Giardia lamblia
|
Giardiasis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Giardia lamblia On the Web |
|
American Roentgen Ray Society Images of Giardia lamblia |
| Giardia lamblia | ||||||||
|---|---|---|---|---|---|---|---|---|
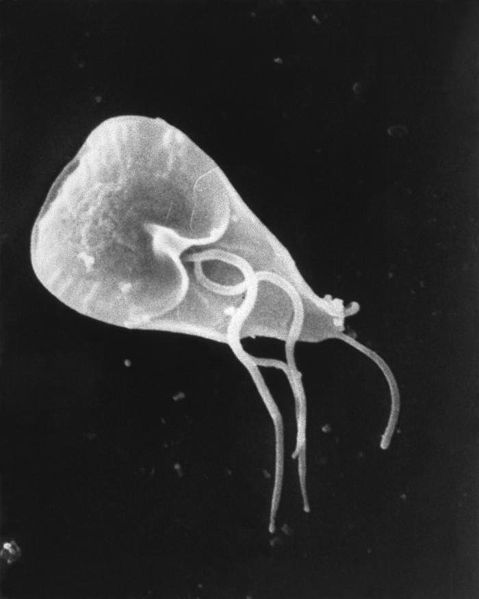 Giardia cell, SEM
| ||||||||
| Scientific classification | ||||||||
| ||||||||
| Binomial name | ||||||||
| Giardia lamblia (Kunstler, 1882) |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Giardia lamblia (synonymous with Lamblia intestinalis and Giardia duodenalis) is a flagellated protozoan parasite that is responsible for the development of giardiasis.
Higher Order Classification
Eukaryota, Diplomonadida group, Diplomonadida, Hexamitidae, Giardiinae, Giardia, G. lamblia
Natural Reservoir
- Giardia affects humans and animals, such as cats, dogs, cows, beavers, deer, and sheep.
Microbiological Characteristicsc
- Giardia lamblia is a flagellated, microaerophilic parasite.
- The trophozoite form of G. lamblia is pear-shaped and has a unique morphology that includes two identical nuclei, a ventral disc for adhesion to the host intestine, and flagella.
Genome
- G. lamblia genome consists of 1.2 million base pairs (average GC content: 46%).[1]
- The genome pairs are distributed across five linear chromosomes.[1]
- Similar to other eukaryotes, each chromosome is flanked by the telomere sequence (5’TAGGG3’).[1]
Life cycle
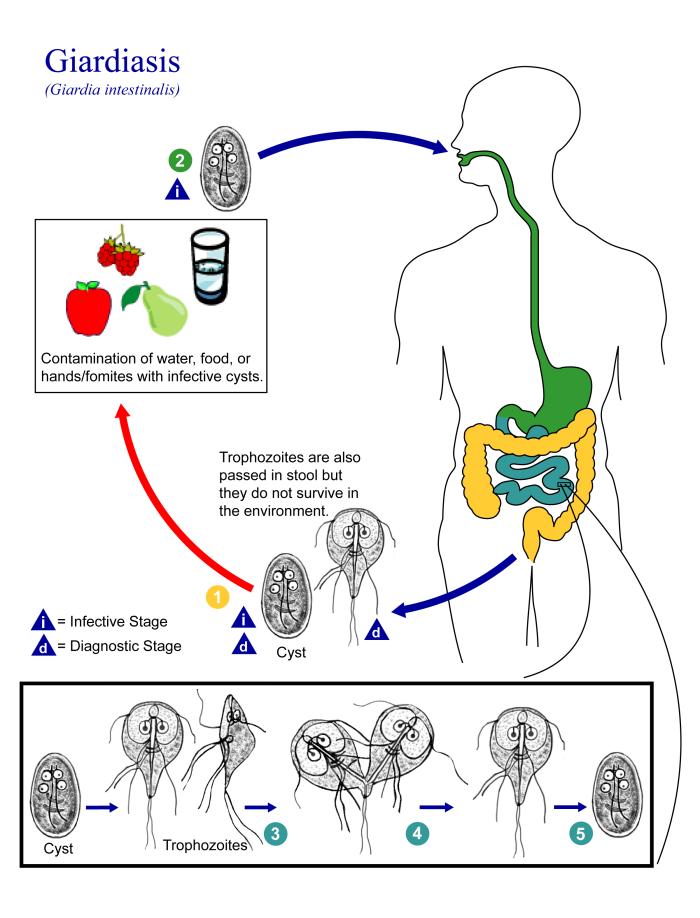
Giardia belongs among the diplomonads.
Non-infective Cyst
- The life cycle begins with a noninfective cyst being excreted with faeces of an infected individual. Once out in the environment, the cyst becomes infective.
- A distinguishing characteristic of the cyst is 4 nuclei and a retracted cytoplasm.
Trophozoite
- Once ingested by a host, the trophozoite emerges to an active state of feeding and motility.
- After the feeding stage, the trophozoite undergoes asexual replication through longitudinal binary fission.
- The resulting trophozoites and cysts then pass through the digestive system in the feces.
- While the trophozoites may be found in the feces, only the cysts are capable of surviving outside of the host.
- Distinguishing features of the trophozoites are large karyosomes and lack of peripheral chromatin, giving the two nuclei a halo appearance.
-
SEM depicts the dorsal surface of a Giardia protozoan, isolated from a rat’s intestine. From Public Health Image Library (PHIL). [2]
-
SEM depicts the mucosal surface of the small intestine of a gerbil infested with Giardia sp. protozoa. From Public Health Image Library (PHIL). [2]
-
SEM depicts a Giardia lamblia protozoan in a late stage of cell division that was about to become two separate organisms, producing a heart-shaped form. From Public Health Image Library (PHIL). [2]
-
SEM depicts the ventral surface of a Giardia muris trophozoite. From Public Health Image Library (PHIL). [2]
-
SEM depicts dorsal surface of a Giardia protozoan, isolated from a rat’s intestine. From Public Health Image Library (PHIL). [2]
-
SEM depicts some of the ultrastructural morphologic details of an oblong-shaped Giardia sp. protozoan cyst. From Public Health Image Library (PHIL). [2]
-
SEM depicts the ventral surface of a Giardia muris trophozoite that had settled atop the mucosal surface of a rat’s intestine. From Public Health Image Library (PHIL). [2]
-
SEM depicts a Giardia lamblia protozoan that was about to become two separate organisms, as it was caught in a late stage of cell division. From Public Health Image Library (PHIL). [2]
-
SEM depicts a Giardia muris protozoan adhering itself to the microvillous border of an intestinal epithelial cell. From Public Health Image Library (PHIL). [2]
-
This photomicrograph depicts Giardia lamblia parasites using indirect immunofluorescence test for giardiasis. From Public Health Image Library (PHIL). [2]
Differential diagnosis
Giardia lamblia infection must be differentiated from other causes of viral, bacterial, and parasitic gastroentritis.
| Organism | Age predilection | Travel History | Incubation Size (cell) | Incubation Time | History and Symptoms | Diarrhea type8 | Food source | Specific consideration | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Fever | N/V | Cramping Abd Pain | Small Bowel | Large Bowel | Inflammatory | Non-inflammatory | |||||||||
| Viral | Rotavirus | <2 y | - | <102 | <48 h | + | + | - | + | + | - | Mostly in day cares, most common in winter. | |||
| Norovirus | Any age | - | 10 -103 | 24-48 h | + | + | + | + | + | - | Most common cause of gastroenteritis, abdominal tenderness, | ||||
| Adenovirus | <2 y | - | 105 -106 | 8-10 d | + | + | + | + | + | - | No seasonality | ||||
| Astrovirus | <5 y | - | 72-96 h | + | + | + | + | + | Seafood | Mostly during winter | |||||
| Bacterial | Escherichia coli | ETEC | Any age | + | 108 -1010 | 24 h | - | + | + | + | + | - | Causes travelers diarrhea, contains heat-labile toxins (LT) and heat-stable toxins (ST) | ||
| EPEC | <1 y | - | 10† | 6-12 h | - | + | + | + | + | Raw beef and chicken | - | ||||
| EIEC | Any ages | - | 10† | 24 h | + | + | + | + | + | Hamburger meat and unpasteurized milk | Similar to shigellosis, can cause bloody diarrhea | ||||
| EHEC | Any ages | - | 10 | 3-4 d | - | + | + | + | + | Undercooked or raw hamburger (ground beef) | Known as E. coli O157:H7, can cause HUS/TTP. | ||||
| EAEC | Any ages | + | 1010 | 8-18 h | - | - | + | + | + | - | May cause prolonged or persistent diarrhea in children | ||||
| Salmonella sp. | Any ages | + | 1 | 6 to 72 h | + | + | + | + | + | Meats, poultry, eggs, milk and dairy products, fish, shrimp, spices, yeast, coconut, sauces, freshly prepared salad. | Can cause salmonellosis or typhoid fever. | ||||
| Shigella sp. | Any ages | - | 10 - 200 | 8-48 h | + | + | + | + | + | Raw foods, for example, lettuce, salads (potato, tuna, shrimp, macaroni, and chicken) | Some strains produce enterotoxin and Shiga toxin similar to those produced by E. coli O157:H7 | ||||
| Campylobacter sp. | <5 y, 15-29 y | - | 104 | 2-5 d | + | + | + | + | + | Undercooked poultry products, unpasteurized milk and cheeses made from unpasteurized milk, vegetables, seafood and contaminated water. | May cause bacteremia, Guillain-Barré syndrome (GBS), hemolytic uremic syndrome (HUS) and recurrent colitis | ||||
| Yersinia enterocolitica | <10 y | - | 104 -106 | 1-11 d | + | + | + | + | + | Meats (pork, beef, lamb, etc.), oysters, fish, crabs, and raw milk. | May cause reactive arthritis; glomerulonephritis; endocarditis; erythema nodosum.
can mimic appendicitis and mesenteric lymphadenitis. | ||||
| Clostridium perfringens | Any ages | > 106 | 16 h | - | - | + | + | + | Meats (especially beef and poultry), meat-containing products (e.g., gravies and stews), and Mexican foods. | Can survive high heat, | |||||
| Vibrio cholerae | Any ages | - | 106-1010 | 24-48 h | - | + | + | + | + | Seafoods, including molluscan shellfish (oysters, mussels, and clams), crab, lobster, shrimp, squid, and finfish. | Hypotension, tachycardia, decreased skin turgor. Rice-water stools | ||||
| Parasites | Protozoa | Giardia lamblia | 2-5 y | + | 1 cyst | 1-2 we | - | - | + | + | + | Contaminated water | May cause malabsorption syndrome and severe weight loss | ||
| Entamoeba histolytica | 4-11 y | + | <10 cysts | 2-4 we | - | + | + | + | + | Contaminated water and raw foods | May cause intestinal amebiasis and amebic liver abscess | ||||
| Cryptosporidium parvum | Any ages | - | 10-100 oocysts | 7-10 d | + | + | + | + | + | Juices and milk | May cause copious diarrhea and dehydration in patients with AIDS especially with 180 > CD4 | ||||
| Cyclospora cayetanensis | Any ages | + | 10-100 oocysts | 7-10 d | - | + | + | + | + | Fresh produce, such as raspberries, basil, and several varieties of lettuce. | More common in rainy areas | ||||
| Helminths | Trichinella spp | Any ages | - | Two viable larvae (male and female) | 1-4 we | - | + | + | + | + | Undercooked meats | More common in hunters or people who eat traditionally uncooked meats | |||
| Taenia spp | Any ages | - | 1 larva or egg | 2-4 m | - | + | + | + | + | Undercooked beef and pork | Neurocysticercosis: Cysts located in the brain may be asymptomatic or seizures, increased intracranial pressure, headache. | ||||
| Diphyllobothrium latum | Any ages | - | 1 larva | 15 d | - | - | - | + | + | Raw or undercooked fish. | May cause vitamin B12 deficiency | ||||
8Small bowel diarrhea: watery, voluminous with less than 5 WBC/high power field
Large bowel diarrhea: Mucousy and/or bloody with less volume and more than 10 WBC/high power field
† It could be as high as 1000 based on patient's immunity system.
The table below summarizes the findings that differentiate inflammatory causes of chronic diarrhea[3][4][5][6][6]
| Cause | History | Laboratory findings | Diagnosis | Treatment |
|---|---|---|---|---|
| Diverticulitis |
|
|
Abdominal CT scan with oral and intravenous (IV) contrast | bowel rest, IV fluid resuscitation, and broad-spectrum antimicrobial therapy which covers anaerobic bacteria and gram-negative rods |
| Ulcerative colitis |
|
|
Endoscopy | Induction of remission with mesalamine and corticosteroids followed by the administration of sulfasalazine and 6-Mercaptopurine depending on the severity of the disease. |
| Entamoeba histolytica |
|
cysts shed with the stool | detects ameba DNA in feces | Amebic dysentery
Luminal amebicides for E. histolytica in the colon:
For amebic liver abscess:
|
References
- ↑ 1.0 1.1 1.2 Le Blancq SM, Kase RS, Van der Ploeg LH (1991). "Analysis of a Giardia lamblia rRNA encoding telomere with [TAGGG]n as the telomere repeat". Nucleic Acids Res. 19 (20): 5790. PMC 328996. PMID 1840670.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 "Public Health Image Library (PHIL)".
- ↑ Konvolinka CW (1994). "Acute diverticulitis under age forty". Am J Surg. 167 (6): 562–5. PMID 8209928.
- ↑ Silverberg MS, Satsangi J, Ahmad T, Arnott ID, Bernstein CN, Brant SR; et al. (2005). "Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a Working Party of the 2005 Montreal World Congress of Gastroenterology". Can J Gastroenterol. 19 Suppl A: 5A–36A. PMID 16151544.
- ↑ Satsangi J, Silverberg MS, Vermeire S, Colombel JF (2006). "The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications". Gut. 55 (6): 749–53. doi:10.1136/gut.2005.082909. PMC 1856208. PMID 16698746.
- ↑ 6.0 6.1 Haque R, Huston CD, Hughes M, Houpt E, Petri WA (2003). "Amebiasis". N Engl J Med. 348 (16): 1565–73. doi:10.1056/NEJMra022710. PMID 12700377.
![SEM depicts the dorsal surface of a Giardia protozoan, isolated from a rat’s intestine. From Public Health Image Library (PHIL). [2]](/images/b/b7/Giardiasis09.jpeg)
![SEM depicts the mucosal surface of the small intestine of a gerbil infested with Giardia sp. protozoa. From Public Health Image Library (PHIL). [2]](/images/3/36/Giardiasis08.jpeg)
![SEM depicts a Giardia lamblia protozoan in a late stage of cell division that was about to become two separate organisms, producing a heart-shaped form. From Public Health Image Library (PHIL). [2]](/images/2/24/Giardiasis07.jpeg)
![SEM depicts the ventral surface of a Giardia muris trophozoite. From Public Health Image Library (PHIL). [2]](/images/0/05/Giardiasis06.jpeg)
![SEM depicts dorsal surface of a Giardia protozoan, isolated from a rat’s intestine. From Public Health Image Library (PHIL). [2]](/images/e/e5/Giardiasis05.jpeg)
![SEM depicts some of the ultrastructural morphologic details of an oblong-shaped Giardia sp. protozoan cyst. From Public Health Image Library (PHIL). [2]](/images/1/1c/Giardiasis04.jpeg)
![SEM depicts the ventral surface of a Giardia muris trophozoite that had settled atop the mucosal surface of a rat’s intestine. From Public Health Image Library (PHIL). [2]](/images/9/9e/Giardiasis03.jpeg)
![SEM depicts a Giardia lamblia protozoan that was about to become two separate organisms, as it was caught in a late stage of cell division. From Public Health Image Library (PHIL). [2]](/images/2/2e/Giardiasis02.jpeg)
![SEM depicts a Giardia muris protozoan adhering itself to the microvillous border of an intestinal epithelial cell. From Public Health Image Library (PHIL). [2]](/images/f/f4/Giardiasis01.jpeg)
![This photomicrograph depicts Giardia lamblia parasites using indirect immunofluorescence test for giardiasis. From Public Health Image Library (PHIL). [2]](/images/5/55/Giardiasis10.jpeg)