Brentuximab vedotin
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Ammu Susheela, M.D. [2]; Sree Teja Yelamanchili, MBBS [3]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
WARNING: PROGRESSIVE MULTIFOCAL LEUKOENCEPHALOPATHY (PML)
See full prescribing information for complete Boxed Warning.
* JC virus infection resulting in PML and death can occur in patients receiving Brentuximab vedotin
|
Overview
Brentuximab vedotin is an antibody-drug conjugate that is FDA approved for the treatment of hodgkin's lymphoma, systemic anaplastic large cell lymphoma. There is a Black Box Warning for this drug as shown here. Common adverse reactions include neutropenia, sensory neuropathy.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Hodgkin Lymphoma
- Brentuximab vedotin is indicated for treatment of patients with Hodgkin's Lymphoma (HL) after failure of autologous stem cell transplant (ASCT) or after failure of at least two prior multi-agent chemotherapy regimens in patients who are not ASCT candidates.
- This indication is approved under accelerated approval based on overall response rate. An improvement in patient-reported outcomes or survival has not been established. Continued approval for this indication may be contingent upon verification and description of clinical benefit in confirmatory trials.
Systemic Anaplastic Large Cell Lymphoma
- Brentuximab vedotin is indicated for treatment of patients with systemic anaplastic large cell lymphoma (sALCL) after failure of at least one prior multi-agent chemotherapy regimen.
- This indication is approved under accelerated approval based on overall response rate. An improvement in patient-reported outcomes or survival has not been established. Continued approval for this indication may be contingent upon verification and description of clinical benefit in confirmatory trials.
- Administer brentuximab vedotin as an intravenous infusion over 30 minutes every 3 weeks until disease progression or unacceptable toxicity.
Dose Modification
- For new or worsening Grade 2 or 3 neuropathy, dosing should be held until neuropathy improves to Grade 1 or baseline and then restarted at 1.2 mg/kg. For Grade 4 peripheral neuropathy, brentuximab vedotin should be discontinued.
- The dose of brentuximab vedotin should be held for Grade 3 or 4 neutropenia until resolution to baseline or Grade 2 or lower. Consider G-CSF prophylaxis for subsequent cycles in patients who experience Grade 3 or 4 neutropenia in the previous cycle. In patients with recurrent Grade 4 neutropenia despite the use of G-CSF prophylaxis, consider discontinuation or dose reduction of Brentuximab vedotin to 1.2 mg/kg.
Instructions for Preparation and Administration
Administration
- Administer brentuximab vedotin as an intravenous infusion only.
Do not mix brentuximab vedotin with, or administer as an infusion with, other medicinal products.
Reconstitution
- Follow procedures for proper handling and disposal of anticancer drugs.
- Use appropriate aseptic technique for reconstitution and preparation of dosing solutions.
- Determine the number of 50 mg vials needed based on the patient’s weight and the prescribed dose.
- Reconstitute each 50 mg vial of brentuximab vedotin with 10.5 mL of Sterile Water for Injection, USP, to yield a single-use solution containing 5 mg/mL brentuximab vedotin.
- Direct the stream toward the wall of vial and not directly at the cake or powder.
- Gently swirl the vial to aid dissolution. DO NOT SHAKE.
- Inspect the reconstituted solution for particulates and discoloration. The reconstituted solution should be clear to slightly opalescent, colorless, and free of visible particulates.
- Following reconstitution, dilute immediately into an infusion bag. If not diluted immediately, store the solution at 2–8°C (36–46°F) and use within 24 hours of reconstitution. DO NOT FREEZE.
- Discard any unused portion left in the vial.
Dilution
- Calculate the required volume of 5 mg/mL reconstituted brentuximab vedotin solution needed.
- Withdraw this amount from the vial and immediately add it to an infusion bag containing a minimum volume of 100 mL of 0.9% Sodium Chloride Injection, 5% Dextrose Injection or Lactated Ringer's Injection to achieve a final concentration of 0.4 mg/mL to 1.8 mg/mL brentuximab vedotin.
- Gently invert the bag to mix the solution.
- Following dilution, infuse the brentuximab vedotin solution immediately.
- If not used immediately, store the solution at 2–8°C (36–46°F) and use within 24 hours of reconstitution. DO NOT FREEZE.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Brentuximab vedotin in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Brentuximab vedotin in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding FDA-Labeled Use of Brentuximab vedotin in pediatric patients.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Brentuximab vedotin in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Brentuximab vedotin in pediatric patients.
Contraindications
- Brentuximab vedotin is contraindicated with concomitant bleomycin due to pulmonary toxicity (e.g., interstitial infiltration and/or inflammation)
Warnings
|
WARNING: PROGRESSIVE MULTIFOCAL LEUKOENCEPHALOPATHY (PML)
See full prescribing information for complete Boxed Warning.
* JC virus infection resulting in PML and death can occur in patients receiving Brentuximab vedotin
|
Peripheral Neuropathy
- Brentuximab vedotin treatment causes a peripheral neuropathy that is predominantly sensory. Cases of peripheral motor neuropathy have also been reported. Brentuximab vedotin-induced peripheral neuropathy is cumulative. In the HL and sALCL clinical trials, 54% of patients experienced any grade of neuropathy. Of these patients, 49% had complete resolution, 31% had partial improvement, and 20% had no improvement. Of the patients who reported neuropathy, 51% had residual neuropathy at the time of their last evaluation. Monitor patients for symptoms of neuropathy, such as hypoesthesia, hyperesthesia, paresthesia, discomfort, a burning sensation, neuropathic pain, or weakness.
- Patients experiencing new or worsening peripheral neuropathy may require a delay, change in dose, or discontinuation of brentuximab vedotin.
Anaphylaxis and Infusion Reactions
- Infusion-related reactions, including anaphylaxis, have occurred with brentuximab vedotin. Monitor patients during infusion. If anaphylaxis occurs, immediately and permanently discontinue administration of brentuximab vedotin and administer appropriate medical therapy. If an infusion-related reaction occurs, the infusion should be interrupted and appropriate medical management instituted. Patients who have experienced a prior infusion-related reaction should be premedicated for subsequent infusions. Premedication may include acetaminophen, an antihistamine, and a corticosteroid.
Hematologic Toxicities
- Prolonged (≥1 week) severe neutropenia and Grade 3 or Grade 4 thrombocytopenia or anemia can occur with brentuximab vedotin. Febrile neutropenia has been reported with treatment with brentuximab vedotin. Complete blood counts should be monitored prior to each dose of brentuximab vedotin and more frequent monitoring should be considered for patients with Grade 3 or 4 neutropenia. Monitor patients for fever. If Grade 3 or 4 neutropenia develops, consider dose delays, reductions, discontinuation, or G-CSF prophylaxis with subsequent brentuximab vedotin doses.
Serious Infections and Opportunistic Infections
- Serious infections and opportunistic infections such as pneumonia, bacteremia, and sepsis or septic shock (including fatal outcomes) have been reported in patients treated with brentuximab vedotin. Patients should be closely monitored during treatment for the emergence of possible bacterial, fungal, or viral infections.
Tumor Lysis Syndrome
- Patients with rapidly proliferating tumor and high tumor burden may be at increased risk of tumor lysis syndrome. Monitor closely and take appropriate measures.
Increased Toxicity in the Presence of Severe Renal Impairment
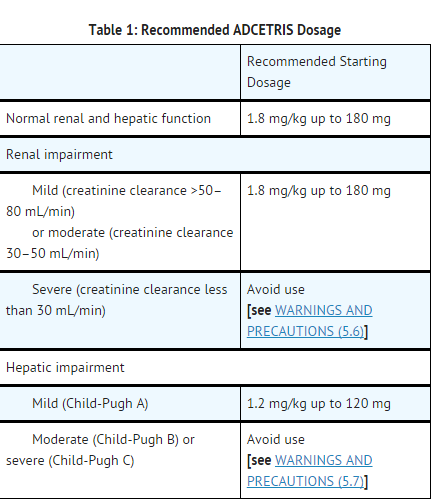
- The frequency of ≥Grade 3 adverse reactions and deaths was greater in patients with severe renal impairment compared to patients with normal renal function. Due to higher MMAE exposure, ≥Grade 3 adverse reactions may be more frequent in patients with severe renal impairment compared to patients with normal renal function. Avoid the use of brentuximab vedotin in patients with severe renal impairment creatinine clearance (CLcr) <30 mL/min].
Increased Toxicity in the Presence of Moderate or Severe Hepatic Impairment
- The frequency of ≥Grade 3 adverse reactions and deaths was greater in patients with moderate and severe hepatic impairment compared to patients with normal hepatic function. Avoid the use of brentuximab vedotin in patients with moderate (Child-Pugh B) or severe (Child-Pugh C) hepatic impairment.
Hepatotoxicity
- Serious cases of hepatotoxicity, including fatal outcomes, have occurred in patients receiving brentuximab vedotin. Cases were consistent with hepatocellular injury, including elevations of transaminases and/or bilirubin. Cases have occurred after the first dose of brentuximab vedotin or after brentuximab vedotin rechallenge. Preexisting liver disease, elevated baseline liver enzymes, and concomitant medications may also increase the risk. Monitor liver enzymes and bilirubin. Patients experiencing new, worsening, or recurrent hepatotoxicity may require a delay, change in dose, or discontinuation of brentuximab vedotin.
Progressive Multifocal Leukoencephalopathy
- JC virus infection resulting in PML and death has been reported in brentuximab vedotin-treated patients. In addition to brentuximab vedotin therapy, other possible contributory factors include prior therapies and underlying disease that may cause immunosuppression. Consider the diagnosis of PML in any patient presenting with new-onset signs and symptoms of central nervous system abnormalities.
- Hold brentuximab vedotin dosing for any suspected case of PML and discontinue brentuximab vedotin dosing if a diagnosis of PML is confirmed.
Serious Dermatologic Reactions
- Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), including fatal outcomes, have been reported with brentuximab vedotin. If SJS or TEN occurs, discontinue brentuximab vedotin and administer appropriate medical therapy.
Embryo-Fetal Toxicity
- There are no adequate and well-controlled studies of brentuximab vedotin in pregnant women. However, based on its mechanism of action and findings in animals, brentuximab vedotin can cause fetal harm when administered to a pregnant woman. Brentuximab vedotin caused embryo-fetal toxicities, including significantly decreased embryo viability and fetal malformations, in animals at maternal exposures that were similar to human exposures at the recommended doses for patients with HL and sALCL. If this drug is used during pregnancy, or if the patient becomes pregnant while receiving the drug, the patient should be apprised of the potential hazard to the fetus.
Adverse Reactions
Clinical Trials Experience
The following are serious adverse reactions.
- Peripheral neuropathy.
- Anaphylaxis and infusion Reactions.
- Hematologic Toxicities.
- Serious Infections and Opportunistic Infections.
- Tumor Lysis Syndrome.
- Increased Toxicity in the Presence of Severe Renal Impairment.
- Increased Toxicity in the Presence of Moderate or Severe Hepatic Impairment.
- Hepatotoxicity.
- Progressive Multifocal Leukoencephalopathy.
- Serious Dermatologic Reactions.
- Embryo-Fetal Toxicity.
Clinical Trial Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
- Brentuximab vedotin was studied as monotherapy in 160 patients in two phase 2 trials. Across both trials, the most common adverse reactions (≥20%), regardless of causality, were neutropenia, peripheral sensory neuropathy, fatigue, nausea, anemia, upper respiratory tract infection, diarrhea, pyrexia, rash, thrombocytopenia, cough, and vomiting. The most common adverse reactions occurring in at least 10% of patients in either trial, regardless of causality, using the NCI Common Toxicity Criteria Version 3.0, are shown in TABLE 2.
Experience in Hodgkin Lymphoma
- Brentuximab vedotin was studied in 102 patients with HL in a single arm clinical trial in which the recommended starting dose and schedule was 1.8 mg/kg intravenously every 3 weeks. Median duration of treatment was 27 weeks (range, 3 to 56 weeks).
- The most common adverse reactions (≥20%), regardless of causality, were neutropenia, peripheral sensory neuropathy, fatigue, upper respiratory tract infection, nausea, diarrhea, anemia, pyrexia, thrombocytopenia, rash, abdominal pain, cough, and vomiting.
Pulmonary Toxicity
- In another clinical trial in patients with HL that studied brentuximab vedotin with bleomycin as part of a combination regimen, the rate of non-infectious pulmonary toxicity was higher than the historical incidence reported with ABVD (adriamycin, bleomycin, vinblastine, dacarbazine). Patients typically reported cough and dyspnea. Interstitial infiltration and/or inflammation were observed on radiographs and computed tomographic imaging of the chest. Most patients responded to corticosteroids. The concomitant use of brentuximab vedotin with bleomycin is contraindicated.
- Experience in Systemic Anaplastic Large Cell Lymphoma
- Brentuximab vedotin was studied in 58 patients with sALCL in a single arm clinical trial in which the recommended starting dose and schedule was 1.8 mg/kg intravenously every 3 weeks. Median duration of treatment was 24 weeks (range, 3 to 56 weeks).
- The most common adverse reactions (≥20%), regardless of causality, were neutropenia, anemia, peripheral sensory neuropathy, fatigue, nausea, pyrexia, rash, diarrhea, and pain.
Combined Experience
Infusion reactions
- Two cases of anaphylaxis were reported in phase 1 trials. There were no Grade 3 or 4 infusion-related reactions reported in the phase 2 trials, however, Grade 1 or 2 infusion-related reactions were reported for 19 patients (12%). The most common adverse reactions (≥2%) associated with infusion-related reactions were chills (4%), nausea (3%), dyspnea (3%), pruritus (3%), pyrexia (2%), and cough (2%).
Serious adverse reactions
- In the phase 2 trials, serious adverse reactions, regardless of causality, were reported in 31% of patients receiving Brentuximab vedotin. The most common serious adverse reactions experienced by patients with HL include peripheral motor neuropathy (4%), abdominal pain (3%), pulmonary embolism (2%), pneumonitis (2%), pneumothorax (2%), pyelonephritis (2%), and pyrexia (2%). The most common serious adverse reactions experienced by patients with sALCL were septic shock (3%), supraventricular arrhythmia (3%), pain in extremity (3%), and urinary tract infection (3%). Other important serious adverse reactions reported include PML, Stevens-Johnson syndrome, and tumor lysis syndrome.
Dose modifications
- Adverse reactions that led to dose delays in more than 5% of patients were neutropenia (14%) and peripheral sensory neuropathy (11%).
Discontinuations
- Adverse reactions led to treatment discontinuation in 21% of patients. Adverse reactions that led to treatment discontinuation in 2 or more patients with HL or sALCL were peripheral sensory neuropathy (8%) and peripheral motor neuropathy (3%).
Postmarketing Experience
- The following adverse reactions have been identified during post-approval use of brentuximab vedotin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Blood and lymphatic system disorders
- Hepatobiliary disorders
- PML
- Serious infections and opportunistic infections.
- Metabolism and nutrition disorders
- Gastrointestinal disorders
- Pancreatitis (including fatal outcomes). Consider the diagnosis of pancreatitis for patients presenting with severe abdominal pain.
- Skin and subcutaneous tissue disorders
- Toxic epidermal necrolysis, including fatal outcomes.
Immunogenicity
- Patients with HL and sALCL in the phase 2 trials were tested for antibodies to brentuximab vedotin every 3 weeks using a sensitive electrochemiluminescent immunoassay. Approximately 7% of patients in these trials developed persistently positive antibodies (positive test at more than 2 timepoints) and 30% developed transiently positive antibodies (positive in 1 or 2 post-baseline timepoints).
- The anti-brentuximab antibodies were directed against the antibody component of brentuximab vedotin in all patients with transiently or persistently positive antibodies. Two of the patients (1%) with persistently positive antibodies experienced adverse reactions consistent with infusion reactions that led to discontinuation of treatment. Overall, a higher incidence of infusion related reactions was observed in patients who developed persistently positive antibodies.
- A total of 58 patient samples that were either transiently or persistently positive for anti-brentuximab vedotin antibodies were tested for the presence of neutralizing antibodies. Sixty-two percent of these patients had at least one sample that was positive for the presence of neutralizing antibodies. The effect of anti-brentuximab vedotin antibodies on safety and efficacy is not known.
- Immunogenicity assay results are highly dependent on several factors including assay sensitivity and specificity, assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. For these reasons, comparison of incidence of antibodies to brentuximab vedotin with the incidence of antibodies to other products may be misleading.
Drug Interactions
- In vitro data indicate that monomethyl auristatin E (MMAE) is a substrate and an inhibitor of CYP3A4/5. In vitro data indicate that MMAE is also a substrate of the efflux transporter P‑glycoprotein (P-gp).
Effect of Other Drugs on Brentuximab Vedotin
- CYP3A4 Inhibitors/Inducers: MMAE is primarily metabolized by CYP3A. Co-administration of brentuximab vedotin with ketoconazole, a potent CYP3A4 inhibitor, increased exposure to MMAE by approximately 34%. Patients who are receiving strong CYP3A4 inhibitors concomitantly with brentuximab vedotin should be closely monitored for adverse reactions. Co-administration of brentuximab vedotin with rifampin, a potent CYP3A4 inducer, reduced exposure to MMAE by approximately 46%.
P-gp Inhibitors
- Co-administration of brentuximab vedotin with P-gp inhibitors may increase exposure to MMAE. Patients who are receiving P-gp inhibitors concomitantly with brentuximab vedotin should be closely monitored for adverse reactions.
Effect of Brentuximab vedotin on Other Drugs
- Co-administration of brentuximab vedotin did not affect exposure to midazolam, a CYP3A4 substrate. MMAE does not inhibit other CYP enzymes at relevant clinical concentrations [see CLINICAL PHARMACOLOGY (12.3)]. brentuximab vedotin is not expected to alter the exposure to drugs that are metabolized by CYP3A4 enzymes.
Use in Specific Populations
Pregnancy
Risk Summary
- There are no adequate and well-controlled studies with brentuximab vedotin in pregnant women. However, based on its mechanism of action and findings in animals, brentuximab vedotin can cause fetal harm when administered to a pregnant woman. Brentuximab vedotin caused embryo-fetal toxicities in animals at maternal exposures that were similar to human exposures at the recommended doses for patients with HL and sALCL. If this drug is used during pregnancy, or if the patient becomes pregnant while receiving this drug, the patient should be apprised of the potential hazard to the fetus.
Animal Data
- In an embryo-fetal developmental study, pregnant rats received 2 intravenous doses of 0.3, 1, 3, or 10 mg/kg brentuximab vedotin during the period of organogenesis (once each on Pregnancy Days 6 and 13). Drug-induced embryo-fetal toxicities were seen mainly in animals treated with 3 and 10 mg/kg of the drug and included increased early resorption (≥99%), post-implantation loss (≥99%), decreased numbers of live fetuses, and external malformations (i.e., umbilical hernias and malrotated hindlimbs). Systemic exposure in animals at the brentuximab vedotin dose of 3 mg/kg is approximately the same exposure in patients with HL or sALCL who received the recommended dose of 1.8 mg/kg every three weeks.
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Brentuximab vedotin in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Brentuximab vedotin during labor and delivery.
Nursing Mothers
- It is not known whether brentuximab vedotin is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from brentuximab vedotin a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
- The safety and effectiveness of brentuximab vedotin have not been established in the pediatric population. Clinical trials of brentuximab vedotin included only 9 pediatric patients and this number is not sufficient to determine whether they respond differently than adult patients.
Geriatic Use
- Clinical trials of brentuximab vedotin did not include sufficient numbers of patients aged 65 and over to determine whether they respond differently from younger patients. Safety and efficacy have not been established.
Gender
There is no FDA guidance on the use of Brentuximab vedotin with respect to specific gender populations.
Race
There is no FDA guidance on the use of Brentuximab vedotin with respect to specific racial populations.
Renal Impairment
- Avoid the use of brentuximab vedotin in patients with severe renal impairment (CLcr <30 mL/min).
- The kidney is a route of excretion for monomethyl auristatin E (MMAE). The pharmacokinetics and safety of brentuximab vedotin and MMAE were evaluated after the administration of 1.2 mg/kg of brentuximab vedotin to patients with mild (CLcr >50-80 mL/min; n=4), moderate (CLcr 30-50 mL/min; n=3) and severe (CLcr <30 mL/min; n=3) renal impairment. In patients with severe renal impairment, the rate of Grade 3 or worse adverse events was 3/3 (100%) compared to 3/8 (38%) in patients with normal renal function. Additionally, the AUC of MMAE (component of brentuximab vedotin) was approximately 2-fold higher in patients with severe renal impairment compared to patients with normal renal function.
- Due to higher MMAE exposure, ≥Grade 3 adverse reactions may be more frequent in patients with severe renal impairment compared to patients with normal renal function.
Hepatic Impairment
- Avoid the use of brentuximab vedotin in patients with moderate or severe hepatic impairment.
- The liver is a route of clearance for MMAE. The pharmacokinetics and safety of brentuximab vedotin and MMAE were evaluated after the administration of 1.2 mg/kg of brentuximab vedotin to patients with mild (Child-Pugh A; n=1), moderate (Child-Pugh B; n=5) and severe (Child-Pugh C; n=1) hepatic impairment. In patients with moderate and severe hepatic impairment, the rate of ≥Grade 3 adverse reactions was 6/6 (100%) compared to 3/8 (38%) in patients with normal hepatic function.
- Additionally, the AUC of MMAE was approximately 2.2-fold higher in patients with hepatic impairment compared to patients with normal hepatic function.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Brentuximab vedotin in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Brentuximab vedotin in patients who are immunocompromised.
Administration and Monitoring
Administration
Monitoring
- Complete blood counts should be monitored prior to each dose of brentuximab vedotin and more frequent monitoring should be considered for patients with Grade 3 or 4 neutropenia
IV Compatibility
There is limited information regarding IV Compatibility of Brentuximab vedotin in the drug label.
Overdosage
- There is no known antidote for overdosage of brentuximab vedotin. In case of overdosage, the patient should be closely monitored for adverse reactions, particularly neutropenia, and supportive treatment should be administered.
Pharmacology
Brentuximab vedotin?
| |
| Therapeutic monoclonal antibody | |
| Source | xi/o |
| Target | CD30 |
| Identifiers | |
| CAS number | |
| ATC code | L01 |
| PubChem | ? |
| Chemical data | |
| Formula | C6476H9930N1690O2030S40 (C68H105N11O15)3–5 |
| Mol. mass | 149.2–151.8 kDa |
| Synonyms | SGN-35, previously cAC10-vcMMAE |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | ? |
| Excretion | ? |
| Therapeutic considerations | |
| Licence data |
|
| Pregnancy cat. |
D(US) |
| Legal status |
[[Prescription drug|Template:Unicode-only]](US) |
| Routes | Intravenous |
Mechanism of Action
- Brentuximab vedotin is an ADC. The antibody is a chimeric IgG1 directed against CD30. The small molecule, MMAE, is a microtubule disrupting agent. MMAE is covalently attached to the antibody via a linker. Nonclinical data suggest that the anticancer activity of brentuximab vedotin is due to the binding of the ADC to CD30-expressing cells, followed by internalization of the ADC‑CD30 complex, and the release of MMAE via proteolytic cleavage. Binding of MMAE to tubulin disrupts the microtubule network within the cell, subsequently inducing cell cycle arrest and apoptotic death of the cells.
Structure
- Brentuximab vedotin (brentuximab vedotin) is a CD30-directed antibody-drug conjugate (ADC) consisting of three components
- The chimeric IgG1 antibody cAC10, specific for human CD30
- The microtubule disrupting agent MMAE
- A protease-cleavable linker that covalently attaches MMAE to cAC10.
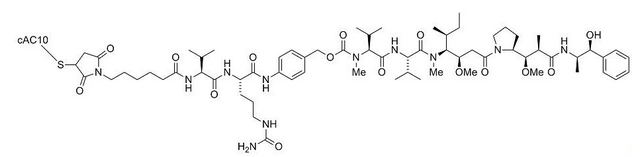
This image is provided by the National Library of Medicine.
Brentuximab vedotin has an approximate molecular weight of 153 kDa. Approximately 4 molecules of MMAE are attached to each antibody molecule. Brentuximab vedotin is produced by chemical conjugation of the antibody and small molecule components. The antibody is produced by mammalian (Chinese hamster ovary) cells, and the small molecule components are produced by chemical synthesis.
brentuximab vedotin (brentuximab vedotin) for Injection is supplied as a sterile, white to off-white, preservative-free lyophilized cake or powder in single-use vials. Following reconstitution with 10.5 mL Sterile Water for Injection, USP, a solution containing 5 mg/mL brentuximab vedotin is produced. The reconstituted product contains 70 mg/mL trehalose dihydrate, 5.6 mg/mL sodium citrate dihydrate, 0.21 mg/mL citric acid monohydrate, and 0.20 mg/mL polysorbate 80 and water for injection. The pH is approximately 6.6.
Pharmacodynamics
QT/QTc Prolongation Potential
- The effect of brentuximab vedotin (1.8 mg/kg) on the QTc interval was evaluated in an open-label, single-arm study in 46 evaluable patients with CD30-expressing hematologic malignancies. Administration of brentuximab vedotin did not prolong the mean QTc interval >10 ms from baseline. Small increases in the mean QTc interval (<10 ms) cannot be excluded because this study did not include a placebo arm and a positive control arm.
Pharmacokinetics
- The pharmacokinetics of brentuximab vedotin were evaluated in phase 1 trials and in a population pharmacokinetic analysis of data from 314 patients. The pharmacokinetics of three analytes were determined: the ADC, MMAE, and total antibody. Total antibody had the greatest exposure and had a similar PK profile as the ADC. Hence, data on the PK of the ADC and MMAE have been summarized.
Absorption
- Maximum concentrations of ADC were typically observed close to the end of infusion. A multiexponential decline in ADC serum concentrations was observed with a terminal half-life of approximately 4 to 6 days. Exposures were approximately dose proportional from 1.2 to 2.7 mg/kg. Steady-state of the ADC was achieved within 21 days with every 3-week dosing of brentuximab vedotin, consistent with the terminal half-life estimate.
- Minimal to no accumulation of ADC was observed with multiple doses at the every 3-week schedule.
- The time to maximum concentration for MMAE ranged from approximately 1 to 3 days. Similar to the ADC, steady‑state of MMAE was achieved within 21 days with every 3 week dosing of brentuximab vedotin. MMAE exposures decreased with continued administration of brentuximab vedotin with approximately 50% to 80% of the exposure of the first dose being observed at subsequent doses.
Distribution
- In vitro, the binding of MMAE to human plasma proteins ranged from 68–82%. MMAE is not likely to displace or to be displaced by highly protein-bound drugs. In vitro, MMAE was a substrate of P-gp and was not a potent inhibitor of P-gp.
- In humans, the mean steady state volume of distribution was approximately 6–10 L for ADC.
Metabolism
- In vivo data in animals and humans suggest that only a small fraction of MMAE released from brentuximab vedotin is metabolized. In vitro data indicate that the MMAE metabolism that occurs is primarily via oxidation by CYP3A4/5. In vitro studies using human liver microsomes indicate that MMAE inhibits CYP3A4/5 but not other CYP isoforms. MMAE did not induce any major CYP450 enzymes in primary cultures of human hepatocytes.
Elimination
- MMAE appeared to follow metabolite kinetics, with the elimination of MMAE appearing to be limited by its rate of release from ADC. An excretion study was undertaken in patients who received a dose of 1.8 mg/kg of brentuximab vedotin. Approximately 24% of the total MMAE administered as part of the ADC during an brentuximab vedotin infusion was recovered in both urine and feces over a 1-week period. Of the recovered MMAE, approximately 72% was recovered in the feces and the majority of the excreted MMAE was unchanged.
Specific Populations
- Effects of Gender, Age, and Race: Based on the population pharmacokinetic analysis; gender, age, and race do not have a meaningful effect on the pharmacokinetics of brentuximab vedotin.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, and Impairment of Fertility
- Carcinogenicity studies with brentuximab vedotin or the small molecule (MMAE) have not been conducted.
- MMAE was genotoxic in the rat bone marrow micronucleus study through an aneugenic mechanism. This effect is consistent with the pharmacological effect of MMAE as a microtubule disrupting agent. MMAE was not mutagenic in the bacterial reverse mutation assay (Ames test) or the L5178Y mouse lymphoma forward mutation assay.
- Fertility studies with brentuximab vedotin or MMAE have not been conducted. However, results of repeat-dose toxicity studies in rats indicate the potential for brentuximab vedotin to impair male reproductive function and fertility. In a 4-week repeat-dose toxicity study in rats with weekly dosing at 0.5, 5 or 10 mg/kg brentuximab vedotin, seminiferous tubule degeneration, Sertoli cell vacuolation, reduced spermatogenesis, and aspermia were observed. Effects in animals were seen mainly at 5 and 10 mg/kg of brentuximab vedotin. These doses are approximately 3 and 6-fold the human recommended dose of 1.8 mg/kg, respectively, based on body weight.
Clinical Studies
Carcinogenesis, Mutagenesis, and Impairment of Fertility
- Carcinogenicity studies with brentuximab vedotin or the small molecule (MMAE) have not been conducted.
- MMAE was genotoxic in the rat bone marrow micronucleus study through an aneugenic mechanism. This effect is consistent with the pharmacological effect of MMAE as a microtubule disrupting agent. MMAE was not mutagenic in the bacterial reverse mutation assay (Ames test) or the L5178Y mouse lymphoma forward mutation assay.
- Fertility studies with brentuximab vedotin or MMAE have not been conducted. However, results of repeat-dose toxicity studies in rats indicate the potential for brentuximab vedotin to impair male reproductive function and fertility. In a 4-week repeat-dose toxicity study in rats with weekly dosing at 0.5, 5 or 10 mg/kg brentuximab vedotin, seminiferous tubule degeneration, Sertoli cell vacuolation, reduced spermatogenesis, and aspermia were observed. Effects in animals were seen mainly at 5 and 10 mg/kg of brentuximab vedotin. These doses are approximately 3 and 6-fold the human recommended dose of 1.8 mg/kg, respectively, based on body weight.
Systemic Anaplastic Large Cell Lymphoma
- The efficacy of brentuximab vedotin in patients with relapsed sALCL was evaluated in one phase 2 open-label, single-arm, multicenter trial. This trial included patients who had sALCL that was relapsed after prior therapy. Fifty-eight patients were treated with 1.8 mg/kg of brentuximab vedotin administered intravenously over 30 minutes every 3 weeks. An independent review facility performed efficacy evaluations which included overall response rate (ORR = complete remission [CR] + partial remission [PR]) and duration of response as defined by clinical and radiographic measures including computed tomography (CT) and positron-emission tomography (PET) as defined in the 2007 Revised Response Criteria for Malignant Lymphoma (modified).
- The 58 patients ranged in age from 14–76 years (median, 52 years) and most were male (57%) and white (83%). Patients had received a median of 2 prior therapies; 26% of patients had received prior autologous stem cell transplant. Fifty percent (50%) of patients were relapsed and 50% of patients were refractory to their most recent prior therapy. Seventy-two percent (72%) were anaplastic lymphoma kinase (ALK)-negative.
- The efficacy results are summarized in TABLE 4. Duration of response is calculated from date of first response to date of progression or data cutoff date.
How Supplied
- Brentuximab vedotin (brentuximab vedotin) for Injection is supplied as a sterile, white to off-white preservative-free lyophilized cake or powder in individually-boxed single-use vials:
NDC (51144-050-01), 50 mg brentuximab vedotin. 16.3 Special Handling Brentuximab vedotin is an antineoplastic product. Follow special handling and disposal procedures1.
Storage
- Store vial at 2–8°C (36–46°F) in the original carton to protect from light.
Images
Drug Images
{{#ask: Page Name::Brentuximab vedotin |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel


{{#ask: Label Page::Brentuximab vedotin |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
Peripheral Neuropathy
- Advise patients that Brentuximab vedotin can cause a peripheral neuropathy. They should be advised to report to their health care provider any numbness or tingling of the hands or feet or any muscle weakness.
Fever/Neutropenia
- Advise patients to contact their health care provider if a fever of 100.5°F or greater or other evidence of potential infection such as chills, cough, or pain on urination develops.
Infusion reactions
- Advise patients to contact their health care provider if they experience signs and symptoms of infusion reactions including fever, chills, rash, or breathing problems within 24 hours of infusion.
Hepatotoxicity
- Advise patients to report symptoms that may indicate liver injury, including fatigue, anorexia, right upper abdominal discomfort, dark urine, or jaundice.
Progressive multifocal leukoencephalopathy
- Instruct patients receiving Brentuximab vedotin to immediately report if they have any of the following neurological, cognitive, or behavioral signs and symptoms or if anyone close to them notices these signs and symptoms.
- • changes in mood or usual behavior
- • confusion, thinking problems, loss of memory
- • changes in vision, speech, or walking
- • decreased strength or weakness on one side of the body
Pancreatitis
- Advise patients to contact their health care provider if they develop severe abdominal pain.
Pregnancy and Nursing
- Brentuximab vedotin can cause fetal harm. Advise women receiving Brentuximab vedotin to avoid pregnancy. Advise patients to report pregnancy immediately. Advise patients to avoid nursing while receiving Brentuximab vedotin.
Precautions with Alcohol
- Alcohol-Brentuximab vedotin interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- ADCETRIS ®[1]
Look-Alike Drug Names
There is limited information regarding Brentuximab vedotin Look-Alike Drug Names in the drug label.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.