Torsades de pointes medical therapy
|
Torsades de pointes Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Torsades de pointes medical therapy On the Web |
|
American Roentgen Ray Society Images of Torsades de pointes medical therapy |
|
Risk calculators and risk factors for Torsades de pointes medical therapy |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Medical Therapy
Acute Treatment
If the episode of does not terminate on its own and degenerates into ventricular fibrillation, cardioversion is required.
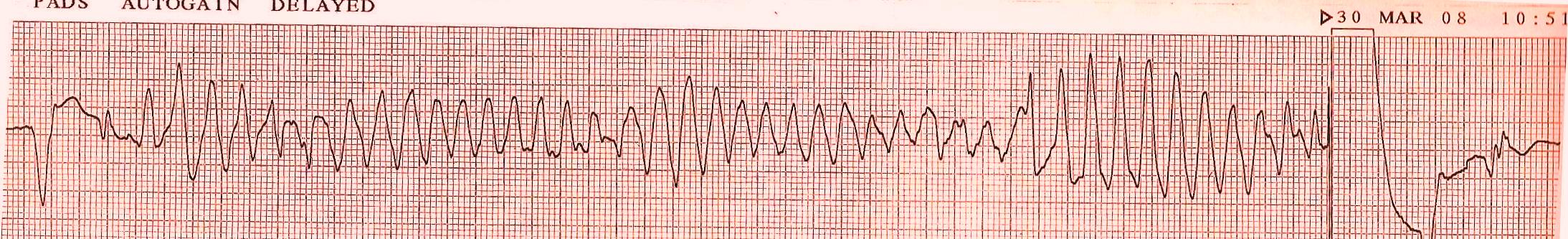
Once the patient is back in normal sinus rhythm, a vigorous search for and correction of conditions that predispose to torsades de pointes which include hypokalemia, hypomagnesemia, and bradycardia should be made. Magnesium sulfate (1-2 g IV over 30-60 seconds) reduces the influx of calcium thereby lowering the amplitude of early after depolarizations and should also be infused even if the magnesium is normal. [1][2] Administration of lidocaine is generally not effective, but mexiletene may be helpful in suppressing the recurrence of torsade de pointe.
References
- ↑ Hoshino K, Ogawa K, Hishitani T, Isobe T, Eto Y (2004). "Optimal administration dosage of magnesium sulfate for torsades de pointes in children with long QT syndrome". J Am Coll Nutr. 23 (5): 497S–500S. PMID 15466950. Unknown parameter
|month=ignored (help) - ↑ Hoshino K, Ogawa K, Hishitani T, Isobe T, Etoh Y (2006). "Successful uses of magnesium sulfate for torsades de pointes in children with long QT syndrome". Pediatr Int. 48 (2): 112–7. doi:10.1111/j.1442-200X.2006.02177.x. PMID 16635167. Unknown parameter
|month=ignored (help)