Gastroesophageal reflux disease pathophysiology
|
Gastroesophageal reflux disease Microchapters |
|
Differentiating Gastroesophageal Reflux Disease from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Gastroesophageal reflux disease pathophysiology On the Web |
|
American Roentgen Ray Society Images of Gastroesophageal reflux disease pathophysiology |
|
Directions to Hospitals Treating Gastroesophageal reflux disease |
|
Risk calculators and risk factors for Gastroesophageal reflux disease pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Ahmed Elsaiey, MBBCH [2]
Overview
Pathophysiology of GERD depends on several mechanisms that lead to the retrograde movement of the acidic content of the stomach to the esophagus. These mechanisms include transient lower esophageal sphincter relaxation, hypotensive lower esophageal sphincter, hiatal hernia, and prolonged esophageal acid clearance.
Pathophysiology
Normal physiology of the food motility through the esophagus
- The esophagus is a part of the gastrointestinal tract which is responsible of moving the food from the mouth to the rectum.[1]
- The esophagus has anti-reflux barrier which prevents the return of the acidic contentof the stomach back to the esophagus. The anti-reflux barrier consists of the lower esophageal sphincter (LES) and the related part of the diaphragm.
- The lower esophageal sphincter is contracting smooth muscle at the end of the esophagus responsible for the food passage to the stomach. LES has high pressure tone which helps keeping it a strong barrier between the esophagus and the stomach.

Pathogenesis
- Pathogenesis of GERD depends on various mechanisms that lead to the reflux of the gastric acidic contents into the esophagus.
- Several mechanisms impair the anti-reflux barrier and cause esophageal dysmotility. These mechanisms include the following:[2][3]
- Transient lower esophageal sphincter relaxations
- Hypotensive lower esophageal sphincter
- Hiatus hernia
- Impaired esophageal acid clearance
- Delayed gastric emptying
Transient lower esophageal sphincter relaxations
- Transient lower esophageal sphincter relaxations is considered the main mechanism of GERD development in most of the patients. It occurs alongside a normal LES and more common with obesity. [4]
- Distension of the stomach worsens the case of transient lower esophageal sphincter relaxation. The diaphragm is also affected by the sphincter relaxation leading to diaphragm inhibition. [5]
- Some of the GERD patients have hypotensive lower esophageal sphincter which leads to retrograde movement of the gastric content into the esophagus.
Hiatal hernia
- A hiatal hernia occurs as part of the stomach is dislocated into the chest. This dislocation leads to placement of the LES above the diaphragm impairing the acid clearance.[6]
- Increase the exposure of the lower esophagus due to a hiatal hernia plays a big role in the pathogenesis of GERD.
Impaired mucosal resistance
- The esophagus has pre-epithelial and epithelial defensive mechanisms against the acidic components that can lead to esophageal injury. However, these defensive mechanisms are limited and weak to stand against injury in case of excessive acid exposure.
- In case of an excessive increase of the noxious agents more than the ability of the mucosal defensive mechanism to eliminate them, mucosal injury occurs and GERD develops.
- The gastric acid leads to erosion of the esophageal mucosa and destruction of the intercellular junctions which leads to increase cellular permeability. The increase in the cellular permeability is proved by the dilation of the intercellular spaces and explains the typical symptoms (e.g, heartburn) of GERD.
Associated Conditions
The most important conditions and diseases associated with GERD include the following: [7][8]
Gross pathology
Findings in gross pathology of GERD include the following:
- Erythematous esophageal mucosa
- Erosions
- Ulcerations in severe cases
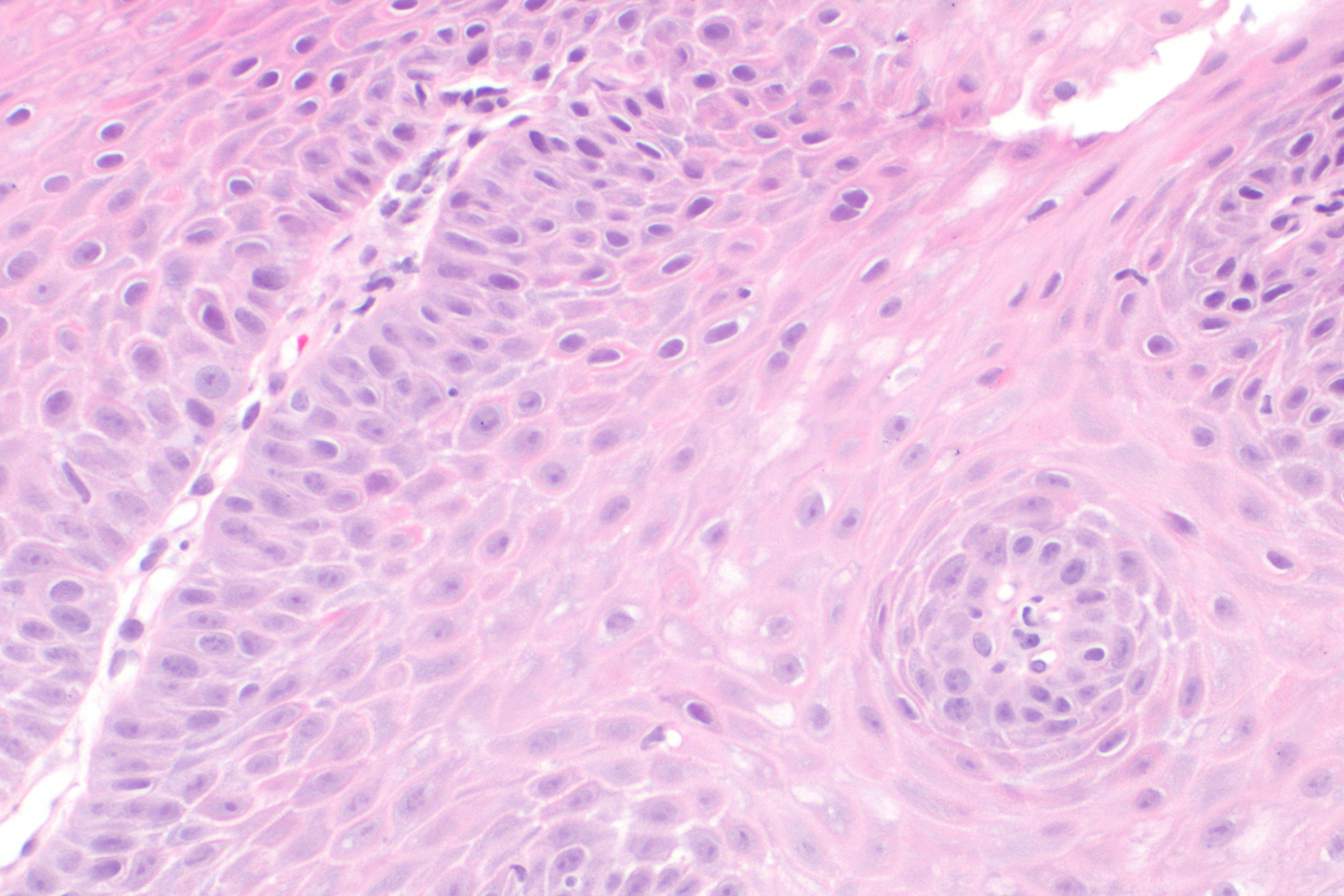
Microscopic pathology
Biopsies can be performed during gastroscopy and these may show:
- Edema and basal hyperplasia (non-specific inflammatory changes)
- Lymphocytic inflammation (non-specific)
- Neutrophilic inflammation (usually due to reflux or Helicobacter gastritis)
- Eosinophilic inflammation (usually due to reflux)
- Goblet cell intestinal metaplasia or Barrett's esophagus.
- Elongation of the papillae
- Thinning of the squamous cell layer
- Dysplasia or pre-cancer.
- Carcinoma.
References
- ↑ Stein HJ, DeMeester TR (1992). "Outpatient physiologic testing and surgical management of foregut motility disorders". Curr Probl Surg. 29 (7): 413–555. PMID 1606845.
- ↑ Storr M, Meining A, Allescher HD (2000). "Pathophysiology and pharmacological treatment of gastroesophageal reflux disease". Dig Dis. 18 (2): 93–102. doi:10.1159/000016970. PMID 11060472.
- ↑ De Giorgi F, Palmiero M, Esposito I, Mosca F, Cuomo R (2006). "Pathophysiology of gastro-oesophageal reflux disease". Acta Otorhinolaryngol Ital. 26 (5): 241–6. PMC 2639970. PMID 17345925.
- ↑ Fisher BL, Pennathur A, Mutnick JL, Little AG (1999). "Obesity correlates with gastroesophageal reflux". Dig Dis Sci. 44 (11): 2290–4. PMID 10573376.
- ↑ Kahrilas PJ, Shi G, Manka M, Joehl RJ (2000). "Increased frequency of transient lower esophageal sphincter relaxation induced by gastric distention in reflux patients with hiatal hernia". Gastroenterology. 118 (4): 688–95. PMID 10734020.
- ↑ Richter J (1999). "Do we know the cause of reflux disease?". Eur J Gastroenterol Hepatol. 11 Suppl 1: S3–9. PMID 10443906.
- ↑ Morse CA, Quan SF, Mays MZ, Green C, Stephen G, Fass R (2004). "Is there a relationship between obstructive sleep apnea and gastroesophageal reflux disease?". Clin. Gastroenterol. Hepatol. 2 (9): 761–8. PMID 15354276.
- ↑ Kasasbeh A, Kasasbeh E, Krishnaswamy G (2007). "Potential mechanisms connecting asthma, esophageal reflux, and obesity/sleep apnea complex--a hypothetical review". Sleep Med Rev. 11 (1): 47–58. doi:10.1016/j.smrv.2006.05.001. PMID 17198758.