Parasympathetic nervous system
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
The parasympathetic nervous system (PSNS) is one of three divisions of the autonomic nervous system (ANS). The ANS—a subdivision of the peripheral nervous system (PNS)—is subdivided into the sympathetic (SNS), parasympathetic (PSNS) and enteric (bowels) nervous system (ENS).
Relationship to sympathetic nervous system
Sympathetic and parasympathetic divisions typically function in opposition to each other. But this opposition is better termed complementary in nature rather than antagonistic. For an analogy, one may think of the sympathetic division as the accelerator and the parasympathetic division as the brake. The sympathetic division typically functions in actions requiring quick responses. The parasympathetic division functions with actions that do not require immediate reaction.
Physical Location
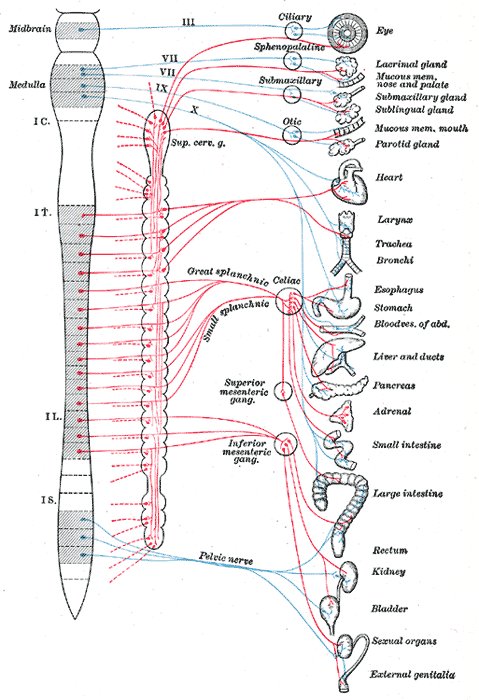
The parasympathetic nervous system is a portion of the visceral (autonomic) branch of the PNS (peripheral nervous system). The regions of the body associated with this division are the cranial and sacral regions of the spinal cord. Specifically, cranial nerves III, VII, IX, X (vagus n.) and in the sacral region (spinal nerves exiting from the sacrum) the spinal nerves S2 to S4.
Similar to the sympathetic division, the parasympathetic division also has pre- and post- ganglionic neurons. Typically, in the parasympathetic division the ganglion will be closer to the area of innervation - unlike the sympathetic ganglion which form immediately lateral and inferior to the spinal nerve - making up the so called "chain ganglion".
Receptors
The parasympathetic nervous system uses only acetylcholine (ACh) as its neurotransmitter. The ACh acts on two types of receptors, the muscarinic and nicotinic cholinergic receptors. Most transmissions occur in two stages: When stimulated, the preganglionic nerve releases ACh at the ganglion, which acts on nicotinic receptors of the postganglionic nerve. The postganglionic nerve then releases ACh to stimulate the muscarinic receptors of the target organ.
Types of muscarinic receptors
The three main types of muscarinic receptors that are well characterised are:
- The M1 muscarinic receptors (CHRM1) are located in the neural system.
- The M2 muscarinic receptors (CHRM2) are located in the heart, and act to bring the heart back to normal after the actions of the sympathetic nervous system: slowing down the heart rate, reducing contractile forces of the atrial cardiac muscle, and reducing conduction velocity of the sinoatrial node (SA node) and atrioventricular node (AV node). Note, they have no minimal on the contractile forces of the ventricular muscle due to sparse innervation of the ventricles from the parasympathetic nervous system.
- The M3 muscarinic receptors (CHRM3) are located at many places in the body, such as the smooth muscles of the blood vessels causing vasodilation, as well as the lungs causing bronchoconstriction. They are also in the smooth muscles of the gastrointestinal tract (GIT), which help in increasing intestinal motility and dilating sphincters. The M3 receptors are also located in many glands that help to stimulate secretion in salivary glands and other glands of the body.
- The M4 muscarinic receptors: Postganglionic cholinergic nerves, possible CNS effects
- The M5 muscarinic receptors: Possible effects on the CNS
External links
Template:Nervous system Template:Autonomic
da:Parasympatiske nervesystem
de:Parasympathikus
dv:ޕެރަސިމްޕަތެޓިކް ނާރވަސް ސިސްޓަމް
lt:Parasimpatinė nervų sistema
nl:Parasympatisch zenuwstelsel
fi:Parasympaattinen hermosto
uk:Парасимпатична нервова система