Anorexia nervosa pathophysiology
|
Anorexia nervosa Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Anorexia nervosa pathophysiology On the Web |
|
American Roentgen Ray Society Images of Anorexia nervosa pathophysiology |
|
Risk calculators and risk factors for Anorexia nervosa pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Joseph Nasr, M.D.[2]
Pathophysiology
Anorexia nervosa has historically been conceptualized as a disorder with a multifactorial pathophysiology involving biological, psychological, and sociocultural factors. Early and subsequent theories proposed numerous causal mechanisms; however, the relative contribution of these factors has remained uncertain, and many early hypotheses have since been revised or rejected. Contemporary understanding emphasizes that no single causal mechanism exists, and that the physiological and psychological effects of starvation play a major role in perpetuating the disorder.[1]
Biological and Physiological Factors
Genetic Factors
(Historically proposed; still supported in principle)
Family and twin studies suggested that genetic factors contribute substantially to the risk of developing eating disorders, accounting for approximately 50% of the variance, and that anorexia nervosa shares genetic risk with major depressive disorder (Klump et al., 2001; Strober et al., 2000). These findings supported early views that genes influencing eating regulation, personality traits, and emotional processing contribute to disease vulnerability.
Animal models, including stress-based paradigms and gene-knockout studies, were historically used to explore biological mechanisms such as hypothalamic–pituitary–adrenal (HPA) axis dysregulation.[2] However, these models are now recognized as having significant limitations because food restriction is externally imposed and cannot replicate voluntary self-starvation or cognitive distortions, limiting their relevance to human anorexia nervosa.[1][2]
Neurobiological Factors
(Historically influential; causal role unresolved)
Early neurobiological research identified associations between anorexia nervosa and serotonergic neurotransmission, given serotonin’s role in mood, anxiety, impulse control, appetite, sleep, and emesis (Kaye et al., 2005).[3] Increased activity at 5-HT1A receptors and reduced activity at 5-HT2A receptors were proposed to contribute to anxiety, behavioral inhibition, and restrictive eating.[3][4]
It was further hypothesized that self-starvation may serve a compensatory function, as reduced tryptophan availability and altered steroid metabolism during starvation could lower serotonin synthesis and thereby reduce anxiety.[3] Subsequent work demonstrated that it is difficult to distinguish whether serotonergic abnormalities are causal risk factors or secondary consequences of malnutrition, and these findings are now interpreted as reflecting a mixture of trait vulnerabilities and state-dependent effects.[1][3]
An autoimmune hypothesis later proposed that autoantibodies directed against melanocortin peptides, which regulate appetite and stress responses, might contribute to anorexia nervosa.[5] This hypothesis remains preliminary, with limited replication, and is not considered an established causal mechanism.[5]
Nutritional and Metabolic Factors
(Historically proposed as causal; now considered secondary)
Earlier research by Bakan in 1979 proposed that micronutrient deficiencies, particularly zinc deficiency, could cause or perpetuate anorexia nervosa by suppressing appetite. Zinc supplementation was reported to improve weight gain in early trials, leading to the hypothesis that zinc deficiency might be a primary driver of anorexic symptoms.
This interpretation is now considered outdated. Contemporary evidence indicates that micronutrient deficiencies, including zinc, thiamine, and amino acid precursors such as tryptophan and tyrosine, are consequences of prolonged starvation, not primary causes of anorexia nervosa. While these deficiencies may exacerbate metabolic and neurochemical disturbances and influence recovery, they are insufficient to explain disease onset.[1]
Starvation produces profound metabolic and endocrine adaptations, including electrolyte disturbances, hypoglycemia, and suppression of reproductive and thyroid hormones. These physiological changes contribute significantly to medical complications and may reinforce restrictive behaviors but are understood as state effects of malnutrition rather than etiologic mechanisms.[1]
Psychological Factors
(Historically proposed and largely retained)
Psychological theories proposed that restrictive eating behaviors arise from feelings of fatness and unattractiveness and are maintained by cognitive biases affecting how individuals evaluate their bodies, food, and eating behaviors.[6]
A consistent finding is body image distortion, now understood not as a sensory perceptual deficit but as a bias in cognitive evaluation. Individuals with anorexia nervosa tend to overestimate body size and lack positive self-evaluative biases commonly observed in unaffected individuals.[7][8][9] Personality traits frequently reported in anorexia nervosa include perfectionism, obsessionality, behavioral restraint, rigidity, and a strong need for control. These traits often precede illness onset and persist after recovery, supporting their role as predisposing characteristics rather than consequences of starvation.[10]
Psychiatric comorbidity is common, with depression, anxiety disorders, obsessive–compulsive disorder, substance use disorders, and personality disorders frequently co-occurring and contributing to illness severity and chronicity.[1][10]
Neuropsychological Findings
(Historically observed; interpretation refined)
Neuropsychological studies have produced variable findings, partly due to the confounding effects of starvation. A relatively consistent observation is reduced cognitive flexibility, reflecting difficulty shifting cognitive strategies, which may contribute to behavioral rigidity. This impairment is now interpreted as reflecting both trait vulnerability and starvation effects, rather than a disease-specific deficit.[11]
Additional studies suggested attentional and memory biases toward body- and weight-related information. These findings are limited and inconsistent and are considered maintaining rather than causal factors.[12][13]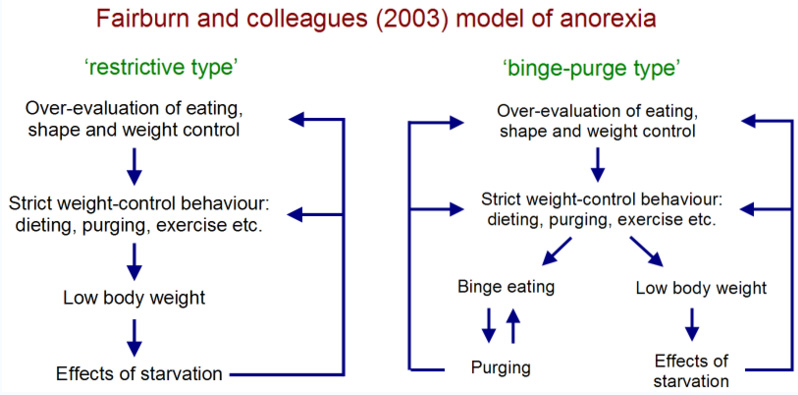
Psychological Models
(Maintenance models, not etiologic)
Fairburn and colleagues proposed a transdiagnostic cognitive-behavioral model, suggesting that eating disorders are maintained by shared psychopathological processes including clinical perfectionism, low self-esteem, mood intolerance, and interpersonal difficulties. This model has been influential in guiding treatment but is understood as a maintenance framework rather than an explanation of disease origin.[14]
Social and Environmental Factors
(Historically emphasized; causal role revised)
Early sociocultural theories emphasized media-driven ideals of thinness as a primary cause of anorexia nervosa, supported by higher prevalence in professions with strong pressures to maintain low body weight.[15] Subsequent evidence indicates that sociocultural factors act as risk modifiers rather than primary causes.[1]
Anorexia nervosa occurs across cultures, and in some non-Western populations restrictive eating may occur without prominent fear of fatness, indicating that sociocultural influences shape symptom expression rather than disease origin.[1]
Adverse life experiences, including childhood sexual abuse, have been associated with greater illness severity and chronicity but are not specific causal factors for anorexia nervosa.[16]
The internet has facilitated both recovery-oriented communities and pro-ana groups that reject medical models of anorexia nervosa. While most online resources promote treatment, pro-ana communities have raised concerns regarding reinforcement of disordered eating behaviors, particularly among adolescents.[17][18]
Understanding as of 2025
A review by Attia and Walsh (2025) synthesizes available evidence and emphasizes that anorexia nervosa is best understood as a multifactorial disorder arising from the interaction of genetic vulnerability, psychological traits, sociocultural influences, and the physiological consequences of starvation. They explicitly caution against attributing causality to any single biological, nutritional, or psychological mechanism and highlights that many abnormalities observed in anorexia nervosa represent state-dependent effects of malnutrition, while others may reflect pre-existing trait vulnerabilities.[1]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 Attia, E. and Walsh, B.T. (2025a) ‘Eating disorders’, JAMA, 333(14), p. 1242. doi:10.1001/jama.2025.0132.
- ↑ 2.0 2.1 Siegfried Z, Berry EM, Hao S, Avraham Y. (2003) Animal models in the investigation of anorexia. Physiol Behav, 79 (1), 39-45. PMID 12818708.
- ↑ 3.0 3.1 3.2 3.3 Kaye WH, Frank GK, Bailer UF, Henry SE, Meltzer CC, Price JC, Mathis CA, Wagner A. (2005) Serotonin alterations in anorexia and bulimia nervosa: new insights from imaging studies. Physiol Behav, 85 (1), 73-81. PMID 15869768.
- ↑ Kaye WH, Bailer UF, Frank GK, Wagner A, Henry SE. (2005) Brain imaging of serotonin after recovery from anorexia and bulimia nervosa. Physiol Behav, 86(1-2), 15-7. PMID 16102788.
- ↑ 5.0 5.1 Fetissov SO, Harro J, Jaanisk M, Jarv A, Podar I, Allik J, Nilsson I, Sakthivel P, Lefvert AK, Hokfelt T. (2005) Autoantibodies against neuropeptides are associated with psychological traits in eating disorders. Proc Natl Acad Sci U S A, 102 (41), 14865-70. PMID 16195379.
- ↑ Rosen JC, Reiter J, Orosan P. (1995) Assessment of body image in eating disorders with the body dysmorphic disorder examination. Behav Res Ther, 1, 77-84. PMID 7872941.
- ↑ Skrzypek S, Wehmeier PM, Remschmidt H. (2001) Body image assessment using body size estimation in recent studies on anorexia nervosa. A brief review. Eur Child Adolesc Psychiatry, 10 (4), 215-21. PMID 11794546.
- ↑ Wonderlich SA, Lilenfeld LR, Riso LP, Engel S, Mitchell JE. (2005) Personality and anorexia nervosa. Int J Eat Disord, 37 Suppl, S68-71. PMID 15852324.
- ↑ Jansen A, Smeets T, Martijn C, Nederkoorn C. (2006) I see what you see: the lack of a self-serving body-image bias in eating disorders. Br J Clin Psychol, 45 (1), 123-35. PMID 16480571.
- ↑ 10.0 10.1 O'Brien KM, Vincent NK. (2003) Psychiatric comorbidity in anorexia and bulimia nervosa: nature, prevalence, and causal relationships. Clin Psychol Rev, 23 (1), 57-74. PMID 12559994
- ↑ Tchanturia K, Campbell IC, Morris R, Treasure J. (2005) Neuropsychological studies in anorexia nervosa. Int J Eat Disord, 37 Suppl, S72-6. PMID 15852325.
- ↑ Tiggemann M and Pickering AS. (1996) Role of television in adolescent women's body dissatisfaction and drive for thinness Int J Eat Disord, Sep;20(2):199-203.
- ↑ Cooper MJ (2005) Cognitive theory in anorexia nervosa and bulimia nervosa: progress, development and future directions. Clin Psychol Rev, 25 (4), 511-31. PMID 15914267.
- ↑ Fairburn CG, Cooper Z, Shafran R. (2003) Cognitive behavior therapy for eating disorders: a "transdiagnostic" theory and treatment. Behav Res Ther, 41 (5), 509-28. PMID 12711261.
- ↑ Garner DM, Garfinkel PE. (1980) Socio-cultural factors in the development of anorexia nervosa. Psychol Med, 10 (4), 647-56. PMID 7208724.
- ↑ Carter JC, Bewell C, Blackmore E, Woodside DB. (2006) The impact of childhood sexual abuse in anorexia nervosa. Child Abuse Negl, 30 (3), 257-69. PMID 16524628.
- ↑ Norris ML, Boydell KM, Pinhas L, Katzman DK. (2006) Ana and the internet: A review of pro-anorexia websites. International Journal of Eating Disorders, 39(6):443-7. PMID 16721839.
- ↑ Reaves, J. (2001). Anorexia goes high tech. Time (July). Retrieved on April 16, 2007.