Influenza primary prevention
|
Influenza Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Influenza primary prevention On the Web |
|
American Roentgen Ray Society Images of Influenza primary prevention |
|
Risk calculators and risk factors for Influenza primary prevention |
For more information about non-human (variant) influenza viruses that may be transmitted to humans, see Zoonotic influenza
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alejandro Lemor, M.D. [2]
Overview
Vaccination and chemoprophylaxis are the two most important methods for preventing influenza among patients. Routine annual influenza vaccination is recommended for all persons aged ≥6 months who do not have contraindications. Annual influenza vaccination is the best way to prevent influenza because vaccination can be given well before influenza virus exposures occur, and can provide safe and effective immunity throughout the influenza season. Chemoprophylaxis is not recommended in all patients and should only be administered for certain populations who are at risk of complications.
Vaccination
| ||||||||||
- Vaccination against influenza with a flu vaccine is strongly recommended for high-risk groups, such as children and the elderly.
- Health care providers should offer vaccination soon after vaccine becomes available (by October, if possible).
- Vaccination should be offered as long as influenza viruses are circulating.
- Children aged 6 months through 8 years who require 2 doses should receive their first dose as soon as possible after vaccine becomes available, and the second dose ≥4 weeks later.

Image courtesy of Public Health Image Library (PHIL)
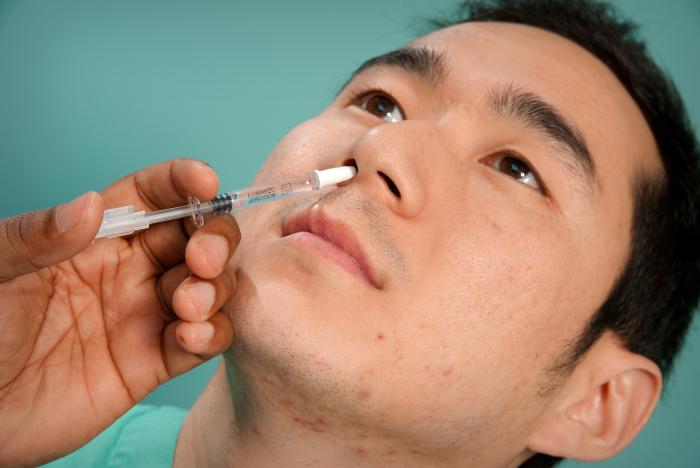
Image courtesy of Public Health Image Library (PHIL)
Influenza Vaccine Dosing Algorithm For Children Aged 6 Months Through 8 Years
Algorithm adapted from CDC Prevention and Control of Seasonal Influenza with Vaccines[2]
Did the child receive at least 1 dose of the 2013-14 vaccine? | |||||||||||||||||||||||||||||
| Yes | No or don't know | ||||||||||||||||||||||||||||
Administer 1 dose | Did the child receive a total of at least 2 doses of influenza vaccine since July 2010? | ||||||||||||||||||||||||||||
Yes | No or don't know | ||||||||||||||||||||||||||||
Administer 1 dose | Administer 2 doses | ||||||||||||||||||||||||||||
Duration of Immunity
- The composition of influenza vaccines is changed in most seasons, with one or more vaccine strains replaced annually to provide protection against viruses that are anticipated to circulate.
- Protection against viruses that are antigenically similar to those contained in the vaccine extends at least for 6–8 months, particularly in non-elderly populations.
- In some situations, duration of immunity might be longer, and such effects can be detected if circulating influenza virus strains remain antigenically similar for multiple seasons.
- Serum HAI influenza antibodies and nasal IgA elicited by vaccination remain detectable in children vaccinated with LAIV for >1 year after vaccination.
- Adults aged ≥65 years typically have diminished immune responses to influenza vaccination compared with healthy younger adults.
- Limited available data suggest that administration of additional vaccine doses during the same season does not increase the antibody response among elderly vaccines.
Chemoprophylaxis Adapted from CDC [3]
- Antiviral medications are approximately 70% to 90% effective in preventing influenza and are useful adjuncts to influenza vaccination.
- CDC does not recommend widespread or routine use of antiviral medications for chemoprophylaxis so as to limit the possibilities that antiviral resistant viruses could emerge.
- Indiscriminate use of chemoprophylaxis might promote resistance to antiviral medications, or reduce antiviral medication availability for treatment of persons at higher risk for influenza complications or those who are severely ill.
- In general, CDC does not recommend seasonal or pre-exposure antiviral chemoprophylaxis, but antiviral medications can be considered for chemoprophylaxis in certain situations.
- The following are examples of situations where antiviral medications can be considered for chemoprophylaxis to prevent influenza:
- Prevention of influenza in persons at high risk of influenza complications during the first two weeks following vaccination after exposure to an infectious person.
- Prevention for people with severe immune deficiencies or others who might not respond to influenza vaccination, such as persons receiving immunosuppressive medications, after exposure to an infectious person.
- Prevention for people at high risk for complications from influenza who cannot receive influenza vaccine due to a contraindication after exposure to an infectious person.
- Prevention of influenza among residents of institutions, such as long-term care facilities, during influenza outbreaks in the institution.
- An emphasis on close monitoring and early initiation of antiviral treatment if fever and/or respiratory symptoms develop is an alternative to chemoprophylaxis after a suspected exposure for some persons.
- To be effective as chemoprophylaxis, an antiviral medication must be taken each day for the duration of potential exposure to a person with influenza and continued for 7 days after the last known exposure. For persons taking antiviral chemoprophylaxis after inactivated influenza vaccination, the recommended duration is until immunity after vaccination develops (antibody development after vaccination takes about two weeks in adults and can take longer in children depending on age and vaccination history).
- Antiviral chemoprophylaxis generally is not recommended if more than 48 hours have elapsed since the first exposure to an infectious person.
- Patients receiving antiviral chemoprophylaxis should be encouraged to seek medical evaluation as soon as they develop a febrile respiratory illness that might indicate influenza.
Dosage and administration
If vaccine is administered for the first time in a 6 month to 8-year-old child, who has never got the flu vaccine before or vaccine history is unknown, it is given as 2 doses, 4 weeks apart. Two forms of flu vaccines are available- inactivated (injectable) vaccine (IIV) -dosage is 0.25cc administered as intramuscular vaccine for 6 to 35 month kid, for 36 months to 9 years kid dosage is 0.5 cc. The other form is live attenuated inactivated vaccine (LAIV) -given only for more than 2 years kid and within 50 years-dosage 0.2 cc sprayed as 0.1 cc in each nostril. Flu Vaccine is administered once every year for recommended population between October and April.
CDC Public Campaigns and Awareness
The following images are provided by the CDC to physicians to promote vaccination among high risk groups and healthcare workers.
Risk for travellers
Travellers are not a particular risk group for influenza, but in some countries appropriate health care may be unavailable or hard to access for non-residents in case of severe disease.
Vaccine
Influenza vaccines are either inactivated or live attenuated.
- Inactivated vaccines are used for children aged more than 6 months, pregnant women, persons with high-risk medical conditions and the elderly.
- Healthy non-pregnant individuals aged 2-49 years may alternatively receive live attenuated influenza vaccines.
prevailing influenza strains in the northern and southern hemispheres may differ significantly, the composition of the influenza vaccine is different for each hemisphere and is specified at different times in the year, just before the start of the influenza season in each.
Contraindications
Vaccination is contraindicated in case of severe egg allergy, including anaphylactic reaction.
References
- ↑ "Prevention and Control of Seasonal Influenza with Vaccines: Recommendations of the Advisory Committee on Immunization Practices (ACIP) — United States, 2014–15 Influenza Season".
- ↑ "Prevention and Control of Seasonal Influenza with Vaccines: Recommendations of the Advisory Committee on Immunization Practices (ACIP) — United States, 2014–15 Influenza Season".


