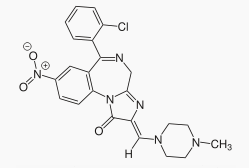
Loprazolam
 | |
 | |
| Clinical data | |
|---|---|
| Pregnancy category |
|
| Routes of administration | Oral |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | Hepatic |
| Elimination half-life | 6-12 hours |
| Excretion | Renal |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| DrugBank | |
| E number | {{#property:P628}} |
| ECHA InfoCard | {{#property:P2566}}Lua error in Module:EditAtWikidata at line 36: attempt to index field 'wikibase' (a nil value). |
| Chemical and physical data | |
| Formula | C23H21ClN6O3 |
| Molar mass | 464.904 g/mol |
|
WikiDoc Resources for Loprazolam |
|
Articles |
|---|
|
Most recent articles on Loprazolam |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Loprazolam at Clinical Trials.gov Clinical Trials on Loprazolam at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Loprazolam
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Loprazolam Discussion groups on Loprazolam Patient Handouts on Loprazolam Directions to Hospitals Treating Loprazolam Risk calculators and risk factors for Loprazolam
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Loprazolam |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
Loprazolam marketed under the band names Dormonoct®, Havlane®, Sonin®, Somnovit®, is a drug which is an imidazole benzodiazepine derivative. It possesses anxiolytic, anticonvulsant, sedative and skeletal muscle relaxant properties. It is available in 1mg tablets. It is licensed and marketed for the short term treatment of severe insomnia.
Indications
Insomnia. Insomnia can be described as a difficulty falling asleep, frequent awakening, early awakenings or a combination of each. Loprazolam is an intermediate acting benzodiazepine and is sometimes used in patients who have difficulty in maintaining sleep or have difficulty falling asleep. Hypnotics should only be used on a short term basis or in those with chronic insomnia on an occasional basis.[1]
Dose
The dose of Loprazolam for insomnia is usually 1 mg but can be increased to 2 mg if necessary. In the elderly a lower dose is recommended due to more pronounced effects and a significant impairment of standing up to 11 hours after dosing of 1 mg of loprazolam. The half life is much more prolonged in the elderly than in younger patients. A half life of 19.8 hours has been reported in elderly patients.[2] Patients and prescribing physicians should however bear in mind that higher doses of loprazolam may impair long term memory functions.[3]
Mechanism of Action
Loprazolam is a benzodiazepine, which acts via positively modulating the GABAa receptor complex via a binding to the benzodiazepine receptor which is situated on alpha subunit containing GABAa receptors. This action enhances the effect of the neurotransmitter GABA on the GABAa receptor complex by increasing the opening frequency of the chloride ion channel. This action allows more chloride ions to enter the neuron which in turn produces the following properties: muscle relaxation, anxiolytic, hypnotic, amnesic and anticonvulsant. These properties can be used for therapeutic benefit in clinical practise. These properties are also sometimes used for recreational purposes in the form of drug abuse of benzodiazepines where high doses are used to achieve intoxication and or sedation.[4] [5]
Pharmacokinetics
After oral administration of loprazolam on an empty stomach it takes 2 hours for serum concentration levels to reach their peak which is a significantly longer time than other benzodiazepine hypnotics. The delay in the time for peak plasma levels to reach their maximum brings into question the benefit of loprazolam for the treatment of insomnia when compared to other hypnotics, although studies have shown that the sleep inducing properties of loprazolam occur within 0.5 hours, which may indicate rapid penetration into the brain and thus the peak plasma delay of loprazolam may not be sigificantly relevant to loprazolams benefit as a hypnotic agent for the treatment of insomnia. If loprazolam is taken after a meal the time for plasma levels to reach their peak may be delayed even further. Loprazolam induces significant changes in the electrical activity of the brain as measured by an EEG, these changes are more pronounced, the higher the dosage. Metabolism of loprazolam in humans produces an active metabolite which is similar in potency to loprazolam, in levels of about half that of parent compound, the other half is excreted unchanged as loprazolam. The half life of the active metabolite is about the same as the parent compound loprazolam.[6]
Cognitive behavioural therapy
Chronic users of sedative hypnotic drugs who took part in a large scale clinical trial were found to have very high levels of insomnia and very low levels of sleep quality at trial intake. Those who received cognitive behavioural therapy and sleep hygiene, stimulus control, relaxation therapies had improved sleep quality, increased vitality, increased physical functioning and improved mental health. Reduced sedative hypnotic drug use also occurred in CBT treated patients with 33% at 6 month follow up reporting zero sedative hypnotic use. Clinical improvements were still apparent at 12 month follow-up. The patients age was not a barrier to successful outcome. It was concluded that psychological treatment can improve sleep quality, reduce hypnotic drug use and thus improve health related quality of life and is cost effective treatment for long term hypnotic users with chronic insomnia. CBT should be considered by healthcare providers and practitioners for insomnia management and to reduce benzodiazepine use in those with chronic insomnia.[7]
Side Effects
Side effects of loprazolam are generally the same as for other benzodiazepines such as diazepam Valium.[8] The only main difference in side effects of loprazolam and diazepam is it is less prone to day time sedation as the half life of loprazolam is considered to be intermediate whereas diazepam has a very long half life. The side effects of loprazolam are the following:
List of Side Effects
- drowsiness
- paradoxical increase in aggression
- lightheadedness
- confusion
- muscle weakness
- ataxia (particularly in the elderly)
- amnesia
- headache
- vertigo
- hypotension
- salivation changes
- gastro-intestinal disturbances
- visual disturbances
- dysarthria
- tremor
- changes in libido
- incontinence
- urinary retention
- blood disorders and jaundice
- skin reactions
- dependence and withdrawal reactions
Residual 'hangover' effects after nighttime administration of loprazolam such as sleepiness, impaired psychomotor and cognitive functions may persist into the next day which may impair the ability of users to drive safely and increase risks of falls and hip fractures.[9]
Tolerance, Dependence and Withdrawal
Loprazolam as with all other benzodiazepines is recommended for only short term management of insomnia in the UK due to the serious concerns of adverse affects of long term usage of benzodiazepines such as tolerance, dependency and withdrawal phenomenon as well as adverse effects on mood and cognition. Prolonged usage of benzodiazepines also is not recommended due to a lack of efficacy in there therapeutic actions due to tolerance to their effects and concerns of increasing physical and psychological adverse effects of some patients on long term benzodiazepines, eg agorophobia, gastrointestinal and peripheral nerve abnormalities such as burning and tingling sensations.[10][11]
Loprazolam however has a low risk of dependence (addiction) and withdrawal phenomenon if it is used for less than 4 weeks or very occasionally. However in one placebo controlled study comparing 3 week treatment for insomnia of either loprazolam or triazolam rebound anxiety and insomnia occurred 3 days after discontinuing loprazolam therapy whereas with triazolam the rebound anxiety and insomnia was seen the next day. The difference between the two benzodiazepines in time for rebound or withdrawal phenomenon to appear is likely due to the difference in the elimination half life of the two drugs.[12] [13] These results would suggest that loprazolam and possibly other benzodiazepines should be prescribed for 1 - 2 weeks rather than 2 - 4 weeks to reduce the risk of physical dependence or and withdrawal or rebound phenomenon.
Withdrawal Symptoms
It should be noted that slow reduction of the dosage over a period of months at a rate which the individual can tolerate greatly minimises the severity of the withdrawal symptoms. It is usually recommended for individuals dependent on benzodiazepines cross to an equivalent dose of diazepam to gradually taper as diazepam has a longer half life and small dose reductions can be achieved compared to other benzodiazepines. [14] [15]
- anxiety and panic attacks
- sweating
- nightmares
- insomnia
- headache
- tremor
- nausea and vomiting
- feelings of unreality
- abnormal sensation of movement
- hypersensitivity to stimuli
- hyperventilation
- flushing
- sweating
- palpitations
- dimensional distortions of rooms and television pictures
- paranoid thoughts and feelings of persecution
- depersonalisation
- fears of 'going mad
- heightened perception of taste, smell, sound, and light; photophobia
- agoraphobia
- clinical depression
- poor memory and concentration
- aggression
- excitability
- Somatic Symptoms
- numbness
- altered sensations of the skin
- pain
- stiffness
- weakness in the neck, head, jaw, and limbs
- muscle fasciculation ranging from twitches to jerks affecting the legs or shoulders
- ataxia
- paraesthesiae
- influenza-like symptoms
- blurred double vision
- menorrhagia
- loss of or dramatic gain in appetite
- thirst with polyuria
- urinary incontinence
- dysphagia
- abdominal pain
- diarrhoea
- constipation
Major complications can occur after abrupt or over rapid withdrawal especially from high doses producing symptoms such as:
- psychosis
- confusion
- visual and auditory hallucinations
- delusions
- epileptic seizures (which may be fatal)
It has been estimated that between 30% and 50% of long term users of benzodiazepines will experience withdrawal symptoms. [16] However up to 90% of patients withdrawing from benzodiazepines experienced withdrawal symptoms in one study, however the rate of taper was very fast at 25% of dose per week. [17] Withdrawal symptoms tend to last between 3 weeks to 3 months, although 10 - 15% of people may experience a protracted benzodiazepine withdrawal syndrome with symptoms persisting and gradually declining over a period of many months and occasional several years.[18]
References
- ↑ Rickels K. (1986). "The clinical use of hypnotics: indications for use and the need for a variety of hypnotics". Acta Psychiatr Scand Suppl. 332: 132–41. PMID 2883820.
- ↑ Swift CG, Swift MR, Ankier SI, Pidgen A, Robinson J. (1985). "Single dose pharmacokinetics and pharmacodynamics of oral loprazolam in the elderly". British journal of clinical pharmacology. Retrieved 2007-03-21.
- ↑ Bareggi SR, Ferini-Strambi L, Pirola R, Franceschi M, Smirne S. (1991). "Effects of loprazolam on cognitive functions". Psychopharmacology (Berl). Retrieved 2007-03-21.
- ↑ Bateson AN (2002). "Basic pharmacologic mechanisms involved in benzodiazepine tolerance and withdrawal". ingentaconnect. Retrieved 2007-03-21.
- ↑ Professor C Heather Ashton (2002). "BENZODIAZEPINE ABUSE". Harwood Academic. Retrieved 2007-03-22.
- ↑ Mamelak M, Bunting P, Galin H, Price V, Csima A, Young T, Klein D, Pelchat JR. (1988). "Serum and quantitative electroencephalographic pharmacokinetics of loprazolam in the elderly". Journal of clinical pharmacology. Retrieved 2007-03-21.
- ↑ Morgan K (2004). "Psychological treatment for insomnia in the regulation of long-term hypnotic drug use" (PDF). Health Technol Assess. National Health Service HTA Program. 8 (8): 1–4. PMID 14960254. Unknown parameter
|coauthors=ignored (help); Unknown parameter|month=ignored (help) - ↑ British National Formulary Benzodiazepines Information
- ↑ Vermeeren A. (2004). "Residual effects of hypnotics: epidemiology and clinical implications". CNS Drugs. 18 (5): 297–328. PMID 15089115.
- ↑ Committee on Safety of Medicines (1988). "BENZODIAZEPINES, DEPENDENCE AND WITHDRAWAL SYMPTOMS". Medicines Control Agency UK Government. Retrieved 2007-03-21.
- ↑ Professor C Heather Ashton (1987). "Benzodiazepine Withdrawal: Outcome in 50 Patients". benzo. Retrieved 2007-03-21.
- ↑ Morgan K, Oswald I (1982). "Anxiety caused by a short-life hypnotic". British medical journal (Clinical research ed.). Retrieved 2007-03-21.
- ↑ Morgan K, Adam K, Oswald I (1984). "Effect of loprazolam and of triazolam on psychological functions". Psychopharmacology. Retrieved 2007-03-21.
- ↑ McConnell JG (2007). "The Clinicopharmacotherapeutics of Benzodiazepine and Z drug dose Tapering Using Diazepam". BCNC. Retrieved 2007-06-09.
- ↑ (Roche Products (UK) Ltd 1990) Benzodiazepines and Your Patients: A Management Programme
- ↑ Schweizer E, Rickels K, Case WG, Greenblatt DJ. (1990). "Long-term therapeutic use of benzodiazepines. II. Effects of gradual taper". Arch Gen Psychiatry. Retrieved 2007-03-21.
- ↑ Ashton CH (2002). "BENZODIAZEPINES: How They Work and How to Withdraw". benzo org uk. Retrieved 2007-03-21.
External links
- Pages with script errors
- CS1 maint: Multiple names: authors list
- Pages with citations using unsupported parameters
- Drugs with non-standard legal status
- E number from Wikidata
- ECHA InfoCard ID from Wikidata
- Chemical articles with unknown parameter in Infobox drug
- Articles without EBI source
- Chemical pages without ChemSpiderID
- Articles without KEGG source
- Articles without InChI source
- Articles without UNII source
- Articles containing unverified chemical infoboxes
- Drug
- Anticonvulsants
- Anxiolytics
- Benzodiazepines
- Hypnotics
- Muscle relaxants
- Sedatives