Testicular cancer natural history, complications and prognosis: Difference between revisions
No edit summary |
No edit summary |
||
| Line 1: | Line 1: | ||
__NOTOC__ | __NOTOC__ | ||
{{CMG}}; {{AE}} {{Rim}} {{SC}} | {{CMG}}; {{AE}} {{G.D}},{{Rim}} {{SC}} | ||
{{Testicular cancer}} | {{Testicular cancer}} | ||
==Overview== | ==Overview== | ||
[[Prognosis]] of testicular cancer is generally good, and the 5-year survival rate is approximately 96.6% (2004-2010).Common complications of testicular cancer include [[metastasis]], [[bleeding]], [[infection]], and [[infertility]]. | [[Prognosis]] of testicular cancer is generally good, and the 5-year survival rate is approximately 96.6% (2004-2010).Common complications of testicular cancer include [[metastasis]], [[bleeding]], [[infection]], and [[infertility]]. | ||
==Natural History== | |||
==Seminoma== | |||
*Seminoma tends to occur in middle aged people | |||
*Rarely metastasize<ref name="pmid26612222">{{cite journal |vauthors=Howitt BE, Berney DM |title=Tumors of the Testis: Morphologic Features and Molecular Alterations |journal=Surg Pathol Clin |volume=8 |issue=4 |pages=687–716 |date=December 2015 |pmid=26612222 |doi=10.1016/j.path.2015.07.007 |url=}}</ref> | |||
*Affects people in their 15 and 35 year old | |||
==Embryonal Cancer== | |||
*Median age is 30 years old<ref name="pmid26612222">{{cite journal |vauthors=Howitt BE, Berney DM |title=Tumors of the Testis: Morphologic Features and Molecular Alterations |journal=Surg Pathol Clin |volume=8 |issue=4 |pages=687–716 |date=December 2015 |pmid=26612222 |doi=10.1016/j.path.2015.07.007 |url=}}</ref> | |||
*Has most of the component of mixed non seminoma germ tumor<ref name="pmid26612222">{{cite journal |vauthors=Howitt BE, Berney DM |title=Tumors of the Testis: Morphologic Features and Molecular Alterations |journal=Surg Pathol Clin |volume=8 |issue=4 |pages=687–716 |date=December 2015 |pmid=26612222 |doi=10.1016/j.path.2015.07.007 |url=}}</ref> | |||
*Tend to metastasize early to lungs, retroperitomeun, and liver<ref name="pmid19066212">{{cite journal |vauthors=Ishida M, Hasegawa M, Kanao K, Oyama M, Nakajima Y |title=Non-palpable testicular embryonal carcinoma diagnosed by ultrasound: a case report |journal=Jpn. J. Clin. Oncol. |volume=39 |issue=2 |pages=124–6 |date=February 2009 |pmid=19066212 |doi=10.1093/jjco/hyn141 |url=}}</ref> | |||
==Choriocarcinoma== | |||
==Complications== | ==Complications== | ||
Revision as of 09:14, 8 April 2019
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Template:G.D,Rim Halaby, M.D. [2] Shanshan Cen, M.D. [3]
|
Testicular cancer Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Testicular cancer natural history, complications and prognosis On the Web |
|
American Roentgen Ray Society Images of Testicular cancer natural history, complications and prognosis |
|
FDA on Testicular cancer natural history, complications and prognosis |
|
CDC on Testicular cancer natural history, complications and prognosis |
|
Testicular cancer natural history, complications and prognosis in the news |
|
Blogs on Testicular cancer natural history, complications and prognosis |
|
Risk calculators and risk factors for Testicular cancer natural history, complications and prognosis |
Overview
Prognosis of testicular cancer is generally good, and the 5-year survival rate is approximately 96.6% (2004-2010).Common complications of testicular cancer include metastasis, bleeding, infection, and infertility.
Natural History
Seminoma
- Seminoma tends to occur in middle aged people
- Rarely metastasize[1]
- Affects people in their 15 and 35 year old
Embryonal Cancer
- Median age is 30 years old[1]
- Has most of the component of mixed non seminoma germ tumor[1]
- Tend to metastasize early to lungs, retroperitomeun, and liver[2]
Choriocarcinoma
Complications
Common complications of testicular cancer include:
- Abdomen
- Lungs
- Retroperitoneal area
- Brain
- Post-surgery complications
Prognosis
- Between 2004 and 2010, the 5-year relative survival of patients with testicular cancer was 96.6%.[3]
- When stratified by age, the 5-year relative survival of patients with testicular cancer was 95.4% and 86.4% for patients <65 and ≥ 65 years of age respectively.[3]
- The survival of patients with testicular cancer varies with the stage of the disease. Shown below is a table depicting the 5-year relative survival by the stage of testicular cancer:[3]
| Stage | 5-year relative survival (%), (2004-2010) |
| All stages | 95.3% |
| Localized | 99.2% |
| Regional | 96% |
| Distant | 73.1% |
| Unstaged | 78.8% |
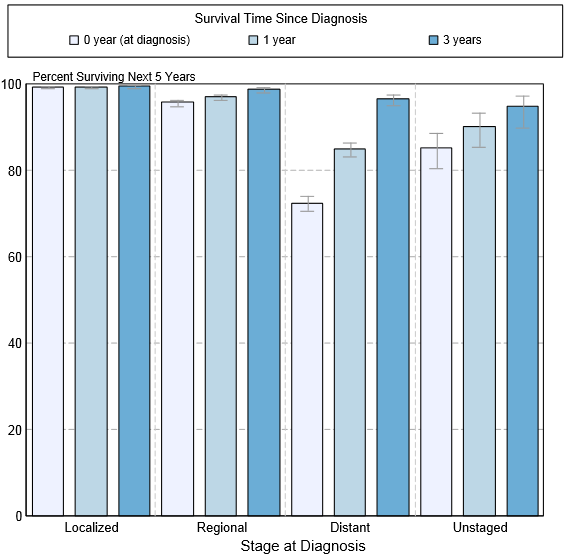
- Shown below is an image depicting the 5-year conditional relative survival (probability of surviving in the next 5-years given the cohort has already survived 0, 1, 3 years) between 1998 and 2010 of testicular cancer by stage at diagnosis according to SEER. These graphs are adapted from SEER: The Surveillance, Epidemiology, and End Results Program of the National Cancer Institute.[3]
References
- ↑ 1.0 1.1 1.2 Howitt BE, Berney DM (December 2015). "Tumors of the Testis: Morphologic Features and Molecular Alterations". Surg Pathol Clin. 8 (4): 687–716. doi:10.1016/j.path.2015.07.007. PMID 26612222.
- ↑ Ishida M, Hasegawa M, Kanao K, Oyama M, Nakajima Y (February 2009). "Non-palpable testicular embryonal carcinoma diagnosed by ultrasound: a case report". Jpn. J. Clin. Oncol. 39 (2): 124–6. doi:10.1093/jjco/hyn141. PMID 19066212.
- ↑ 3.0 3.1 3.2 3.3 Howlader N, Noone AM, Krapcho M, Garshell J, Miller D, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z,Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (eds). SEER Cancer Statistics Review, 1975-2011, National Cancer Institute. Bethesda, MD, http://seer.cancer.gov/csr/1975_2011/, based on November 2013 SEER data submission, posted to the SEER web site, April 2014.