Suvorexant
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Turky Alkathery, M.D. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Suvorexant is an orexin receptor antagonist that is FDA approved for the treatment of insomnia, characterized by difficulties with sleep onset and/or sleep maintenance. Common adverse reactions include with BELSOMRA was somnolence.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Indications
- BELSOMRA® (suvorexant) is indicated for the treatment of insomnia characterized by difficulties with sleep onset and/or sleep maintenance.
Dosage
Dosing Information
- Use the lowest dose effective for the patient.
- The recommended dose for BELSOMRA is 10 mg, taken no more than once per night and within 30 minutes of going to bed, with at least 7 hours remaining before the planned time of awakening. If the 10 mg dose is well-tolerated but not effective, the dose can be increased. The maximum recommended dose of BELSOMRA is 20 mg once daily.
Special Populations
- Exposure to BELSOMRA is increased in obese compared to non-obese patients, and in women compared to men. Particularly in obese women, the increased risk of exposure-related adverse effects should be considered before increasing the dose.
Use with CNS Depressants
- When BELSOMRA is combined with other CNS depressant drugs, dosage adjustment of BELSOMRA and/or the other drug(s) may be necessary because of potentially additive effects.
Use with CYP3A Inhibitors
- The recommended dose of BELSOMRA is 5 mg when used with moderate CYP3A inhibitors and the dose generally should not exceed 10 mg in these patients. BELSOMRA is not recommended for use with strong CYP3A inhibitors.
Food Effect
- Time to effect of BELSOMRA may be delayed if taken with or soon after a meal.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
- There is limited information regarding Off-Label Guideline-Supported Use of Suvorexant in adult patients.
Non–Guideline-Supported Use
- There is limited information regarding Off-Label Non–Guideline-Supported Use of Suvorexant in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
- Safety and effectiveness in pediatric patients have not been established.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Suvorexant in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Suvorexant in pediatric patients.
Contraindications
- BELSOMRA is contraindicated in patients with narcolepsy.
Warnings
CNS Depressant Effects and Daytime Impairment
- BELSOMRA is a central nervous system (CNS) depressant that can impair daytime wakefulness even when used as prescribed. Prescribers should monitor for somnolence and CNS depressant effects, but impairment can occur in the absence of symptoms, and may not be reliably detected by ordinary clinical exam (i.e., less than formal testing of daytime wakefulness and/or psychomotor performance). CNS depressant effects may persist in some patients for up to several days after discontinuing BELSOMRA.
- BELSOMRA can impair driving skills and may increase the risk of falling asleep while driving. Discontinue or decrease the dose in patients who drive if daytime somnolence develops. In a study of healthy adults, driving ability was impaired in some individuals taking 20 mg BELSOMRA. Although pharmacodynamic tolerance or adaptation to some adverse depressant effects of BELSOMRA may develop with daily use, patients using the 20 mg dose of BELSOMRA should be cautioned against next-day driving and other activities requiring full mental alertness. Patients taking lower doses of BELSOMRA should also be cautioned about the potential for driving impairment because there is individual variation in sensitivity to BELSOMRA.
- Co-administration with other CNS depressants (e.g., benzodiazepines, opioids, tricyclic antidepressants, alcohol) increases the risk of CNS depression. Patients should be advised not to consume alcohol in combination with BELSOMRA because of additive effects. Dosage adjustments of BELSOMRA and of concomitant CNS depressants may be necessary when administered together because of potentially additive effects. The use of BELSOMRA with other drugs to treat insomnia is not recommended.
- The risk of next-day impairment, including impaired driving, is increased if BELSOMRA is taken with less than a full night of sleep remaining, if a higher than the recommended dose is taken, if co-administered with other CNS depressants, or if co-administered with other drugs that increase blood levels of BELSOMRA. Patients should be cautioned against driving and other activities requiring complete mental alertness if BELSOMRA is taken in these circumstances.
Need to Evaluate for Co-morbid Diagnoses
- Because sleep disturbances may be the presenting manifestation of a physical and/or psychiatric disorder, treatment of insomnia should be initiated only after careful evaluation of the patient. The failure of insomnia to remit after 7 to 10 days of treatment may indicate the presence of a primary psychiatric and/or medical illness that should be evaluated. Worsening of insomnia or the emergence of new cognitive or behavioral abnormalities may be the result of an unrecognized underlying psychiatric or physical disorder, and can emerge during the course of treatment with hypnotic drugs such as BELSOMRA.
Abnormal Thinking and Behavioral Changes
- A variety of cognitive and behavioral changes (e.g., amnesia, anxiety, hallucinations and other neuro-psychiatric symptoms) have been reported to occur in association with the use of hypnotics such as BELSOMRA. Complex behaviors such as "sleep-driving" (i.e., driving while not fully awake after taking a hypnotic) and other complex behaviors (e.g., preparing and eating food, making phone calls, or having sex), with amnesia for the event, have been reported in association with the use of hypnotics. These events can occur in hypnotic-naïve as well as in hypnotic-experienced persons. The use of alcohol and other CNS depressants may increase the risk of such behaviors. Discontinuation of BELSOMRA should be strongly considered for patients who report any complex sleep behavior.
Worsening of Depression/Suicidal Ideation
- In clinical studies, a dose-dependent increase in suicidal ideation was observed in patients taking BELSOMRA as assessed by questionnaire. Immediately evaluate patients with suicidal ideation or any new behavioral sign or symptom.
- In primarily depressed patients treated with sedative-hypnotics, worsening of depression, and suicidal thoughts and actions (including completed suicides) have been reported. Suicidal tendencies may be present in such patients and protective measures may be required. Intentional overdose is more common in this group of patients; therefore, the lowest number of tablets that is feasible should be prescribed for the patient at any one time.
- The emergence of any new behavioral sign or symptom of concern requires careful and immediate evaluation.
Patients with Compromised Respiratory Function
- Effect of BELSOMRA on respiratory function should be considered if prescribed to patients with compromised respiratory function. BELSOMRA has not been studied in patients with severe obstructive sleep apnea (OSA) or severe chronic obstructive pulmonary disease (COPD).
Sleep Paralysis, Hypnagogic/Hypnopompic Hallucinations, Cataplexy-like Symptoms
- Sleep paralysis, an inability to move or speak for up to several minutes during sleep-wake transitions, and hypnagogic/hypnopompic hallucinations, including vivid and disturbing perceptions by the patient, can occur with the use of BELSOMRA. Prescribers should explain the nature of these events to patients when prescribing BELSOMRA.
- Symptoms similar to mild cataplexy can occur, with risk increasing with the dose of BELSOMRA. Such symptoms can include periods of leg weakness lasting from seconds to a few minutes, can occur both at night and during the day, and may not be associated with an identified triggering event (e.g., laughter or surprise).
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
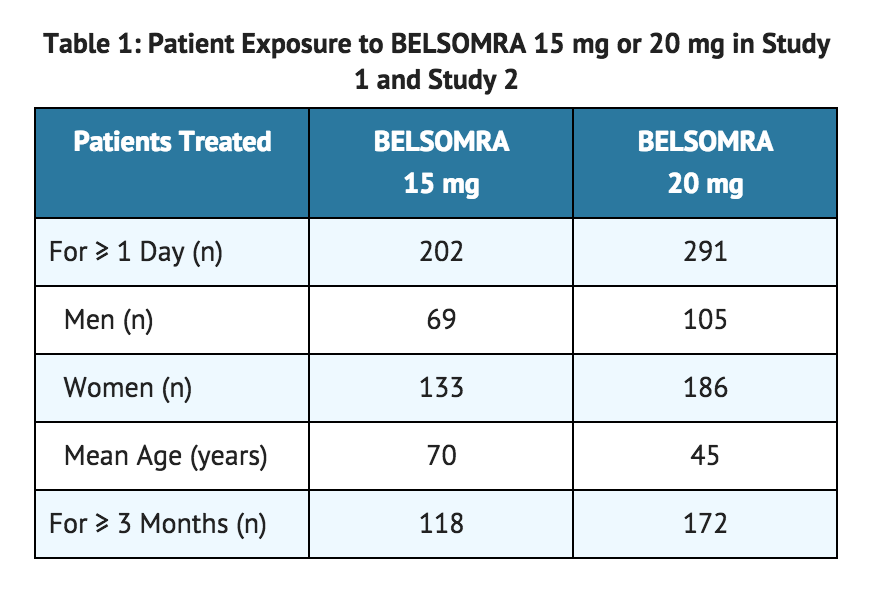
- In 3-month controlled efficacy trials (Study 1 and Study 2), 1263 patients were exposed to BELSOMRA including 493 patients who received BELSOMRA 15 mg or 20 mg (see TABLE 1).
- In a long-term study, additional patients (n=521) were treated with BELSOMRA at higher than recommended doses, including a total of 160 patients who received BELSOMRA for at least one year.
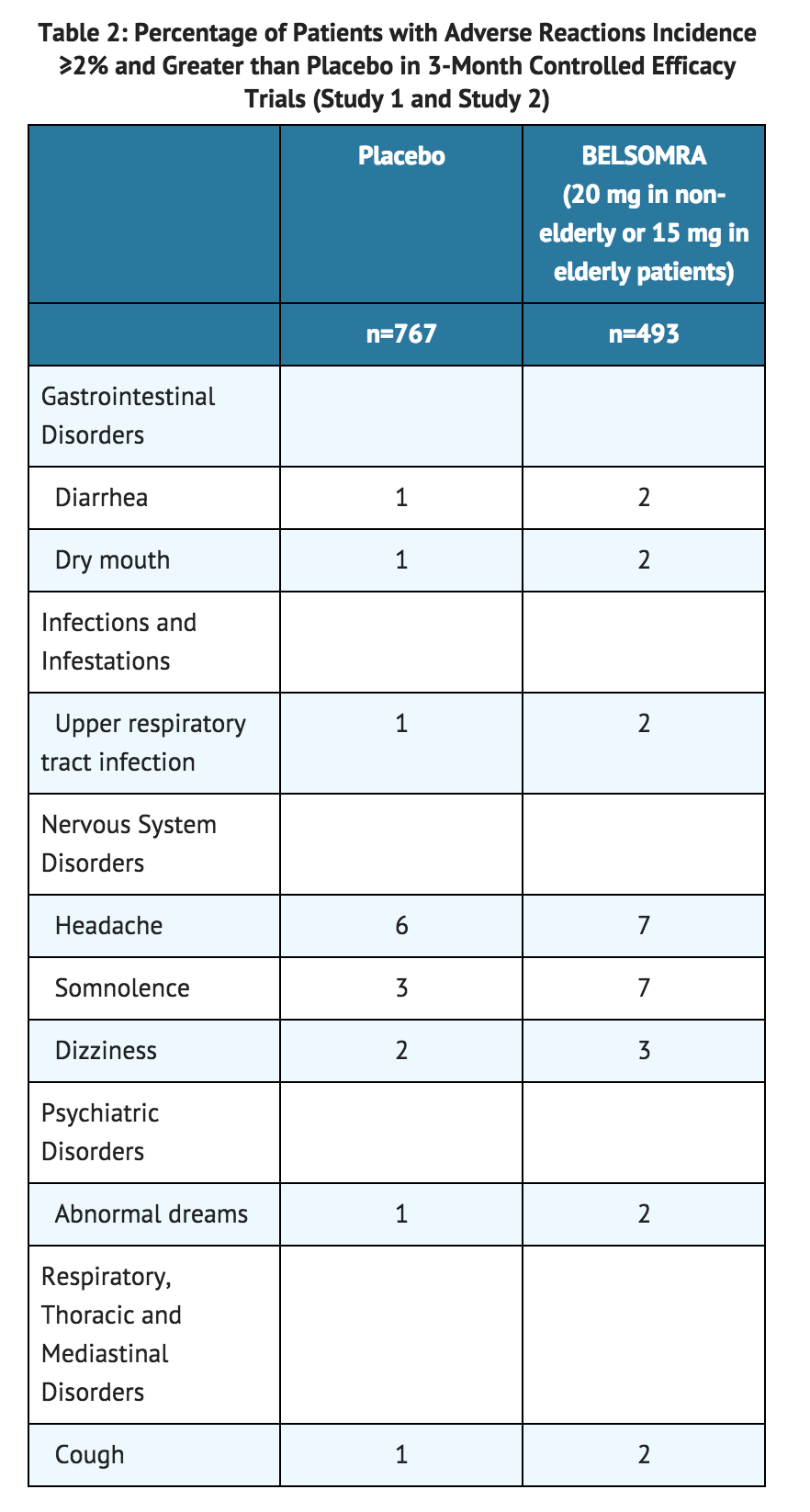
The pooled safety data described below (see TABLE 2) reflect the adverse reaction profile during the first 3 months of treatment.
Adverse Reactions Resulting in Discontinuation of Treatment
- The incidence of discontinuation due to adverse reactions for patients treated with 15 mg or 20 mg of BELSOMRA was 3% compared to 5% for placebo. No individual adverse reaction led to discontinuation at an incidence ≥1%.
Most Common Adverse Reactions
- In clinical trials of patients with insomnia treated with BELSOMRA 15 mg or 20 mg, the most common adverse reaction (reported in 5% or more of patients treated with BELSOMRA and at least twice the placebo rate) was somnolence (BELSOMRA 7%; placebo 3%).
- Table 2 shows the percentage of patients with adverse reactions during the first three months of treatment, based on the pooled data from 3-month controlled efficacy trials (Study 1 and Study 2).
- At doses of 15 or 20 mg, the incidence of somnolence was higher in females (8%) than in males (3%). Of the adverse reactions reported in Table 2, the following occurred in women at an incidence of at least twice that in men: headache, abnormal dreams, dry mouth, cough, and upper respiratory tract infection.
- The adverse reaction profile in elderly patients was generally consistent with non-elderly patients. The adverse reactions reported during long-term treatment up to 1 year were generally consistent with those observed during the first 3 months of treatment.
Dose Relationship for Adverse Reactions
- There is evidence of a dose relationship for many of the adverse reactions associated with BELSOMRA use, particularly for certain CNS adverse reactions.
- In a placebo-controlled crossover study (Study 3), non-elderly adult patients were treated for up to one month with BELSOMRA at doses of 10 mg, 20 mg, 40 mg (2 times the maximum recommended dose) or 80 mg (4 times the maximum recommended dose). In patients treated with BELSOMRA 10 mg (n=62), although no adverse reactions were reported at an incidence of ≥2%, the types of adverse reactions observed were similar to those observed in patients treated with BELSOMRA 20 mg. BELSOMRA was associated with a dose-related increase in somnolence: 2% at the 10 mg dose, 5% at the 20 mg dose, 12% at the 40 mg dose, and 11% at the 80 mg dose, compared to <1% for placebo. BELSOMRA was also associated with a dose-related increase in serum cholesterol: 1 mg/dL at the 10 mg dose, 2 mg/dL at the 20 mg dose, 3 mg/dL at the 40 mg dose, and 6 mg/dL at the 80 mg dose after 4 weeks of treatment, compared to a 4 mg/dL decrease for placebo.
Postmarketing Experience
There is limited information regarding postmarketing experience.
Drug Interactions
CNS-Active Agents
- When BELSOMRA was co-administered with alcohol, additive psychomotor impairment was demonstrated. There was no alteration in the pharmacokinetics of BELSOMRA .
Effects of Other Drugs on BELSOMRA
- Metabolism by CYP3A is the major elimination pathway for suvorexant.
- CYP3A Inhibitors
- Concomitant use of BELSOMRA with strong inhibitors of CYP3A (e.g., ketoconazole, itraconazole, posaconazole, clarithromycin, nefazodone, ritonavir, saquinavir, nelfinavir, indinavir, boceprevir, telaprevir, telithromycin and conivaptan) is not recommended.
- The recommended dose of BELSOMRA is 5 mg in subjects receiving moderate CYP3A inhibitors (e.g., amprenavir, aprepitant, atazanavir, ciprofloxacin, diltiazem, erythromycin, fluconazole, fosamprenavir, grapefruit juice, imatinib, verapamil). The dose can be increased to 10 mg in these patients if necessary for efficacy.
- CYP3A Inducers
- Suvorexant exposure can be substantially decreased when co-administered with strong CYP3A inducers (e.g., rifampin, carbamazepine and phenytoin). The efficacy of BELSOMRA may be reduced.
Effects of BELSOMRA on Other Drugs
- Digoxin
- Concomitant administration of BELSOMRA with digoxin slightly increased digoxin levels due to inhibition of intestinal P-gp. Digoxin concentrations should be monitored when co-administering BELSOMRA with digoxin.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA): C here are no adequate and well-controlled studies in pregnant women. BELSOMRA should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Administration of suvorexant to pregnant rats throughout organogenesis in two separate studies at oral doses of 30, 150, and 1000 mg/kg or 30, 80, and 325 mg/kg resulted in a decrease in fetal body weight at doses greater than 80 mg/kg. Plasma exposures (AUC) at the no-effect dose were approximately 25 times that in humans at the maximum recommended human dose (MRHD) of 20 mg/day.
Administration of suvorexant to pregnant rabbits throughout organogenesis in two separate studies at oral doses of 40, 100, and 300 mg/kg or 50, 150, and 325 mg/kg resulted in no apparent adverse effects on embryo-fetal development. Excessive toxicity resulted in premature sacrifice of pregnant animals at 325 mg/kg. The highest maternal plasma exposures (AUC) for which there are fetal data were up to approximately 40 times that in humans at the MRHD.
Administration of suvorexant (oral doses of 30, 80, and 200 mg/kg) to pregnant rats throughout gestation and lactation resulted in decreased body weight in offspring at the highest dose tested. Plasma AUCs at the no-effect dose were approximately 25 times that in humans at the MRHD.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Suvorexant in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Suvorexant during labor and delivery.
Nursing Mothers
Suvorexant and a hydroxyl-suvorexant metabolite were excreted in rat milk at levels higher (9 and 1.5 times, respectively) than that in maternal plasma. It is not known whether this drug is secreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when BELSOMRA is administered to a nursing woman.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
Geriatic Use
Of the total number of patients treated with BELSOMRA (n=1784) in controlled clinical safety and efficacy studies, 829 patients were 65 years and over, and 159 patients were 75 years and over. No clinically meaningful differences in safety or effectiveness were observed between these patients and younger patients at the recommended doses.
Gender
There is no FDA guidance on the use of Suvorexant with respect to specific gender populations.
Race
There is no FDA guidance on the use of Suvorexant with respect to specific racial populations.
Renal Impairment
No dose adjustment is required in patients with renal impairment.
Hepatic Impairment
No dose adjustment is required in patients with mild and moderate hepatic impairment. BELSOMRA has not been studied in patients with severe hepatic impairment and is not recommended for these patients.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Suvorexant in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Suvorexant in patients who are immunocompromised.
Patients with Compromised Respiratory Function
Effects of BELSOMRA on respiratory function should be considered if prescribed to patients with compromised respiratory function.
Obstructive Sleep Apnea
The respiratory depressant effect of BELSOMRA was evaluated after one night and after four consecutive nights of treatment in a randomized, placebo-controlled, 2-period crossover study in patients (n=26) with mild to moderate obstructive sleep apnea. Following once-daily doses of 40 mg, the mean Apnea/Hypopnea Index treatment difference (suvorexant – placebo) on Day 4 was 2.7 (90% CI: 0.22 to 5.09), but there was wide inter- and intra-individual variability such that clinically meaningful respiratory effects of BELSOMRA in obstructive sleep apnea cannot be excluded. BELSOMRA has not been studied in patients with severe obstructive sleep apnea.
Chronic Obstructive Pulmonary Disease
The respiratory depressant effect of BELSOMRA was evaluated after one night and after four consecutive nights of treatment in a randomized, placebo-controlled, 2-period crossover study in patients (n=25) with mild to moderate chronic obstructive pulmonary disease (COPD). BELSOMRA (40 mg in non-elderly, 30 mg in elderly) had no respiratory depressant effects in patients with mild to moderate COPD, as measured by oxygen saturation. There was wide inter- and intra-individual variability such that clinically meaningful respiratory effects of BELSOMRA in COPD cannot be excluded. BELSOMRA has not been studied in patients with severe COPD.
Administration and Monitoring
Administration
There is limited information regarding Suvorexant Administration in the drug label.
Monitoring
There is limited information regarding Suvorexant Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Suvorexant and IV administrations.
Overdosage
There is limited premarketing clinical experience with an overdosage of BELSOMRA. In clinical pharmacology studies, healthy subjects who were administered morning doses of up to 240 mg of suvorexant showed dose-dependent increases in the frequency and duration of somnolence.
General symptomatic and supportive measures should be used, along with immediate gastric lavage where appropriate. Intravenous fluids should be administered as needed. As in all cases of drug overdose, vital signs should be monitored and general supportive measures employed. The value of dialysis in the treatment of overdosage has not been determined. As suvorexant is highly protein-bound, hemodialysis is not expected to contribute to elimination of suvorexant.
As with the management of all overdosage, the possibility of multiple drug ingestion should be considered. Consider contacting a poison control center for up-to-date information on the management of hypnotic drug product overdosage.
Pharmacology
There is limited information regarding Suvorexant Pharmacology in the drug label.
Mechanism of Action
The mechanism by which suvorexant exerts its therapeutic effect in insomnia is presumed to be through antagonism of orexin receptors. The orexin neuropeptide signaling system is a central promoter of wakefulness. Blocking the binding of wake-promoting neuropeptides orexin A and orexin B to receptors OX1R and OX2R is thought to suppress wake drive.
Antagonism of orexin receptors may also underlie potential adverse effects such as signs of narcolepsy/cataplexy. Genetic mutations in the orexin system in animals result in hereditary narcolepsy; loss of orexin neurons has been reported in humans with narcolepsy.
Structure
There is limited information regarding Suvorexant Structure in the drug label.
Pharmacodynamics
Evaluation of QTc Interval
The effects of suvorexant on the QTc interval were evaluated in a randomized, placebo-, and active-controlled (moxifloxacin 400 mg) crossover study in healthy subjects (n=53). The upper bound of the one-sided 95% confidence interval for the largest placebo-adjusted, baseline-corrected QTc interval was below 10 ms based on analysis of suvorexant doses up to 240 mg, 12 times the maximum recommended dose. BELSOMRA thus does not prolong the QTc interval to any clinically relevant extent.
Pharmacokinetics
There is limited information regarding Suvorexant Pharmacokinetics in the drug label.
Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility Carcinogenesis
In a 26-week study in Tg.rasH2 mice, there was no evidence of suvorexant-induced neoplasms at oral doses of 25, 50, 200, and 650 mg/kg/day.
In a 2-year study in rats (oral suvorexant doses of 80, 160, and 325 mg/kg/day), increases in thyroid (follicular cell adenoma and combined adenoma/carcinoma in high-dose females; follicular cell adenoma in mid- and high-dose males) and liver (hepatocellular adenoma in high-dose males) neoplasms were observed. These findings were consistent with increased TSH and hepatic enzyme induction, respectively, which are mechanisms believed to be rodent-specific. Plasma exposures (AUC) at doses not associated with drug-induced neoplasms in rats were approximately 7 times that in humans at the maximum recommended human dose (MRHD) of 20 mg.
Mutagenesis
Suvorexant was negative in in vitro (bacterial reverse mutation and chromosomal aberration) and in vivo (mouse and rat micronucleus) assays.
Impairment of Fertility
In two separate studies, male and female rats were treated with suvorexant prior to and during mating and continuing in females to gestation day 7. Increases in peri-implantation loss and resorptions, resulting in a decrease in live fetuses, were observed at the highest doses tested (1200 or 325 mg/kg) when treated males and females were mated with untreated animals. At the no-effect dose for adverse effects on fertility in males and females, plasma AUCs were approximately 20 times that in humans at the MRHD.
13.2 Animal Toxicology and/or Pharmacology In dogs, daily oral administration of suvorexant (5, 30 mg/kg) for 4-7 days resulted in behavior characteristic of cataplexy (e.g., transient limb buckling, prone posture) when presented with food enrichment, a stimulus demonstrated to induce cataplexy in dogs with hereditary narcolepsy.
In the 2-year carcinogenicity study in rats, an increased incidence of retinal atrophy was observed at all doses. Plasma AUCs at the lowest dose tested were approximately 7 times that in humans at the MRHD.
In subsequent studies of suvorexant in albino and pigmented rats, retinal atrophy was delayed in onset and, after approximately one year of dosing, was of lower incidence and severity in pigmented rats.
Clinical Studies
There is limited information regarding Suvorexant Clinical Studies in the drug label.
How Supplied
No. 3062 — BELSOMRA tablets, 5 mg, are yellow, round, film-coated tablets, with "5" on one side and plain on the other side. They are supplied as follows: NDC 0006-0005-30 unit-of-use blisters of 30
No. 3063 — BELSOMRA tablets, 10 mg, are green, round, film-coated tablets, with "33" on one side and plain on the other side. They are supplied as follows: NDC 0006-0033-30 unit-of-use blisters of 30
No. 3981 — BELSOMRA tablets, 15 mg, are white, oval, film-coated tablets with the Merck logo on one side and "325" on the other side. They are supplied as follows: NDC 0006-0325-30 unit-of-use blisters of 30
No. 3982 — BELSOMRA tablets, 20 mg, are white, round, film-coated tablets with the Merck logo and "335" on one side and plain on the other side. They are supplied as follows: NDC 0006-0335-30 unit-of-use blisters of 30
Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F), [see USP Controlled Room Temperature]. Store in the original package until use to protect from light and moisture.
Images
Drug Images
{{#ask: Page Name::Suvorexant |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Suvorexant |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Suvorexant Patient Counseling Information in the drug label.
Precautions with Alcohol
Alcohol-Suvorexant interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
There is limited information regarding Suvorexant Brand Names in the drug label.
Look-Alike Drug Names
There is limited information regarding Suvorexant Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.