Sandbox:Sahar: Difference between revisions
Jump to navigation
Jump to search
No edit summary |
No edit summary |
||
| (3 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
{| class="wikitable" | |||
! style="background: #4479BA; width: 100px;" | {{fontcolor|#FFF|Amyloisosis subtype}} | |||
! style="background: #4479BA; width: 100px;" | {{fontcolor|#FFF|Protein}} | |||
! style="background: #4479BA; width: 100px;" | {{fontcolor|#FFF|Involved organs severity}} | |||
! style="background: #4479BA; width: 100px;" | {{fontcolor|#FFF|}} | |||
! | |||
|- | |||
! | |||
! | |||
! | |||
! | |||
! | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC; font-weight: bold" |Primary | |||
|_ | |||
|[[Anemia]] | |||
|[[MRI]] is the best radiologic tool to differentiate between retroperitoneal masses. | |||
| | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC; font-weight: bold" |Secondary | |||
|✔ | |||
|[[Leukocytosis]], positive inflammatory markers | |||
| | |||
| | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC; font-weight: bold" |DRA (dialysis related amyloidosis) | |||
|✔ | |||
|positive [[tumor marker]] | |||
| | |||
| | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC; font-weight: bold" |Senile systemic (cardiac) amyloidosis | |||
|_ | |||
|[[Diabetes mellitus|DM type II]], [[amylase]] and [[lipase]] levels may be slightly elevated | |||
| | |||
| | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC; font-weight: bold" |Meretoja syndrome | |||
| | |||
| | |||
| | |||
| | |||
|} | |||
{{familytree/start |summary=Sample 1}} | {{familytree/start |summary=Sample 1}} | ||
{{familytree | | | | | E04 | | | | |E04=[[Infection]]/[[Inflammation]]}} | {{familytree | | | | | E04 | | | | |E04=[[Infection]]/[[Inflammation]]}} | ||
| Line 18: | Line 62: | ||
{{familytree | | | | | K05 | | | | |K05=Resistant to proteolysis}} | {{familytree | | | | | K05 | | | | |K05=Resistant to proteolysis}} | ||
{| | {| | ||
! colspan="2" style="background:#DCDCDC;" align="center" + |The above algorithm is adopted from International Journal of Nephrology and Renovascular Disease | ! colspan="2" style="background:#DCDCDC;" align="center" + |The above algorithm is adopted from International Journal of Nephrology and Renovascular Disease | ||
|- | |- | ||
|} | |} | ||
| Line 812: | Line 856: | ||
</gallery> | </gallery> | ||
</div> | </div> | ||
<references /> | |||
Revision as of 05:29, 10 November 2019
| Amyloisosis subtype | Protein | Involved organs severity | ||
|---|---|---|---|---|
| Primary | _ | Anemia | MRI is the best radiologic tool to differentiate between retroperitoneal masses. | |
| Secondary | ✔ | Leukocytosis, positive inflammatory markers | ||
| DRA (dialysis related amyloidosis) | ✔ | positive tumor marker | ||
| Senile systemic (cardiac) amyloidosis | _ | DM type II, amylase and lipase levels may be slightly elevated | ||
| Meretoja syndrome |
| Infection/Inflammation | |||||||||||||||||||||||
| Increased production of IL-1/IL-6/TNF-α | |||||||||||||||||||||||
| Upregulation of hepatic serum amyloid A production | |||||||||||||||||||||||
| SAA production uptake by macrophages | |||||||||||||||||||||||
| C-terminal cleavage of SAA | |||||||||||||||||||||||
| β-sheet configuration of SAA | |||||||||||||||||||||||
| Fibril deposition in extracellular space | |||||||||||||||||||||||
| Binding of glycosaminoglycan, serum amyloid P, and lipid components | |||||||||||||||||||||||
| Resistant to proteolysis | |||||||||||||||||||||||
| The above algorithm is adopted from International Journal of Nephrology and Renovascular Disease |
|---|
| Organ System Involvement | Differential Diagnosis | Causes | Clinical Features | Laboratory Findings | Gold Standard Test | Therapy |
|---|---|---|---|---|---|---|
| Nephrotic Syndrome and Renal Failure | Secondary (AA) Amyloidosis |
|
|
|
|
|
| Primary (AL) Amyloidosis |
|
|
|
|||
| Diabetic Nephropathy |
|
|
|
|||
| Minimal Change Disease |
|
| ||||
| Focal Segmental Glomerulosclerosis | ||||||
| Fabry's Disease |
|
|
|
|
| |
| Light Chain Deposition Disease |
|
|
| |||
| Membranous Glomerulonephritis |
|
|
|
|
| |
| Fibrillary-Immunotactoid Glomerulopathy |
|
|
|
|||
| Organ System Involvement | Differential Diagnosis | Causes | Clinical Features | Laboratory Findings | Gold Standard Test | Therapy |
| Polyneuropathy | POEMS syndrome (Demyelinating) |
|
|
|||
| Metabolic Syndrome (Axonal pathology) |
|
|
|
|||
| Vitamin Deficiencies (Axonal Pathology) |
|
|
|
| ||
| Guillain-Barre Syndrome (Demyelinating) |
|
|
|
|||
| Chronic Inflammatory Demyelinating Polyneuropathy (CIDP) (Mixed axonal and demyelinatiing) |
|
|
|
|
||
| Multifocal Motor Neuropathy |
|
|||||
| Organ System Involvement | Differential Diagnosis | Causes | Features | Laboratory Findings | Gold Standard Test | Therapy |
| Organomegaly (Hepatosplenomegaly and Lymphadenopathy) | Malaria |
|
|
| ||
| Kala-azar |
|
|
|
|||
| Infective Hepatitis |
|
|
||||
| Chronic Myelogenous Leukemia (CML) |
|
|
||||
| Lymphoma |
|
|
||||
| Primary (AL) Amyloidosis |
|
|
|
| ||
| Gaucher's Disease |
|
|
|
|
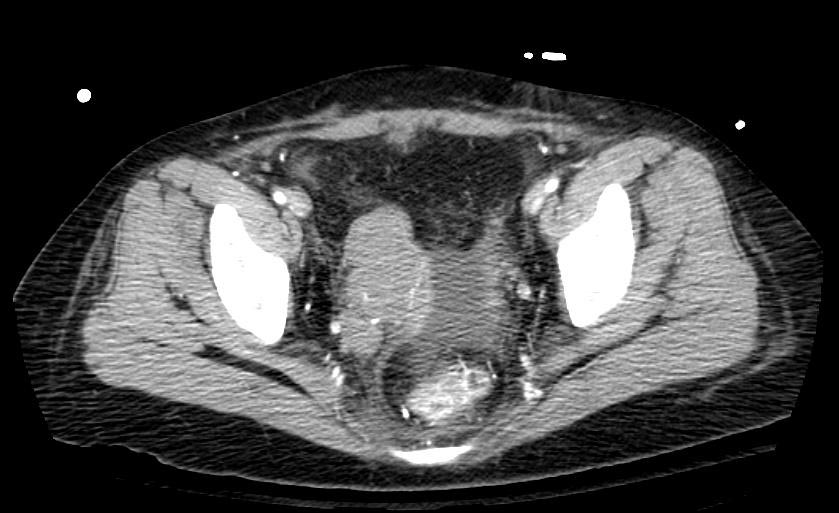
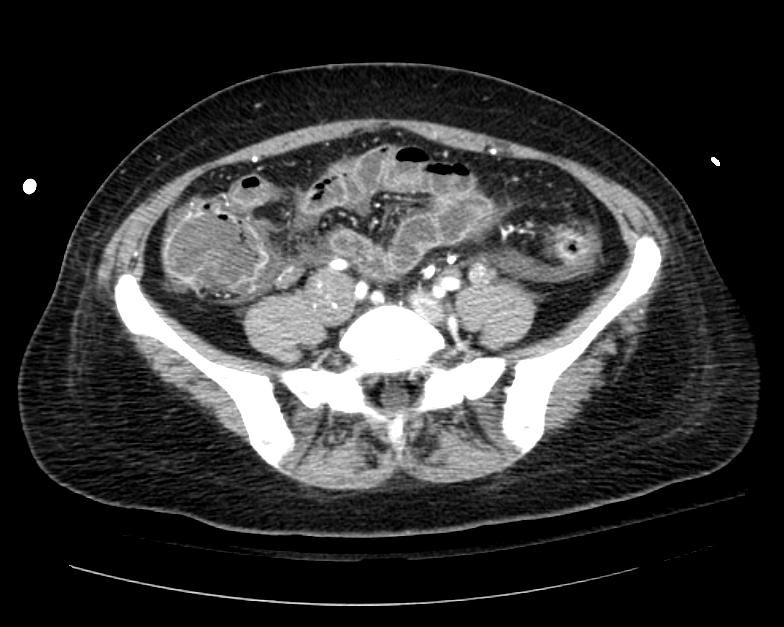
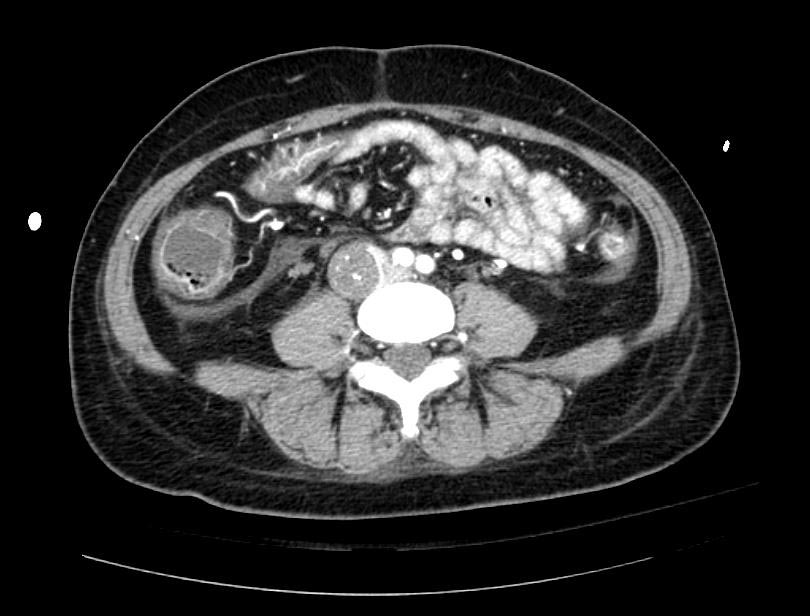
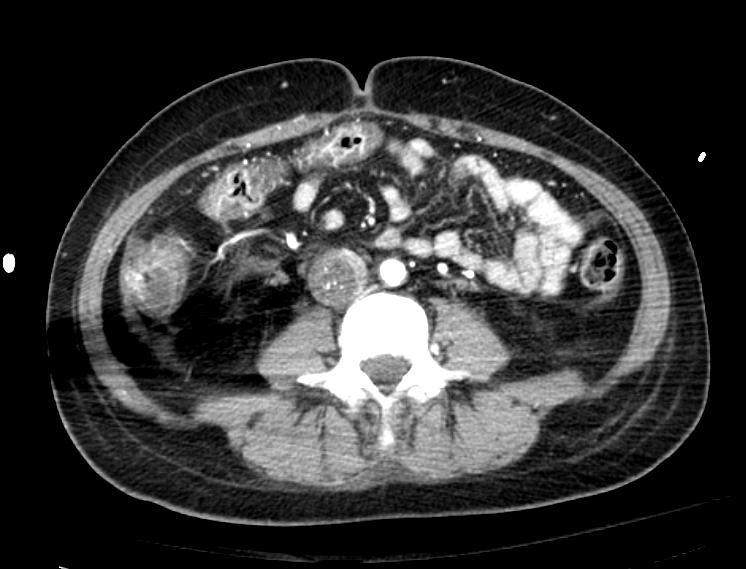
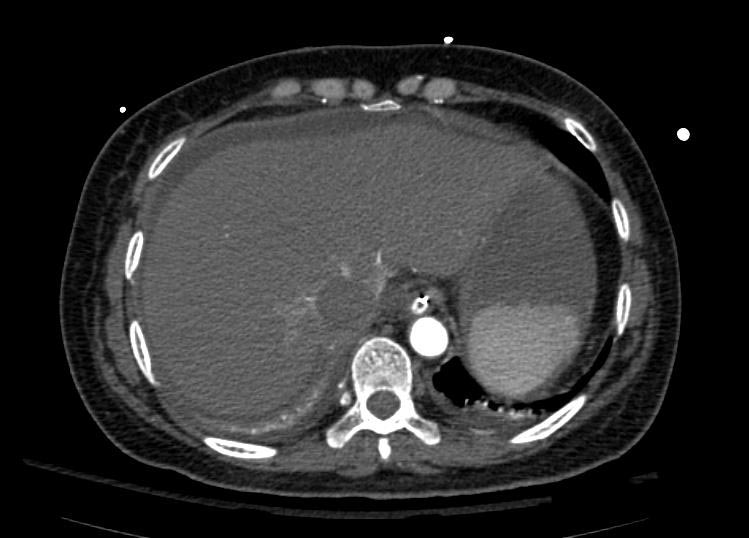
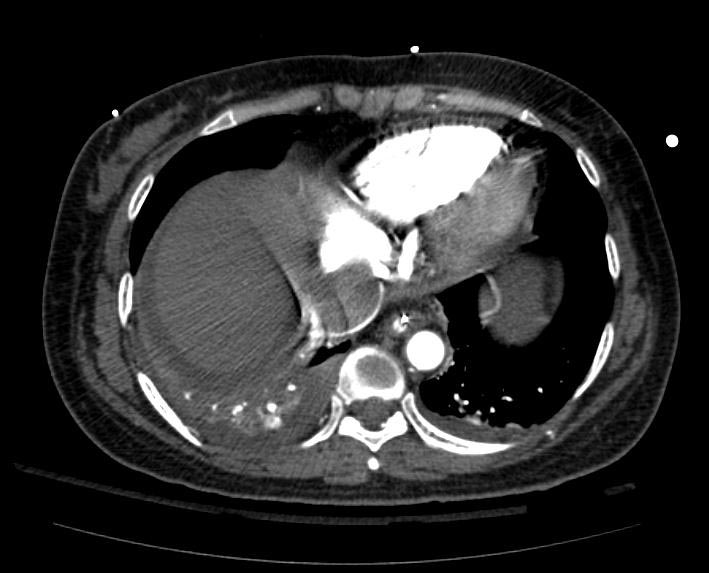
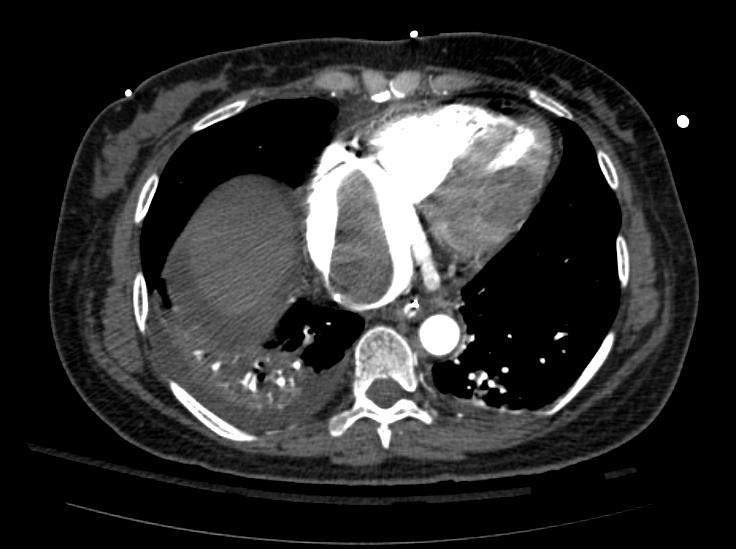
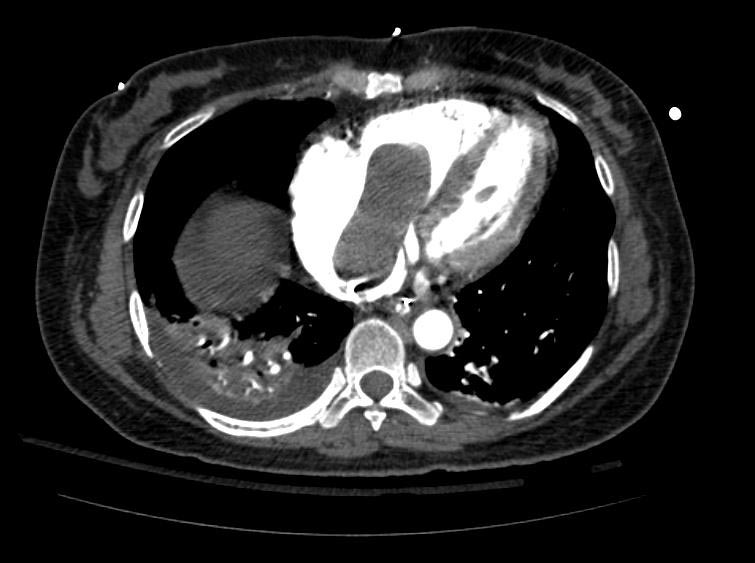
Example #1
The patient presented with S.O.B. one year after hysterectomy for a leiomyomatous uterus.