Endoscopic thoracic sympathectomy
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Jesus Rosario Hernandez, M.D. [2]
Template:Interventions infobox
Overview
Endoscopic thoracic sympathectomy (ETS) is a surgical procedure where certain portions of the sympathetic nerve trunk are destroyed. ETS is used to treat hyperhidrosis, facial blushing, social phobia, Raynaud's disease and Reflex Sympathetic Dystrophy. By far the most common complaint treated with ETS is palmar hyperhidrosis, or "sweaty palms".
Sympathectomy refers to the destruction of tissue anywhere in either of the two sympathetic trunks, long chains of nerve ganglia lying along either side of the spine. Each trunk is broadly divided into three regions: cervical (up by the neck), thoracic (in the chest) and lumbar (in the lower back). The most common area targeted in sympathectomy is the upper thoracic region, that part of the sympathetic chain lying between the first and fifth thoracic vertebrae.
History
Scientists became fascinated with the idea of sympathectomy in the mid-19th century when it was learned that the autonomic nervous system runs to almost every organ, gland and muscle system in the body, and it was surmised that somehow these nerves must play a role in how the body is able to automatically adjust levels on many different body functions in response to changes in the environment, exercise and emotion. They wondered how exactly it was that the autonomic nervous system was able to do all that, and they wondered what might change if various parts of it were removed.
The first sympathectomy was performed by Dr. Alexander in 1889. Since the sympathetic nervous system was well known to affect many body systems, the surgery was performed in attempts to treat many conditions, including idiocy, Goitre, epilepsy, glaucoma, and angina pectoris. Thoracic sympathectomy has been indicated for hyperhidrosis (excessive sweating) since 1920, when Dr. A. Kotzareff showed it would cause anhidrosis (total inability to sweat) from the nipple line upwards.
A lumbar sympathectomy was also developed and used to treat excessive sweating of the feet and other ailments, and typically resulted in impotence in men.
Sympathectomy itself is relatively easy to perform; however, accessing the nerve tissue in the chest cavity by conventional surgical methods was difficult, painful, and spawned several different approaches. The posterior approach was developed by Dr. A.W. Adson in 1908, and required resection (sawing off) of ribs. Dr. E.D. Telford came up with a supraclavical (above the collar-bone) approach in 1935, which was less painful than the posterior, but was more prone to damaging important nerves and blood vessels.
Because of these difficulties, and because of disabling sequelae associated with sympathetic denervation, conventional or "open" sympathectomy was never a very popular procedure, although it continued to be practiced for hyperhidrosis, Raynaud's disease, and various psychiatric disorders. With the popularization of lobotomy in the 1940s, sympathectomy fell out of favor when utilised as psychosurgery.
The endoscopic version of thoracic sympathectomy was pioneered by Drs. Goren Claes and Christer Drott at the Borås hospital in Sweden in the late 1980s. The development of endoscopic "minimally invasive" surgical techniques have made possible the mass-marketing of sympathectomy, and today ETS surgery is practiced in many countries throughout the industrial world. The total number of ETS surgeries performed worldwide to date numbers well over 100,000.
In addition to hyperhidrosis and Raynaud's, the indications for ETS have expanded to include facial blushing, and, once again, psychiatric disorders such as social phobia and agoraphobia. There are reports of ETS being used to treat headaches and hyperactive bronchial tubes.
In the mid 1990s a group of Swedish ETS patients complaining of disabling side effects formed the organization FFSO (people disabled by sympathectomy). The group grew to over 300 members (about 0.3% of estimated world-wide number of patients).
Overview
ETS surgery works by dissection nerve tissue in the upper thoracic region of the sympathetic nervous system, thus interrupting neural messages that ordinarily would travel to many different organs, glands and muscles. It is via these nerves of the autonomic nervous system that the brain is able to make adjustments in the body in response to changing conditions in the environment, changing emotional states, level of exercise, and other factors.
When performed endoscopically, the surgeon penetrates the chest cavity, making holes about the diameter of a soda straw between ribs. This allows the surgeon to insert a tiny video camera in one hole and a surgical instrument in another.
Sympathectomy is accomplished by dissecting the nerve tissue. The clamping method, also referred to as ESB (Endoscopic Sympathetic Blockade) employs titanium clamps around the nerve tissue, and was developed in an attempt to make the procedure reversible. However, reversal of the clamping procedure has a short time window (a few days or weeks at most) and may be incomplete. In a study by Dr. Rafael Reisfeld, it was concluded that the clamping method at the T3-T4 level is as effective as the coagulation or the excisional method done at the T2-T3 level.[1]
It has been proposed that ETS can alter many bodily functions, including sweating, heart rate, heart stroke volume, blood pressure, thyroid, baroreflex, lung volume, pupil dilation, skin temperature, goose bumps and other aspects of the autonomic nervous system. It has been proposed that it can also diminish the body's physical reaction to exercise and possibly reactions to strong emotion.
Results
The most common indication for ETS surgery is hyperhidrosis, or excessive sweating. However, the only empirical study on sweat before and after ETS demonstrated that the procedure increases total body sweating. [2]
Swedish National Board of Health and Welfare statement on treatment results says (English translation is available at: [3], the original Swedish text can be found at [4]): "A large amount of international studies shows that an incision on the sympatikotomi nerve gives a very positive result when it come to hand perspiration and also that the side effects are rare.". Critics have raised serious questions about the methodology of such studies.
Exact results of ETS are impossible to predict, because of considerable anatomic variations in sympathetic nerve function from one patient to the next, and also because of variations in surgical technique.
Studies by ETS surgeons have claimed a satisfaction rate around 85-95% with at least 2% regretting the surgery.[3][4][5] One surgeon study shows a satisfaction rate as low as 28.6.[6] Most patients report various adverse reactions as a result of the surgery. However, ETS surgeon Samuel S. Ahn of UCLA claims "100% success with no negative side effects". [7]
A large study of psychiatric patients treated with this surgery showed significant reductions in fear and alertness, among other emotional changes (Teleranta, Pohjavaara, et al 2003, 2004). [8]
ETS patients are being studied using the autonomic failure protocol headed by David Goldstein, M.D. Ph.D., senior investigator at the U.S National Institute of Neurological Disorders and Stroke. He has documented loss of thermoregulatory function, cardiac denervation, and loss of vasoconstriction.
Risks and controversy
Quoting the above-mentioned Swedish National Board of Health and Welfare statement: "The method can give permanent side effects that in some cases first will become obvious after some time. One of the side effects might be increased perspiration on different places on your body. Why and how this happens is still unknown. According to the research available about 25-75% of all patients can expect more or less serious perspiration on different places on their body, such as the trunk and groin area. However, it is also mentioned in the research that 0-10% regrets having the surgery done for this reason. Other documented side effects are the inability to raise the heart rate when working out physically. This has in some cases led to decreased ability to perform your work and daily activities. Some patients also complained of not being able to control their body temperature and it is experienced as very uncomfortable."
A reduced efficiency in maintaining normal body temperature in warm environments is consistent with the reduced ability or complete inability to sweat above the nipple line, a common ETS outcome first shown by Dr. Kotzareff. For a fully clothed person, only the hands, cranial region and neck are typically exposed. In a hot environment, a normal person's body is cooled primarily by evaporation of water vapor through the warmest areas of exposed skin. These areas are associated with the head and neck, which under very warm circumstances or vigorous exercise, visibly show moisture (sweat) accumulating as part of the cooling process. For an ETS patient that has lost ability to sweat from cranium, neck, and arms, an increased amount of body heat must be rejected via transpiration/sweating involving skin of the lower body. Unfortunately, this skin is generally at a lower temperature and usually covered by clothing - both factors that reduce the cooling efficiency and result in poor thermoregulation. An uncomfortably warm sensation and accumulation of sweat on large areas of skin underneath clothing can result.
There is much disagreement among ETS surgeons about the best surgical method, optimal location for nerve dissection, and as to the nature and extent of the consequent primary effects and side effects. The internet now features many websites run by surgeons extolling the benefits of ETS backed by patient testimonials. However, there are also many websites run by disabled ETS victims who complain of severe adverse reactions and lack of adequate informed consent. Several online discussion forums are dedicated to the subject of ETS surgery, where both positive and negative patient testimonials abound.
In 2003, ETS was banned in its birthplace, Sweden, due to overwhelming complaints by disabled patients (0.3% of the total world-wide number of patients). In 2004, Taiwanese health authorities banned the procedure on patients under 20 years of age.
In 2006, the FinOHTA group, the Finnish Office for Health Technology Assessment, showed in a review that there were strong indications of side effects as a result of this surgery.[9]
According to Dr. Reisfeld some of the reasons why ETS is banned in certain countries is because of the unjustified performance of ETS on patients with facial blushing and or facial sweating and or armpit sweating . Dr. Reisfeld believes that ETS should only be performed on patients with severe palmar hyperhidrosis. [10]
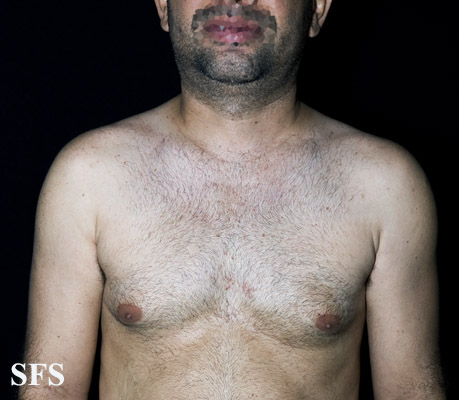
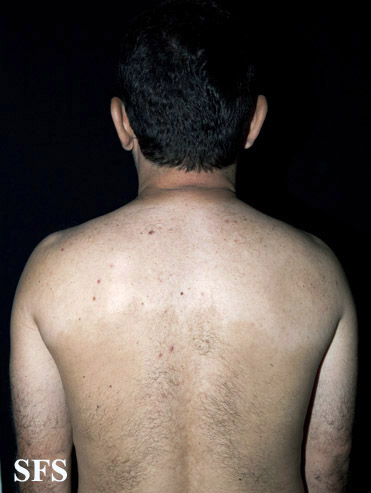
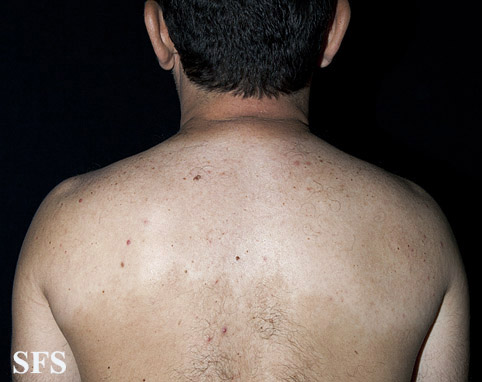
Dermatological findings due sympathectomy
-
. Acquired hypomelanosis-hipopigmentation after sympathectomy.
-
Acquired hypomelanosis-hipopigmentation after sympathectomy.
-
Acquired hypomelanosis-hipopigmentation after sympathectomy.
Popular culture
In the movie Sublime the character George Grieves (played by Tom Cavanagh) accidentally undergoes the procedure. The American TV show "Grey's Anatomy" featured ETS surgery for facial blushing in an episode titled "Make Me Lose Control". [11]
References
- ↑ Reisfeld, Rafael. "Sympathectomy for hyperhidrosis: should we place the clamps at T2-T3 or T3-T4?" Clinical Autonomic Research, December 2006, Volume 16, Number 6.
- ↑ Kopelman D, Assalia A, Ehrenreich M, Ben-Amnon Y, Bahous H, Hashmonai M (2000). "The effect of upper dorsal thoracoscopic sympathectomy on the total amount of body perspiration". Surg. Today. 30 (12): 1089–92. PMID 11193740.
- ↑ Choi BC, Lee YC, Sim SB (2003). "Treatment of palmar hyperhidrosis by endoscopic clipping of the upper part of the T4 sympathetic ganglion. Preliminary results". Clin. Auton. Res. 13 Suppl 1: I48–51. doi:10.1007/s10286-003-1112-4. PMID 14673674.
- ↑ Lardinois D, Ris HB (2002). "Minimally invasive video-endoscopic sympathectomy by use of a transaxillary single port approach". Eur J Cardiothorac Surg. 21 (1): 67–70. PMID 11788259.
- ↑ Drott C, Claes G, Olsson-Rex L, Dalman P, Fahlén T, Göthberg G (1998). "Successful treatment of facial blushing by endoscopic transthoracic sympathicotomy". Br. J. Dermatol. 138 (4): 639–43. PMID 9640370.
- ↑ "KoreaMed - Basic Search". Retrieved 2007-12-02.
- ↑ "Sweaty Palms Hereditary". Retrieved 2007-12-02.
- ↑ http://herkules.oulu.fi/isbn9514274571/isbn9514274571.pdf
- ↑ "Reports - Publications - Finohta". Retrieved 2007-12-02.
- ↑ "The Center for Hyperhidrosis. Dr. Reisfeld, world renowned expert and pioneer, can help!". Retrieved 2007-12-02.
- ↑ "Introduction - Corposcindosis". Retrieved 2007-12-02.
External links
- Corposcindosis A medical treatise on the effects of ETS surgery
- Truth About ETS Covering all aspects of the sympathectomy industry since 2004
- [5] Total number of ETS surgeries performed worldwide
- [6] Social phobia world hyperhidrosis forum
- ESFB Channel - Discussion about excessive sweating, facial blushing, rosacea and social phobia
- ETS & Reversals - Discussion about ETS, the side effects, the surgeons, and the ongoing search for a working reversal
- FfSo - People disabled by sympathectomies
- P.A.S.S. - Patients Against Sympathetic Surgery
Template:Neurosurgical procedures