.
IV Compatibility
There is limited information regarding the compatibility of Ocrelizumab and IV administrations.
Overdosage
There is limited information regarding Ocrelizumab overdosage. If you suspect drug poisoning or overdose, please contact the National Poison Help hotline (1-800-222-1222) immediately.
Pharmacology
Mechanism of Action
- The precise mechanism by which Ocrelizumab exerts its therapeutic effects in multiple sclerosis is unknown, but is presumed to involve binding to CD20, a cell surface antigen present on pre-B and mature B lymphocytes. Following cell surface binding to B lymphocytes, Ocrelizumab results in antibody-dependent cellular cytolysis and complement-mediated lysis.
Structure
There is limited information regarding Ocrelizumab Structure in the drug label.
Pharmacodynamics
- For B-cell counts, assays for CD19+ B-cells are used because the presence of Ocrelizumab interferes with the CD20 assay. Treatment with Ocrelizumab reduces CD19+ B-cell counts in blood by 14 days after infusion. In clinical studies, B-cell counts rose to above the lower limit of normal (LLN) or above baseline counts between infusions of Ocrelizumab at least one time in 0.3% to 4.1% of patients. In a clinical study of 51 patients, the median time for B-cell counts to return to either baseline or LLN was 72 weeks (range 27-175 weeks) after the last Ocrelizumab infusion. Within 2.5 years after the last infusion, B-cell counts rose to either baseline or LLN in 90% of patients.
Pharmacokinetics
- Pharmacokinetics (PK) of Ocrelizumab in MS clinical studies fit a two compartment model with time-dependent clearance. The overall exposure at the steady-state (AUC over the 24 week dosing intervals) of Ocrelizumab was 3,510 mcg/mL per day. In clinical studies in MS patients, maintenance doses of Ocrelizumab were either 600 mg every 6 months (RMS patients) or two 300 mg infusions separated by 14 days every 6 months (PPMS patients). The mean maximum concentration was 212 mcg/mL in patients with RMS (600 mg infusion) and 141 mcg/mL in patients with PPMS (two 300 mg infusions administered within two weeks). The pharmacokinetics of Ocrelizumab was essentially linear and dose proportional between 400 mg and 2000 mg.
Distribution
- The population PK estimate of the central volume of distribution was 2.78 L. Peripheral volume and inter-compartment clearance were estimated at 2.68 L and 0.29 L/day, respectively.
Elimination
- Constant clearance was estimated at 0.17 L/day, and initial time-dependent clearance at 0.05 L/day, which declined with a half-life of 33 weeks. The terminal elimination half-life was 26 days.
Metabolism
- The metabolism of Ocrelizumab has not been directly studied because antibodies are cleared principally by catabolism.
Specific Populations
Renal impairment
- Patients with mild renal impairment were included in clinical trials. No significant change in the pharmacokinetics of Ocrelizumab was observed in those patients.
Hepatic impairment
- Patients with mild hepatic impairment were included in clinical trials. No significant change in the pharmacokinetics of Ocrelizumab was observed in those patients.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- No carcinogenicity studies have been performed to assess the carcinogenic potential of Ocrelizumab.
- No studies have been performed to assess the mutagenic potential of Ocrelizumab. As an antibody, Ocrelizumab is not expected to interact directly with DNA.
- No effects on reproductive organs were observed in male monkeys administered Ocrelizumab by intravenous injection (three loading doses of 15 or 75 mg/kg, followed by weekly doses of 20 or 100 mg/kg) for 8 weeks. There were also no effects on estrus cycle in female monkeys administered Ocrelizumab over three menstrual cycles using the same dosing regimen. The doses tested in monkey are 2 and 10 times the recommended human dose of 600 mg, on a mg/kg basis.
Clinical Studies
Relapsing Forms of Multiple Sclerosis (RMS)
- The efficacy of Ocrelizumab was demonstrated in two randomized, double-blind, double-dummy, active comparator-controlled clinical trials of identical design, in patients with RMS treated for 96 weeks (Study1 and Study 2). The dose of Ocrelizumab was 600 mg every 24 weeks (initial treatment was given as two 300 mg IV infusions administered 2 weeks apart, and subsequent doses were administered as a single 600 mg IV infusion) and placebo subcutaneous injections were given 3 times per week. The dose of REBIF, the active comparator, was 44 mcg given as subcutaneous injections 3 times per week and placebo IV infusions were given every 24 weeks. Both studies included patients who had experienced at least one relapse within the prior year, or two relapses within the prior two years, and had an Expanded Disability Status Scale (EDSS) score from 0 to 5.5. Patients with primary progressive forms of multiple sclerosis (MS) were excluded. Neurological evaluations were performed every 12 weeks and at the time of a suspected relapse. Brain MRIs were performed at baseline and at Weeks 24, 48, and 96.
- The primary outcome of both Study 1 and Study 2 was the annualized relapse rate (ARR). Additional outcome measures included the proportion of patients with confirmed disability progression, the mean number of MRI T1 gadolinium (Gd)-enhancing lesions at Weeks 24, 48, and 96, and new or enlarging MRI T2 hyperintense lesions. Progression of disability was defined as an increase of 1 point or more from the baseline EDSS score attributable to MS when the baseline EDSS score was 5.5 or less, or 0.5 points or more when the baseline EDSS score was above 5.5. Disability progression was considered confirmed when the increase in the EDSS was confirmed at a regularly scheduled visit 12 weeks after the initial documentation of neurological worsening. The primary population for analysis of confirmed disability progression was the pooled population from Studies 1 and 2.
- In Study 1, 410 patients were randomized to Ocrelizumab and 411 to REBIF; 11% of Ocrelizumab-treated and 17% of REBIF-treated patients did not complete the 96-week double-blind treatment period. The baseline demographic and disease characteristics were balanced between the two treatment groups. At baseline, the mean age of patients was 37 years; 66% were female. The mean time from MS diagnosis to randomization was 3.8 years, the mean number of relapses in the previous year was 1.3, and the mean EDSS score was 2.8; 74% of patients had not been treated with a non-steroid therapy for MS in the 2 years prior to the study. At baseline, 40% of patients had one or more T1 Gd-enhancing lesions (mean 1.8).
- In Study 2, 417 patients were randomized to Ocrelizumab and 418 to REBIF; 14% of Ocrelizumab-treated and 23% of REBIF-treated patients did not complete the 96-week double-blind treatment period. The baseline demographic and disease characteristics were balanced between the two treatment groups. At baseline, the mean age of patients was 37 years; 66% were female. The mean time from MS diagnosis to randomization was 4.1 years, the mean number of relapses in the previous year was 1.3, and the mean EDSS score was 2.8; 74% of patients had not been treated with a non-steroid therapy for MS in the 2 years prior to the study. At baseline, 40% of Ocrelizumab-treated patients had one or more T1 Gd-enhancing lesions (mean 1.9).
- In Study 1 and Study 2, Ocrelizumab significantly lowered the annualized relapse rate and the proportion of patients with disability progression confirmed at 12 weeks after onset compared to REBIF. Results for Study 1 and Study 2 are presented in TABLE 4 and FIGURE 1.
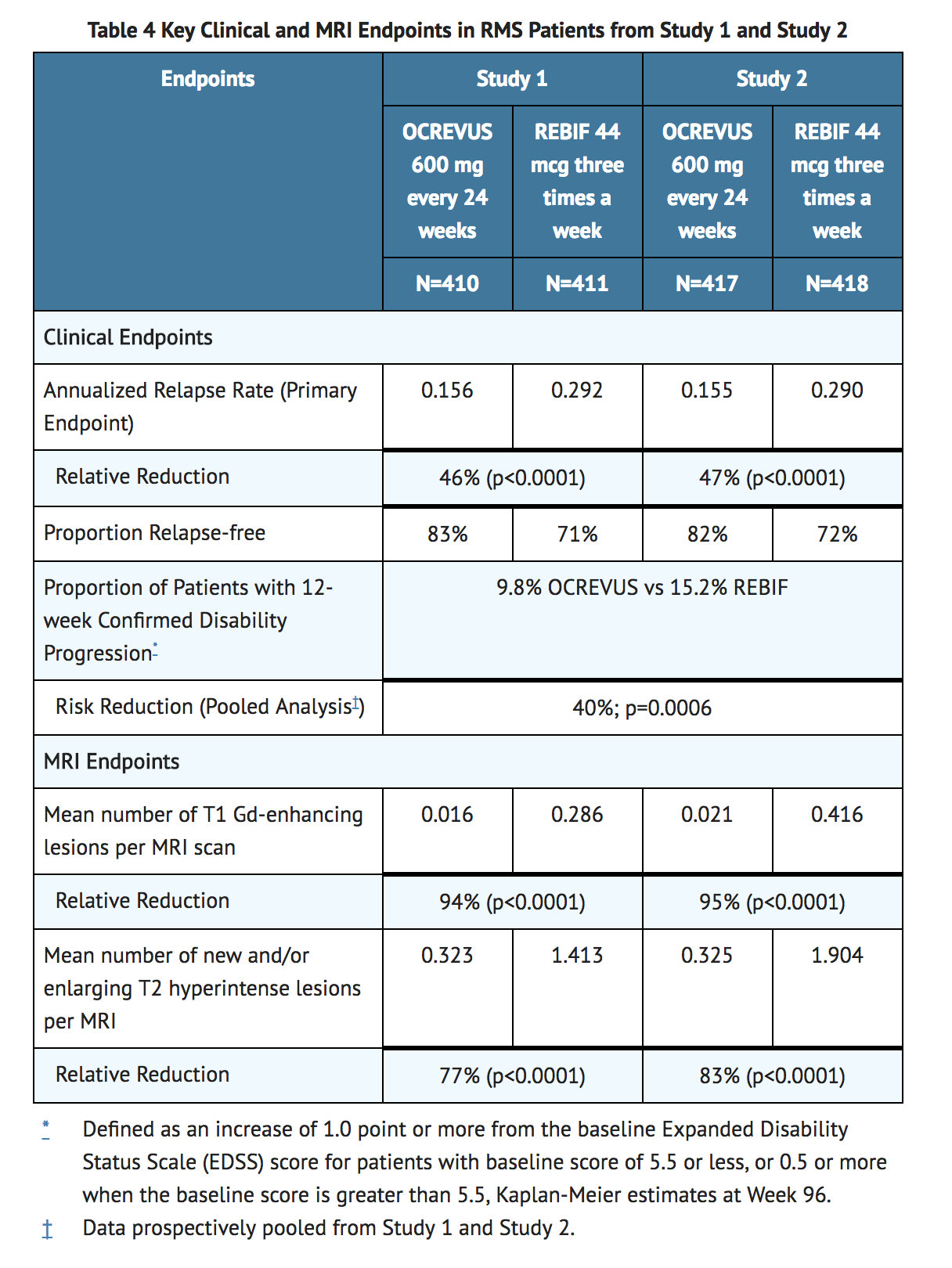
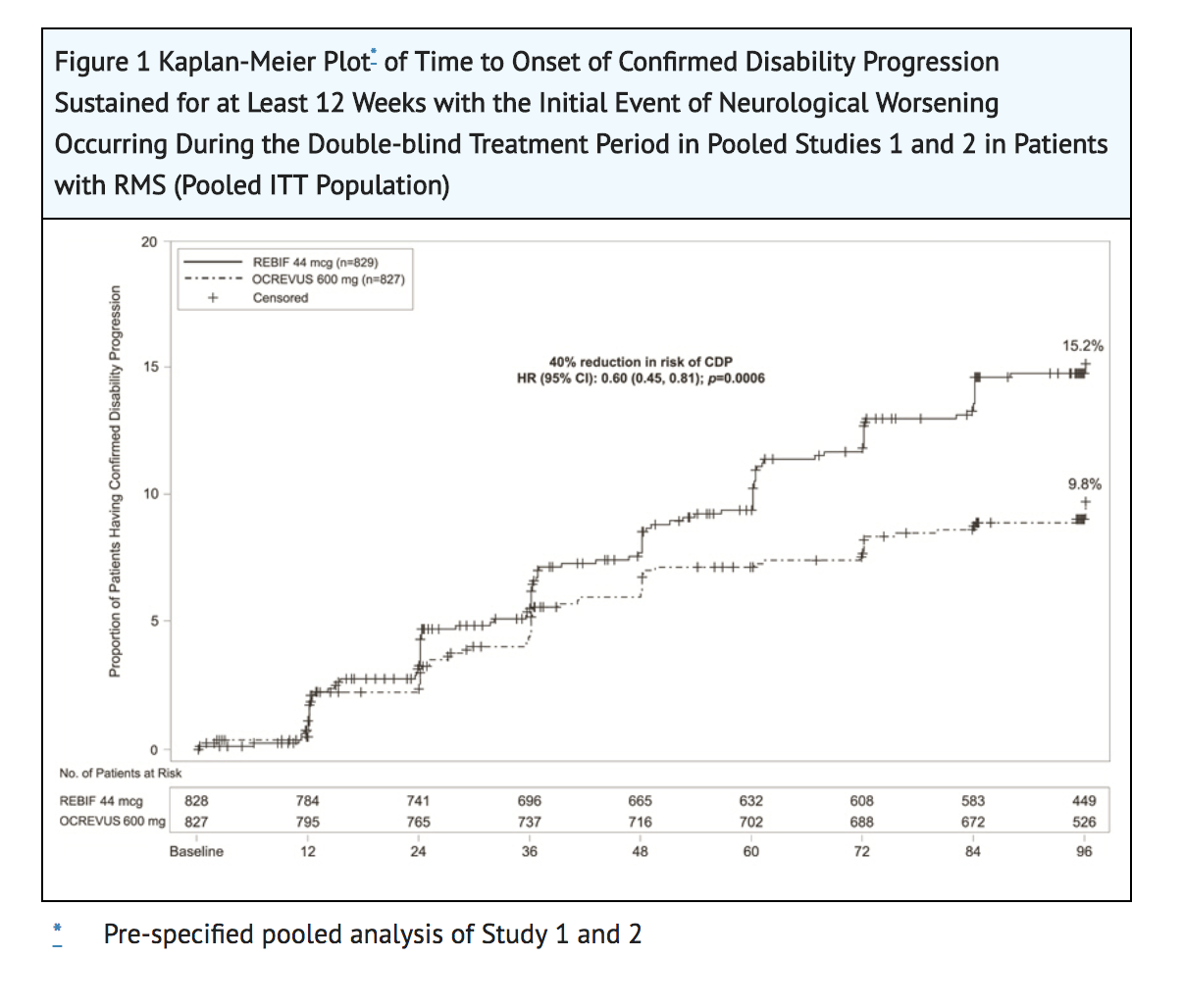
- In exploratory subgroup analyses of Study 1 and Study 2, the effect of Ocrelizumab on annualized relapse rate and disability progression was similar in male and female patients.
Primary Progressive Multiple Sclerosis (PPMS)
- Study 3 was a randomized, double-blind, placebo-controlled clinical trial in patients with PPMS. Patients were randomized 2:1 to receive either Ocrelizumab 600 mg or placebo as two 300 mg intravenous infusions 2 weeks apart every 24 weeks for at least 120 weeks. Selection criteria required a baseline EDSS of 3 to 6.5 and a score of 2 or greater for the EDSS pyramidal functional system due to lower extremity findings. Neurological assessments were conducted every 12 weeks. An MRI scan was obtained at baseline and at Weeks 24, 48, and 120.
- In Study 3, the primary outcome was the time to onset of disability progression attributable to MS confirmed to be present at the next neurological assessment at least 12 weeks later. Disability progression occurred when the EDSS score increased by 1 point or more from the baseline EDSS if the baseline EDSS was 5.5 points or less, or by 0.5 points or more if the baseline EDSS was more than 5.5 points. In Study 3, confirmed disability progression also was deemed to have occurred if patients who had onset of disability progression discontinued participation in the study before the next assessment. Additional outcome measures included timed 25-foot walk, and percentage change in T2 hyperintense lesion volume.
- Study 3 randomized 488 patients to Ocrelizumab and 244 to placebo; 21% of Ocrelizumab-treated patients and 34% of placebo-treated patients did not complete the trial. The baseline demographic and disease characteristics were balanced between the two treatment groups. At baseline, the mean age of patients was 45; 49% were female. The mean time since symptom onset was 6.7 years, the mean EDSS score was 4.7, and 26% had one or more T1 Gd-enhancing lesions at baseline; 88% of patients had not been treated previously with a non-steroid treatment for MS. The time to onset of disability progression confirmed at 12 weeks after onset was significantly longer for Ocrelizumab-treated patients than for placebo-treated patients (see FIGURE 2). Results for Study 3 are presented in TABLE 5 and FIGURE 2.
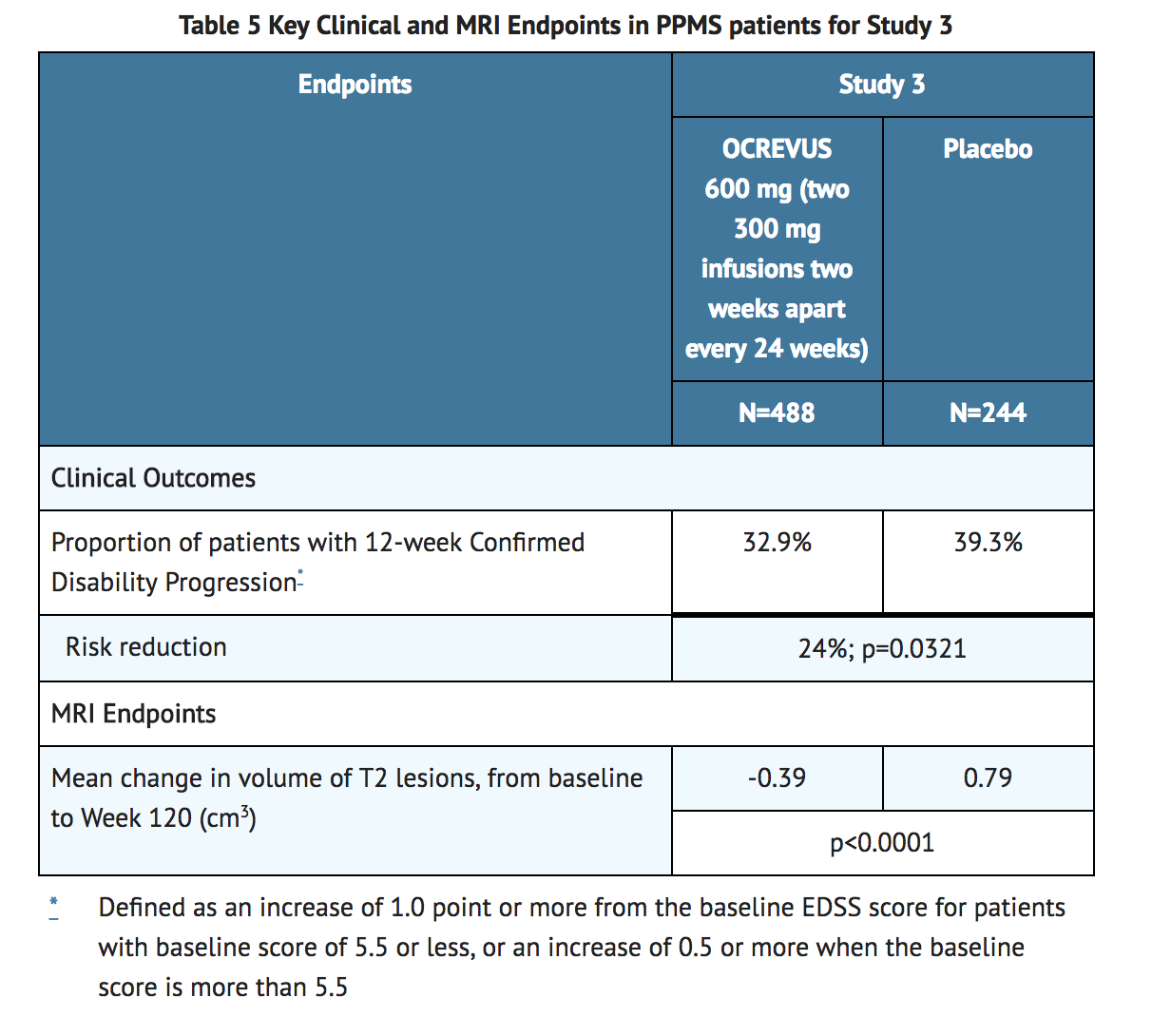
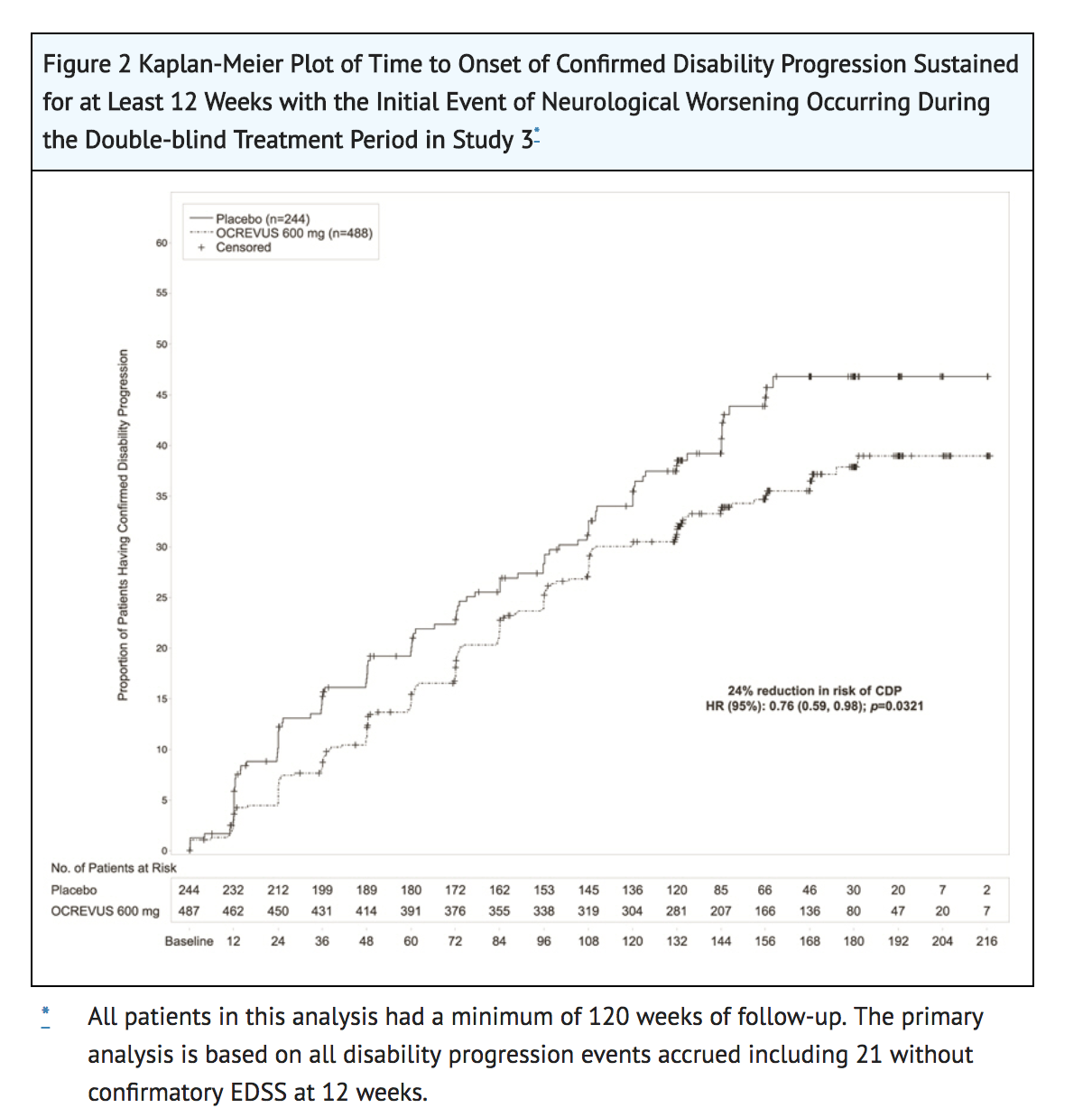
- In the overall population in Study 3, the proportion of patients with 20 percent worsening of the timed 25-foot walk confirmed at 12 weeks was 49% in Ocrelizumab-treated patients compared to 59% in placebo-treated patients (25% risk reduction).
- In exploratory subgroup analyses of Study 3, the proportion of female patients with disability progression confirmed at 12 weeks after onset was similar in Ocrelizumab-treated patients and placebo-treated patients (approximately 36% in each group). In male patients, the proportion of patients with disability progression confirmed at 12 weeks after onset was approximately 30% in Ocrelizumab-treated patients and 43% in placebo-treated patients. Clinical and MRI endpoints that generally favored Ocrelizumab numerically in the overall population, and that showed similar trends in both male and female patients, included annualized relapse rate, change in T2 lesion volume, and number of new or enlarging T2 lesions.
How Supplied
- Ocrelizumab injection is a preservative-free, sterile, clear or slightly opalescent, and colorless to pale brown solution supplied as a carton containing one 300 mg/10 mL (30 mg/mL) single-dose vial (NDC 50242-150-01).
Storage
- Store Ocrelizumab vials at 2°C–8°C (36°F–46°F) in the outer carton to protect from light. Do not freeze or shake.
Images
Drug Images
{{#ask: Page Name::Ocrelizumab |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel

{{#ask: Label Page::Ocrelizumab |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
Infusion Reactions
- Inform patients about the signs and symptoms of infusion reactions, and that infusion reactions can occur up to 24 hours after infusion. Advise patients to contact their healthcare provider immediately for signs or symptoms of infusion reactions.
Infection
- Advise patients to contact their healthcare provider for any signs of infection during treatment or after the last dose. Signs include fever, chills, constant cough, or signs of herpes such as cold sore, shingles, or genital sores.
- Advise patients that PML has happened with drugs that are similar to Ocrelizumab and may happen with Ocrelizumab. Inform the patient that PML is characterized by a progression of deficits and usually leads to death or severe disability over weeks or months. Instruct the patient of the importance of contacting their doctor if they develop any symptoms suggestive of PML. Inform the patient that typical symptoms associated with PML are diverse, progress over days to weeks, and include progressive weakness on one side of the body or clumsiness of limbs, disturbance of vision, and changes in thinking, memory, and orientation leading to confusion and personality changes.
- Advise patients that Ocrelizumab may cause reactivation of hepatitis B infection and that monitoring will be required if they are at risk.
Vaccination
- Advise patients to complete any required vaccinations at least 6 weeks prior to initiation of Ocrelizumab. Administration of live-attenuated or live vaccines is not recommended during Ocrelizumab treatment and until B-cell recovery.
Malignancies
- Advise patients that an increased risk of malignancy, including breast cancer, may exist with Ocrelizumab. Advise patients that they should follow standard breast cancer screening guidelines.
Pregnancy
- Instruct patients that if they are pregnant or plan to become pregnant while taking Ocrelizumab they should inform their healthcare provider.

Precautions with Alcohol
Alcohol-Ocrelizumab interaction has not been established. Talk to your doctor regarding the effects of taking alcohol with this medication.
Brand Names
- Ocrevus
Look-Alike Drug Names
There is limited information regarding Ocrelizumab Look-Alike Drug Names in the drug label.
Drug Shortage
Price
References
The contents of this FDA label are provided by the National Library of Medicine.