Cryptococcosis epidemiology and demographics
|
Cryptococcosis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Cryptococcosis epidemiology and demographics On the Web |
|
American Roentgen Ray Society Images of Cryptococcosis epidemiology and demographics |
|
Risk calculators and risk factors for Cryptococcosis epidemiology and demographics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Serge Korjian M.D., Yazan Daaboul, M.D.
Overview
The prevalence of cryptococcal antigenemia among patients with HIV in the United States is approximately 2.9%. The overall incidence is estimated to be 0.4 to 1.3 cases per 100,000 persons yearly in the United States. Cryptococcosis has no age, gender, or racial predilections.[1]
Epidemiology and Demographics
Prevalence
- The prevalence of cryptococcal antigenemia in the general population is unknown. Given the low incidence in the general population, it is thought to be very low.
- Among HIV patients in the United States, the prevalence of cryptococcal antigenemia is approximately 2.9%, indicating that the prevalence of cryptococcal infection may be high enough to consider targeted screening for HIV patients.[1]
Incidence
- Nationally, representative estimates for the incidence of cryptococcosis are difficult to establish because cryptococcosis is only reportable in a few states.
- Results from active, population-based surveillance in two US locations in the year 2000 indicated that the annual incidence of cryptococcosis among persons with AIDS was between 2 and 7 cases per 1,000.
- The overall incidence is estimated to be 0.4 to 1.3 cases per 100,000 persons yearly in the United States.[2]
- C. neoformans is a major cause of illness in people living with HIV/AIDS, with an estimated 1 million cases of cryptococcal meningitis occurring worldwide each year.[1][3]
Age, Gender, and Race
Cryptococcosis has no age, gender, or racial predilection.[1]

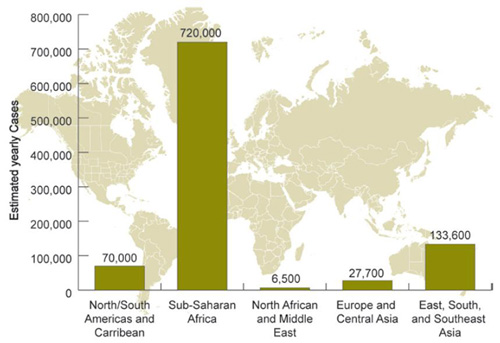
Developed vs. developing countries
The geographical distribution of endemic fungi causing meningitis are shown below:[4]
| Fungus | Demography |
|---|---|
| Blastomyces dermatiditis | Midwest and Southeast of USA, lower Mississippi valley up to the North Central states, and into the Mid-Atlantic states. |
| Coccidiodes immitis | Mostly in dry, slightly acidic soil, making it common in southwest of USA, parts of Mexico, and Central and South America. |
| Histoplasma capsulatum: | Ohio, central Mississippi River Valley, and Appalachian Mountains. |
| Cryptococcus spp. | Cryptococcus neoformans is distributed worldwide with the following specifics:
|
| Paracoccidioides brasiliensi | Subtropical areas of Central and South America. |
| Hyalohyphomycoses | There are numerous molds in this group, including Aspergillus, Scedosporium, and Fusarium species. It has a worldwide distribution. |
| Candida species | Worldwide distribution |
| Sporothrix schenckii | Worldwide distribution |
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 C. neoformans Infection Statistics. Centers for Disease Control and Prevention (2015). http://www.cdc.gov/fungal/diseases/cryptococcosis-neoformans/statistics.html Accessed on December 31, 2015
- ↑ Mirza SA, Phelan M, Rimland D, Graviss E, Hamill R, Brandt ME; et al. (2003). "The changing epidemiology of cryptococcosis: an update from population-based active surveillance in 2 large metropolitan areas, 1992-2000". Clin Infect Dis. 36 (6): 789–94. doi:10.1086/368091. PMID 12627365.
- ↑ Park BJ, Wannemuehler KA, Marston BJ, Govender N, Pappas PG, Chiller TM (2009). "Estimation of the current global burden of cryptococcal meningitis among persons living with HIV/AIDS". AIDS. 23 (4): 525–30. doi:10.1097/QAD.0b013e328322ffac. PMID 19182676.
- ↑ Koroshetz WJ. Chapter 382. Chronic and Recurrent Meningitis. In: Longo DL, Fauci AS, Kasper DL, Hauser SL, Jameson JL, Loscalzo J, eds. Harrison's Principles of Internal Medicine. 18th ed. New York: McGraw-Hill; 2012.