Diabetes mellitus type 2 (patient information)
| https://https://www.youtube.com/watch?v=QRLZwXL6w1c%7C350}} |
|
Diabetes mellitus type 2 |
|
Diabetes mellitus type 2 On the Web |
|---|
|
Risk calculators and risk factors for Diabetes mellitus type 2 |
For the WikiDoc page for this topic, click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Jinhui Wu, M.D.; Laura Linnemeier
Overview
Diabetes is a disease in which blood glucose levels are above normal. Type 2 diabetes, also known as adult-onset diabetes, is the most common form of diabetes, accounting for 90-95% of all diagnosed cases of diabetes. In type 2 diabetes, either the body does not produce enough insulin or the cells ignore the insulin. Insulin is necessary for the body to be able to use glucose for energy. When you eat food, the body breaks down all of the sugars and starches into glucose, which is the basic fuel for the cells in the body. Insulin takes the sugar from the blood into the cells. When glucose builds up in the blood instead of going into cells, it can cause two problems: Right away, your cells may be starved for energy and over time, high blood glucose levels may hurt your eyes, kidneys, nerves or heart.
What are the symptoms of Diabetes mellitus type 2?
Pre-Diabetes
Before people develop type 2 diabetes, they almost always have "pre-diabetes" -- blood glucose levels that are higher than normal but not yet high enough to be diagnosed as diabetes. There are 57 million people in the United States who have pre-diabetes. About 11 percent of people with pre-diabetes in the Diabetes Prevention Program standard or control group developed type 2 diabetes each year during the average 3 years of follow-up. Other studies show that many people with pre-diabetes develop type 2 diabetes in 10 years. Recent research has shown that some long-term damage to the body, especially the heart and circulatory system, may already be occurring during pre-diabetes.
Symptoms
People with diabetes may exhibit some or none of the following symptoms:
- Frequent urination
- Excessive thirst
- Unexplained weight loss
- Extreme hunger
- Sudden vision changes
- Tingling or numbness in hands or feet
- Fatigue
- Very dry skin
- Sores that are slow to heal
- More infections than usual
Diseases with similar symptoms
What causes Diabetes mellitus type 2?
Diabetes is caused by a problem in the way your body makes or uses insulin. Insulin is needed to move blood sugar (glucose) into cells, where it is stored and later used for energy. When you have type 2 diabetes, the body does not respond correctly to insulin. This is called insulin resistance. Insulin resistance means that fat, liver, and muscle cells do not respond normally to insulin. As a result blood sugar does not get into cells to be stored for energy.
When sugar cannot enter cells, abnormally high levels of sugar build up in the blood. This is called hyperglycemia. High levels of blood sugar often trigger the pancreas to produce more and more insulin, but it is not enough to keep up with the body's demand. People who are overweight are more likely to have insulin resistance, because fat interferes with the body's ability to use insulin.
Type 2 diabetes usually occurs gradually. Most people with the disease are overweight at the time of diagnosis. However, type 2 diabetes can also develop in those who are thin, especially the elderly. Family history and genetics play a large role in type 2 diabetes. Low activity level, poor diet, and excess body weight (especially around the waist) significantly increase your risk for type 2 diabetes.
Who is at highest risk?
Risk factors for type 2 diabetes include:
- Older age
- Obesity or being overweight
- Family history of diabetes
- Prior history of gestational diabetes (a type of diabetes that only pregnant women get)
- Or birth of at least one baby weighing more than 9 pounds
- nearly 40% of women with a history of gestational diabetes developed diabetes in the future
- High blood pressure measuring 140/90 or higher
- Abnormal cholesterol with HDL ("good") cholesterol is 35 or lower, or triglyceride level is 250 or higher
- Impaired glucose tolerance
- Physical inactivity (exercising fewer than 3 times a week)
- Race/ethnicity
African Americans, Hispanic/Latino Americans, American Indians, and some Asian Americans and Pacific Islanders are at particularly high risk for type 2 diabetes. Are you at risk for diabetes mellitus type 2? Take the American Diabetes Association Risk Test!
When to seek urgent medical care?
Anyone aged 45 years or older should consider getting tested for diabetes, especially if you are overweight. If you are younger than 45, but are overweight and have one or more additional risk factors, you should consider testing. In addition, if blood glucose levels get too high or low, urgent medical care may be needed to prevent losing consciousness or a diabetic coma.
Diagnosis
There are two different tests your doctor can use to determine whether you have pre-diabetes or diabetes: the fasting plasma glucose test (FPG) or the oral glucose tolerance test (OGTT). The blood glucose levels measured after these tests determine whether you have a normal metabolism, or whether you have pre-diabetes or diabetes. If your blood glucose level is abnormal following the FPG, you have impaired fasting glucose (IFG); if your blood glucose level is abnormal following the OGTT, you have impaired glucose tolerance (IGT).
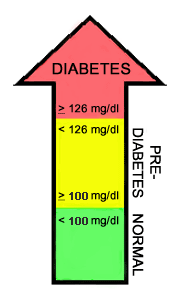
FPG OGTT
When to seek urgent medical care?
Treatment options
The main goal of treatment is to get your blood glucose (sugar) levels under control in order to increase your chances of a complication-free life. People with diabetes should see a health care provider who will monitor their diabetes control and help them learn to manage their diabetes. In addition, many people with type 2 diabetes require oral medication, insulin, or both to control their blood glucose levels.
Healthy Living
Healthy eating, physical activity, and blood glucose testing are the basic therapies for type 2 diabetes. People with diabetes must take responsibility for their day-to-day care, and keep blood glucose levels from going too low or too high. Blood glucose monitoring is the main tool you have to check your diabetes control. This check tells you your blood glucose level at any one time. Keeping a log of your results is vital. When you bring this record to your health care provider, you have a good picture of your body's response to your diabetes care plan. Blood glucose checks let you see what works and what doesn't. This allows you and your doctor, dietitian, or nurse educator to make needed changes.
How do blood checks work? You stick your finger with a special needle, called a lancet, to get a drop of blood. With some meters, you can also use your forearm, thigh or fleshy part of your hand. There are spring-loaded lancing devices that make sticking yourself less painful. Before using the lancing device, wash your hands or site you chose with soap and water. If you use your fingertip, stick the side of your fingertip by your fingernail to avoid having sore spots on the frequently used part of your finger. Blood glucose meters are small computerized machines that "read" your blood glucose. In all types of meters, your blood glucose level shows up as a number on a screen (like that on your pocket calculator). Be sure your doctor or nurse educator shows you the correct way to use your meter. With all the advances in blood glucose meters, use of a meter is better than visual checking. In addition, you may need to check your urine for ketones once in a while. Ketones in the urine is a sign that your body is using fat for energy instead of using glucose because not enough insulin is available to use glucose for energy. Ketones in the urine is more common in type 1 diabetes however.
Insulin
Inside the pancreas, beta cells make the hormone insulin. With each meal, beta cells release insulin to help the body use or store the blood glucose it gets from food. People with type 2 diabetes make insulin, but their bodies don't respond well to it. Some people with type 2 diabetes need diabetes pills or insulin shots to help their bodies use glucose for energy. Insulin cannot be taken as a pill. The insulin would be broken down during digestion just like the protein in food. Insulin must be injected into the fat under your skin for it to get into your blood. There are many different insulins for many different situations and lifestyles and there are more than 20 types of insulin sold in the United States. These insulins differ in how they are made, how they work in the body, and price.
Diabetes Pills
The first treatment for type 2 diabetes is often meal planning for blood glucose (sugar) control, weight loss, and exercising. Sometimes these measures are not enough to bring blood glucose levels down near the normal range. The next step is taking a medicine that lowers blood glucose levels. All diabetes pills sold today in the United States are members of five classes of drugs: sulfonylureas, meglitinides, biguanides, thiazolidinediones, and alpha-glucosidase inhibitors. These five classes of drugs work in different ways to lower blood glucose levels. Diabetes pills don't work for everyone. These pills work best when used with meal planning and exercise. This way you have three therapies working together to lower your blood glucose levels. Your chances of diabetes pills working are low if you have had diabetes for more than 10 years or already take more than 20 units of insulin each day. On the other hand, your chances are good if you developed diabetes recently or have needed little or no insulin to keep your blood glucose levels near normal. Diabetes pills sometimes stop working after a few months or years. Even if diabetes pills do bring your blood glucose levels near the normal range, you may still need to take insulin if you have a severe infection or need surgery. Pills may not be able to control blood glucose levels during these stressful times when blood glucose levels shoot up. Also, if you plan to become pregnant, you will need to control your diabetes with diet and exercise or with insulin. It is not safe for pregnant women to take oral diabetes medications.
Combination Therapy
Because diabetes pills seem to help the body use insulin better, some people take them along with insulin shots. The idea behind this "combination" therapy is to try to help insulin work better.
Other
In addition, people with diabetes may see endocrinologists, who may specialize in diabetes care; ophthalmologists for eye examinations; podiatrists for routine foot care; and dietitians and diabetes educators who teach the skills needed for daily diabetes management. Adults with diabetes are at high risk for cardiovascular disease (CVD). In fact, at least 65 percent of those with diabetes die from heart disease or stroke. Managing diabetes is more than keeping blood glucose levels under control—it is also important to manage blood pressure and cholesterol levels through healthy eating, physical activity, and the use of medications, if needed. By doing so, those with diabetes can lower their risk. Aspirin therapy, if recommended by a person’s health care team, and smoking cessation can also help lower risk.
Medications to avoid
Patients diagnosed with Type 2 Diebetes should avoid using the following medications:
- Eplerenone
If you have been diagnosed with Type 2 Diebetes, consult your physician before starting or stopping any of these medications.
Where to find medical care for Diabetes mellitus type 2?
Directions to hospitals treating Diabetes mellitus type 2
What to expect (Outlook/Prognosis)?
Hypoglycemia, Hyperglycemia, and a High Risk for Diabetic Comas
Hypoglycemia, low blood glucose (sugar), sometimes called an insulin reaction, can happen even during those times when you're doing all you can to manage your diabetes. So, although many times you can't prevent it from happening, hypoglycemia can be treated before it gets worse. The symptoms of hypoglycemia include:
- Shakiness
- Dizziness
- Sweating
- Hunger
- Headache
- Pale skin color
- Sudden moodiness or behavior changes, such as crying for no apparent reason
- Clumsy or jerky movements
- Seizure
- Difficulty paying attention, or confusion
- Tingling sensations around the mouth
The quickest way to raise your blood glucose and treat hypoglycemia is with some form of sugar, such as 3 glucose tablets (you can buy these at the drug store), 1/2 cup of fruit juice, or 5-6 pieces of hard candy. Ask your health care professional or dietitian to list foods that you can use to treat low blood glucose. Good diabetes control is the best way we know to prevent hypoglycemia. Hyperglycemia is the technical term for high blood glucose (sugar). High blood glucose happens when the body has too little, or not enough, insulin or when the body can't use insulin properly. If you have type 2 diabetes, your body may have enough insulin, but it is not as effective as it should be. The problem could be that you ate more than planned or exercised less than planned. The stress of an illness, such as a cold or flu, could also be the cause. Other stresses, such as family conflicts or school or dating problems, could also cause hyperglycemia. The signs and symptoms include: high blood glucose, high levels of sugar in the urine, frequent urination, and increased thirst. It's important to treat hyperglycemia as soon as you detect it. If you fail to treat hyperglycemia, a condition called ketoacidosis (diabetic coma) could occur. Ketoacidosis develops when your body doesn't have enough insulin. Often, you can lower your blood glucose level by exercising. Cutting down on the amount of food you eat might also help. Your best bet to prevent hyperglycemia is to practice good diabetes management. Ketoacidosis is life-threatening and needs immediate treatment. It can occur when a case of hyperglycemia gets out of control. Symptoms include:
- Shortness of breath
- Breath that smells fruity
- Nausea and vomiting
- Very dry mouth
Possible complications
Heart Disease and Stroke
People with diabetes have extra reason to be mindful of heart and blood vessel disease. Diabetes carries an increased risk for heart attack, stroke, and complications related to poor circulation. 2 out of 3 people with diabetes die from heart disease or stroke. Diabetes management is more than control of blood glucose. People with diabetes must also manage blood pressure and cholesterol and talk to their health provider to learn about other ways to reduce their chance for heart attacks and stroke. Again, lifestyle changes, such as choosing foods wisely and being physically active, as well as taking medication can help. Many people find that changing what they eat can make a big difference in their blood glucose, blood pressure, and cholesterol levels.
Kidney Disease
Diabetes can damage the kidneys, which not only can cause them to fail, but can also make them lose their ability to filter out waste products. Diabetes can damage the filtering ability of kidneys. High levels of blood sugar make the kidneys filter too much blood. All this extra work is hard on the filters. After many years, they start to leak. Useful protein is lost in the urine. Having small amounts of protein in the urine is called microalbuminuria. When kidney disease is diagnosed early, (during microalbuminuria), several treatments may keep kidney disease from getting worse. Having larger amounts is called macroalbuminuria. When kidney disease is caught later (during macroalbuminuria), end-stage renal disease, or ESRD, usually follows. In time, the stress of overwork causes the kidneys to lose their filtering ability. Waste products then start to build up in the blood. Finally, the kidneys fail. This failure, ESRD, is very serious. A person with ESRD needs to have a kidney transplant or to have the blood filtered by machine (dialysis). Diabetic kidney disease can be prevented by keeping blood sugar in your target range.
Eye Complications
People with diabetes are 40% more likely to suffer from glaucoma than people without diabetes. The longer someone has had diabetes, the more common glaucoma is. Risk also increases with age. Glaucoma occurs when pressure builds up in the eye, and vision is gradually lost because the retina and nerve are damaged. Many people without diabetes get cataracts, but people with diabetes are 60% more likely to develop this eye condition. People with diabetes also tend to get cataracts at a younger age and have them progress faster. With cataracts, the eye's clear lens clouds, blocking light. Diabetic retinopathy is a general term for all disorders of the retina caused by diabetes. In nonproliferative retinopathy, capillaries in the back of the eye balloon and form pouches. Nonproliferative retinopathy can move through three stages (mild, moderate, and severe), as more and more blood vessels become blocked. In some people, retinopathy progresses after several years to a more serious form called proliferative retinopathy which can lead to blindness caused by retinal detachment. People who keep their blood sugar levels closer to normal are less likely to have retinopathy or to have milder forms.
Diabetic Neuropathy and Nerve Damage
One of the most common complications of diabetes is diabetic neuropathy. Neuropathy means damage to the nerves that run throughout the body, connecting the spinal cord to muscles, skin, blood vessels, and other organs. There are two common types of nerve damage. The first is sensorimotor neuropathy, also known as peripheral neuropathy. This can cause tingling, pain, numbness, or weakness in your feet and hands. The second is called autonomic neuropathy. This type can lead to:
- Digestive problems such as feeling full, nausea,
- Vomiting, diarrhea, or constipation
- Problems with how well your bladder works
- Problems having sex
- Dizziness or faintness
- Loss of the typical warning signs of a heart attack
- Loss of the warning signs of low blood glucose
- Increased or decreased sweating
- Changes in how your eyes react to light and dark
People with diabetes can also have what is called focal neuropathy. In this kind of nerve damage, a nerve or a group of nerves is affected, causing sudden weakness or pain. It can lead to double vision, a paralysis on one side of the face called Bell's palsy, or pain in the front of the thigh or other parts of the body. People with diabetes also are at risk for compressed nerves. Something in the body presses against a nerve preventing it from sending a signal. Carpal tunnel syndrome is a common cause of numbness and tingling in the fingers and can lead to muscle pain and weakness as well. Keeping your blood glucose levels in the target range can prevent or delay further damage and may lessen your symptoms.
Foot Complications
Although it can hurt, diabetic nerve damage can also lessen your ability to feel pain, heat, and cold. Loss of feeling often means you may not feel a foot injury. You might not notice a foot injury until the skin breaks down and becomes infected. Nerve damage can also lead to changes in the shape of your feet and toes. Ulcers occur most often on the ball of the foot or on the bottom of the big toe. Neglecting ulcers can result in infections, which in turn can lead to loss of a limb. Poor circulation (blood flow) can make your foot less able to fight infection and to heal. Diabetes causes blood vessels of the foot and leg to narrow and harden. You can control some of the things that cause poor blood flow. Don't smoke - smoking makes arteries harden faster. People with diabetes are far more likely to have a foot or leg amputated than other people. The problem? Many people with diabetes have artery disease, which reduces blood flow to the feet. Also, many people with diabetes have nerve disease, which reduces sensation. Together, these problems make it easy to get ulcers and infections that may lead to amputation. One of the biggest threats to your feet is smoking. Smoking affects small blood vessels. It can cause decreased blood flow to the feet and make wounds heal slowly. A lot of people with diabetes who need amputations are smokers.
Gastroparesis
Gastroparesis is a disorder affecting people with both type 1 and type 2 diabetes, where the stomach takes too long to empty its contents. It happens when nerves to the stomach are damaged or stop working. The vagus nerve controls the movement of food through the digestive tract. If the vagus nerve is damaged, the muscles of the stomach and intestines do not work normally, and the movement of food is slowed or stopped. Gastroparesis can make diabetes worse by making it more difficult to manage blood glucose. When food that has been delayed in the stomach finally enters the small intestine and is absorbed, blood glucose levels rise. If food stays too long in the stomach, it can cause problems like bacterial overgrowth because the food has fermented. Also, the food can harden into solid masses called bezoars that may cause nausea, vomiting, and obstruction in the stomach. Bezoars can be dangerous if they block the passage of food into the small intestine.
Prevention
A number of studies have shown that regular physical activity and a healthy diet can significantly reduce the risk of developing type 2 diabetes. Type 2 diabetes also appears to be associated with obesity. The Diabetes Prevention Program (DPP), a major federally funded study of 3,234 people at high risk for diabetes, showed that moderate diet and exercise of about 30 minutes or more, 5 or more days per week, or of 150 or more minutes per week, resulting in a 5% to 7% weight loss can delay and possibly prevent type 2 diabetes. Below are several strategies for making wise food and exercise choices. Determine which ones you would be willing to try.
- I’ll eat less fat, especially saturated fat (found in fatty meats, poultry skin, butter, 2% or whole milk, ice cream, cheese, palm oil, coconut oil, trans fats, hydrogenated oils, lard, and shortening).
- I’ll choose lean meats and meat substitutes.
- I’ll switch to low-fat or fat-free dairy products.
- I’ll eat at least 5 servings of fruits and vegetables each day.
- I’ll cut back on foods that are high in cholesterol (such as egg yolks, high-fat meat and poultry, and high-fat dairy products).
- I’ll choose the kinds of fat that can help lower my cholesterol, such as olive oil or canola oil. Nuts also have a healthy type of fat.
- I’ll eat fish two or three times a week, choosing kinds that are high in heart-protective fat (such as albacore tuna, herring, mackerel, rainbow trout, sardines, and salmon).
- I’ll cook using low-fat methods (such as baking, roasting, or grilling foods or by using nonstick pans and cooking sprays).
- I’ll eat more foods that are high in fiber (such as oatmeal, oat bran, dried beans and peas like kidney beans, fruits, and vegetables).
- I’ll eat less salt and sodium.
- I’ll cut down on calories and fat.
- I’ll try to be more physically active than I am now.
What kind of a diet prevents or slows down the onset of type II diabetes? Check out what the American Diabetes Association recommends! What kind of exercise prevents or slows down the onset of type II diabetes? Check out what the American Diabetes Association recommends!