Oral ulcer
For patient information click here
|
WikiDoc Resources for Oral ulcer |
|
Articles |
|---|
|
Most recent articles on Oral ulcer |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Oral ulcer at Clinical Trials.gov Clinical Trials on Oral ulcer at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Oral ulcer
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Oral ulcer Discussion groups on Oral ulcer Patient Handouts on Oral ulcer Directions to Hospitals Treating Oral ulcer Risk calculators and risk factors for Oral ulcer
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Oral ulcer |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [3]; Associate Editor(s)-in-Chief: Shankar Kumar, M.B.B.S. [4]
Overview
An oral ulcer (from Latin ulcus) is the name for the appearance of an open sore inside the mouth caused by a break in the mucous membrane or the epithelium on the lips or surrounding the mouth. The types of oral ulcers are diverse, with a multitude of associated causes including: physical or chemical trauma, infection from microorganisms or viruses, medical conditions or medications, cancerous and sometimes nonspecific processes. Once formed, the ulcer may be maintained by inflammation and/or secondary infection. Two common oral ulcer types are aphthous ulcers (canker sores) and cold sores, which are caused by the herpes simplex virus.[1][2]
Causes
Common Causes
There are many processes which can lead to ulceration of the oral tissues. In some cases they are caused by an overreaction by the body's own immune system. Factors that appear to provoke them include stress, fatigue, illness, injury from accidental biting, hormonal changes, menstruation, sudden weight loss, food allergies and deficiencies in vitamin B12, iron and folic acid. Some drugs, such as nicorandil, have also been linked with oral ulcers. Some recreational drugs cause mouth ulcers. They may also be caused by eating too much sour food.
Trauma
Minor physical injuries
Trauma to the mouth is a common cause of oral ulcers. A sharp edge of a tooth, accidental biting (this can be particularly common with sharp canine teeth), sharp or abrasive food (particularly if left overnight), poorly fitting dentures, dental braces or trauma from a tooth brush may injure the mucosal lining of the mouth resulting in an ulcer. These ulcers usually heal at a moderate speed if the source of the injury is removed (for example, if poorly fitting dentures are removed or replaced).[1]
Chemical injuries
Chemicals such as Aspirin or alcohol that are held or that come in contact with the oral mucosa may cause tissues to become necrotic and slough off creating an ulcerated surface. Sodium Lauryl Sulfate (SLS), one of the main ingredients in most toothpastes, has been implicated in increased incidence of oral ulcers.
Infection
Viral, fungal and bacterial processes can lead to oral ulceration.[1]
Viral
The most common is Herpes simplex virus which causes recurrent herpetiform ulcerations preceded by usually painful multiple vesicles which burst. Herpes Zoster (shingles), Varicella Zoster (chicken pox), Coxsackie A virus and its associated subtype presentations, are some of the other viral processes that can lead to oral ulceration. HIV creates immunodeficiencies which allow opportunistic infections or neoplasms to proliferate.[2]
Bacterial
Bacterial processes leading to ulceration can be caused by Mycobacterium tuberculosis (tuberculosis) and Treponema pallidum (syphilis).[2]
Opportunistic activity by combinations of otherwise normal bacterial fauna, such as aerobic streptococci, Neisseria, Actinomyces, spirochetes, and Bacteroides species can prolong the ulcerative process.[3]
Fungal
Coccidioides immitis (valley fever), Cryptococcus neoformans (cryptococcosis), Blastomyces dermatitidis ("North American Blastomycosis") are some of the fungal processes causing oral ulceration.[2]
Immune system
Many researchers view the causes of aphthous ulcers as a common end product of many different disease processes, each of which is mediated by the immune system.[2]
Aphthous ulcers are thought to form when the body becomes aware of and attacks chemicals which it does not recognize. The presence of the unrecognized molecules garners a reaction by the lymphocytes, which trigger a reaction that causes the damage of an oral ulcer.
Immunodeficiency
Repeat episodes of mouth ulcers can be indicative of an immunodeficiency, signaling low levels of immunoglobulin in the oral mucous membranes. Chemotherapy and HIV are both causes of immunodeficiency with which oral ulcers become a common manifestation.
Autoimmunity
Autoimmunity is also a cause of oral ulceration. Mucous membrane pemphigoid, an autoimmune reaction to the epithelial basement membrane, causes desquamation/ulceration of the oral mucosa.
Allergy
Contact with allergens can lead to ulcerations of the mucosa.
Dietary
Vitamin C deficiencies may lead to scurvy which impairs wound healing, which can contribute to ulcer formation.[2] Similarly deficiencies in vitamin B12, iron, zinc[4] and folic acid have been linked to oral ulceration.
A common cause of ulcers is Coeliac disease, in which case consumption of wheat, rye, or barley can result in chronic oral ulcers. If gluten intolerance is the cause, prevention means taking most breads, pastas, cakes, pies, cookies, scones, biscuits, beers etc. out of the diet and substituting gluten-free varieties where available. Artificial sugars, such as those found in diet cola and sugarless gum, have been reported as causes of oral ulcers as well.
Cancer
Oral cancers can lead to ulceration as the center of the lesion loses blood supply and necroses. Squamous cell carcinoma is just one of these.
Causes Of Mouth Sores By Organ System
(By organ system)
Causes of Mouth Sores In Alphabetical Order
|
Diagnosis
Symptoms
The symptoms preceding the ulcer may vary according to the cause of the ulcerative process.
Some oral ulcers may begin with a sharp stinging or burning sensation at the site of the future mouth ulcer. In a few days, they often progress to form a red spot or bump, followed by an open ulcer. Sometimes this takes a little bit longer, depending on the cause of the ulcer.
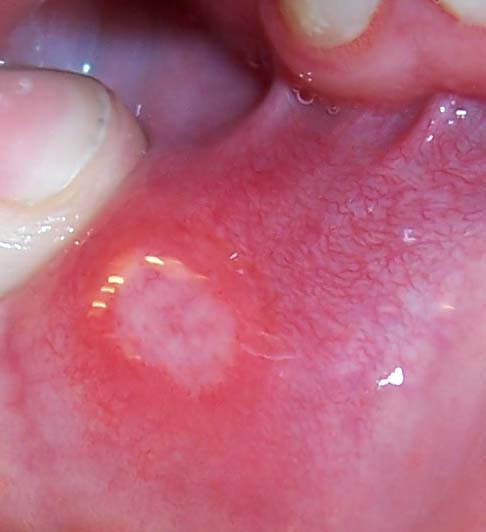
The oral ulcer appears as a white or yellow oval with an inflamed red border. Sometimes a white circle or halo around the lesion can be observed. The grey, white, or yellow coloured area within the red boundary is due to the formation of layers of fibrin, a protein involved in the clotting of blood. The ulcer, which itself is often extremely painful, especially when agitated, may be accompanied by a painful swelling of the lymph nodes below the jaw, which can be mistaken for toothache.
In some cases, the ulcer can cause other parts of the mouth to become slightly inflamed with patches of 'red bumps' which can feel rough to the tongue. It should be noted however, that any inflamed part of the mouth that remains there after 2 weeks should be seen by a doctor or dentist as soon as possible as this could be a warning sign of oral cancer.
Treatment
The majority of the types of ulceration require treatment of the underlying cause of the oral ulceration for successful prevention; controlling imbalances in vitamins and minerals related to ulceration, managing or restricting the disease processes has shown to reduce the ulcerative process. For trauma related cases, avoiding the offending source will prevent ulceration, but since such trauma is usually accidental, this type of prevention is not usually practical.
Individuals who have a high incidence of opportunistic bacterial infections subsequent to an accidental oral injury (biting etc.) can prevent the injury from becoming infected by directly bathing the wound with an anti-bacterial mouthwash for one minute every 12 hours for 2 days; it is important to use a small vessel to contain the solution as most antibacterial mouth washes that remain in the mouth for a full minute will have detrimental effects such as a prolonged impairement to the sense of taste and the potential loss of otherwise desirable flora. Quantities around 1ml are more than sufficient. Ideally, the first treatment should occur within 3 hours. A subsequent rinse in accordance with the manufacturers directions can only be of benefit.
See also
- Aphthous ulcer (Canker sores)
- Herpes simplex virus
- Squamous cell carcinoma
- Ulcer