Bronchiectasis CT
Jump to navigation
Jump to search
|
Bronchiectasis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Bronchiectasis CT On the Web |
|
American Roentgen Ray Society Images of Bronchiectasis CT |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Hamid Qazi, MD, BSc [2], Saarah T. Alkhairy, M.D.
Overview
High-resolution computed tomography (HRCT) is the preferred diagnostic tool in identifying bronchiectasis. Common findings include increased diameter of a bronchus, tree-in-bud abnormalities, and cysts with definable borders.
Bronchiectasis CT
- The diagnosis of bronchiectasis is based on the review of clinical history and characteristic patterns in the HRCT findings
- The internal diameter of a bronchus is >1.5 times (>150%) the diameter of the pulmonary artery (also known as the ‘signet ring’ pattern)[1]
- Bronchial wall thickening (parallel tram lines)
- "Tree-in-bud" appearance
- Failure of bronchial tapering
- Crowding of bronchi with lobar volume loss
- Thickening an plugging of small airways
- Cysts with definable borders
- Bronchiectasis may also be diagnosed without CT scan confirmation if clinical history clearly demonstrates frequent, respiratory infections, as well as confirmation of an underlying problem via blood work and sputum culture samples[2]
CT scan
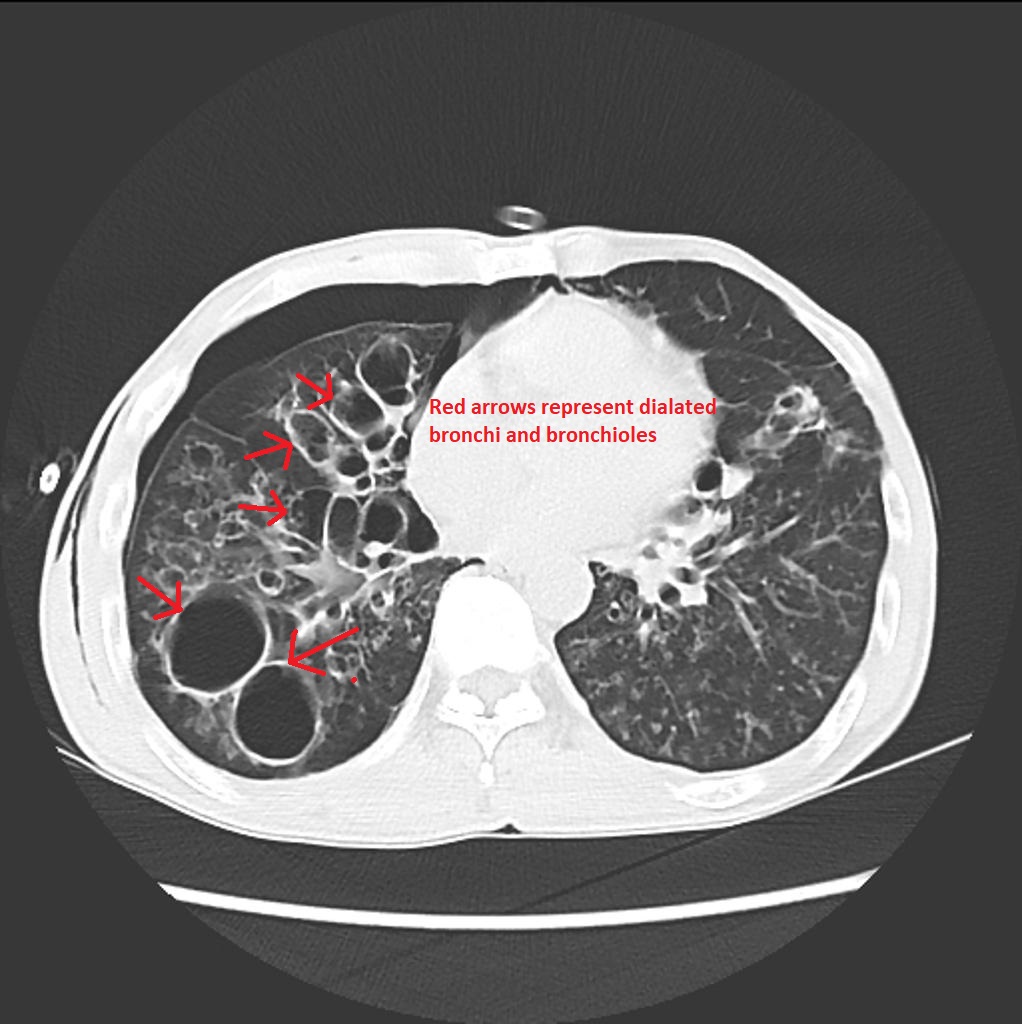
References
- ↑ McDonnell MJ, Ward C, Lordan JL, Rutherford RM (2013). "Non-cystic fibrosis bronchiectasis". QJM. 106 (8): 709–15. doi:10.1093/qjmed/hct109. PMID 23728208.
- ↑ Miller, JC (2006). "Pulmonary Mycobacterium Avium-Intracellular Infections in Women". Radiology Rounds. 4 (2).