Pineal gland cyst
|
WikiDoc Resources for Pineal gland cyst |
|
Articles |
|---|
|
Most recent articles on Pineal gland cyst Most cited articles on Pineal gland cyst |
|
Media |
|
Powerpoint slides on Pineal gland cyst |
|
Evidence Based Medicine |
|
Cochrane Collaboration on Pineal gland cyst |
|
Clinical Trials |
|
Ongoing Trials on Pineal gland cyst at Clinical Trials.gov Trial results on Pineal gland cyst Clinical Trials on Pineal gland cyst at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Pineal gland cyst NICE Guidance on Pineal gland cyst
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Pineal gland cyst Discussion groups on Pineal gland cyst Patient Handouts on Pineal gland cyst Directions to Hospitals Treating Pineal gland cyst Risk calculators and risk factors for Pineal gland cyst
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Pineal gland cyst |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
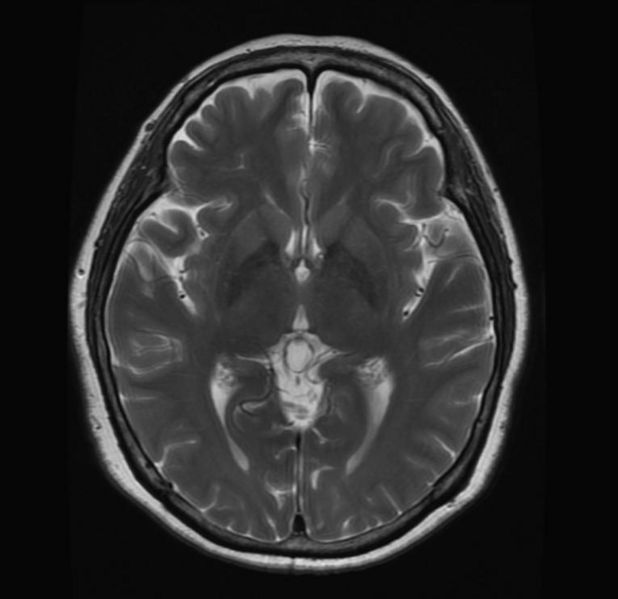
A pineal gland cyst is a cyst in the pineal gland, a small endocrine gland in the brain.. Statisically, these fluid-filled bodies appear on 1-4% of magnetic resonance imaging (MRI) brain scans. They are more frequent at death, seen in 21-41% of autopsies, though researchers are not sure why. They are in most cases asymptomatic, and it is rare for a pineal cyst to cause symptoms. If they do, these would most likely be headache, visual disturbances, or hydrocephalus, which can be extremely dangerous if left untreated. Pineal cysts are not cancer and most of the time they do not enlarge over 2 centimeters.
Asymptomatic cysts require no treatment. Some doctors choose to monitor patients with CT scans or MRI to look for cyst growth, but most doctors do not.
Differentiating Pineal gland cyst from Other Diseases
- Pineal cysts are most often mistaken for and may be indistinguishable from a benign pineocytoma. Pineocytomas are more likely to have solid components.
- Other cysts in the quadrigeminal cistern that mimic pineal cysts include arachnoid cysts and, rarely, epidermoids.
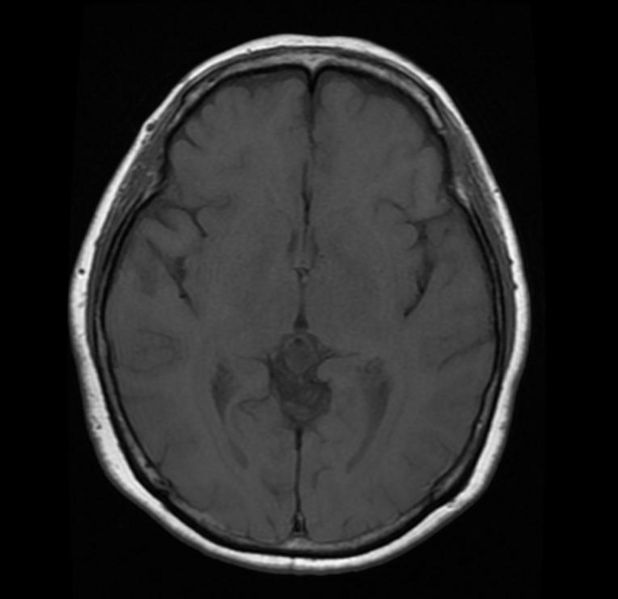
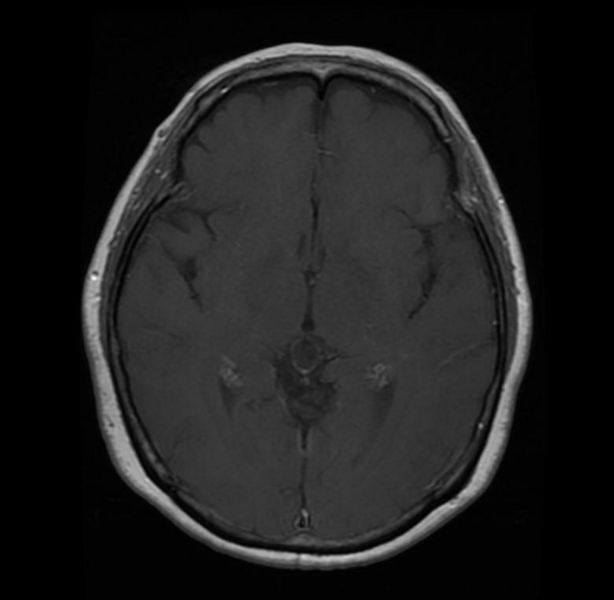
Diagnosis
- Attenuation or signal intensity varies with cyst content.
- One-fourth have rim or nodular calcium in the cyst wall on nonenhanced CT scans.
- Rim or nodular enhancement is also common.
- On T1-weighted MR images, 55%–60% are slightly hyperintense to CSF. Most do not appear hypointense on FLAIR images, and 60% enhance with use of contrast material.
Treatment
| Management Options of Penial Gland tumors | |
|---|---|
| CSF diversion |
|
| Surgical resection |
|
| Radiation |
|
| Stereotactic radiosurgery |
|
| Chemotherapy as part of multimodality therapy |
|