Blalock-Taussig shunt: Difference between revisions
Sara Mohsin (talk | contribs) No edit summary |
Sara Mohsin (talk | contribs) |
||
| Line 8: | Line 8: | ||
==Overview== | ==Overview== | ||
The '''Blalock-Taussig shunt''' is a [[surgical procedure]] that are done as [[Palliative treatment|palliative]] procedures for [[cyanotic heart defect]]s. This procedure is used to deviate blood flow to lungs from the systemic circulation to relieve [[cyanosis]] while a definitive [[corrective surgery]] can be performed at a later time. Connection between [[subclavian artery]] and [[pulmonary artery]] is usually made. There are usually two types of [[Shunt (medical)|shunts]] that are used i.e classic or original Blalock-Taussig shunt and modified Blalock Taussig shunt. The classic or original BT shunt has been modified into modified Blalock-Taussig Shunt (mBTS). In this modified procedure a [[graft]] from [[innominate artery]] or [[subclavian artery]] is placed to the corresponding [[pulmonary artery]]. This type of BT shunt has superior [[Prognosis|prognostic]] value over classical shunt leading to a greater rate of shunt patency at 3-5 years as compared to classic or original BT Shunt. | |||
== Historical Perspective == | == Historical Perspective == | ||
Revision as of 16:22, 23 July 2020
|
Blalock-Taussig shunt Microchapters |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Usman Ali Akbar, M.B.B.S.[2]
Synonyms and keywords: Blalock Taussig Procedure,Procedure, Blalock-Taussig,Subclavian Pulmonary Artery Shunt,Blue Baby Operations,Modified Blalock-Taussig Procedure
Overview
The Blalock-Taussig shunt is a surgical procedure that are done as palliative procedures for cyanotic heart defects. This procedure is used to deviate blood flow to lungs from the systemic circulation to relieve cyanosis while a definitive corrective surgery can be performed at a later time. Connection between subclavian artery and pulmonary artery is usually made. There are usually two types of shunts that are used i.e classic or original Blalock-Taussig shunt and modified Blalock Taussig shunt. The classic or original BT shunt has been modified into modified Blalock-Taussig Shunt (mBTS). In this modified procedure a graft from innominate artery or subclavian artery is placed to the corresponding pulmonary artery. This type of BT shunt has superior prognostic value over classical shunt leading to a greater rate of shunt patency at 3-5 years as compared to classic or original BT Shunt.
Historical Perspective
Classic or Original Shunt
- The classic or original BT shunt procedure was named for Alfred Blalock, surgeon, Baltimore, (1899–1964) and Helen B. Taussig, cardiologist, Baltimore/Boston, (1898–1986) who, along with Blalock's African American laboratory technician Vivien Thomas (1910–1985), developed and described the procedure.
- Taussig noticed that the children with cyanosis along with congenital heart disease accompanied by patent ductus arteriosus have longer life time than those without PDA.
- Dr. Taussig approached Blalock and Thomas in their Hopkins laboratory in 1943 to work upon in this shunt as it was hypothesized that a shunt mimicking PDA can relieve the cyanosis and improve oxygenation in congential cyanotic diseases. Thomas, Vivien (1985). Partners of the heart : Vivien Thomas and his work with Alfred Blalock : an autobiography. Philadelphia: University of Pennsylvania Press. ISBN 0812216342.
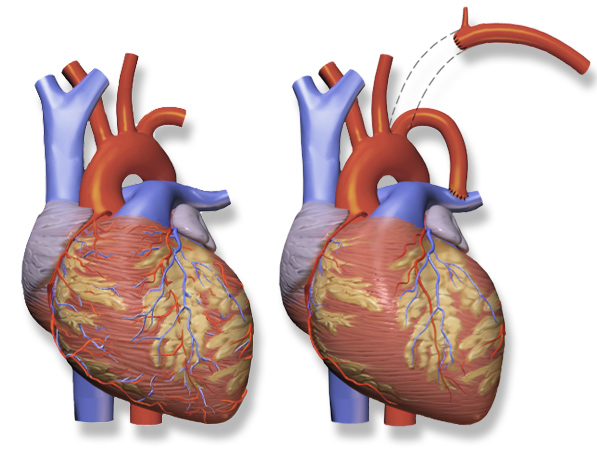
Modified Blalock-Taussig Shunt
A modified method of inserting a shunt was developed in 1962 by Klinner using teflon as prosthetic graft material between the subclavian artery and the pulmonary artery is used to prevent scarring of the subclavian artery. [1]

Classification
Classic/Original Blalock-Taussig Shunt
- For classic Blalock-Taussig shunt end to end anastomosis between the subclavian and pulmonary arteries is performed on opposite to the aortic arch to minimize the kinking of subclavian artery as it crosses aortic prominence.[2]
| Advantages | Disadvantages |
|---|---|
| The relative diameter of subclavian artery prevents excessive blood flow to lungs | Thrombosis of shunt due to less diameter |
| Easily Reversible | Risk of Dissection |
| Increased rate of anastomosis growth | Subclavian artery is lost during the procedure |
Modified Blalock Taussig Shunt
It is the most commonly used procedure now a days. First described and performed by Klinner et. al in 1962, this procedure hold superb prognosis over classic one. An Interposition PTFE or Gore-Tex graft is placed between the subclavian artery and the pulmonary artery. Hence no scarring of subclavian artery results.[2]
| Advantages | Disadvantages |
|---|---|
| It can be done on the same side of the arch | Thrombosis |
| More patency than Classic BT shunt i.e >90 % at 2 years | Pseudoaneurysm |
| Pulmonary artery is less distorted | Chylothorax, Chylopericardium, chylous ascites |
Goals of BT shunt
The ultimate endpoint goals of BT shunt is
- To stabilize the preload hence preventing hemodilution.
- To maintain Systemic Vascular Resistance ( afterload ) hence adequate diastolic pressure to maintain coronary perfusion
- Increase the blood flow to the pulmonary vasculature in a supervised manner
Indications
- Tricuspid atresia
- Tetralogy of Fallot
- Ebstein's Anomaly
- Hypoplastic Left Heart syndrome
- Pulmonary atresia
- Inadequate pulmonary arteries
Risk Factors
Multiple risk factors have been identified which leads to high morbidity and mortality in neonates. [3] [4]
- Sternal approach for MBTS construction
- Univentricular heart
- Complicated surgery(CABG)
- Weight <3 kg
- Pre-op ventilation support
- Pre-op acidosis and shock
- Use of Innominate artery-PA shunt
- Diagnosis of Ebstein's Anomaly
Preparation for BT Shunt
To perform a BT shunt following pre-op preparation is done
- Preoperative psychological counselling of the patient
- Preoperative fasting
- Pre-op medications
Anesthesia induction will be based on the following patient and surgical factors
Patient Related Factors
- Diagnosis of relative congenital cardiac anomaly
- Age of the patient
- Weight <3 kg leads to high mortality and morbidity
- Premature infants
- Any non cardiac coexisting congenital anomaly like Tracheoesophageal fistula , cleft lip and palate , renal anomalies and skeletal defects.
- Atlantoaxial instability or subluxation in down syndrome that should be considered when managing airway.
- Fatigue , dyspnea on feeding or any other factor showing exercise intolerance
- Use of medications that can lead to increase in operative mortality such as aspirin, warfarin , anti-depressants , diuretics ,angiotensin converting enzyme (ACE ) inhibitors, antiarrhythmics
- Congenital conditions such as subglottic stenosis that can lead to difficulty in access for intubation
- Optimal right ventricular function
Factors Related to Surgical Procedure
- Complex lesions leads to high in-hospital and overall mortality.
- Duration of surgery
- Cardiovascular anomalies that can lead to complexity of procedure like aortic arch anomaly or presence of aberrant subclavian artery
- Injury to recurrent laryngeal nerve or phrenic nerve during the procedure
- Nature and approach of cardiac surgery e.g, Cardiopulmonary bypass, sternotomy or thoracotomy
Approach
- For right sided modified Blalock-Taussig shunt (mBTS), left lateral position is used and for left sided mBTS right lateral position is used. The approach used is usually thoracotomy.
- For central shunts sternotomy is performed.
Complications
The immediate post-operative complications include [5]
- Development of chylothorax, chylopericardium and chylous ascites
- Phrenic nerve resection leading to diaphragmatic paralysis
- Anemia
- Congestive Heart failure resulting from excessive blood flow
- Modified PTFE grafts can result in formation of seroma or shunt occlusion due to hyperplasia of neo-intima
- Stenosis of innominate artery
- Sunt Infection resulting into sepsis

Management of Complications
Shunt failure
It is the most immediate risk during the post-operative period. It can lead to drop in oxygen saturation secondary due to shunt thrombosis or kinking. Shunt failure is a surgical emergency and should be managed as following :
- Anticoagulation should be started. Heparin should be instituted promptly. It should be again administered if there is less risk of bleeding usually after 4 hours post-op ( when the drainage of chest shows <3ml/kg/h and aPTT is <60s. Heparin induced thrombocytopenia can occur and should be managed accordingly.
- Patient is put on aspirin which is usually started at 3-5 mg/kg (max. dose 75mg ) OD.
- Heparin should be continued until there is second dose of aspirin.
Blockage of BT shunt
Blockage or shunt thrombosis is another surgical emergency. It's incidence has reported around 12 %. Any recent onset murmur or significant drop in oxygen saturation must be investigated . Operative management is usually required and the shunt is usually repaired or replaced if necessary.
High pulmonary blood flow
The appropriate size of BT shunt is very important to prevent the long term complications regarding to high pulmonary blood flow or high oxygen saturation. Chest X Ray usually shows edematous lungs with low mixed venous saturation , rising lactate levels or signs of right heart failure, systemic diastolic pressure may be low , persistent metabolic acidosis leading to "pink patient" and pulmonary hemorrhage.
Causes
Treatment
Following treatment is instituted.
- For mild to moderate symptoms fluid resuscitation and diuretics is given. Permissive hypercapnia and lowering of FiO2 is done.
- For severe symptoms systemic vascular resistance and pulmonary vascular resistance is adjusted.
- Refractory to medical management cases are usually treated with surgical approach which involves pulmonary artery band or clamping.
Prognosis
Modified Blalock-Taussig Shunt has superior prognostic value over classic Blalock-Taussig Shunts. Following prognostic factors are compared between the two procedures in multiple studies. [6] [7] [8] [9] [10] [11]
- Rise in saturation of oxygen is greater in modified than in classic shunt
- Shunt patency is 88.8 % in modified for 3-5 years versus 90 % in first year, 62 % in two years and 78.0 % in 3 years for classic shunt.
- The risk of early shunt faliure is 20.8 % in modified and 51.7% in classic shunt.
- Post-shunt increase in pulmonary arterial index (mm2/m2) is 158 +/- 21 versus 117 +/- 52 in classic Blalock-Taussig shunt.
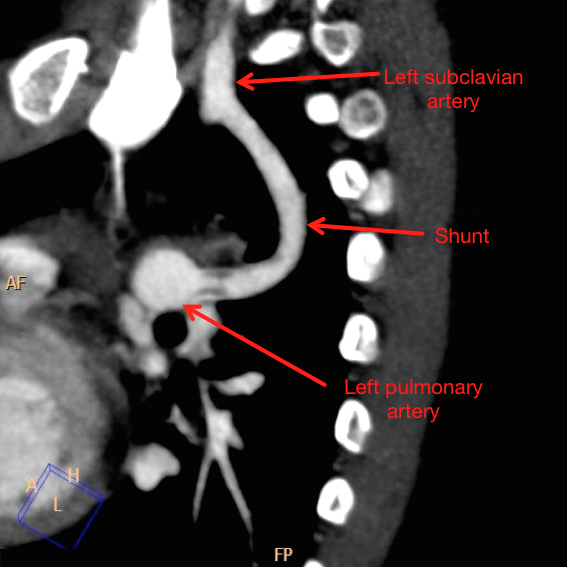
Alternative Shunts
Central Shunt
Central shunt is made by making a anastomosis between ascending aorta and main pulmonary artery. A short PTFE conduit for this purpose is used. It is also known as Mee's shunt. [12] Internal mammary artery is used for this purpose and to create a systemic to pulmonary conduit after there has been failure of previously used BT shunt. It leads to adaptation of growth and flow and reduces the risk for graft infection.
| Advantages | Disadvantages |
|---|---|
| Can be done in small children with small vessels | Can not be performed without in patients without patent ductus arteriosus |
| Distortion of pulmonary vessels is avoided | Entry into pericardium |
| Equal blood flow is provided to both lungs | |
| Low chance of occlusion rate | |
| Subclavian steal syndrome is usually avoided |
Potts shunt
It can be used as an alternative to Classic BT shunt. To avoid the consequences of right heart failure, it has been used as an alternative to offload the right ventricle. This improves the cardiac output but the oxygen saturation is lowered and there is decreased oxygen delivery to lower extremities. Pott's shunt includes a connection that is made between descending aorta and left pulmonary artery. [13]
| Advantages | Disadvantages |
|---|---|
| Subclavian artery is used hence large diameter so surgery can be easily performed | Increased incidence of pulmonary hypertension |
| Lower chance of occlusion than CBTS and mBTS | Increased blood flow to one lung while there is kinking of pulmonary artery |
| Increased risk of congestive heart failure [14] |
Waterston shunt
It is made by connecting the ascending aorta and right pulmonary artery. It has not been clinically performed now due to increased risk of congestive heart failure , pulmonary hypertension and kinking of pulmonary artery
Cooley Shunt
It is an intrapericardial anastomosis between ascending aorta and the right pulmonary artery. Right anterolateral thoracotomy approach is used.
| Advantages | Disadvantages |
|---|---|
| Use of right anterolateral incision for all approaches - Mediastinal dissection is avoided | Improper size of shunt can lead to right heart failure and pulmonary congestion |
| Total repair can be done after this shunt in future | Risk of intracardiac adhesions |
| Complexity of the procedure |
References
- ↑ KLINNER W, PASINI M, SCHAUDIG A (1962). "[Anastomosis between systemic and pulmonary arteries with the aid of plastic prostheses in cyanotic heart diseases]". Thoraxchirurgie. 10: 68–75. doi:10.1055/s-0028-1096482. PMID 14457041.
- ↑ 2.0 2.1 Kiran U, Aggarwal S, Choudhary A, Uma B, Kapoor PM (2017). "The blalock and taussig shunt revisited". Ann Card Anaesth. 20 (3): 323–330. doi:10.4103/aca.ACA_80_17. PMC 5535574. PMID 28701598.
- ↑ Schmoldt A, Benthe HF, Haberland G (1975). "Digitoxin metabolism by rat liver microsomes". Biochem Pharmacol. 24 (17): 1639–41. PMID https://doi.org/10.1016/j.jamcollsurg.2012.12.027 Check
|pmid=value (help). - ↑ Schmoldt A, Benthe HF, Haberland G (1975). "Digitoxin metabolism by rat liver microsomes". Biochem Pharmacol. 24 (17): 1639–41. PMID https://doi.org/10.1016/j.athoracsur.2011.02.030 Check
|pmid=value (help). - ↑ Yuan SM, Shinfeld A, Raanani E (2009). "The Blalock-Taussig shunt". J Card Surg. 24 (2): 101–8. doi:10.1111/j.1540-8191.2008.00758.x. PMID 19040408.
- ↑ Al Jubair KA, Al Fagih MR, Al Jarallah AS, Al Yousef S, Ali Khan MA, Ashmeg A; et al. (1998). "Results of 546 Blalock-Taussig shunts performed in 478 patients". Cardiol Young. 8 (4): 486–90. doi:10.1017/s1047951100007150. PMID 9855103.
- ↑ Kim HK, Kim WH, Kim SC, Lim C, Lee CH, Kim SJ (2006). "Surgical strategy for pulmonary coarctation in the univentricular heart". Eur J Cardiothorac Surg. 29 (1): 100–4. doi:10.1016/j.ejcts.2005.10.032. PMID 16337132.
- ↑ Karpawich PP, Bush CP, Antillon JR, Amato JJ, Marbey ML, Agarwal KC (1985). "Modified Blalock-Taussig shunt in infants and young children. Clinical and catheterization assessment". J Thorac Cardiovasc Surg. 89 (2): 275–9. PMID 3968910.
- ↑ Kulkarni H, Rajani R, Dalvi B, Gupta KG, Vora A, Kelkar P (1995). "Effect of Blalock Taussig shunt on clinical parameters, left ventricular function and pulmonary arteries". J Postgrad Med. 41 (2): 34–6. PMID 10707705.
- ↑ Bove EL, Kohman L, Sereika S, Byrum CJ, Kavey RE, Blackman MS; et al. (1987). "The modified Blalock-Taussig shunt: analysis of adequacy and duration of palliation". Circulation. 76 (3 Pt 2): III19–23. PMID 2441893.
- ↑ Ullom RL, Sade RM, Crawford FA, Ross BA, Spinale F (1987). "The Blalock-Taussig shunt in infants: standard versus modified". Ann Thorac Surg. 44 (5): 539–43. doi:10.1016/s0003-4975(10)62119-4. PMID 3675059.
- ↑ Eghtesady, Pirooz (2015). "Potts Shunt for Children With Severe Pulmonary Hypertension". Operative Techniques in Thoracic and Cardiovascular Surgery. Elsevier BV. 20 (3): 293–305. doi:10.1053/j.optechstcvs.2016.02.003. ISSN 1522-2942.
- ↑ Yuan, Shi-Min; Jing, Hua (2009). "Palliative procedures for congenital heart defects". Archives of Cardiovascular Diseases. Elsevier BV. 102 (6–7): 549–557. doi:10.1016/j.acvd.2009.04.011. ISSN 1875-2136.
- ↑ TRUCCONE, NESTOR J.; BOWMAN, FREDERICK O.; MALM, JAMES R.; GERSONY, WELTON M. (1974). "Systemic-Pulmonary Arterial Shunts in the First Year of Life". Circulation. Ovid Technologies (Wolters Kluwer Health). 49 (3): 508–511. doi:10.1161/01.cir.49.3.508. ISSN 0009-7322.