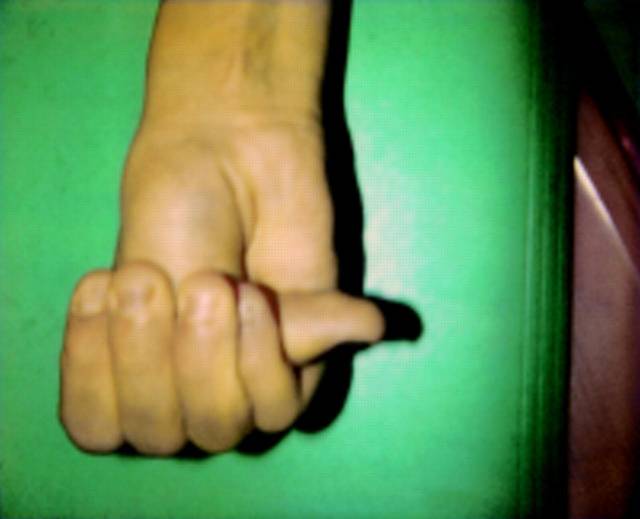
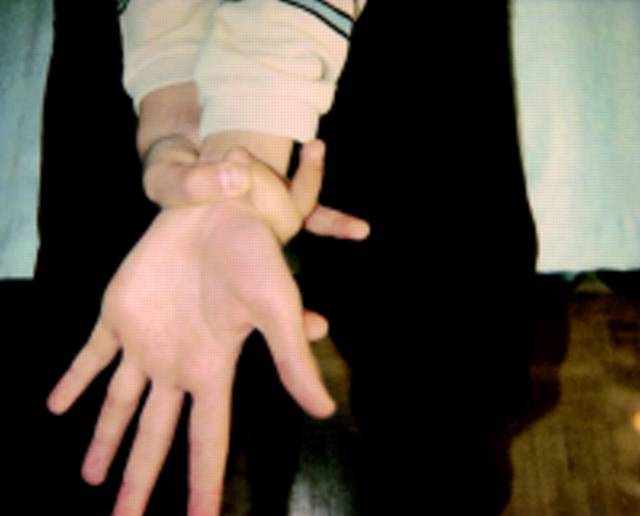
Marfan's syndrome diagnostic criteria
|
Marfan's syndrome Microchapters | |
|
Diagnosis | |
|---|---|
|
Treatment | |
|
Marfan's syndrome diagnostic criteria On the Web | |
|
American Roentgen Ray Society Images of Marfan's syndrome diagnostic criteria | |
|
Risk calculators and risk factors for Marfan's syndrome diagnostic criteria | |
Editors-In-Chief: William James Gibson, C. Michael Gibson, M.S., M.D.
Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [1] ; Assistant Editor-In-Chief: Cassandra Abueg, M.P.H. [2]
Overview
The major criteria for diagnosis of Marfan syndrome are ectopia lentis, aortic root dilation/dissection, dural ectasia, or a combination of more than 4 out of 8 major skeletal features. In an individual with no known family history of Marfan syndrome and in the absence of any known FBN1 mutations, major involvement of two organs systems (e.g. skeletal, cardiovascular, ocular) and minor involvement of a third system is required for diagnosis. However, if the patient has a known FBN1 mutation or affected relative, major involvement of only one system and minor involvement of another is sufficient for diagnosis.
Diagnostic Criteria
Several standards of diagnostic criteria for Marfan syndrome have been proposed. In 1986, the Berlin nosology was established which represented a consensus on clinical features diagnostic of Marfan syndrome with an emphasis on skeletal features [1]. Advances in molecular testing and the realization that many individuals diagnosed with Marfan syndrome according to the Berlin nosology did not have mutations in the FBN1 gene, led to the establishment of the Ghent nosology in 1996, a new set of criteria with stricter diagnostic requirements [2]. The Ghent nosology remains the current standard for diagnosis, although a revised version of the guidelines was published in 2010. The criteria are divided into major and minor manifestations which have allowed physicians to correctly diagnose 95% of patients as confirmed by molecular analysis of the FBN1 gene [3]. The new criteria establish aortic root aneurysm and ectopia lentis as the principal clinical features of the disease and stress cardiovascular manifestations.
The major criteria for diagnosis of Marfan syndrome are ectopia lentis, aortic root dilation/dissection, dural ectasia, or a combination of more than 4 out of 8 major skeletal features . In an individual with no known family history of Marfan syndrome and in the absence of any known FBN1 mutations, major involvement of two organs systems (e.g. skeletal, cardiovascular, ocular) and minor involvement of a third system is required for diagnosis. However, if the patient has a known FBN1 mutation or affected relative, major involvement of only one system and minor involvement of another is sufficient for diagnosis . Major manifestations of the cardiovascular system include ascending aortic dilation involving the sinuses of valsalva or dissection of the ascending aorta. Ectopia Lentis is the sole major criterion for involvement of the ocular system, and dural ectasia in the lumbosacral region diagnosed by CT or MRI is the criterion for major involvement of the dura. Having a known FBN1 mutation or a relative who independently satisfies criteria for diagnosis satisfies major involvement of family/genetic history. Physical examination for Marfan syndrome requires extensive evaluation of the skeletal system. Patients must fulfill four of the eight following criteria for major involvement of the skeletal system: pectus carinatum, pectus ex cavatum requiring surgery, reduced upper to lower segment ratio, wrist and thumb signs. Minor criteria for the various systems including pulmonary and skin/integument can be found in the supplement.
| Skeletal System | |
|---|---|
| Major Criterion. | Presence of at least 4 of the following manifestations.
• pectus carinatum • pectus ex cavatum requiring surgery • reduced upper to lower segment ratio or arm span to height ratio greater than 1.05 • wrist and thumb signs • scoliosis of > 20" or spondylolisthesis • reduced extension at the elbows (< 170") • medial displacement of the medial malleolus causing pes planus protmsio acetabulae of any degree (ascertained on radiographs) |
| Minor criteria. |
• pectus excavatum of moderate severity • joint hypermobility • highly arched palate with crowding of teeth • facial appearance (dolichocephaly, malar hypo- plasia,enophthalmos,retrognathia,down-Slanting palpebral fissures) |
| Ocular System | |
| Major criterion. | • Ectopia lentis |
| Minor criteria. |
• abnormally flat cornea (as measured by keratometry) • increased axial length of globe (as measured by ultrasound) • hypoplastic iris or hypoplastic ciliary muscle causing decreased miosis |
| Cardiovascular System | |
| Major criteria. |
• dilatation of the ascending aorta with or without aortic regurgitation and involving at least the sinuses of Valsalva; or • dissection of the ascending aorta |
| Minor criteria. |
• Mitral valve prolapsed • Mitral valve prolapsed with or without mitral valve regurgitation; • dilatation of the main pulmonary artery, in the absence of valvular or peripheral pulmonic stenosis or any other obvious cause, below the age of 40 years; • calcification of the mitral annulus below the age of 40 years; or dilatation or dissection of the descending thoracic or abdominal aorta below the age of 50 years |
| Pulmonary System | |
| Minor criteria. |
• spontaneous pneumothorax [Hall et al., 1984] • apical blebs (ascertained by chest radiography) |
| Skin and Integument | |
| Minor criteria. |
• striaeatrophicae (stretchmarks) not associated with marked weight changes, pregnancy or repetitive stress • recurrent or incisional herniae |
| Dura | |
| Major criterion. |
• Lumbosacral dural ectasia by CT or MRI |
| Family/Genetic History | |
| Major criteria. | • having a parent, child or sib who meets these diagnostic criteria independently;
• presence of a mutation in FBNl known to cause the Marfan syndrome; • presence of a haplotype around FBNl, inherited by descent, known to be associated with unequivocal- ly diagnosed Marfan syndrome in the family |
Adapted from De Paepe A, Devereux RB, Dietz HC, Hennekam RC, Pyeritz RE. Revised diagnostic criteria for the Marfan syndrome. Am J Med Genet 1996;62:417-26.
Images
References
- ↑ Beighton P, de Paepe A, Danks D, Finidori G, Gedde-Dahl T, Goodman R, Hall JG, Hollister DW, Horton W, McKusick VA (1988). "International Nosology of Heritable Disorders of Connective Tissue, Berlin, 1986". American Journal of Medical Genetics. 29 (3): 581–94. doi:10.1002/ajmg.1320290316. PMID 3287925. Unknown parameter
|month=ignored (help);|access-date=requires|url=(help) - ↑ De Paepe A, Devereux RB, Dietz HC, Hennekam RC, Pyeritz RE (1996). "Revised diagnostic criteria for the Marfan syndrome". American Journal of Medical Genetics. 62 (4): 417–26. doi:10.1002/(SICI)1096-8628(19960424)62:4<417::AID-AJMG15>3.0.CO;2-R. PMID 8723076. Unknown parameter
|month=ignored (help);|access-date=requires|url=(help) - ↑ Loeys BL, Dietz HC, Braverman AC, Callewaert BL, De Backer J, Devereux RB, Hilhorst-Hofstee Y, Jondeau G, Faivre L, Milewicz DM, Pyeritz RE, Sponseller PD, Wordsworth P, De Paepe AM (2010). "The revised Ghent nosology for the Marfan syndrome". Journal of Medical Genetics. 47 (7): 476–85. doi:10.1136/jmg.2009.072785. PMID 20591885. Retrieved 2010-12-22. Unknown parameter
|month=ignored (help) - ↑ Cocco G (2001). "Images in cardiology: The "thumb and wrist sign" in Marfan syndrome". Heart (British Cardiac Society). 86 (6): 602. PMC 1730018. PMID 11711445. Retrieved 2010-12-22. Unknown parameter
|month=ignored (help)