Lung cancer CT: Difference between revisions
No edit summary |
|||
| (6 intermediate revisions by the same user not shown) | |||
| Line 4: | Line 4: | ||
==Overview== | ==Overview== | ||
Chest CT scan | Chest CT scan is the modality of choice in the diagnosis of lung cancer. Findings on CT scan suggestive of lung cancer include, a solitary [[pulmonary nodule]], centrally located [[Tumor|masses]], [[Mediastinum|mediastinal]] invasion | ||
CT scans help stage the lung cancer. A CT scan of the abdomen and brain can help visualize the common sights of metastases: adrenal glands, liver, and brain. CT scans diagnose lung cancer by providing anatomical detail to locate the [[tumor]], demonstrating proximity to nearby structures, and deciphering whether [[lymph nodes]] are enlarged in the [[mediastinum]]. | CT scans help stage the lung cancer. A CT scan of the abdomen and brain can help visualize the common sights of metastases: adrenal glands, liver, and brain. CT scans diagnose lung cancer by providing anatomical detail to locate the [[tumor]], demonstrating proximity to nearby structures, and deciphering whether [[lymph nodes]] are enlarged in the [[mediastinum]]. | ||
== CT Scan == | == CT Scan == | ||
Chest CT scan is the modality of choice in the diagnosis of lung cancer. Findings on CT scan suggestive of lung cancer include:<ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref> | |||
*Solitary [[pulmonary nodule]] | |||
*Centrally located [[Tumor|masses]] | |||
*[[Mediastinum|Mediastinal]] invasion | |||
*Peripherally situated [[Lesion|lesions]] invading the [[Thoracic cavity|chest wall]] | |||
*A [[Ground glass opacification on CT|ground-glass opacity]] | |||
*[[Consolidation (medicine)|Consolidation]] | |||
*Mixed density or pure ground glass [[Nodule (medicine)|nodules]] | |||
*Mixed density or pure ground glass [[Consolidation (medicine)|consolidation]] | |||
{| class="wikitable" | {| class="wikitable" | ||
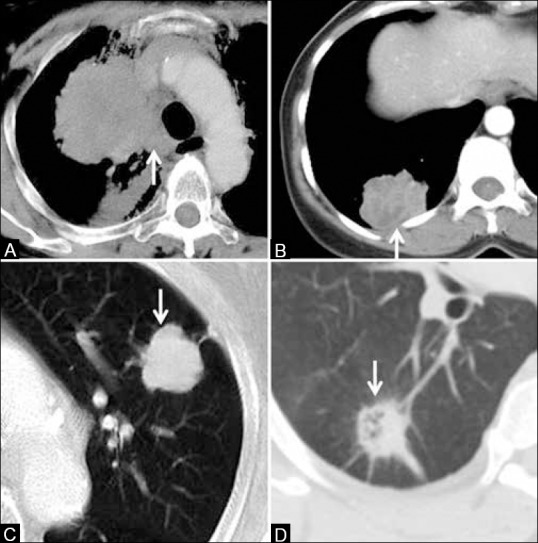
|[[Image:IJRI-25-109-g001.jpg|thumb|300px|Common radiological appearances of lung cancer. Centrally located mass with mediastinal invasion (arrow, A), peripherally situated mass abutting the pleura (arrow, B), mass with smooth, lobulated margins (arrow, C) and with spiculated, irregular margins (arrow, D), via <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F1/> | |[[Image:IJRI-25-109-g001.jpg|thumb|300px|Common radiological appearances of lung cancer. Centrally located mass with mediastinal invasion (arrow, A), peripherally situated mass abutting the pleura (arrow, B), mass with smooth, lobulated margins (arrow, C) and with spiculated, irregular margins (arrow, D), via <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F1/><ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
|[[Image:IJRI-25-109-g002.jpg|thumb|300px|Lung cancers with atypical radiological pattern. Squamous cell cancer presenting as a cavitating mass (arrow, A). Adenocarcinoma presenting as dense consolidation (arrow, B). Bronchoalveolar carcinoma (adenocarcinoma in situ) presenting as ground-glass opacity (arrow, C) and mixed density, solid (arrow), and ground-glass nodules (arrowhead) in D via <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F2/> | |[[Image:IJRI-25-109-g002.jpg|thumb|300px|Lung cancers with atypical radiological pattern. Squamous cell cancer presenting as a cavitating mass (arrow, A). Adenocarcinoma presenting as dense consolidation (arrow, B). Bronchoalveolar carcinoma (adenocarcinoma in situ) presenting as ground-glass opacity (arrow, C) and mixed density, solid (arrow), and ground-glass nodules (arrowhead) in D via <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F2/><ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
|- | |- | ||
|[[Image:IJRI-25-109-g003.jpg|thumb|300px|Stage T1 and T2 tumors. Stage T1 tumor due to size <3 cm (arrow, A). Stage T2 endobronchial tumor (arrowhead) causing pneumonitis restricted to the upper lobe (arrow) in B. T2a tumor >3 cm but <5 cm (arrow, C). T2b tumor >5 cm but <7 cm (arrow in D) via <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F3/> | |[[Image:IJRI-25-109-g003.jpg|thumb|300px|Stage T1 and T2 tumors. Stage T1 tumor due to size <3 cm (arrow, A). Stage T2 endobronchial tumor (arrowhead) causing pneumonitis restricted to the upper lobe (arrow) in B. T2a tumor >3 cm but <5 cm (arrow, C). T2b tumor >5 cm but <7 cm (arrow in D) via <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F3/><ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
|[[Image:IJRI-25-109-g004.jpg|thumb|300px|Stage T3 tumors. T3 tumor due to size >7 cm in size (arrow, A), eroding the ribs (arrow, B), infiltrating the mediastinal pleura but not the vessels (arrow, C), and causing atelectasis of the entire lung (arrowhead, D via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F4/> | |[[Image:IJRI-25-109-g004.jpg|thumb|300px|Stage T3 tumors. T3 tumor due to size >7 cm in size (arrow, A), eroding the ribs (arrow, B), infiltrating the mediastinal pleura but not the vessels (arrow, C), and causing atelectasis of the entire lung (arrowhead, D via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F4/>.<ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
|- | |- | ||
|[[Image:IJRI-25-109-g004.jpg|thumb|300px|Stage T4 tumors. T4 tumor due to invasion of pulmonary artery (arrow, A), descending aorta (arrow, B), vertebral body (arrow, C), superior vena cava with thrombus (arrow, D)via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F5/> | |[[Image:IJRI-25-109-g004.jpg|thumb|300px|Stage T4 tumors. T4 tumor due to invasion of pulmonary artery (arrow, A), descending aorta (arrow, B), vertebral body (arrow, C), superior vena cava with thrombus (arrow, D)via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F5/><ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
|[[Image:IJRI-25-109-g016.jpg|thumb|300px| | |[[Image:IJRI-25-109-g016.jpg|thumb|300px| | ||
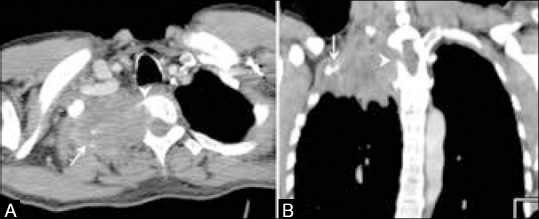
Superior sulcus tumor. Axial (A) and coronal (B) CT scans show a large mass in the apex of the right lung causing destruction of the first and second ribs (arrows) with erosion of the right half of the vertebral body (arrowheads) suggestive of a superior sulcus tumor, via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F16/> | Superior sulcus tumor. Axial (A) and coronal (B) CT scans show a large mass in the apex of the right lung causing destruction of the first and second ribs (arrows) with erosion of the right half of the vertebral body (arrowheads) suggestive of a superior sulcus tumor, via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F16/><ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
|} | |} | ||
== Spiral CT perfusion imaging == | == Spiral CT perfusion imaging == | ||
*Spiral CT perfusion imaging is analyzed for: | *Spiral CT perfusion study can be used as a diagnostic method for peripheral pulmonary nodules. | ||
*Spiral CT perfusion study provides non-invasive method of quantitative assessment about the blood flow patterns of peripheral pulmonary nodules. | |||
*Spiral CT perfusion imaging is analyzed and evaluated for:.<ref name="MaLe2008">{{cite journal|last1=Ma|first1=Shu-Hua|last2=Le|first2=Hong-Bo|last3=Jia|first3=Bao-hui|last4=Wang|first4=Zhao-Xin|last5=Xiao|first5=Zhuang-Wei|last6=Cheng|first6=Xiao-Ling|last7=Mei|first7=Wei|last8=Wu|first8=Min|last9=Hu|first9=Zhi-Guo|last10=Li|first10=Yu-Guang|title=Peripheral pulmonary nodules: Relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression|journal=BMC Cancer|volume=8|issue=1|year=2008|issn=1471-2407|doi=10.1186/1471-2407-8-186}}</ref>]] | |||
**TDC (time density curve) | **TDC (time density curve) | ||
**Perfusion parametric maps | |||
**The respective perfusion parameters. | |||
**Immunohistochemical findings of microvessel density (MVD) measurement | |||
**VEGF expression | |||
{| class="wikitable" | {| class="wikitable" | ||
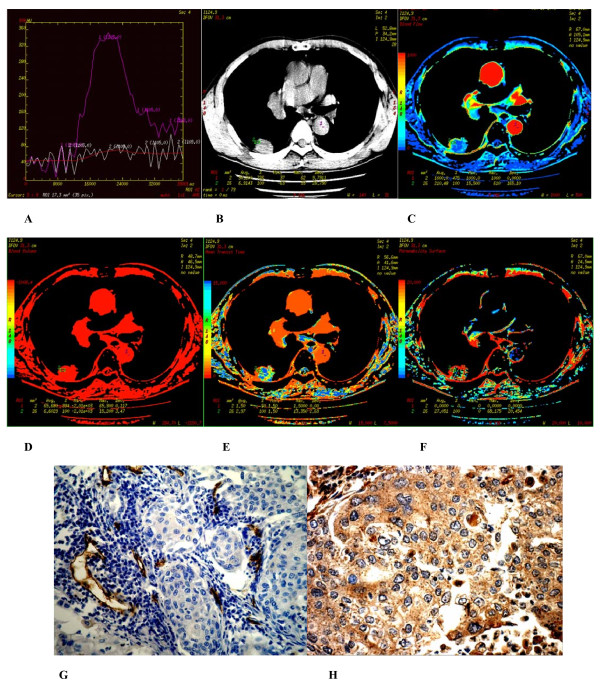
|[[Image:Peripheral pulmonary nodules1.jpg|300px|(A-H) Poorly differentiated adenocarcinoma found in the apicoposterior segment of superior lobe of the left lung of a 56 year-old male. (A) Time density curve. (B-F) (original image, BF, BV, MTT, PS) typeI parametric maps, PS value is higher (30.883). (G) CD34 staining shows many immature tumor microvessels (× 200). (H) VEGF expression is strong positive (× 400) via, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2474637/figure/F6/.<ref name="MaLe2008">{{cite journal|last1=Ma|first1=Shu-Hua|last2=Le|first2=Hong-Bo|last3=Jia|first3=Bao-hui|last4=Wang|first4=Zhao-Xin|last5=Xiao|first5=Zhuang-Wei|last6=Cheng|first6=Xiao-Ling|last7=Mei|first7=Wei|last8=Wu|first8=Min|last9=Hu|first9=Zhi-Guo|last10=Li|first10=Yu-Guang|title=Peripheral pulmonary nodules: Relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression|journal=BMC Cancer|volume=8|issue=1|year=2008|issn=1471-2407|doi=10.1186/1471-2407-8-186}}</ref>]] | |[[Image:Peripheral pulmonary nodules1.jpg|thumb|300px|(A-H) Poorly differentiated adenocarcinoma found in the apicoposterior segment of superior lobe of the left lung of a 56 year-old male. (A) Time density curve. (B-F) (original image, BF, BV, MTT, PS) typeI parametric maps, PS value is higher (30.883). (G) CD34 staining shows many immature tumor microvessels (× 200). (H) VEGF expression is strong positive (× 400) via, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2474637/figure/F6/.<ref name="MaLe2008">{{cite journal|last1=Ma|first1=Shu-Hua|last2=Le|first2=Hong-Bo|last3=Jia|first3=Bao-hui|last4=Wang|first4=Zhao-Xin|last5=Xiao|first5=Zhuang-Wei|last6=Cheng|first6=Xiao-Ling|last7=Mei|first7=Wei|last8=Wu|first8=Min|last9=Hu|first9=Zhi-Guo|last10=Li|first10=Yu-Guang|title=Peripheral pulmonary nodules: Relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression|journal=BMC Cancer|volume=8|issue=1|year=2008|issn=1471-2407|doi=10.1186/1471-2407-8-186}}</ref>]] | ||
||[[Image:Squamous_cell_Ca.jpg|thumb|300px|(A-H) (A-H) Well differentiated squamous cell carcinoma found in the posterior basal segment of inferior lobe of the right lung of a 61-year-old male. (A) Time density curve. (B-F) (original image, BF, BV, MTT, PS) TypeII parametric maps, PS value is higher (27.051). (G) CD34 staining shows many immature tumor microvessels (× 200). (H) VEGF expression is strong positive (× 400). via, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2474637/figure/F3/.<ref name="MaLe2008">{{cite journal|last1=Ma|first1=Shu-Hua|last2=Le|first2=Hong-Bo|last3=Jia|first3=Bao-hui|last4=Wang|first4=Zhao-Xin|last5=Xiao|first5=Zhuang-Wei|last6=Cheng|first6=Xiao-Ling|last7=Mei|first7=Wei|last8=Wu|first8=Min|last9=Hu|first9=Zhi-Guo|last10=Li|first10=Yu-Guang|title=Peripheral pulmonary nodules: Relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression|journal=BMC Cancer|volume=8|issue=1|year=2008|issn=1471-2407|doi=10.1186/1471-2407-8-186}}</ref>]] | |||
|} | |} | ||
== CT Findings of Metastatic disease == | == CT Findings of Metastatic disease == | ||
| Line 52: | Line 53: | ||
{| class="wikitable" | {| class="wikitable" | ||
|[[Image:IJRI-25-109-g010.jpg|thumb|300px|Metastatic disease. Bilateral pleural effusions-M1a (arrow, A), lung metastases-M1a (arrows, B), adrenal metastasis-M1b (arrow, C), vertebral metastasis-M1b (arrow, D), brain metastasis-M1b (arrow, E), liver metastases-M1b (arrows, F)via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F10/>This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.<ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | |[[Image:IJRI-25-109-g010.jpg|thumb|300px|Metastatic disease. Bilateral pleural effusions-M1a (arrow, A), lung metastases-M1a (arrows, B), adrenal metastasis-M1b (arrow, C), vertebral metastasis-M1b (arrow, D), brain metastasis-M1b (arrow, E), liver metastases-M1b (arrows, F)via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F10/>This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.<ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
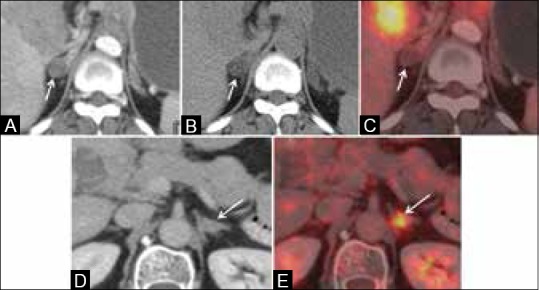
|[[Image:IJRI-25-109-g011.jpg|thumb|300px|Adrenal adenoma versus metastasis. Enhancing solid adrenal nodule on CT scan in a case of lung cancer (arrow, A) suggestive of metastatic deposit. Unenhanced CT scan shows fatty attenuation within the nodule with an HU value of 0 suggesting the possibility of an adenoma (arrow, B). FDG PET/CT shows no tracer concentration in the nodule, confirming the diagnosis of adenoma. Enhancing solid adrenal nodule on CT scan in another patient of lung cancer (arrow, D), which is indeterminate in nature. FDG PET/CT shows abnormal focal tracer concentration in the nodule (arrow, E) highly suggestive of a metastatic deposit via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F11/> | |[[Image:IJRI-25-109-g011.jpg|thumb|300px|Adrenal adenoma versus metastasis. Enhancing solid adrenal nodule on CT scan in a case of lung cancer (arrow, A) suggestive of metastatic deposit. Unenhanced CT scan shows fatty attenuation within the nodule with an HU value of 0 suggesting the possibility of an adenoma (arrow, B). FDG PET/CT shows no tracer concentration in the nodule, confirming the diagnosis of adenoma. Enhancing solid adrenal nodule on CT scan in another patient of lung cancer (arrow, D), which is indeterminate in nature. FDG PET/CT shows abnormal focal tracer concentration in the nodule (arrow, E) highly suggestive of a metastatic deposit via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F11/><ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
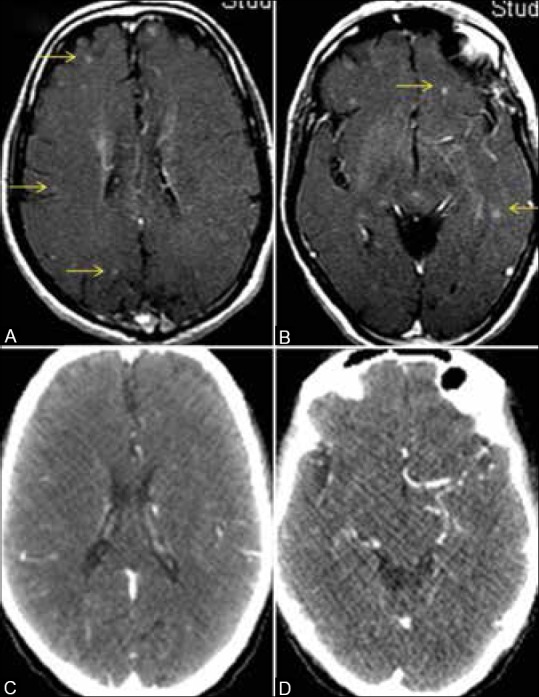
|[[Image:IJRI-25-109-g012.jpg|thumb|300px|Brain metastases in asymptomatic patient, CT scan versus MRI. MRI brain in a patient of lung cancer shows multiple tiny enhancing foci scattered in the parenchyma bilaterally (arrows in A and B) suggestive of metastatic lesions. Corresponding contrast CT scan sections of the brain show no obvious lesions (C and D). Note the beam hardening effects due to bone, leading to a loss of resolution on the CT images (C and D)|thumb|Brain metastases in asymptomatic patient, CT scan versus MRI. MRI brain in a patient of lung cancer shows multiple tiny enhancing foci scattered in the parenchyma bilaterally (arrows in A and B) suggestive of metastatic lesions. Corresponding contrast CT scan sections of the brain show no obvious lesions (C and D). Note the beam hardening effects due to bone, leading to a loss of resolution on the CT images (C and D)via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F12/> | |[[Image:IJRI-25-109-g012.jpg|thumb|300px|Brain metastases in asymptomatic patient, CT scan versus MRI. MRI brain in a patient of lung cancer shows multiple tiny enhancing foci scattered in the parenchyma bilaterally (arrows in A and B) suggestive of metastatic lesions. Corresponding contrast CT scan sections of the brain show no obvious lesions (C and D). Note the beam hardening effects due to bone, leading to a loss of resolution on the CT images (C and D)|thumb|Brain metastases in asymptomatic patient, CT scan versus MRI. MRI brain in a patient of lung cancer shows multiple tiny enhancing foci scattered in the parenchyma bilaterally (arrows in A and B) suggestive of metastatic lesions. Corresponding contrast CT scan sections of the brain show no obvious lesions (C and D). Note the beam hardening effects due to bone, leading to a loss of resolution on the CT images (C and D)via<https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4419420/figure/F12/><ref name="PurandareRangarajan2015">{{cite journal|last1=Purandare|first1=NilenduC|last2=Rangarajan|first2=Venkatesh|title=Imaging of lung cancer: Implications on staging and management|journal=Indian Journal of Radiology and Imaging|volume=25|issue=2|year=2015|pages=109|issn=0971-3026|doi=10.4103/0971-3026.155831}}</ref>]] | ||
|} | |} | ||
Latest revision as of 00:21, 17 February 2018
|
Lung cancer Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Lung cancer CT On the Web |
|
American Roentgen Ray Society Images of Lung cancer CT |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Dildar Hussain, MBBS [2]
Overview
Chest CT scan is the modality of choice in the diagnosis of lung cancer. Findings on CT scan suggestive of lung cancer include, a solitary pulmonary nodule, centrally located masses, mediastinal invasion CT scans help stage the lung cancer. A CT scan of the abdomen and brain can help visualize the common sights of metastases: adrenal glands, liver, and brain. CT scans diagnose lung cancer by providing anatomical detail to locate the tumor, demonstrating proximity to nearby structures, and deciphering whether lymph nodes are enlarged in the mediastinum.
CT Scan
Chest CT scan is the modality of choice in the diagnosis of lung cancer. Findings on CT scan suggestive of lung cancer include:[1]
- Solitary pulmonary nodule
- Centrally located masses
- Mediastinal invasion
- Peripherally situated lesions invading the chest wall
- A ground-glass opacity
- Consolidation
- Mixed density or pure ground glass nodules
- Mixed density or pure ground glass consolidation
 |
 |
 |
 |
 |
 |
Spiral CT perfusion imaging
- Spiral CT perfusion study can be used as a diagnostic method for peripheral pulmonary nodules.
- Spiral CT perfusion study provides non-invasive method of quantitative assessment about the blood flow patterns of peripheral pulmonary nodules.
- Spiral CT perfusion imaging is analyzed and evaluated for:.[2]]]
- TDC (time density curve)
- Perfusion parametric maps
- The respective perfusion parameters.
- Immunohistochemical findings of microvessel density (MVD) measurement
- VEGF expression
 |
 |
CT Findings of Metastatic disease
- CT scans help stage the lung cancer. A CT scan of the abdomen and brain can help visualize the common sights of metastases: adrenal glands, liver, and brain.
- The benefits of CT Scans in lung cancer patients are the following:[3]
- Provides anatomical detail to locate the tumor
- Demonstrates proximity to nearby structures
- Deciphers whether lymph nodes are enlarged in the mediastinum
 |
 |
 |
- Unfortunately, research has shown that there are a number of false positives associated with CT scanning because a CT scan on its own cannot determine malignancy.
- A positive result for a tumor using a CT scan is typically followed up with a biopsy for confirmation.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 Purandare, NilenduC; Rangarajan, Venkatesh (2015). "Imaging of lung cancer: Implications on staging and management". Indian Journal of Radiology and Imaging. 25 (2): 109. doi:10.4103/0971-3026.155831. ISSN 0971-3026.
- ↑ 2.0 2.1 2.2 Ma, Shu-Hua; Le, Hong-Bo; Jia, Bao-hui; Wang, Zhao-Xin; Xiao, Zhuang-Wei; Cheng, Xiao-Ling; Mei, Wei; Wu, Min; Hu, Zhi-Guo; Li, Yu-Guang (2008). "Peripheral pulmonary nodules: Relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression". BMC Cancer. 8 (1). doi:10.1186/1471-2407-8-186. ISSN 1471-2407.
- ↑ Gerard A. Silvestri, Lynn T. Tanoue, Mitchell L. Margolis, John Barker, Frank Detterbeck.11/30/11.The Noninvasive Staging of Non Small-cell Lung Cancer. Chestpubs. http://chestjournal.chestpubs.org/content/123/1_suppl/147S.full/