Marfan's syndrome: Difference between revisions
No edit summary |
No edit summary |
||
| Line 19: | Line 19: | ||
{{Editor Help}} | {{Editor Help}} | ||
==Overview== | |||
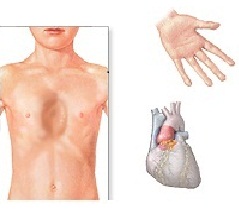
'''Marfan syndrome''' is an [[autosomal dominant]] genetic disorder of the [[connective tissue]] characterized by disproportionately long [[limb]]s, long thin fingers, a typically tall stature, and a predisposition to cardiovascular abnormalities, specifically those affecting the [[heart valves]] and [[aorta]]. The disorder may also affect numerous other structures and organs — including the [[lung]]s, eyes, dural sac surrounding the [[spinal cord]], and [[hard palate]]. | '''Marfan syndrome''' is an [[autosomal dominant]] genetic disorder of the [[connective tissue]] characterized by disproportionately long [[limb]]s, long thin fingers, a typically tall stature, and a predisposition to cardiovascular abnormalities, specifically those affecting the [[heart valves]] and [[aorta]]. The disorder may also affect numerous other structures and organs — including the [[lung]]s, eyes, dural sac surrounding the [[spinal cord]], and [[hard palate]]. | ||
Revision as of 16:22, 19 March 2009
| Marfan syndrome | |
 | |
|---|---|
| ICD-10 | Q87.4 |
| ICD-9 | 759.82 |
| OMIM | 154700 |
| DiseasesDB | 7845 |
| MedlinePlus | 000418 |
| eMedicine | ped/1372 orthoped/414 |
| MeSH | C17.300.500 |
|
WikiDoc Resources for Marfan's syndrome |
|
Articles |
|---|
|
Most recent articles on Marfan's syndrome Most cited articles on Marfan's syndrome |
|
Media |
|
Powerpoint slides on Marfan's syndrome |
|
Evidence Based Medicine |
|
Cochrane Collaboration on Marfan's syndrome |
|
Clinical Trials |
|
Ongoing Trials on Marfan's syndrome at Clinical Trials.gov Trial results on Marfan's syndrome Clinical Trials on Marfan's syndrome at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Marfan's syndrome NICE Guidance on Marfan's syndrome
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Marfan's syndrome Discussion groups on Marfan's syndrome Patient Handouts on Marfan's syndrome Directions to Hospitals Treating Marfan's syndrome Risk calculators and risk factors for Marfan's syndrome
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Marfan's syndrome |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
| Cardiology Network |
 Discuss Marfan's syndrome further in the WikiDoc Cardiology Network |
| Adult Congenital |
|---|
| Biomarkers |
| Cardiac Rehabilitation |
| Congestive Heart Failure |
| CT Angiography |
| Echocardiography |
| Electrophysiology |
| Cardiology General |
| Genetics |
| Health Economics |
| Hypertension |
| Interventional Cardiology |
| MRI |
| Nuclear Cardiology |
| Peripheral Arterial Disease |
| Prevention |
| Public Policy |
| Pulmonary Embolism |
| Stable Angina |
| Valvular Heart Disease |
| Vascular Medicine |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [2] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Overview
Marfan syndrome is an autosomal dominant genetic disorder of the connective tissue characterized by disproportionately long limbs, long thin fingers, a typically tall stature, and a predisposition to cardiovascular abnormalities, specifically those affecting the heart valves and aorta. The disorder may also affect numerous other structures and organs — including the lungs, eyes, dural sac surrounding the spinal cord, and hard palate.
Etymology
It is named after Antoine Marfan, the French pediatrician who first described it in 1899.
Epidemiology
Marfan syndrome affects males and females equally,[1] and the mutation shows no geographical bias. Estimates indicate that approximately 60 000 (1 in 5000, or 0.02% of the population)[1] to 200 000[2] Americans have Marfan syndrome. Each parent with the condition has a 50% chance of passing it on to a child due to its autosomal dominant nature. Most individuals with Marfan syndrome have another affected family member, but approximately 15-30% of all cases are due to de novo genetic mutations[3] — such spontaneous mutations occur in about 1 in 20 000 births. Marfan syndrome is also an example of dominant negative mutation and haploinsufficiency.[4][5] It is associated with variable expressivity. Incomplete penetrance, has not been definitively documented.
Pathogenesis
Marfan syndrome has been linked to a defect in the FBN1 gene on chromosome 15,[6] which encodes a glycoprotein called fibrillin-1. Fibrillin is essential for the formation of the elastic fibers found in connective tissue, as it provides the scaffolding for tropoelastin.[3] Elastic fibers are found throughout the body but are particularly abundant in the aorta, ligaments and the ciliary zonules of the eye, consequently these areas are among the worst affected. Without the structural support provided by fibrillin many connective tissues are weakened, which can have severe consequences for support and stability.
A related disease has been found in mice, and the study of mouse fibrillin synthesis and secretion, and connective tissue formation, has begun to further our understanding of Marfan syndrome in humans. It has been found that simply reducing the level of normal fibrillin-1 causes a Marfan-related disease in mice.[7]
Transforming growth factor beta (TGFβ) plays an important role in Marfan syndrome. Fibrillin-1 binds TGFβ and inactivates it. In Marfan syndrome, reduced levels of fibrillin-1 allow activated TGFβ to damage the lungs and heart. A defect in the gene TGFβR2 on chromosome 3, a receptor protein of TGFβ, has also been related to Marfan syndrome.[8] Marfan syndrome can often be confused with Loeys-Dietz syndrome, a similar connective tissue disorder resulting from mutations in the TGFβ receptor genes TGFβR1 and TGFβR2.[9]
Symptoms
There are no signs or symptoms that are unique to Marfan syndrome. It is usually a single apparent sign or symptom that leads doctors to look for others and eventually to diagnose the syndrome, which affects connective tissue in diverse organs and systems. Even affected individuals in the same family might exhibit various combinations and severities of symptoms.
Skeletal system
The most readily visible signs are associated with the skeletal system. Many individuals with Marfan Syndrome grow to above average height. Some have long slender limbs with fingers and toes that are also abnormally long and slender (arachnodactyly). An individual's arms may be disproportionately long. In addition to affecting height and limb proportions, Marfan syndrome can produce other skeletal signs. Abnormal curvature of the spine (scoliosis) is common, as is abnormal indentation (pectus excavatum) or protrusion (pectus carinatum) of the sternum. Other signs include abnormal joint flexibility, a high palate, malocclusions, flat feet, stooped shoulders, and unexplained stretch marks on the skin. Some people with Marfans have speech disorders resulting from symptomatic high palates and small jaws.
Eyes
Marfan syndrome can also seriously affect the eyes and vision. Nearsightedness and astigmatism are common, but farsightedness can also result. Periodic eye exams can lead to an ophthalmologist or optometrist discovering dislocation, or subluxation, of the crystalline lens in one or both eyes (ectopia lentis) by carefully observing these structures using a slit-lamp biomicroscope. This can be differentiated from the similar condition homocystinuria, where the dislocation is inferonasal; in Marfan's the dislocation is superotemporal. Sometimes eye problems appear only after the weakening of connective tissue has caused detachment of the retina.[10] Early onset glaucoma can be another complication.
Cardiovascular system
The most serious conditions associated with Marfan syndrome involve the cardiovascular system. Undue fatigue, shortness of breath, heart palpitations, racing heartbeats, or pain in the left chest, back, shoulder, or arm, can bring an individual into the doctor's office. A heart murmur heard on a stethoscope, an abnormal reading on an electrocardiogram, or symptoms of angina can lead a doctor to order an echocardiogram. This can reveal signs of leakage or prolapse of the mitral or aortic valves that control the flow of blood through the heart. (See mitral valve prolapse.) However, the major sign that would lead a doctor to consider an underlying condition is a dilated aorta or an aortic aneurysm. Sometimes, no heart problems are apparent until the weakening of the connective tissue in the ascending aorta causes an aortic aneurysm or even aortic dissection.
Because of the underlying connective tissue abnormalities that cause Marfan syndrome, there is an increased incidence of dehiscence of prosthetic mitral valve.[11] Care should be taken to attempt repair of damaged heart valves rather than replacement.
During pregnancy, even in the absence of preconceived cardiovascular abnormality, women with Marfan syndrome are at significant risk of acute aortic dissection, which can be lethal if untreated. For this reason, women with Marfan syndrome should receive a thorough assessment prior to conception, and echocardiography should be performed every 6-10 weeks during pregnancy, to assess the aortic root diameter. Most women however tolerate pregnancy well and safe vaginal delivery is possible.[12]
- A typical aortic root in Marfan's syndrome.
<googlevideo>-760162053984535443&hl=en</googlevideo>
Lungs
Marfan syndrome is a risk factor for spontaneous pneumothorax. In spontaneous unilateral pneumothorax, air escapes from a lung and occupies the pleural space between the chest wall and a lung. The lung becomes partially compressed or collapsed. This can cause pain, shortness of breath, cyanosis, and, if not treated, death. Marfan syndrome has also been associated with sleep apnea and idiopathic obstructive lung disease.
Central nervous system
Another condition that can reduce the quality of life for an individual, though not life-threatening, is dural ectasia, the weakening of the connective tissue of the dural sac, the membrane that encases the spinal cord.
Dural ectasia can be present for a long time without producing any noticeable symptoms. Symptoms that can occur are lower back pain, leg pain, abdominal pain, other neurological symptoms in the lower extremities, or headaches. Such symptoms usually diminish when the individual lies flat on his or her back.
These types of symptoms might lead a doctor to order an X-ray of the lower spine. Dural ectasia is usually not visible on an X-ray in the early phases. A worsening of symptoms and the lack of finding any other cause should eventually lead a doctor to order an upright MRI of the lower spine.
Dural ectasia that has progressed to the point of causing these symptoms would appear in an upright MRI image as a dilated pouch that is wearing away at the lumbar vertebrae.[10] Other spinal issues associated with Marfan include degenerative disk disease and spinal cysts.
Management
There is no cure for Marfan syndrome, but life expectancy has increased significantly over the last few decades, and clinical trials are underway for a promising new treatment.[13] The syndrome is treated by addressing each issue as it arises, and, in particular, considering prophylactic medication, even for young children, to slow progression of aortic dilation.
Regular checkups by a cardiologist are needed to monitor the health of the heart valves and the aorta. The goal of treatment is to slow the progression of aortic dilation and damage to heart valves by eliminating arrythmias, minimizing the heart rate, and minimizing blood pressure.
Beta blockers have been used to control arrythmias and slow the heart rate. Other medications might be needed to further minimize blood pressure without slowing the heart rate, such as ACE inhibitors and angiotensin II receptor antagonists, also known as angiontensin receptor blockers (ARBs).
If the dilation of the aorta progresses to a significant diameter aneurysm, causes a dissection or a rupture, or leads to failure of the aortic or other valve, then surgery (possibly a composite aortic valve graft [CAVG] or valve-sparing procedure) becomes necessary.
Although aortic graft surgery (or any vascular surgery) is a serious undertaking it is generally successful if undertaken on an elective basis. Surgery in the setting of acute aortic dissection or rupture is considerably more problematic. Elective aortic valve/graft surgery is usually considered when aortic root diameter reaches 50 millimetres, but each case needs to be specifically evaluated by a qualified cardiologist. New valve-sparing surgical techniques are becoming more common.[14] As Marfan patients live longer, other vascular repairs are becoming more common, e.g. repairs of descending thoractic aortic aneurysms and aneurysms of vessels other than the aorta.
The skeletal and ocular manifestations of Marfan syndrome can also be serious, although not life-threatening. These symptoms are usually treated in the typical manner for the appropriate condition. This can also affect height, arm length, and life span. The Nuss procedure is now being offered to people with Marfan syndrome to correct 'sunken chest' or (pectus excavatum).[15] Because Marfan may cause spinal abnormalities that are asymptomatic, any spinal surgery contemplated on a Marfan patient should only follow detailed imaging and careful surgical planning, regardless of the indication for surgery.
Clinical trials have been conducted of the drug acetazolamide in the treatment of symptoms of dural ectasia. The treatment has demonstrated significant functional improvements in some sufferers.[16] Other medical treatments, as well as physical therapy, are also available.
Treatment of a spontaneous pneumothorax is dependant on the volume of air in the pleural space and the natural progression of the individual's condition. A small pneumothorax might resolve without active treatment in 1 to 2 weeks. Recurrent pneumothoraxes might require chest surgery. Moderately sized pneumothoraxes might need chest drain management for several days in hospital. Large pneumothoraxes are likely to be medical emergencies requiring emergency decompression.
Research in laboratory mice has suggested that the angiotensin II receptor antagonist losartan, which appears to block TGF-beta activity, can slow or halt the formation of aortic aneurysms in Marfan syndrome.[17] A large clinical trial sponsored by the National Institutes of Health comparing the effects of losartan and atenolol on the aortas of Marfan patients is scheduled to begin in early 2007, coordinated by Johns Hopkins.[18]
Genetic counseling and specialized clinics are available at many academic medical centers for affected persons and family members.
Related disorders
The following conditions that can result from having Marfan's syndrome and may also occur in people without any known underlying disorder. what leads doctors to a diagnosis of marfan syndrome is family history and a combination of major and minor indicators of the disorder that occur in one individual which is a rare manifestation in general population. Example: four skeletal signs with one or more signs in another body system such as ocular and cardiovascular in one individual.
- Aortic aneurysm or dilatation
- Arachnodactyly
- Bicuspid aortic valve
- Cysts
- Craniosynostosis
- Cystic medial necrosis
- Dural ectasia
- Ectopia lentis
- Flat feet
- Gigantism
- Glaucoma
- Hernias
- Hypermobility of the joints
- Malocclusion
- Mitral valve prolapse
- Myopia
- Obstructive lung disease
- Osteoarthritis
- Pectus carinatum or excavatum
- Pneumothorax
- Retinal detachment
- Scoliosis
- Sleep apnea
- Stretch marks
References
- ↑ 1.0 1.1 "The role of heredity and family history". National Marfan Foundation. 1999.
- ↑ "New, Deadly Relative of Marfan's Syndrome Discovered". MedicineNet.com. 2006.
- ↑ 3.0 3.1 Cotran. Robbins Pathologic Basis of Disease. Philadelphia: W.B Saunders Company. 0-7216-7335-X. Unknown parameter
|coauthors=ignored (help) - ↑ Judge, Daniel P. "Evidence for a critical contribution of haploinsufficiency in the complex pathogenesis of Marfan syndrome". The Journal of Clinical Investigation. 114 (2): 172–181. doi:10.1172/JCI200420641. PMID 15254584. Unknown parameter
|coauthors=ignored (help) - ↑ Judge, Daniel P. (2005). "Marfan's syndrome". Lancet. 366 (9501): 1965–76. doi:10.1016/S0140-6736(05)67789-6. Check
|doi=value (help). PMID 16325700. Unknown parameter|coauthors=ignored (help) - ↑ McKusick V (1991). "The defect in Marfan syndrome". Nature. 352 (6333): 279–81. PMID 1852198.
- ↑ Lygia Pereira; et al. (1999). "Pathogenetic sequence for aneurysm revealed in mice underexpressing fibrillin-1". Proceedings of the National Academy of Sciences. 96 (7): 3819-3823.
- ↑ Entrez Gene (2007). "TGFBR2 transforming growth factor, beta receptor II" (Entrez gene entry). NCBI.
- ↑ "Related Disorders: Loeys-Dietz". National Marfan Foundation.
- ↑ 10.0 10.1 "Marfan Syndrome". Mayo Clinic.
- ↑ Braunwald's Heart Disease ~ A Textbook of Cardiovascular Medicine, Seventh Edition. United States of America: Elseview Saunders. 2005. p. 1894. ISBN 0-7216-0509-5. Unknown parameter
|coauthors=ignored (help) - ↑ "Marfan Syndrome, special concerns".
- ↑ Freeman, Elaine (2007) "A Silver Bullet for Blake", Johns Hopkins Magazine, Fall, 2007.
- ↑ "Heart Surgery for Marfan Syndrome". Mayo Clinic.
- ↑ "Overview of the Nuss Procedure for Pectus Excavatum". Children's Hospital of The King's Daughters.
- ↑ "Dural Ectasia in the Marfan Spine: Symptoms and Treatment". Scoliosis Research Society.
- ↑ Habashi, Jennifer P. (April 7, 2006). "Losartan, an AT1 Antagonist, Prevents Aortic Aneurysm in a Mouse Model of Marfan Syndrome". 312 (5770): 117–121. doi:10.1126/science.1124287. Unknown parameter
|news=ignored (|newspaper=suggested) (help); Unknown parameter|abstract=ignored (help); Unknown parameter|coauthors=ignored (help); Check date values in:|date=(help) - ↑ "Atenolol vs. Losartan in Individuals with Marfan Syndrome Clinial Trial". National Marfan Foundation.
External links
- International Federation of Marfan Syndrome Organisations
- National Marfan Foundation (USA)
- Marfan diagnosis criteria
- National Institute for Health Marfan syndrome page (USA)
- Marfan Syndrome Center at medicinenet.com
- Marfan Syndrome Research - recent literature on Marfan Syndrome
- Marfan support
- Canadian Marfan Association
- Marfan Association UK
- Marfan de Mexico
- Norwegian Marfan Organization
- Marfan Life blog - mostly links to news articles about Marfan Syndrome
- MarfanSyndrome.Info - Findings in Marfan Syndrome and link collection
- Marfan-List - email discussion list for people and families with Marfan Syndrome
- South African Marfan Syndrome Organisation - support group for Africa
- Eye Findings in Marfan's syndrome
Template:Phakomatoses and other congenital malformations not elsewhere classified Template:SIB
ar:متلازمة مارفان de:Marfan-Syndrom ko:마르팡 증후군 it:Sindrome di Marfan he:תסמונת מרפן nl:Syndroom van Marfan nn:Marfans syndrom sr:Марфанов синдром fi:Marfanin oireyhtymä sv:Marfans syndrom uk:Синдром Марфана