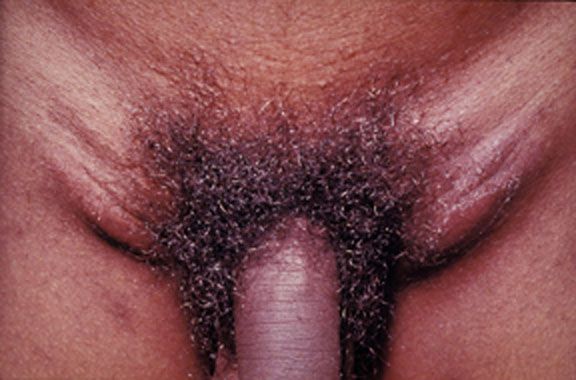
Lymphogranuloma venereum physical examination
|
Lymphogranuloma venereum Microchapters |
|
Differentiating Lymphogranuloma venereum from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Lymphogranuloma venereum physical examination On the Web |
|
American Roentgen Ray Society Images of Lymphogranuloma venereum physical examination |
|
Risk calculators and risk factors for Lymphogranuloma venereum physical examination |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Nate Michalak, B.A.
Overview
Primary LGV is characterized by a small, nontender papule or ulcer. The primary lesion is typically unnoticed so few patients present at this stage. Majority of patients that do present are male. Secondary LGV is characterized by tender, swollen lymph nodes, typically unilateral, known as buboes. Enlarged inguinal and/or femoral lymph nodes occur after primary lesion of anterior genital area. Enlarged iliac and/or perirectal lymph nodes occure after primary lesion of posterior genital area. 20% of patients present with "groove sign". Buboes may be indurated or draining sinuses. Tertiary LGV is characterized by [perirectal]] fistulas and/or strictures, ulcerative proctitis, and/or Elephantiasis of gentials. Males may present with "saxophone penis". Females may present with with ulceration and thickening of the vulva.
Physcial Examination
Vital Signs
- Fever during later stages
Primary LGV
- Patients presenting at first stage of LGV usually have a small, nontender papule or ulcer.[1]
- Common locations in males:
- Common locations in females:
- Posterior vaginal wall
- Posterior cervix
- Fourchette
- Vulva
- Due to lesion location on each sex, more males present at this stage than females.[1]
Secondary LGV
- Patients present with tender, swollen lymph nodes, typically unilateral, known as buboes.
- Enlarged inguinal and/or femoral lymph nodes occur after primary lesion of anterior genital area (anterior vulva, penis, or urethra).
- Enlarged iliac and/or perirectal lymph nodes occure after primary lesion of posterior genital area (posterior vulva, vagina, or anus).
- Inguinal inflammation more common in men while anorectal lymphadenopathy more common in women
- 20% of patients develop "groove sign": enlarged inguinal and femoral lymph nodes separated by the inguinal ligament.[2]
- Buboes may present as indurated abscesses or ruptured, draining sinuses.[3]
Tertiary LGV
- Patients present with perirectal fistulas and/or strictures
- Patients presenting at this stage are predominantly female or homosexual males
- Proctoscopy may reveal ulcerative proctitis[4]
- Elephantiasis of gentials
- Ulceration and thickening of the vulva in females
- Penile and scrotal edema termed "saxophone penis"[5]
Gallery
-
Lymphogranuloma venereum: is caused by the invasive serovars L1, L2, or L3 of Chlamydia trachomatis. This young adult experienced the acute onset of tender, enlarged lymph nodes in both groins.
References
- ↑ 1.0 1.1 Ceovic R, Gulin SJ (2015). "Lymphogranuloma venereum: diagnostic and treatment challenges". Infect Drug Resist. 8: 39–47. doi:10.2147/IDR.S57540. PMC 4381887. PMID 25870512.
- ↑ Roest RW, van der Meijden WI, European Branch of the International Union against Sexually Transmitted Infection and the European Office of the World Health Organization (2001). "European guideline for the management of tropical genito-ulcerative diseases". Int J STD AIDS. 12 Suppl 3: 78–83. PMID 11589803.
- ↑ Mabey, D (2002). "Lymphogranuloma venereum". Sexually Transmitted Infections. 78 (2): 90–92. doi:10.1136/sti.78.2.90. ISSN 1368-4973.
- ↑ Lynch CM, Felder TL, Schwandt RA, Shashy RG (1999). "Lymphogranuloma venereum presenting as a rectovaginal fistula". Infect Dis Obstet Gynecol. 7 (4): 199–201. doi:10.1155/S1064744999000344. PMC 1784745. PMID 10449269.
- ↑ Koley S, Mandal RK (2013). "Saxophone penis after unilateral inguinal bubo of lymphogranuloma venereum". Indian J Sex Transm Dis. 34 (2): 149–51. doi:10.4103/0253-7184.120575. PMC 3841672. PMID 24339471.