Frostbite
Template:DiseaseDisorder infobox
|
WikiDoc Resources for Frostbite |
|
Articles |
|---|
|
Most recent articles on Frostbite |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Frostbite at Clinical Trials.gov Clinical Trials on Frostbite at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Frostbite
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Frostbite Discussion groups on Frostbite Directions to Hospitals Treating Frostbite Risk calculators and risk factors for Frostbite
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Frostbite |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Jaspinder Kaur, MBBS[2]
Frostbite (congelatio in medical terminology) is a freezing, cold thermal injury, which occurs on being exposed to temperatures below the freezing point of typically −0.55°C to as high as 2°C for a sustained period of time. It is a condition characterized by the consequences in terms of functional morbidity among the panel of population that are often young, fit and healthy prior to sustaining thermal injury. Currently, the prevalence of frostbite is increasing within the civilian population, particularly among those who partake in winter sports such as skiing, hiking, mountain and ice climbing. The outdoor activities are more accessible so the individuals with limited experience or inadequate preparation and protection are highly prone to it. Additionally, vagrancy, homelessness, industrial injury and malfunctioning or misuse of equipment using NO or CO2 have also been causative factors. Cutaneous circulation plays an important role in thermoregulation by varying blood flow through peripheral structures to maintain core body temperature for survival. In a cold environment, maximal vasoconstriction is reached in hands and feet when their temperature drops to 15° C which is followed by local protective cycles of vasodilation on persistence of freezing temperature; but leads to progressive local ischemia if further exposure continues. However, thawing restores blood flow; but induces congestion, inflammation and thrombosis in the injured endothelium which may prompt erythrocyte extravasation due to distorted vessel wall. According to the depth of the skin damage, necrosis can be deeply severe which can results in spontaneous or surgical amputation. Frostbite can present with a wide spectrum of injury ranging from complete resolution without significant sequelae to major limb amputation and its functional consequences. Timely pre-hospital and definitive hospital management are important to minimize final tissue loss and maximize functionality of the affected limb. Once in the hospital setting, a multidisciplinary approach must be utilized to achieve the best outcomes. Either intravenous iloprost or thrombolysis with rTPA should be considered in all patients presenting within 24 h of sustaining an appropriately severe injury, and if the facility is capable of appropriate administration and monitoring. The treatment should be started with an immediate action to have a maximal output. Bone scanning is helpful to ascertain deep tissue injury and response to therapy. However, surgeons should avoid rushing to an early amputation; if case managed correctly in the earlier days, significant tissue can be salvaged for the final functional outcome. Prevention with education, behavior modification, following workplace guidelines, and appropriate use of modern equipment in most adventurous tourist destinations is important to reduce frostbite incidence. Once frostbite injury has occurred, little can be done to reverse the changes. Hence, a great preventive care should be taken to avoid its incidence.
- 5,000 years ago: An earliest evidence of frostbite was documented among pre-Columbian mummy discovered in the Andes.[1]
- 218 BC: Hannibal lost nearly half his army of 46,000 to frostbite injuries over a two week period of crossing the Southern Alps to reach Italy. [2]
- 1778: Dr. James Thatcher reported that Washington lost 10% of his army to cold-related tissue casualties during the winter times of the Revolutionary War. [2]
- 1812–1813: Baron Dominique Jean Larrey, Surgeon-in-Chief to Napoleon's Army, reported the first systematic medical observations of frostbite during the ill-fated invasion of Moscow during the fall season, and the subsequent retreat in a harsh Russian winter. He noted the deleterious effects of the freeze–thaw–refreeze cycle by identifing the debilitating effects of daily refreezing that occurred with bonfire thawing and subsequent marching in frigid conditions. He further stated that warming was beneficial; however, not by using the excessive heat of fires. Hence, he concluded the friction massage with snow or ice which results in slow rewarming is an optimal therapeutic standard of care for frostbite in military medicine and practiced for more than 100 years. [3]
- 1930:During World War II, both German and Russian troops moved to a philosophy of rapid rewarming based on work conducted at the Kirov Institute.[4] [5]
- 1941–1942: German troops sustained an estimated 250,000 frostbite injuries in the attempt to take over Moscow; and hence, constitutes the largest reported number of frostbite related injuries in history. Moreover, it was reported that the German army alone performed more than 15,000 amputations for cold related injuries on the Russian front during the winter season.[4]
- 1960: Mills published the first major clinical experience with rapid rewarming and included a concept of preventive care for frostbite with his report.[6]
- Frostbite has been divided into 4 tiers or degrees of injury based on acute physical findings and advanced imaging after rewarming following the classification scheme for thermal burn injury. However, these categories are difficult to use in the field and before rewarming as the still-frozen tissue is hard, pale, and anesthetic. Hence, an alternate 2-tiered classification has been proposed for the field use. [7]
Table 1: A two and four tiers classification scheme for Frostbite
| Two tier level of damage | Four tier level of damage | Clinical characteristics |
|---|---|---|
| Superficial damage | First degree |
|
| Superficial damage | Second degree |
|
| Deep damage | Third degree |
|
| Deep damage | Fourth degree |
|
Table 2: Classification scheme for the frostbite injuries of the extremity[8]
| Frostbite injuries of the extremity | Grade 1 | Grade 2 | Grade 3 | Grade 4 |
|---|---|---|---|---|
| Extent of initial lesion at day 0 after rewarming | Absence of initial lesion | Initial lesion on distal phalanx | Initial lesion on intermediary and proximal phalanx | Initial lesion on carpal or/and tarsal |
| Bone scanning at day 2 | Useless | Hypofixation of radiotracer uptake area | Absence of radiotracer uptake on the digit | Absence of radiotracer uptake area on the carpal or/and tarsal region |
| Blisters at day 2 | Absence of blisters | Clear blisters | Hemorrhagic blisters on the digit | Hemorrhagic blisters over carpal or/and tarsal region |
| Prognosis at day 2 | No amputation; No sequelae | Tissue amputation; Fingernail sequelae | Bone amputation of digit; Functional sequelae | Bone amputation of the limb; +/− systemic involvement; +/− sepsis functional sequelae |
- The rate of normal skin blood flow is about 250 ml/min, however; the flow drops to less than 20-50 ml/min during frostbite. As the temperature drops to below 0°C, the stasis of blood flow occurs especially in the slower venous system before the arterial system which subsequently leads to the cellular damage and results in reversible or irreversible injuries depending upon the extent of the exposure.
- Normal physiological responses to the cold environment:[9]
- Aim: To conserve the internal body core temperature and the viability of the extremities.
- Peripheral vasoconstriction: It is caused by sympathetic stimulation and catecholamine release which reduces the heat loss.
- Shivering: It is a muscular activity which maintain or augment the body heat; however, it cannot be sustained for more than a few hours because of the depletion of glycogen, which is the source of heat during shivering.
- Hunting reaction: It protects the extremities by the process of irregular 5 to 10-minute cycles of alternating vasoconstriction and vasodilation against excessive sustained peripheral vasoconstriction with minimal loss of internal body temperature.
- However, this mechanism fails when the body is exposed to freezing temperature of a magnitude or a duration that disrupt the internal body temperature maintenance because of the following reasons:
- Disruption of body core temperature is more deleterious than peripheral vasoconstriction;
- Conservation of core temperature takes precedence over rewarming of the extremities;
- The hunting response is replaced by continuous and more intense vasoconstriction resulting in frostbite via ice crystal formation, cellular dehydration, and microvasculature thrombosis.
- Four pathophysiological phases: Frostbite occurs through four interconnected progressive processes depending upon the rate and duration of freezing, rate of rewarming, and anatomic extent of exposure. [10]
- Prefreeze phase: The tissue cooling leads to local vasoconstriction and ischemia which results in the neuronal effects of hyperesthesia and paresthesia.[11]
- Freeze thaw phase: The cellular changes observed during freezing include extracellular ice formation, intracellular ice formation, cell dehydration and crenation, abnormal electrolyte concentrations due to altered oncotic pressures, and perturbations in lipid–protein complexes. However, the body initially responds to tissue freezing with alternating cycles of vasodilation and vasoconstriction (the “hunting reaction”) which lead to cycles of partial thawing and a prothrombotic microenvironment. Subsequently, rewarming melts ice crystals, promotes edema from injured endothelium, forms epidermal blisters and free radicals which continues the insult further. Additionally, an elaboration of inflammatory mediators, prostaglandins, and thromboxanes induces vasoconstriction and causes the vascular stasis period.[12]
- Vascular stasis phase: The persistence of the local vasoconstriction causes hypoxia and acidotic damage to the endothelium; and promotes coagulation and interstitial edema. Since, the vascular endothelium is highly susceptible; it may be completely obliterated and replaced by fibrin deposition 72 hours after the phase of freezing and thawing. The electron microscopic further shows an evidence of perivascular fluid extravasation and endothelial swelling and lysis.[11] [13]
- Ischemic phase: Finally, hypoxia, endothelial injury, and local thrombosis lead to the late ischemic phase, in which inflammatory mediators such as prostaglandins, thromboxanes, bradykinins, and histamine trigger additional vasoconstriction, platelet aggregation, and vessel thrombosis. As these inflammatory mediators peak during rewarming, the cycles of refreezing and rewarming can worsen the extent of tissue loss. Therefore, an initial frostbite treatment is targeted at restoring perfusion to the affected limb(s) and limiting tissue loss after rewarming.[11] [12] [13]
- Various types of cold injury can mimic each other which are categorized into hypothermia, tissue-freezing injury (frostbite), non–tissue-freezing injury (frostnip, trenchfoot, chilblain, or pernio) in the following Table.
Table 3: List of differential diagnosis for the Frostbite
| Differential disease | Clinical characteristics |
|---|---|
| Hypothermia [14] |
|
| Cutaneous burns [15] |
|
| Cold Urticaria [16] |
|
| Raynaud phenomenon [17] |
|
| Frostnip [18] |
|
| Chilblains (Pernio or Perniosis) [19] |
|
| Immersion foot (trench foot) [18] |
|
- Age: Although the elderly and young children are highly susceptible to the frostbite injury; however, the published epidemiological studies showed that frostbite is uncommon in these age groups and instead tends to affect adults between the ages of 30–49 years.[13]
- Anatomic location: The feet and the hands account for 90% of injuries reported. Other includes the face (nose, chin, earlobes, cheeks and lips), buttocks/perineum (from sitting on metal seats) and penis (joggers,runners and Nordic skiers). [13]
- A 12 year review on the inpatient frostbite injuries conducted in Saskatchewan, Canada revealed the incidence of predisposing factors in a decreasing order: Alcohol consumption (46%), psychiatric illness (17%), vehicular failure (19%), and drug misuse (4%). [20]
- Alcohol: It causes heat loss through peripheral vasodilatation and deranged judgement which may results in not seeking timely adequate shelter and consequently turns to a higher level of injury.[13]
- Various behavioural, physiological and mechanical factors play an important roles in increasing the likelihood of its development and the extent of the damage.
Table 4: Factors that increases risk for frostbite[10] [13][20]
| Behavioural factors | Physiological factors | Mechanical factors |
|---|---|---|
|
|
|
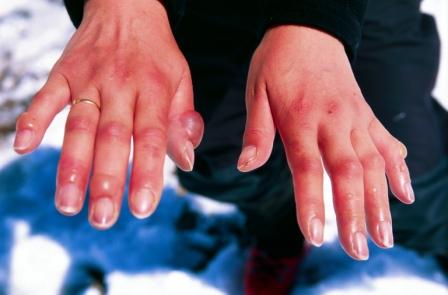
- Most common: Complex regional pain syndrome and arthritis
- Late or chronic sequelae (70%): Infection, increased cold sensitivity, hyperhydrosis, numbness, skin pigmentation, abnormalities of the nails, joint stiffness, and premature closure of physeal growth plate in children.[9]
- Skin areas affected by frostbite are susceptible to chronic ulceration due to poor tissue quality after healing; and can undergo a malignant transformation akin to the formation of Marjolin's ulcers similar to old burn scars.[21]
- Frostbite Arthropathy: In the growing child, frostbite produces a characteristic growth stunting of the small bones through premature closure of physeal growth plate and acro-osteolysis. Additionally, secondary osteoarthritic changes may be seen in early adulthood.[22]
- Favourable prognostic factors: Retained sensation, normal skin colour, and clear rather than cloudy fluid in the blisters, early edema formation and clear blisters extending to the tips of the digits are considered favourable sign.
- Poor prognostic factors: Non-blanching cyanosis, firm skin, lack of edema, and small, proximal, dark haemorrhagic vesicles indicates damage to the subdermal vascular plexus.[23]
- However, no prognostic features are entirely predictive; and weeks or months may pass before the demarcation between viable and non-viable tissue becomes visible.[10]
- Hence, patients should avoid cold exposure for up to a year after the initial injury.
Clinical Symptoms
- Severity of symptoms is directly proportional to the severity of injury.
- Initial presenting complaint: A cold numbness associated with a sensory loss, the extremities are cold to the touch, and patients complains of clumsiness, ‘‘like a block of wood’’. Thawing and reperfusion are often accompanied by intense pain. [13]
- At 2-3 days: A throbbing pain begins after rewarming and may persist for weeks or months even after the tissue becomes demarcated.
- At a week: A residual tingling sensation appears probably due to an ischemic neuritis. However, a variable presentation can be seen with no painful sensation especially among diabetics with previous neuropathic damage. [24]
- Symptoms usually subside within 1 month in mild cases of no tissue loss; contrarily, in cases with severe tissue loss, disablement may exceed 6 months. Usually frostbite victims experience some degree of sensory loss for at least 4 years or indefinitely post injury.
- Aggravating factor: Symptoms gets exacerbated by a warm environment.
- Other sensory deficits: Spontaneous burning and electric current-like sensations in the affected body areas.[25]
Clinical Signs
- Frostbite is a clinical diagnosis.
- However, initial injuries appear similar and make it difficult to determine the severity or grade of injury until post rewarming.
- The extent of the freezing and tissue loss may not be apparent for 4 to 5 days.
- Frostbite injuries can be classified clinically as either superficial or deep.[26]
- Superficial injuries: It may appear as either a numb central white plaque with surrounding erythema, or as blisters filled with clear or milky fluid with surrounding erythema and edema.
- Deep injuries: It is characterized by either hemorrhagic blisters that develop into a black eschar in 2 weeks or have a complete tissue loss and necrosis. Final tissue demarcation may take 3 to 4 weeks to establish. The appearance of the skin, sensation to pinprick, and whether the vesicles are clear or hemorrhagic should be noted. Identify signs of dehydration, hypothermia, altitude effects (pulmonary edema), and exhaustion.
- Rewarming injuries: During rewarming, edema may start to appear within 3-5 hours and may last 7 days. Blisters tend to appear within 4-24 hours. Presence of eschar will be obvious at 10-15 days and mummification with a line of demarcation may develop in 3-8 weeks. [27]
Diagnostic modality
- The primary role of imaging in frostbite injuries is to define the precisely the severity, depth, and extent of tissue injury to better direct nonsurgical and surgical treatment. Additionally, imaging plays an important role in monitoring response to the provided treatment.
Table 5: Elaborates the different imaging modality used for Frostbite[28]
| Diagnostic test | Characteristics |
|---|---|
| Radiographs [29] |
|
| Digital subtraction angiography (DSA) [30] |
|
| Multiphase bone scintigraphy [31] |
|
| SPECT/CT [32] |
|
- Other miscellaneous tests: Infrared thermography, laser doppler studies, digital plethysmography and magnetic resonance imaging/ magnetic resonance angiography. [10]
- Almost all patients should be admitted to hospital; considering alcohol intoxication, psychiatric illness, and homelessness as the common features of the frostbite patient; an immediate discharge is rarely prudent. Hence, treatment of frostbite can be divided into three phases: prethaw field care phase, immediate hospital care phase, and postthaw phase.

Field Treatment
- If a body part found frozen in the field area, it should be protected from further damage with the following measures:[33]
- The patient should be immediately moved out of the wind, provided with shelter and given warm fluids.
- Remove boots but the problems of replacement can arise if swelling occurs, and replace wet gloves and socks with dry ones. Warm the cold extremity by placing them in a companion's armpit or groin for 10 min and then replace the boots/gloves. Rubbing the affected part is not recommended because of the potential for worsening direct tissue injury.
- If sensation returns, the patient may mitigate the further risks and continue to walk. If there is no return of sensation, the injured should go to the nearest warm shelter (hut or base camp) and seek medical treatment. If at high altitude (>4,000 m), supplementary oxygen should be considered. [10]
- Aspirin 75 mg can be given for its rheologic effect. Ibuprofen 12 mg/kg/day divided into two daily doses (maximum of 2,400 mg/day) should be given for its prostaglandin effect.
- Field rewarming should only be attempted if there is no further risk of refreezing as the cycle of thawing and refreezing results in a more extensive injury.[34] [35]
- The decision to thaw the frostbitten tissue in the field may involve pain control, maintaining warm water baths at a constant temperature, protecting tissue from further injury during rewarming, and eventual transport.
- In extreme scenarios, it may be better to let a casualty walk on a frozen limb to safety rather than risk refreezing.[36]
Immediate hospital care
- The standard approach to the initial treatment of frostbite is the strategy originally outlined by McCauley and Heggers as mentioned below: [36]
- Admit frostbite patient to specialist unit if possible
- Evaluate for hypothermia, concomitant injury, or complicating problems
- On admission, rapidly rewarm the affected areas in warm water at 37–39°C (99–102°F) for 15–30 mins or until thawing is complete
- Debride clear or white blisters and apply topical aloe vera (Dermaide aloe) every 6 h
- Leave haemorrhagic blisters intact and apply topical aloe vera every 6 h
- Splint and elevate the extremity
- Administer antitetanus prophylaxis (toxoid or immunoglobulin (Ig))
- Analgesia: opiate (intravenously or intramuscularly) as indicated
- Administer ibuprofen 400 mg orally every 12 h
- Administer benzyl penicillin 500 000 U every 6 h for 48–72 h
- Administer daily hydrotherapy in 40°C water for 30–45 mins. Do not towel dry affected tissue.
- Prohibit smoking

Fluids[34]
- Rehydration can be provided orally or intravenously depending upon severity and ability of the patient to accept the warm fluids.
- Oral fluids should be given if the patient is alert and has no gastrointestinal symptoms.
- In case of nausea, vomiting, or an altered mental status; IV normal saline should be given if available.
- High altitude increases the risk of dehydration. A hypothermia in combination to dehydration may be compounded by cold diuresis due to suppression of antidiuretic hormone which mandates the replenishment with intravenous fluids.
- Intravenous fluids should be warmed before infusion if possible; and should be infused in small boluses as slower infusion will result in fluid cooling as it passes through the IV tubing.
- Volume status should be optimized as per the signs of clinical dehydration.
Rewarming
- Hypothermia and concomitant injury should be thoroughly evaluated.
- Systemic hypothermia should be corrected to a core temperature of 34°C before frostbite management is initiated.
- Rewarming should be carried out in a whirlpool of recirculating water with a mild antibacterial solutions (povidone-iodine or chlorhexidine).
- The State of Alaska Cold-injury Guidelines recommend a lower temperature water bath of 37–39°C which decreases the patient pain with slightly slowing the rewarming process. [35]
- The time period recommended for rewarming varies from 15–30 mins up to 1 h.[36]
- Rewarming should continue until a red/purple color appears and the extremity becomes pliable. [34]
- Active motion during the rewarming period is beneficial but care should be taken to prevent the extremity from touching the sides of the whirlpool.
- It is important to provide good analgesic cover by including narcotic medication. [33]
Blisters and dressings[10]
- Blisters containing clear or milky fluid should be debrided and covered every 6 h with aloe vera ointment, a potent anti-prostaglandin agent.
- Splinting, elevating, and wrapping the affected part in a loose and protective dressing should follow the administration of the aloe vera cream.
- Padding should be put between the patient’s toes if affected.
- Haemorrhagic blisters should be left intact to prevent desiccation of the underlying tissue. If they restrict movement, they can be drained with their roofs left on.
Antibiotics
- Frostbite is not an inherently infection-prone injury. Therefore, the use of antibiotics specifically for preventing infection during or after frostbite injury is still controversial.
- However, when associated with significant edema or malnutrition due to homelessness, chronic alcohol abuse or return from extreme altitude; penicillin is administered as edema deranges the skin bactericidal properties.[12]
- Additionally, systemic antibiotics are administered in the presence of proven infection, trauma or cellulitis. [13]
Tetanus toxoid
- Tetanus prophylaxis should be done as per the standard guidelines.
Analgesia and NSAIDs
- Rewarming the extremities can be extremely painful process, so use of NSAID drugs or opiates should be administered.
- Oral ibuprofen 12 mg/kg divided over two daily doses provides systemic anti-prostaglandin activity that limits the cascade of inflammatory damage. This dose can be increased to a maximum of 2,400 mg/day if the patient is still experiencing pain, and can be continued until wounds are healed or amputation occurs. A dose of 400 mg BID is a practical regime to start with the most patients, but it can be increased later on to 600 mg QDS as pain dictates. [37]
- If aspirin has not been given in the field, 300 mg once a day can be given provided no contraindications. However, aspirin is less useful as it prolongs blockade of all prostaglandin synthesis and some prostacyclins that are considered beneficial for wound healing. [37]
- The role of clopidogrel in frostbite has yet to be assessed.
Definitive treatment
Angiography and thrombolysis
- rTPA delivery should be provided at a centre accustomed to performing thrombolysis and providing adequate monitoring in a critical care/high-dependency setting.
- If the patient presents less than 24 h after injury to a hospital without these facilities, consider urgent transfer to avoid further delay in the commencement of therapy.
- An initial selective diagnostic DSA should be performed in patients being considered for thrombolysis.
- Intravenous vasodilators such as nitroglycerin or papaverine are useful in conjunction with rTPA to treat the vasospasm associated with a frostbite injury.[38] [39]
- rTPA is used in combination with heparin which reduces the recurrence of microvascular thrombosis. [39]
- Repeat angiograms should be performed every 12–24 h to evaluate response to therapy.
- rTPA treatment should be discontinued when perfusion is restored to distal vessels or at 48 h if no improvement is observed.[40]
Table 6: Enumuerates the protocol for intravenous rTPA[41]
| Administration |
|
| Ideally given with a portable syringe pump |
|
| Indications |
|
| Contraindications |
|
| Precautions |
|
| Complications and their management |
|
| Route of administration |
|
Vasodilators: Iloprost
- Iloprost is a prostacyclin analogue with vasodilatory properties that mimic the effects of a sympathectomy. Additionally, it may affect platelet aggregation and hence, decrease microvascular occlusion.
Table 7: Protocol of intravenous prostacyclin[41]
| Administration and monitoring |
|
| Complications and their management |
|
| Contraindications |
|
| Precautions |
|
| Advantage over rTPA |
|
Surgery
Fasciotomies
- Early surgical intervention in the form of fasciotomy in the immediate post-thaw phase is required if compartment syndrome compromises the reperfusion. [42]
Amputation
- Angiography, technetium-99 bone scan and/or magnetic resonance imaging may be used to assist determination of surgical margins in conjunction with clinical findings.
- An early amputation is indicated occasionally if liquefaction, moist gangrene, or overwhelming infection and sepsis develops.
- Otherwise, amputation should be delayed until definitive demarcation occurs which takes around 6–12 weeks. [43]
- Negative pressure devices can aid in speeding up healing of amputation sites by secondary intention.[44]
- The healed affected limb is often insensate. Hence, an approach that addresses both protective footwear and orthotics to provide optimal limb function is essential. [43]
Tissue protection
- The functional use of extremities following a partial amputation is variable and injury specific.
- The biomechanics of the foot/hand can be radically altered and frostbite neuropathy can compound the problem; hence, liaison with orthotic/podiatry department to provide custom-made footwear may be required to optimize the long-term limb functional result and minimize secondary injuries. [45]
Adjuvant therapies
Hyperbaric oxygen therapy (HBOT)
- Benefits of HBOT in frostbite are as follows:[46]
- It reverses vasoconstriction in ischemic tissue and the resulting hyperoxia from oxygen dissolved in plasma surpasses any potential blood flow reduction.
- It increases a diffusion distance and improves oxygenation in hypoxic tissue.
- Angiogenesis is also promoted by HBOT which further reduces edema and necrosis in hypoxic skeletal muscle by improving the blood supply.
- It increases the deformability of erythrocytes, has a bacteriostatic effect and may act as an antioxidant.
- It delineates the viable tissue from necrotic part and allows marginal tissue to be maintained until revascularization has been established.
- However, HBOT showed mixed results with no level 1 evidence available. Hence, its role warrants further investigation as it is a relatively safe and inexpensive treatment. [33]
Sympathectomy
- The role of sympathectomy, either surgical (via open or minimally invasive) or chemical, has yielded mixed results.
- Early sympathectomy, performed within the first few hours of injury, has led to increase in edema formation and tissue destruction.[47]
- However, if performed 24–48 h after thawing, it is considered to hasten resolution of edema and decrease tissue loss.
- Sympathectomy may prevent some long term sequelae such as pain due to vasospasm, paresthesias and hyperhidrosis.
- However, since the advent of alternative therapies such as rTPA and Iloprost, and being irreversible nature of sympathectomy procedure, a great caution should be exercised while considering its use; and hence, some consider no role for its use in frostbite. [10]
Telemedicine
- A recent development in accessing expert advice by the use of the internet and satellite phones has been driven both by the patients and the clinicians with a limited experience of frostbite. A virtual opinion can be sought from any remote or difficult situations in the world. [48]
- The UK based service can be accessed via the Diploma in Mountain Medicine or the British Mountaineering Council websites which is run by Diploma Faculty Members and is being increasingly used by climbers and physicians worldwide, often to obtain a second opinion or to seek more specialized advice. [49]
- Patients can be readily followed up in a ‘‘virtual clinic’’ by reviewing recent digital images and discussing management options either by phone or via email.
- As in many instances, it can be prevented so the key is deterrence and patient education.
- Risk modification including proper clothing, access to shelter, and maintaining hydration and nutrition are vital for protection against frostbite.
- Patients should be advised to carry extra clothing supplies if they are into winter sports and avoid tight restrictive clothing.
- Emollients, although traditionally believed in Nordic countries to prevent frostbite, do not have protective effects in preventing frostbite and should be discouraged.[50]
- Advise against the abuse of alcohol, illicit drugs, and tobacco.
- For those with medical conditions, it is important to ensure that their health is stable before venturing on an adventurous outdoor trip during winter.
- Prolonged exposure to freezing cold temperatures may cause serious health problems so if signs related to it are observed, call for emergency help.
- The Occupational Safety and Health Act (OSHA) Cold Stress Card provides a reference guide and recommendations to combat and prevent many illnesses and injuries. Available in English and Spanish, this laminated fold-up card is free to employers, workers and the public. [51]
- Tips include how to protect workers:
- Recognize the environmental and workplace conditions that may be dangerous.
- Learn the signs and symptoms of cold-induced illnesses and injuries and what to do to help workers.
- Train workers about cold-induced illnesses and injuries.
- Encourage workers to wear proper clothing for cold, wet and windy conditions, including layers that can be adjusted to changing conditions.
- Be sure workers in extreme conditions take a frequent short break in warm dry shelters to allow their bodies to warm up.
- Try to schedule work for the warmest part of the day.
- Avoid exhaustion or fatigue because energy is needed to keep muscles warm.
- Use the buddy-system, work in pairs so that one worker can recognize danger signs.
- Drink warm, sweet beverages (sugar water, sports-type drinks) and avoid drinks with caffeine (coffee, tea, sodas or hot chocolate) or alcohol.
- Eat warm, high-calorie foods such as hot pasta dishes.
- Remember, workers are at an increased risks who takes certain medications, are in poor physical condition or suffer from illnesses such as diabetes, hypertension or cardiovascular disease.
References
- ↑ Post PW, Donner DD: Frostbite in a pre-Columbian mummy. Am J Phys Anthropol 1972, 37(2):187–191.
- ↑ 2.0 2.1 Cochran, Amalia; Morris, Stephen E. (2018). "Cold-Induced Injury": 403–407.e2. doi:10.1016/B978-0-323-47661-4.00038-1.
- ↑ Larrey DJ. Memoirs of Military Surgery. Vol.2. Baltimore, MD: Joseph Cushing; 1814
- ↑ 4.0 4.1 Killian H. Cold Injury With Special Reference to the German Experience During World War II. Aulendorf i Württ, Germany: Editio Cantor KG; 1952.
- ↑ Ariev TJ. Monograph on Frostbite. Steiman I, trans. Narkomzdrav, USSR: State Health Committee. Translation published by Defense Research Board, Canada; 1955: 1–169
- ↑ Mills WJ, Whaley R, Fish W. Frostbite, I: Experience with rapid rewarming and ultrasonic therapy. Alaska Med. 1960;2(1):1–4. Reprinted in Alaska Med. 1993;35(1):5–9.
- ↑ Cauchy E, Chetaille E, Marchand V, Marsigny B. Retrospective study of 70 cases of severe frostbite lesions: a proposed new classification scheme. Wilderness Environ Med. 2001;12:248 –255.
- ↑ Cauchy E, Marsigny B, Allamel G, Verhellen R, Chetaille E: The value of technetium 99 scintigraphy in the prognosis of amputation in severe frostbite injuries of the extremities: a retrospective study of 92 severe frostbite injuries. J Hand Surg 2000, 25(5):969–978.
- ↑ 9.0 9.1 Olin, Jeffrey W. (2012). "Other Peripheral Arterial Diseases": 493–499. doi:10.1016/B978-1-4377-1604-7.00080-4.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 Imray, C; Grieve, A; Dhillon, S (2009). "Cold damage to the extremities: frostbite and non-freezing cold injuries". Postgraduate Medical Journal. 85 (1007): 481–488. doi:10.1136/pgmj.2008.068635. ISSN 0032-5473.
- ↑ 11.0 11.1 11.2 McIntosh SE, Opacic M, Freer L, et al. Wilderness Medical Society practice guidelines for the prevention and treatment of frostbite: 2014 update. Wilderness Environ Med 2014;25(4 suppl):S43–S54.
- ↑ 12.0 12.1 12.2 Murphy JV, Banwell PE, Roberts AH, McGrouther DA. Frostbite: pathogenesis and treatment. J Trauma 2000;48(1):171–178.
- ↑ 13.0 13.1 13.2 13.3 13.4 13.5 13.6 13.7 Reamy BV. Frostbite: review and current concepts. J Am Board Fam Pract 1998;11(1):34–40.
- ↑ Gelb, D. (2014). "Hypothermia": 657–658. doi:10.1016/B978-0-12-385157-4.00059-2.
- ↑ Foley, F.D. (1970). "Pathology of Cutaneous Burns". Surgical Clinics of North America. 50 (6): 1201–1210. doi:10.1016/S0039-6109(16)39280-5. ISSN 0039-6109.
- ↑ Pizzorno, Joseph E.; Murray, Michael T.; Joiner-Bey, Herb (2016). "Urticaria": 923–935. doi:10.1016/B978-0-7020-5514-0.00085-3.
- ↑ Britton, Carmelita V. (2007). "Raynaud's Disease": 478. doi:10.1016/B978-032303506-4.10274-3.
- ↑ 18.0 18.1 Ingram, Benjamin J.; Raymond, Tyler J. (2013). "Recognition and Treatment of Freezing and Nonfreezing Cold Injuries". Current Sports Medicine Reports. 12 (2): 125–130. doi:10.1249/JSR.0b013e3182877454. ISSN 1537-890X.
- ↑ Vano-Galvan, S.; Martorell, A. (2011). "Chilblains". Canadian Medical Association Journal. 184 (1): 67–67. doi:10.1503/cmaj.110100. ISSN 0820-3946.
- ↑ 20.0 20.1 Valnicek SM, Chasmar LR, Clapson JB. Frostbite in the prairies: a 12-year review. Plast Reconstr Surg 1993;92:633–41.
- ↑ Rossis CG, Yiacoumettis AM, Elemenoglou J: Squamous cell carcinoma of the heel developing at site of previous frostbite. J R Soc Med 1982, 75(9):715–718.
- ↑ Carrera GF, Kozin F, Flaherty L, McCarty DJ: Radiographic changes in the hands following childhood frostbite injury. Skeletal Radiol 1981, 6(1):33–37.
- ↑ Pollard AJ, Murdoch DR. The high altitude medicine handbook. Abingdon: Radcliffe Medical Press, 2003.
- ↑ Oakley EHN. In: Tooke JE, Lowe GD, eds. A textbook of vascular medicine. Arnold UK, 1996.
- ↑ West JB, Schoene RB, Milledge JS. High altitude medicine and physiology. Hodder Arnold, 2007.
- ↑ Wathen, Joe; Emery, Kathryn D. (2011). "Thermal injury (frostbite/burns)": 462–467. doi:10.1016/B978-0-323-05405-8.00115-7.
- ↑ Basit H, Wallen TJ, Dudley C. Frostbite. [Updated 2020 Jun 30]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK536914/
- ↑ Millet, John D.; Brown, Richard K. J.; Levi, Benjamin; Kraft, Casey T.; Jacobson, Jon A.; Gross, Milton D.; Wong, Ka Kit (2016). "Frostbite: Spectrum of Imaging Findings and Guidelines for Management". RadioGraphics. 36 (7): 2154–2169. doi:10.1148/rg.2016160045. ISSN 0271-5333.
- ↑ Vinson HA, Schatzki R. Roentgenologic bone changes encountered in frostbite, Korea 1950–51. Radiology 1954;63(5): 685–695.
- ↑ Gonzaga, Teresa; Jenabzadeh, Kamrun; Anderson, Christopher P.; Mohr, William J.; Endorf, Frederick W.; Ahrenholz, David H. (2016). "Use of Intra-arterial Thrombolytic Therapy for Acute Treatment of Frostbite in 62 Patients with Review of Thrombolytic Therapy in Frostbite". Journal of Burn Care & Research. 37 (4): e323–e334. doi:10.1097/BCR.0000000000000245. ISSN 1559-047X.
- ↑ Cauchy E, Chetaille E, Lefevre M, Kerelou E, Marsigny B. The role of bone scanning in severe frostbite of the extremities: a retrospective study of 88 cases. Eur J Nucl Med 2000;27(5): 497–502.
- ↑ Kraft CT, Millet JD, Agarwal S, et al. SPECT/CT in the evaluation of frostbite. J Burn Care Res doi:10.1097/ BCR.0000000000000359.
- ↑ 33.0 33.1 33.2 Handford, Charles; Buxton, Pauline; Russell, Katie; Imray, Caitlin EA; McIntosh, Scott E; Freer, Luanne; Cochran, Amalia; Imray, Christopher HE (2014). "Frostbite: a practical approach to hospital management". Extreme Physiology & Medicine. 3 (1): 7. doi:10.1186/2046-7648-3-7. ISSN 2046-7648.
- ↑ 34.0 34.1 34.2 McIntosh, Scott E.; Hamonko, Matthew; Freer, Luanne; Grissom, Colin K.; Auerbach, Paul S.; Rodway, George W.; Cochran, Amalia; Giesbrecht, Gordon; McDevitt, Marion; Imray, Christopher H.; Johnson, Eric; Dow, Jennifer; Hackett, Peter H. (2011). "Wilderness Medical Society Practice Guidelines for the Prevention and Treatment of Frostbite". Wilderness & Environmental Medicine. 22 (2): 156–166. doi:10.1016/j.wem.2011.03.003. ISSN 1080-6032.
- ↑ 35.0 35.1 Murkowski FH, Mandsager R, Choromanski Hull-Jilly D. State of Alaska Cold Injuries Guidelines. Juneau: Department of Health and Social Services of Alaska; 2003. pp. 36–41. Revised 01/2005.
- ↑ 36.0 36.1 36.2 McCauley RL, Hing DN, Robson MC, Heggers JP (1983). "Frostbite injuries: a rational approach based on the pathophysiology". J Trauma. 23 (2): 143–7. PMID 6827634.
- ↑ 37.0 37.1 Hallam MJ, Cubison T, Dheansa B, Imray C (2010). "Managing frostbite". BMJ. 341: c5864. doi:10.1136/bmj.c5864. PMID 21097571.
- ↑ Saemi, Arash M.; Johnson, Jason M.; Morris, Christopher S. (2009). "Treatment of Bilateral Hand Frostbite Using Transcatheter Arterial Thrombolysis After Papaverine Infusion". CardioVascular and Interventional Radiology. 32 (6): 1280–1283. doi:10.1007/s00270-009-9584-9. ISSN 0174-1551.
- ↑ 39.0 39.1 Sheridan, Robert L.; Cabot, Richard C.; Harris, Nancy Lee; Shepard, Jo-Anne O.; Rosenberg, Eric S.; Cort, Alice M.; Ebeling, Sally H.; Peters, Christine C.; Goldstein, Mark A.; Stoddard, Frederick J.; Walker, T. Gregory (2009). "Case 41-2009". New England Journal of Medicine. 361 (27): 2654–2662. doi:10.1056/NEJMcpc0910088. ISSN 0028-4793.
- ↑ Bruen, Kevin J. (2007). "Reduction of the Incidence of Amputation in Frostbite Injury With Thrombolytic Therapy". Archives of Surgery. 142 (6): 546. doi:10.1001/archsurg.142.6.546. ISSN 0004-0010.
- ↑ 41.0 41.1 Cauchy, Emmanuel; Davis, Christopher B.; Pasquier, Mathieu; Meyer, Eric F.; Hackett, Peter H. (2016). "A New Proposal for Management of Severe Frostbite in the Austere Environment". Wilderness & Environmental Medicine. 27 (1): 92–99. doi:10.1016/j.wem.2015.11.014. ISSN 1080-6032.
- ↑ Mills WJ (1993). "Frostbite. A discussion of the problem and a review of the Alaskan experience. 1973". Alaska Med. 35 (1): 29–40. PMID 8214378.
- ↑ 43.0 43.1 Jurkovich GJ. Environmental cold-induced injury. Surg Clin North Am. 2007;87:247–267.
- ↑ Poulakidas, Stathis; Cologne, Kyle; Kowal-Vern, Areta (2008). "Treatment of Frostbite With Subatmospheric Pressure Therapy". Journal of Burn Care & Research. 29 (6): 1012–1014. doi:10.1097/BCR.0b013e31818ba0ad. ISSN 1559-047X.
- ↑ Khaira, H.S.; Coddington, T.; Drew, A.; Roberts, P.N.; Imray, C.H.E. (1998). "Patellar tendon bearing orthosis — Application as adjunctive treatment in healing of lower-limb tissue loss". European Journal of Vascular and Endovascular Surgery. 16 (6): 485–488. doi:10.1016/S1078-5884(98)80238-4. ISSN 1078-5884.
- ↑ von Heimburg, Dennis; Noah, E.Magnus; Sieckmann, Ullrich P.F; Pallua, Norbert (2001). "Hyperbaric oxygen treatment in deep frostbite of both hands in a boy". Burns. 27 (4): 404–408. doi:10.1016/S0305-4179(00)00132-7. ISSN 0305-4179.
- ↑ Taylor MS (1999). "Lumbar epidural sympathectomy for frostbite injuries of the feet". Mil Med. 164 (8): 566–7. PMID 10459266.
- ↑ Imray CHE, Hillebrandt D. Telemedicine and frostbite injuries. BMJ 2004;328:1210.
- ↑ "How to get expert frostbite advice".
- ↑ Lehmuskallio E. Cold protecting ointments and frostbite. Acta Derm Venereol (Stockh) 1999;79:67–70.
- ↑ "Tips To Protect Workers In Cold Environments".
Related Chapters
Template:Consequences of external causes cs:Omrzliny de:Erfrierung eo:Frostiĝo he:כוויית קור it:Congelamento lt:Nušalimas nl:Bevriezing (medisch) fi:Paleltuma sv:Köldskada