Onychomycosis
Jump to navigation
Jump to search
| Onychomycosis | |
 | |
|---|---|
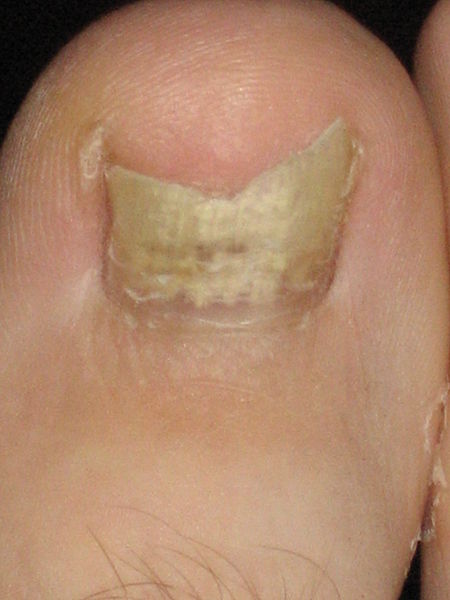
| A toenail affected by Onychomycosis | |
| ICD-10 | B35.1 |
| ICD-9 | 110.1 |
| DiseasesDB | 13125 |
| MedlinePlus | 001330 |
| MeSH | D014009 |
|
Onychomycosis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Onychomycosis On the Web |
|
American Roentgen Ray Society Images of Onychomycosis |
For patient information, click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Kiran Singh, M.D. [2]
Synonyms and keywords:Fungal infection of claw; Fungal infection of nail; Ringworm of nail
Diagnosis
History and Symptoms | Physical Examination | Laboratory Findings | Other Imaging Findings | Other Diagnostic Studies
Treatment
Medical Therapy | Surgery | Primary Prevention | Secondary Prevention | Future or Investigational Therapies
Case Studies