Lacunar stroke
| Lacunar stroke | |
| ICD-10 | G46.5-G46.7 |
|---|---|
| ICD-9 | 434.91 |
| DiseasesDB | 31186 |
| MeSH | D020520 |
|
WikiDoc Resources for Lacunar stroke |
|
Articles |
|---|
|
Most recent articles on Lacunar stroke Most cited articles on Lacunar stroke |
|
Media |
|
Powerpoint slides on Lacunar stroke |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Lacunar stroke at Clinical Trials.gov Trial results on Lacunar stroke Clinical Trials on Lacunar stroke at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Lacunar stroke NICE Guidance on Lacunar stroke
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Lacunar stroke Discussion groups on Lacunar stroke Patient Handouts on Lacunar stroke Directions to Hospitals Treating Lacunar stroke Risk calculators and risk factors for Lacunar stroke
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Lacunar stroke |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Synonyms and keywords: Lacunar infarction
Introduction
Lacunar stroke occurs when one of the small arteries(Φ:0.2 - 15mm) that provide blood to the brain's deep structures is blocked and injure deeper structures underneath the cortex.
Pathophysiology
Lacunes are caused by occlusion of a single deep penetrating artery. The deep penetrating arteries are small nonbranching end arteries (usually smaller than 500 micrometers in diameter), which arise directly from much larger arteries (eg, the middle cerebral artery, anterior choroidal artery, anterior cerebral artery, posterior cerebral artery, posterior communicating artery, cerebellar arteries, basilar artery). Their small size and proximal position predisposes them to the development of microatheroma and lipohyalinosis.
At the beginning, lipohyalinosis was thought to be the main small vessel pathology of lacunes; however, microatheroma now is thought to be the most common mechanism of arterial occlusion (or stenosis). Occasionally, atheroma in the parent artery blocks the orifice of the penetrating artery (luminal atheroma), or atheroma involves the origin of the penetrating artery (junctional atheroma).
A hemodynamic (hypoperfusion) mechanism is suggested when there is a stenosis (and not occlusion) of the penetrating artery. When no evidence of small vessel disease is found on histologic examination, an embolic cause is assumed, either artery-to-artery embolism or cardioembolism. In one recent series, 25% of patients with clinical radiologically defined lacunes had a potential cardiac cause for their strokes.
Diagnosis
It is estimated that lacunar infarcts account for 25% of all strokes that are due to infarction.
Patients tend to present with a pure motor, pure sensory or sensorimotor dysfunction or 'ataxic hemiparesis'. They will often recover well.
The imaging findings are
- An acute lacunar infarction (12 hours up to 7 days) appears as a small high-signal-intensity region on T2-weighted and FLAIR images and as a hypointense area on T1-weighted images.
- High signal intensity is seen on diffusion-weighted images with corresponding low signal intensity on the apparent diffusion coefficient map.
- Enhancement is variable
- A chronic lacunar infarction is better defined and has high signal intensity on T2-weighted images and low signal intensity on T1-weighted images. On FLAIR images, a hyperintense lesion or a lesion with a hypointense center and a hyperintense rim reflecting gliosis is seen.
- Enhancement may last for up to 8 weeks after the acute event
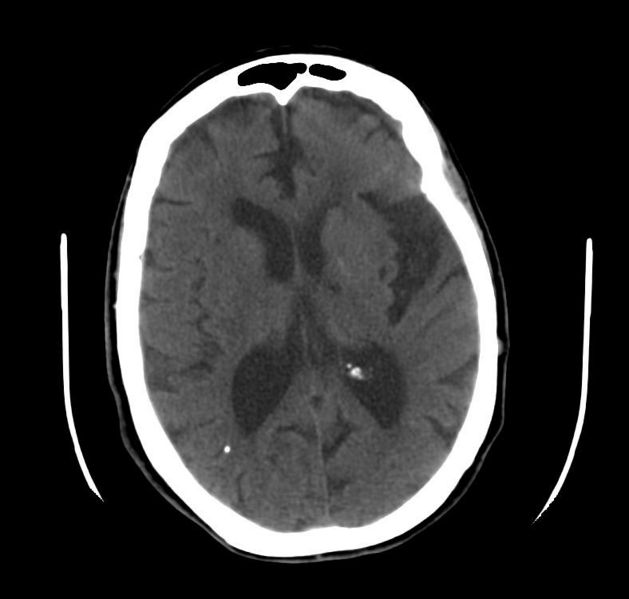
Patient #1: Chronic lacunar infarctions on CT
Related conditions
If there is enough white matter disease from lacunar pathology, one can see a subcortical dementia such as Binswanger disease.