Fetal alcohol syndrome
For patient information, click here
|
WikiDoc Resources for Fetal alcohol syndrome |
|
Articles |
|---|
|
Most recent articles on Fetal alcohol syndrome Most cited articles on Fetal alcohol syndrome Review articles on Fetal alcohol syndrome Articles on Fetal alcohol syndrome in N Eng J Med, Lancet, BMJ |
|
Media |
|
Powerpoint slides on Fetal alcohol syndrome Images of Fetal alcohol syndrome Photos of Fetal alcohol syndrome |
|
Evidence Based Medicine |
|
Cochrane Collaboration on Fetal alcohol syndrome |
|
Clinical Trials |
|
Ongoing Trials on Fetal alcohol syndrome at Clinical Trials.gov Trial results on Fetal alcohol syndrome Clinical Trials on Fetal alcohol syndrome at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Fetal alcohol syndrome NICE Guidance on Fetal alcohol syndrome
|
|
Books |
|
News |
|
Fetal alcohol syndrome in the news |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Fetal alcohol syndrome Discussion groups on Fetal alcohol syndrome Patient Handouts on Fetal alcohol syndrome Directions to Hospitals Treating Fetal alcohol syndrome Risk calculators and risk factors for Fetal alcohol syndrome
|
|
Healthcare Provider Resources |
|
Symptoms of Fetal alcohol syndrome Causes & Risk Factors for Fetal alcohol syndrome |
|
Continuing Medical Education (CME) |
|
International |
|
Fetal alcohol syndrome en Espanol Fetal alcohol syndrome en Francais
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Aditya Ganti M.B.B.S. [2]
Overview
Fetal alcohol spectrum disorders (FASDs) are a group of disorders that encompass fetal alcohol syndrome (FAS), partial fetal alcohol syndrome, alcohol-related birth defects (ARBD), alcohol-related neurodevelopmental disorder (ARND), and neurobehavioral disorder associated with prenatal alcohol exposure (ND-PAE). The most potent risk factor for FASD's include prenatal exposure to alcohol. FASD's is the leading preventable cause of birth defects and intellectual and neurodevelopmental disabilities in children. Early recognition, diagnosis, and therapy for FASD is associated with improved outcomes.
History
- In 1899. Dr William Sullivan, a Liverpool prison physician was the first to report a case study describing an association between maternal alcohol use and fetal damage in female prisoners.[1]
- In 1968, Fetal alcohol syndrome was discovered and separated as a entire new diseases at the University of Washington’s Harborview Medical Center in Washington.
- By 1973, sufficient research evidence had accrued to devise basic diagnostic criteria such that FAS became established as a diagnostic entity.[2][3]
- In 1973, Dr keneth Lyons Jones and David W Smith professors of University of Washington Medical School in Seattle was the first to introduce the term Fetal alcohol syndrome.[4]
- By 1978, 245 cases of FAS had been reported by medical researchers, and the syndrome began to be described as the most frequent known cause of mental retardation.
- In 1981, The US Surgeon General issued the first public health advisory that alcohol during pregnancy is responsible birth defects.
- In 1989, US Congress mandated warning labels about potential birth defects on alcohol products.
Classification
According to American Academy of Pediatrics fetal alcohol spectrum disorders (FASDs) encompasses group of disorders based upon the manifestations into 5 sub types.
- Fetal alcohol syndrome (FAS)
- Partial fetal alcohol syndrome
- Alcohol-related birth defects (ARBD)
- Alcohol-related neurodevelopmental disorder (ARND)
- Neurobehavioral disorder associated with prenatal alcohol exposure (ND-PAE).
| Fetal alcohol spectrum disorders | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Fetal alcohol syndrome (FAS) | Partial fetal alcohol syndrome | Alcohol-related birth defects (ARBD) | Alcohol-related neurodevelopmental disorder (ARND) | Neurobehavioral disorder associated with prenatal alcohol exposure (ND-PAE) | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| A▪ Confirmed maternal alcohol exposure. B▪ Evidence of characteristic pattern of facial anomalies C▪ Evidence of growth retardation D▪ Evidence of CNS abnormalities | A, B, C, D and E▪ Evidence of a complex pattern of behavior or cognitive abnormalities | ▪ Cardiac ▪ Skeletal ▪ Renal ▪ Ocular ▪ Auditory ▪ Other | A,B, D, and E ▪ No growth retardation | Behavioral abnormalities predominant with no growth retardation | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Pathophysiology
- Drinking alcohol during pregnancy is the most potent etiological factor for the development of fetal alcohol syndrome disorders.
- The developing embryo is susceptible to dysmorphogenisis during the first few weeks of pregnancy.
- Alcohol can pass through umbilical cord to the baby effecting morphogeneisis leading to
- Miscarriage
- Stillbirth
- Behavioral, and intellectual disabilities
Risk Factors
The most potent risk factor in the development of FASD's include prenatal exposure of alcohol. Other risk factors include:
- Alcohol consumption
- Increase in maternal age
- Maternal genotype|
- Increase in parity/gravidity
- Higher birth order of the child
- Low socioeconomic status
Epidemiology and Demographics
Prevalence
- According to National Institute on Alcohol Abuse and Alcoholism study, CDC and AAP it is estimated that FASD's is prevalent in 2-5% of children in the United States.
- CDC released a fact sheet in 2016, according to which prevalence of fetal alcohol syndrome is believed to be 1 in 20 children.
- Comprehensive data on the number of individuals with an FASD in the general population of the Unites States, or by state, race or ethnicity, is currently not available.
- Journal of the American Medical Association published the results of a National Institute on Alcohol Abuse and Alcoholism study that measured the prevalence of fetal alcohol spectrum disorders (FASD) among first-grade students in four US communities.
- Over 6,500 children were evaluated and the most conservative estimate for FASD ranged from 1 to 5 percent, or 1 in 20 students.
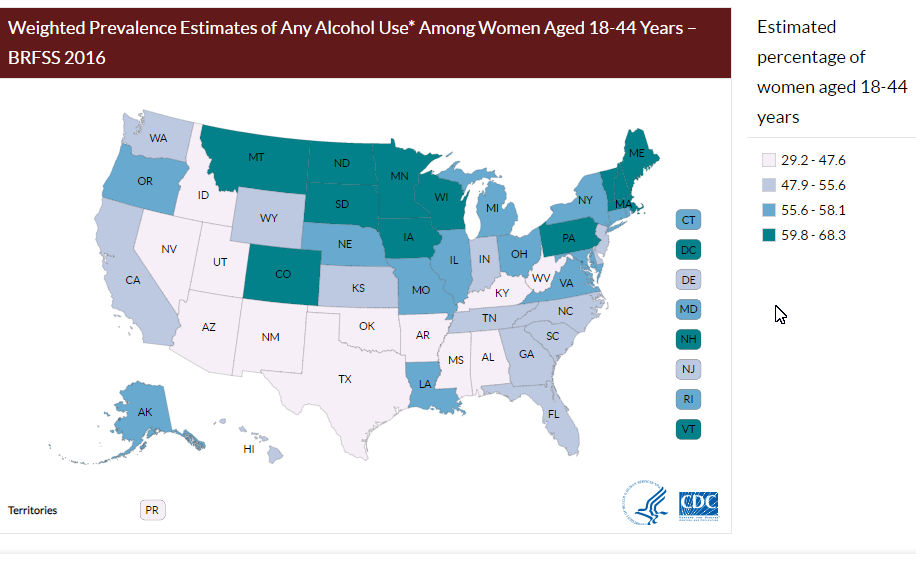
- Data from the Centers for Disease Control and Prevention (CDC) asserts that 10 percent of pregnant women report drinking alcohol and 3 percent report binge drinking, putting over 100,000 births in the US each year at high risk for FASD.
Differential Diagnosis
Fetal alcohol syndrome must be differentiated from other genetic diseases, with similar manifestations such as smooth philtrum, thin vermillion border and small palpebral fissures. American academy of pediatrics and CDC reviewed and recommended 9 genetic diseases that has to screened and differentiated from FAD's which include Aarskog syndrome, Williams syndrome, Noonan syndrome, Dubowitz syndrome, Brachman-DeLange syndrome, Toluene syndrome, Fetal hydantoin syndrome, Fetal valproate syndrome, and Maternal PKU fetal effects.
| Syndrome | Overlapping features | Differentiating features |
|---|---|---|
| Aarskog syndrome |
|
|
| Williams syndrome |
|
|
| Noonan syndrome |
|
|
| Dubowitz syndrome |
|
|
| Brachman-DeLange syndrome |
|
|
| Toluene syndrome |
|
|
| Fetal hydantoin syndrome |
|
|
| Fetal valproate syndrome |
|
|
| Maternal PKU fetal effects |
|
|
The following tables summarizes the differential diagnosis of individual features associated with FAS
| Differential diagnosis of individual features associated with FAS | |
|---|---|
| Smooth philtrum |
|
| Thin Vermillion border |
|
| Small palpebral fissures |
|
Diagnosis
FASD is clinical diagnosis and there are no specific diagnostic laboratory findings associated with FASD. However, American Academy of Pediatrics and CDC brought up a diagnostic criteria. [5][6][7][8][9][10][11]
Diagnostic criteria for Fetal alcohol spectral disorders
| Components of Diagnostic criteria For FASD's | ||
|---|---|---|
| Growth deficiency |
| |
| Facial features |
| |
| Central nervous system damage | Structural |
|
| Neurological | Neurological problems not due to:
| |
| Functional | Global cognitive or intellectual deficits representing multiple domains of deficit with performance below the 3rd percentile | |
Functional deficits below the 16th percentile in at least three of the following domains:
| ||
| Maternal alcohol exposure |
| |
Diagnostic criteria for Fetal alcohol syndrome
4 diagnostic criteria had been developed in the recent times to diagnose fetal alcohol syndrome
- Four digit code
- Hoyme- Revised IOM
- Chudley–Canadian
- National Task Force/CDC
| Fetal alcohol syndrome | |||
|---|---|---|---|
| Facial Characterstics | Growth retardation | CNS involvement | |
| Four digit code | Simultaneous presentation of
|
Height or weight ≤10th percentile |
|
| Hoyme–Revised IOM | ≥2 of the following
|
Height or weight ≤10th percentile |
|
| Chudley–Canadian | Simultaneous presentation of
|
Height or weight or disproportionately low weight-to-height ratio (≤10th percentile) | Evidence of ≥3 impairments in the following CNS domains
|
| National Task Force/CDC | Simultaneous presentation of
|
Height or weight ≤10th percentile at any point in time. |
|
History and Symptoms
| Alcohol exposure | CNS abnormalities | Facial anomalies | Growth retardation | |
|---|---|---|---|---|
| Fetal alcohol syndrome (FAS) | + | Severe | + | + |
| Partial fetal alcohol syndrome | + | Severe | + | - |
| Alcohol-related neurodevelopmental disorder (ARND) | + | Severe | - | - |
| Neurobehavioral disorder associated with prenatal alcohol exposure (ND-PAE). | + | Moderate | - |
Common symptoms of FASDs include :[16][17][16][3][15][13][14]
- Abnormal facial features, such as a smooth ridge between the nose and upper lip (this ridge is called the philtrum)
- Small head size
- Shorter-than-average height
- Low body weight
- Poor coordination
- Hyperactive behavior
- Difficulty with attention
- Poor memory
- Difficulty in school (especially with math)
- Learning disabilities
- Speech and language delays
- Intellectual disability or low IQ
- Poor reasoning and judgment skills
- Sleep and sucking problems as a baby
- Vision or hearing problems
- Problems with the heart, kidneys, or bones
Prognosis
| Prognosis | |
|---|---|
| Primary disabilities |
|
| Secondary disabilities |
|
| Protective factors and strengths | Eight factors were identified as universal protective factors that reduced the incidence rate of the secondary disabilities:[20][1]
|
Treatment
There is no specific cure for FAS as the CNS damage is irreversible leading to permanent disability. Treatment can be focused on halting the progression and behavioral therapy to improve the quality of life.[21][22][23][24][25][26][27]
- Management of fetal alcohol spectrum disorders classically is divided into two main areas.
- Pre-conceptual: Recognition of the dangers of alcohol consumption in [pregnancy]] and the prevention of damage to the fetus.
- Post diagnosis: Relates to the management of people who have the condition.
Behavioral management of FASD can be summarized in the following table:
| Time Period For Intervention | |||
|---|---|---|---|
| Pre-Conception | During Pregnancy | Childhood 0-18 | Adult 18+ |
|
|
|
|
| Treatment | |
|---|---|
| Medical interventions | Due to overlapping symptoms between other diseases such as ADHD, traditional medical interventions (i.e., psychoactive drugs) are frequently tried.
|
| Behavioral interventions | Following are behavior and education therapies that have been shown to be effective for some children with FASDs:
Good Buddies
Families Moving Forward (FMF) program to provide support for families who deal with challenging FASD behaviors
Math Interactive Learning Experience (MILE) program to help with mathematics difficulty
Parents and Children Together (PACT) a neurocognitive habilitation program to improve self-regulation and executive function
|
| Parent Training | Children with FASDs might not respond to the usual parenting practices. However, the following parenting tips are recommended:
|
| Alternative therapies | |
Prevention
The only certain way to prevent FAS is to simply avoid drinking alcohol during pregnancy.[1] Some studies have shown that light to moderate drinking during pregnancy might not pose a risk to the fetus, although no amount of alcohol during pregnancy can be guaranteed to be absolutely safe. The Royal College of Obstetricians and Gynaecologists conducted a study of over 400,000 women, all of whom had consumed alcohol during pregnancy. No case of fetal alcohol syndrome occurred and no adverse effects on children were found when consumption was under 8.5 drinks per week. A review of research studies found that fetal alcohol syndrome only occurred among alcoholics; no apparent risk to the child occurred when the pregnant women consumed no more than one drink per day. A study of moderate drinking during pregnancy found no negative effects and the researchers concluded that one drink per day provides a significant margin of safety, although they did not encourage drinking during pregnancy. A study of pregnancies in eight European countries found that consuming no more than one drink per day did not appear to have any effect on fetal growth. A follow-up of children at 18 months of age found that those from women who drank during pregnancy, even two drinks per day, scored higher in several areas of development. An analysis of seven medical research studies involving over 130,000 pregnancies found that consuming two to 14 drinks per week did not increase the risk of giving birth to a child with either malformations or fetal alcohol syndrome.
In the United States, the Surgeon General recommended in 1981, and again in 2005, that women abstain from alcohol use while pregnant or while planning a pregnancy, the latter to avoid damage in the earliest stages of a pregnancy, as the woman may not be aware that she has conceived.[28] In the United States, federal legislation has required that warning labels be placed on all alcoholic beverage containers since 1988 under the Alcoholic Beverage Labeling Act.
See also
- Fetal Alcohol Spectrum Disorder
- Recommended maximum intake of alcoholic beverages
- Alex Burril's Guide to F.A.S.
References
- ↑ 1.0 1.1 1.2 1.3 Invalid
<ref>tag; no text was provided for refs namedFASGuide - ↑ Invalid
<ref>tag; no text was provided for refs namedforeword - ↑ 3.0 3.1 Invalid
<ref>tag; no text was provided for refs namedIOM - ↑ Invalid
<ref>tag; no text was provided for refs namedJonesetal1973 - ↑ Cook JL, Green CR, Lilley CM, Anderson SM, Baldwin ME, Chudley AE, Conry JL, LeBlanc N, Loock CA, Lutke J, Mallon BF, McFarlane AA, Temple VK, Rosales T (February 2016). "Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan". CMAJ. 188 (3): 191–7. doi:10.1503/cmaj.141593. PMC 4754181. PMID 26668194.
- ↑ Hoyme HE, Kalberg WO, Elliott AJ, Blankenship J, Buckley D, Marais AS, Manning MA, Robinson LK, Adam MP, Abdul-Rahman O, Jewett T, Coles CD, Chambers C, Jones KL, Adnams CM, Shah PE, Riley EP, Charness ME, Warren KR, May PA (August 2016). "Updated Clinical Guidelines for Diagnosing Fetal Alcohol Spectrum Disorders". Pediatrics. 138 (2). doi:10.1542/peds.2015-4256. PMC 4960726. PMID 27464676.
- ↑ Astley SJ, Clarren SK (2000). "Diagnosing the full spectrum of fetal alcohol-exposed individuals: introducing the 4-digit diagnostic code". Alcohol Alcohol. 35 (4): 400–10. PMID 10906009.
- ↑ Chudley AE, Conry J, Cook JL, Loock C, Rosales T, LeBlanc N (March 2005). "Fetal alcohol spectrum disorder: Canadian guidelines for diagnosis". CMAJ. 172 (5 Suppl): S1–S21. doi:10.1503/cmaj.1040302. PMC 557121. PMID 15738468.
- ↑ Hoyme HE, May PA, Kalberg WO, Kodituwakku P, Gossage JP, Trujillo PM, Buckley DG, Miller JH, Aragon AS, Khaole N, Viljoen DL, Jones KL, Robinson LK (January 2005). "A practical clinical approach to diagnosis of fetal alcohol spectrum disorders: clarification of the 1996 institute of medicine criteria". Pediatrics. 115 (1): 39–47. doi:10.1542/peds.2004-0259. PMC 1380311. PMID 15629980.
- ↑ Hagan JF, Balachova T, Bertrand J, Chasnoff I, Dang E, Fernandez-Baca D, Kable J, Kosofsky B, Senturias YN, Singh N, Sloane M, Weitzman C, Zubler J (October 2016). "Neurobehavioral Disorder Associated With Prenatal Alcohol Exposure". Pediatrics. 138 (4). doi:10.1542/peds.2015-1553. PMC 5477054. PMID 27677572.
- ↑ Hoyme HE, Coles CD (October 2016). "Alcohol-Related Neurobehavioral Disabilities: Need for Further Definition and Common Terminology". Pediatrics. 138 (4). doi:10.1542/peds.2016-1999. PMC 5051212. PMID 27677571.
- ↑ Invalid
<ref>tag; no text was provided for refs namedgrowthchart - ↑ 13.0 13.1 Invalid
<ref>tag; no text was provided for refs namedCDC - ↑ 14.0 14.1 Invalid
<ref>tag; no text was provided for refs namedCanadian - ↑ 15.0 15.1 Invalid
<ref>tag; no text was provided for refs named4digitcode - ↑ 16.0 16.1 Invalid
<ref>tag; no text was provided for refs namedMattson10 - ↑ Invalid
<ref>tag; no text was provided for refs namedJones1973 - ↑ Invalid
<ref>tag; no text was provided for refs namedMalbinTry - ↑ Invalid
<ref>tag; no text was provided for refs namedMalbinFAE - ↑ 20.0 20.1 Invalid
<ref>tag; no text was provided for refs named2disabilities - ↑ Bertrand J, Floyd LL, Weber MK (October 2005). "Guidelines for identifying and referring persons with fetal alcohol syndrome". MMWR Recomm Rep. 54 (RR-11): 1–14. PMID 16251866.
- ↑ Bertrand J (2009). "Interventions for children with fetal alcohol spectrum disorders (FASDs): overview of findings for five innovative research projects". Res Dev Disabil. 30 (5): 986–1006. doi:10.1016/j.ridd.2009.02.003. PMID 19327965.
- ↑ Peadon E, Rhys-Jones B, Bower C, Elliott EJ (May 2009). "Systematic review of interventions for children with Fetal Alcohol Spectrum Disorders". BMC Pediatr. 9: 35. doi:10.1186/1471-2431-9-35. PMC 2698825. PMID 19463198.
- ↑ Kodituwakku PW, Kodituwakku EL (June 2011). "From research to practice: an integrative framework for the development of interventions for children with fetal alcohol spectrum disorders". Neuropsychol Rev. 21 (2): 204–23. doi:10.1007/s11065-011-9170-1. PMID 21544706.
- ↑ Masotti P, Longstaffe S, Gammon H, Isbister J, Maxwell B, Hanlon-Dearman A (October 2015). "Integrating care for individuals with FASD: results from a multi-stakeholder symposium". BMC Health Serv Res. 15: 457. doi:10.1186/s12913-015-1113-8. PMC 4594899. PMID 26438317.
- ↑ Olson HC, Oti R, Gelo J, Beck S (2009). ""Family matters:" fetal alcohol spectrum disorders and the family". Dev Disabil Res Rev. 15 (3): 235–49. doi:10.1002/ddrr.65. PMID 19731388.
- ↑ Kalberg WO, Buckley D (2007). "FASD: what types of intervention and rehabilitation are useful?". Neurosci Biobehav Rev. 31 (2): 278–85. doi:10.1016/j.neubiorev.2006.06.014. PMID 16919732.
- ↑ Invalid
<ref>tag; no text was provided for refs namedSG
Further reading
- Astley S (2004). "Fetal alcohol syndrome prevention in Washington State: evidence of success". Paediatric and Perintal Epidemiology. 18 (5): 344–51. doi:10.1111/j.1365-3016.2004.00582.x. PMID 15367321.
- Astley S, Clarren S (2001). "Measuring the facial phenotype of individuals with prenatal alcohol exposure: correlations with brain dysfunction". Alcohol and Alcoholism. 36 (2): 147–59. doi:10.1093/alcalc/36.2.147. PMID 11259212.
- Gideon Koren, Idan Roifman, Irena Nullman. Hypothetical Framework; FASD and criminality-causation or association? The limits of evidence based knowledge. Journal of FAS International volume=2, issue=6, year=2004 |http://www.motherisk.org/JFAS/econtent_commonDetail.jsp?econtent_id=59
- Grant T, Ernst C, Streissguth A (1996). "An intervention with high-risk mothers who abuse alcohol and drugs: the Seattle Advocacy Model". American Journal of Public Health. 86 (12): 1816–7. PMID 9003147.
- Mattson, S.N., & Riley, E.P. (2002). Neurobehavioral and Neuroanatomical Effects of Heavy Prenatal Exposure to Alcohol, in Streissguth, A.P., & Kanter, J. (Eds.) The Challenge in Fetal Alcohol Syndrome: Overcoming Secondary Disabilities. First published in 1997. ISBN 0-295-97650-0
- Olegård R, Sabel K, Aronsson M, Sandin B, Johansson P, Carlsson C, Kyllerman M, Iversen K, Hrbek A (1979). "Effects on the child of alcohol abuse during pregnancy. Retrospective and prospective studies". Acta Paediatrica Scandinavica Suppl. 275: 112–21. doi:10.1111/j.1651-2227.1979.tb06170.x. PMID 291283.
- Ratey, J.J. (2001). A User's Guide to the Brain: Perception, Attention, and the Four Theaters of the Brain. New York: Vintage Books. ISBN 0-375-70107-9.
- Ulleland CN, Wennberg RP, Igo RP, Smith NJ (1970). "The offspring of alcoholic mothers". Abstract. American Pediatric Society for Pediatric Research.
Template:Phakomatoses and other congenital malformations not elsewhere classified
de:Fetales Alkoholsyndrom io:FAS-filio it:Sindrome alcolica fetale fi:Fetaalialkoholisyndrooma