Brain tumor
For patient information click here
| Brain tumor | |
 | |
|---|---|
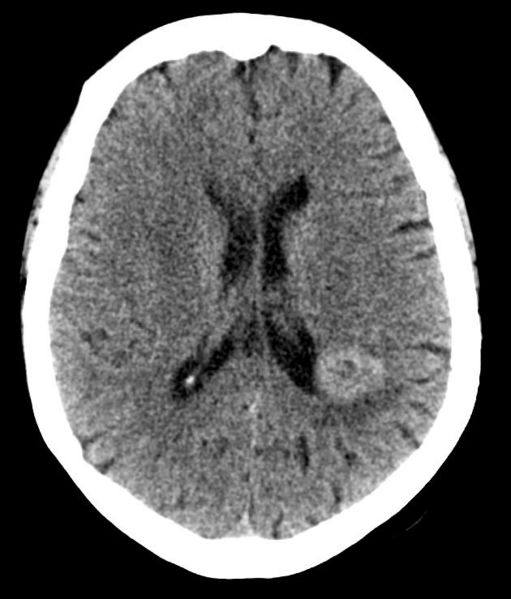
| CT scan of brain showing brain cancer to left parietal lobe in the peri-ventricular area. | |
| ICD-10 | C71, D33.0-D33.2 |
| ICD-9 | 191, 225.0 |
| DiseasesDB | 30781 |
| MedlinePlus | 007222 000768 |
|
Brain tumor Microchapters |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Classification
Historical Perspective
Pathophysiology
Epidemiology and Demographics
Risk Factors
Screening
Causes
Diagnosis
Although there is no specific clinical symptom or sign for brain tumors, slowly progressive focal neurologic signs and signs of elevated intracranial pressure, as well as epilepsy in a patient with a negative history for epilepsy should raise red flags. However, a sudden onset of symptoms, such as an epileptic seizure in a patient with no prior history of epilepsy, sudden intracranial hypertension (this may be due to bleeding within the tumor, brain swelling or obstruction of cerebrospinal fluid's passage) is also possible.
Symptoms include phantom odors and tastes. Often, in the case of metastatic tumors, the smell of vulcanized rubber is prevalent.
Imaging plays a central role in the diagnosis of brain tumors. Early imaging methods—invasive and sometimes dangerous—such as pneumoencephalography and cerebral angiography, have been abandoned in recent times in favor of non-invasive, high-resolution modalities, such as computed tomography (CT) and especially magnetic resonance imaging (MRI). Benign brain tumors often show up as hypodense (darker than brain tissue) mass lesions on cranial CT-scans. On MRI, they appear either hypo- (darker than brain tissue) or isointense (same intensity as brain tissue) on T1-weighted scans, or hyperintense (brighter than brain tissue) on T2-weighted MRI. Perifocal edema also appears hyperintense on T2-weighted MRI. Contrast agent uptake, sometimes in characteristic patterns, can be demonstrated on either CT or MRI-scans in most malignant primary and metastatic brain tumors. This is due to the fact that these tumors disrupt the normal functioning of the blood-brain barrier and lead to an increase in its permeability.
Electrophysiological exams, such as electroencephalography (EEG) play a marginal role in the diagnosis of brain tumors.
The definitive diagnosis of brain tumor can only be confirmed by histological examination of tumor tissue samples obtained either by means of brain biopsy or open surgery. The histologic examination is essential for determining the appropriate treatment and the correct prognosis.
Treatment and prognosis
Meningiomas, with the exception of some tumors located at the skull base, can be successfully removed surgically, but the chances are less than 50%. In more difficult cases, stereotactic radiosurgery, such as Gamma Knife radiosurgery, remains a viable option.
Most pituitary adenomas can be removed surgically, often using a minimally invasive approach through the nasal cavity and skull base (trans-nasal, trans-sphenoidal approach). Large pituitary adenomas require a craniotomy (opening of the skull) for their removal. Radiotherapy, including stereotactic approaches, is reserved for the inoperable cases.
Although there is no generally accepted therapeutic management for primary brain tumors, a surgical attempt at tumor removal or at least cytoreduction (that is, removal of as much tumor as possible, in order to reduce the number of tumor cells available for proliferation) is considered in most cases[1]. However, due to the infiltrative nature of these lesions, tumor recurrence, even following an apparently complete surgical removal, is not uncommon. Postoperative radiotherapy and chemotherapy are integral parts of the therapeutic standard for malignant tumors. Radiotherapy may also be administered in cases of "low-grade" gliomas, when a significant tumor burden reduction could not be achieved surgically.
Survival rates in primary brain tumors depend on the type of tumor, age, functional status of the patient, the extent of surgical tumor removal, to mention just a few factors[2].
Patients with benign gliomas may survive for many years[3][4] while survival in most cases of glioblastoma multiforme is limited to a few months after diagnosis.
The main treatment option for single metastatic tumors is surgical removal, followed by radiotherapy and/or chemotherapy. Multiple metastatic tumors are generally treated with radiotherapy and chemotherapy. Stereotactic radiosurgery, such as Gamma Knife radiosurgery, remains a viable option. However, the prognosis in such cases is determined by the primary tumor, and it is generally poor.
A shunt operation is used not as a cure but to relieve the symptoms.[2] The hydrocephalus caused by the blocking drainage of the cerebrospinal fluid can be removed with this operation.
References
- ↑ Nakamura M, Konishi N, Tsunoda S, Nakase H, Tsuzuki T, Aoki H, Sakitani H, Inui T, Sakaki T. Analysis of prognostic and survival factors related to treatment of low-grade astrocytomas in adults. Oncology 2000;58:108-16. PMID 10705237.
- ↑ Nicolato A, Gerosa MA, Fina P, Iuzzolino P, Giorgiutti F, Bricolo A. Prognostic factors in low-grade supratentorial astrocytomas: a uni-multivariate statistical analysis in 76 surgically treated adult patients. Surg Neurol 1995;44:208-21; discussion 221-3. PMID 8545771.
- ↑ Janny P, Cure H, Mohr M, Heldt N, Kwiatkowski F, Lemaire JJ, Plagne R, Rozan R. Low grade supratentorial astrocytomas. Management and prognostic factors. Cancer 1994;73:1937-45. PMID 8137221.
- ↑ Piepmeier J, Christopher S, Spencer D, Byrne T, Kim J, Knisel JP, Lacy J, Tsukerman L, Makuch R. Variations in the natural history and survival of patients with supratentorial low-grade astrocytomas. Neurosurgery 1996;38:872-8; discussion 878-9. PMID 8727811.