Acetaminophen overdose resident survival guide
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Vidit Bhargava, M.B.B.S [2], Rim Halaby, M.D. [3]
Overview
Acetaminophen overdose is the intentional or accidental ingestion of a high dose of acetaminophen. Acute acetaminophen overdose occurs ≤8 hours before presentation, while chronic acetaminophen overdose occurs following the repeated supratherapeutic ingestion of acetaminophen.
Acetaminophen is available in the U.S. market under the following brand names:
- Tylenol
- Anacin-3
- Liquiprin
- Percocet
- Tempra
- Cold and flu medicines
- Aceta
- Actimin
- Apacet
- Aspirin Free Anacin
- Atasol
- Banesin
- Dapa
- Datril Extra-Strength
- Feverall
- Fibi
- Genapap
- Genebs
- Panadol
Acetaminophen Dosage
Shown below is a table summarizing the commonly used dosages of paracetamol.[1]
| Suppository | 120 mg, 125 mg, 325 mg, 650 mg |
| Chewable tablets | 80 mg |
| Regular strength | 325 mg |
| Extra strength | 500 mg |
| Liquid | 160 mg/teaspoon |
| Drops | 100 mg / mL, 120 mg / 2.5 mL |
Shown below is a table summarizing the recommended maximum doses of paracetamol.[1]
| Patients | Maximum single dose | Minimum dosing intervals (hours) | Maximum dose in 24 hours |
|---|---|---|---|
| Adults | 1 g | 4 | 4 g |
| Children 6-12 years | 500 mg | 4 | 2 g |
| Children 1-5 years | 240 mg | 4 | 960 mg |
| Infants 3-12 months | 120 mg | 4 | 480 mg |
Management
General Approach
Shown below is an algorithm depicting the approach to acetaminophen overdose.[2][3][4]
Obtain a focused history: ❑ Time since last ingestion ❑ Number of tablets/other dosing form taken ❑ Frequency of dosage ❑ Other ingested substances | |||||||||||||||||||||||||||||||||||||||
Characterize the symptoms & examine the patient: Stage I (first 24 hours): Preclinical toxic effects ❑ Asymptomatic ❑ Nausea & vomiting ❑ Diaphoresis ❑ Coma (with massive doses) Stage II (24 to 72 hours): Hepatic injury Stage III (72 to 96 hours): Hepatic failure | |||||||||||||||||||||||||||||||||||||||
Order labs: ❑ Serum paracetamol concentration (4 hours after acetaminophen ingestion, but not later than 16 hours) ❑ Liver function tests ❑ Prothrombin time (PT) or International normalized ratio (INR) ❑ Renal function tests | |||||||||||||||||||||||||||||||||||||||
| Clear information on the timing of acetaminophen ingestion | No clear information on the timing of acetaminophen ingestion | ||||||||||||||||||||||||||||||||||||||
| ❑ Order acetaminophen level ❑ Initiate N-acetylcysteine therapy without waiting for acetaminophen levels | |||||||||||||||||||||||||||||||||||||||
| < 2 hours | 2-4 hours | 4-8 hours | > 8 hours | Recurrent supratherapeutic ingestions | |||||||||||||||||||||||||||||||||||
❑ Administer activated charcoal 1g/kg (max 50 kg) ❑ Wait until 4 hours has passed and measure acetaminophen level | ❑ Wait until 4 hours has passed and measure acetaminophen level | ❑ Measure acetaminophen level | ❑ Order acetaminophen level ❑ Initiate N-acetylcysteine therapy without waiting for acetaminophen levels | Initiate N-acetlycysteine therapy if, one or more true: ❑ ALT is elevated, AND ❑ Ingestion of >4 g of acetaminophen per day OR ❑ Established hepatic failure | |||||||||||||||||||||||||||||||||||
| ❑ Plot acetaminophen level on the Rumack-Matthew nomogram | |||||||||||||||||||||||||||||||||||||||
| Acetaminophen level below the nomogram line ❑ Discharge home | Acetaminophen level above the nomogram line ❑ Initiate N-acetylcysteine therapy | ||||||||||||||||||||||||||||||||||||||
Acetylcysteine Therapy
Shown below is an algorithm depicting the oral and IV regimen of N-acetylcysteine.[2][3]
| N-Acetylcysteine treatment | |||||||||||||||||
Consider oral regimen in case of: ❑ Preclinical toxicity ❑ Hepatic injury | Consider IV regimen in case of: ❑ Malnourishment/eating disorders ❑ Failure to thrive in children ❑ AIDS ❑ Alcoholism ❑ Associated febrile illness ❑ Using drugs that induce CYP2E1 p450 system ♦ Carbamazepine, or phenytoin, or phenobarbital ❑ Vomiting and intolerance to oral regimen ❑ Altered mental status | ||||||||||||||||
| Outpatient | Critical care unit | ||||||||||||||||
| Oral regimen: ❑ Administer a loading dose of 140 mg/kg ❑ Administer a maintenance dose of 70 mg/kg every 4 hours for 17 doses | IV regimen: ❑ Administer 150 mg/kg in 200 mL glucose 5% solution infused over 15 minutes ❑ Administer 50 mg/kg in 500 mL glucose 5% solution infused over the next 4 hours ❑ Administer 100 mg/kg in 1000 mL glucose 5% solution over the following 16 hours | ||||||||||||||||
❑ Monitor the patient for vomiting after the loading dose ❑ Discharge the patient with three maintenance doses to be taken at home | ❑ Monitor ♦ Blood pressure ♦ Oxygen saturation ♦ Hypoglycemia ❑ Monitor the liver and renal function every 12 hours | ||||||||||||||||
| Reevaluate the patient in 12 hours ❑ Measure ALT level ❑ Measure acetaminophen level | Continue the treatment until: ❑ Resolution of encephalopathy ❑ Improvement of ALT, creatinine and INR ❑ The patient receives a liver transplant (if applicable) | ||||||||||||||||
Rumack-Matthew Nomogram
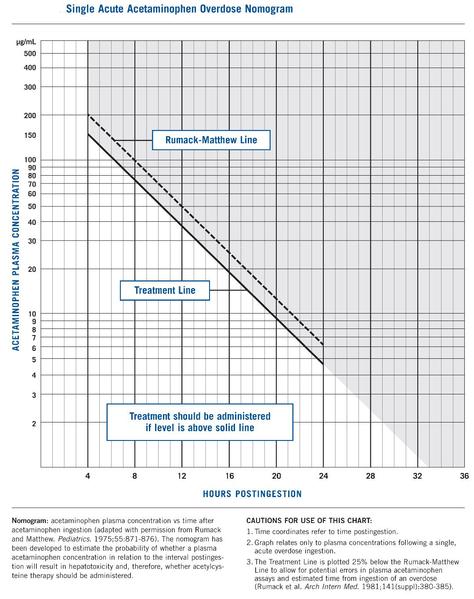
Criteria for Liver Transplantation
- Arterial pH < 7.3
- Hepatic encephalopathy grade III/IV
- Serum creatinine concentration > 300 μmol/L
- Prothrombin time > 100 seconds
- Arterial lactate concentration > 3.5 mmol/L on admission or > 3.0 mmol/L 24 hours after paracetamol ingestion[2]
Do's
- Measure serum acetaminophen concentrations between 4 and 16 hours post-ingestion. Values taken before 4 hours are not useful as it takes about 4 hours for maximal drug absorption. Likewise values taken after 16 hours are less useful as liver failure may have already occurred.
- Look for ketones on urinalysis and low blood urea concentration as a sign for malnourishment or starvation.
- In case of acetaminophen ingestion prior to 2 hours of the presentation, administer activated charcoal as it was found to be superior to gastric lavage and substance induced emesis, although both of them are potentially useful.[5][6]
- N-acetylcysteine can be administered 8 hours following the ingestion of acetaminophen; however, it is most beneficial within the first 8 hours of ingestion.
- Provide a supportive treatment when needed: fluid replacement, symptomatic treatment for nausea and vomiting, intensive supportive treatment in case of acute liver failure.
- If a patient vomits following oral N-acetylcysteine, administer a trial of anti emetic; however, in such cases IV N-acetylcysteine is preferred.
- Stop the infusion if IV N-acetylcysteine precipitates an anaphylactoid reaction, treat with H1-antihistaminics and resume IV N-acetylcysteine at a slower infusion rate.
- If acetaminophen level can not be obtained, assume that that patient has overdose of acetaminophen and treat with N-acetylcysteine.
- Consider liver transplantation if the patient has liver failure and meets the criteria for transplantation.[2][3][4]
Dont's
- Do not overlook acetaminophen in those who have signs suggestive of overdose with other agents.
- Do not use activated charcoal after 4 hours of acetaminophen ingestion.[7]
- Do not delay treatment with antidote more than 8 hours following the ingestion of acetaminophen.
- Do not use the Rumack-Matthew nomogram to stratify patients who ingested acetaminophen more than 8 hours ago or whose history of ingestion is unclear.[2][3][4]
References
- ↑ 1.0 1.1 Ferner, RE.; Dear, JW.; Bateman, DN. (2011). "Management of paracetamol poisoning". BMJ. 342: d2218. PMID 21508044.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Ferner RE, Dear JW, Bateman DN (2011). "Management of paracetamol poisoning". BMJ. 342: d2218. doi:10.1136/bmj.d2218. PMID 21508044.
- ↑ 3.0 3.1 3.2 3.3 Heard KJ (2008). "Acetylcysteine for acetaminophen poisoning". N Engl J Med. 359 (3): 285–92. doi:10.1056/NEJMct0708278. PMC 2637612. PMID 18635433.
- ↑ 4.0 4.1 4.2 Wallace CI, Dargan PI, Jones AL (2002). "Paracetamol overdose: an evidence based flowchart to guide management". Emerg Med J. 19 (3): 202–5. PMC 1725876. PMID 11971827.
- ↑ Buckley, NA.; Whyte, IM.; O'Connell, DL.; Dawson, AH. (1999). "Activated charcoal reduces the need for N-acetylcysteine treatment after acetaminophen (paracetamol) overdose". J Toxicol Clin Toxicol. 37 (6): 753–7. PMID 10584587.
- ↑ Underhill, TJ.; Greene, MK.; Dove, AF. (1990). "A comparison of the efficacy of gastric lavage, ipecacuanha and activated charcoal in the emergency management of paracetamol overdose". Arch Emerg Med. 7 (3): 148–54. PMID 1983801. Unknown parameter
|month=ignored (help) - ↑ Spiller, HA.; Winter, ML.; Klein-Schwartz, W.; Bangh, SA. (2006). "Efficacy of activated charcoal administered more than four hours after acetaminophen overdose". J Emerg Med. 30 (1): 1–5. doi:10.1016/j.jemermed.2005.02.019. PMID 16434328. Unknown parameter
|month=ignored (help)