Lymphadenopathy
|
Lymphadenopathy Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Lymphadenopathy On the Web |
|
American Roentgen Ray Society Images of Lymphadenopathy |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Shyam Patel [2] Associate Editor(s)-in-Chief: Maria Fernanda Villarreal, M.D. [3] Raviteja Guddeti, M.B.B.S. [4]
Synonyms and keywords: Lymph nodes enlarged; Enlarged lymph nodes; Lymphadenitis; Swollen lymph nodes; Swollen/enlarged lymph nodes
Overview
Lymphadenopathy (also known as "enlarged lymph nodes") refers to lymph nodes which are abnormal in size, number or consistency. Common causes of lymphadenopathy are infection, autoimmune disease, or malignancy. Lymphadenopathy may be classified according to distribution into 2 groups: generalized lymphadenopathy and localized lymphadenopathy. The pathogenesis of lymphadenopathy is characterized by the inflammation of lymph nodes. This process is primarily due to an elevated rate of trafficking of lymphocytes into the node from the blood, exceeding the rate of outflow from the node. Lymph nodes may also be enlarged secondarily as a result of the activation and proliferation of antigen-specific T and B cells (clonal expansion). Lymphadenopathy is very common, the estimated incidence of lymphadenopathy among children in the United States ranges from 35%- 45%. Patients of all age groups may develop lymphadenopathy. Lymphadenopathy is more commonly observed among children. Common complications of lymphadenopathy, may include: abscess formation, superior vena cava syndrome, and intestinal obstruction. Diagnostic criteria for malignant lymphadenopathy, may include: node > 2 cm, node that is draining, hard, or fixed to underlying tissue, atypical location (e.g. supraclavicular node), associated risk factors (e.g. HIV or TB), fever and/or weight loss, and splenomegaly. On the other hand, diagnostic criteria for benign lymphadenopathy, may include: node < 1 cm, node that is mobile, soft-or tender, and is not fixed to underlying tissue, typical location (e.g. supraclavicular node), no associated risk factors, and palpable and painful enlargement. Laboratory findings consistent with the diagnosis of lymphadenopathy, may include: elevated lactate dehydrogenase (LDH), mild neutropenia, and leukocytosis. There is no treatment for lymphadenopathy; the mainstay of therapy is treating the underlying condition.
Classification
- Generalized lymphadenopathy
- Localized lymphadenopathy
Pathophysiology
- The pathogenesis of lymphadenopathy is characterized by the inflammation of lymph nodes. This process is primarily due to an elevated rate of trafficking of lymphocytes into the node from the blood, exceeding the rate of outflow from the node.[1]
- The inmune response between the antigen and lymphocyte that leads to cellular proliferation and enlargement of the lymph nodes.
- Lymph nodes may also be enlarged secondarily as a result of the activation and proliferation of antigen-specific T and B cells (clonal expansion).
- On gross pathology, characteristic findings of lymphadenopathy, include:
- Enlarged lymph node
- Soft greasy yellow areas within capsule
- On microscopic histopathological analysis, characteristic findings of lymphadenopathy will depend on the aetiology.
- Common findings, include:[1][2]
Non-specific reactive follicular hyperplasia (NSRFH)
- Large spaced cortical follicles
- Tingible body macrophages, normal dark/light GC pattern
Lymph node metastasis
- Foreign cell population (usually in subcapsular sinuses)
- +/-nuclear atypia
- +/-malignant architecture
Toxoplasmosis
- Large follicles
- Epithelioid cells perifollicular & intrafollicular
- Reactive GCs
- Monocytoid cell clusters
Cat-scratch disease
- PMNs in necrotic area
- "Stellate" (or serpentine) shaped micro-abscesses
- Presence of granulomas
Dermatopathic lymphadenopathy
- Melanin-laden histiocytes
- Histiocytosis
Systemic lupus erythematosus lymphadenopathy
- Blue hematoxylin bodies
- Necrosis
- No PMNs
Causes
Differentiating Lymphadenopathy from other Diseases
- Lymphadenopathy must be differentiated from syphilis, which may present as fever, myalgias, weight loss, and lymph node enlargement.[3]
Epidemiology and Demographics
Risk Factors
- The most common risk factors in the development of lymphadenopathy, include:
- Local soft-tissue infections
- Upper respiratory tract infection
- Foreign travel
Natural History, Complications and Prognosis
- Patients with lymphadenopathy may be symptomatic or asymptomatic, depending on the aetiology.[1]
- Early clinical features include palpable tenderness, pain, and fever.[2]
- Common complications of lymphadenopathy, include:[2]
Mediastinal lymphadenopathy
- Superior vena cava syndrome
- Tracheal and bronchial obstruction
- Dysphagia
- Hemoptysis
- Uric acid nephropathy
- Hyperkalemia
- Hypercalcemia
- Hypocalcemia
- Hyperphosphatemia
- Renal failure
Abdominal lymphadenopathy
Superficial lymphadenopathy
- Abscess formation
- Cellulitis
- Fistulas (seen in lymphadenitis that is due to tuberculosis)
- Sepsis
- Prognosis will depend on the aetiology of the underlying disease.
Diagnosis
Diagnostic Criteria
Malignant Lymphadenopathy
- Node > 2 cm
- Node that is draining, hard, or fixed to underlying tissue
- Atypical location (e.g. supraclavicular node)
- Risk factors (e.g. HIV or TB)
- Fever and/or weight loss
- Splenomegaly
Benign Lymphadenopathy
- Node < 1 cm
- Node that is mobile, soft-or tender, and is not fixed to underlying tissue
- Common location (e.g. supraclavicular node)
- No associated risk factors
- Palpable and painful enlargement
Symptoms
- Constitutional symptoms
- Use of drugs causing lymphadenopathy
- Travel to endemic areas
- Occupational risk (e.g. Fishermen, slaughterhouse workers, hunters, trappers)
- High risk behavior or high risk sexual behaviors (e.g. I.V drug abuse, multiple partners)
Physical Examination
- Patients with lymphadenopathy may have a pale or normal appearance.
- Physical examination may be remarkable for:
Vitals
- Temperature
- Rapid (e.g. acute infections)
Skin
- Rash may be present
- Color change (indicative of inflammation)
- Skin fistula draining pus may be present
- Ulcers
Head
Palpating Anterior Cervical Lymph Nodes
Lymph nodes should be examined in the following order:[1][2]
Characteristics to be noted while palpating lymph nodes:[2]
- Size
- Pain/ tenderness
- Increased tenderness (e.g infected lymph nodes)
- Consistency
- Matting
Gallery
-
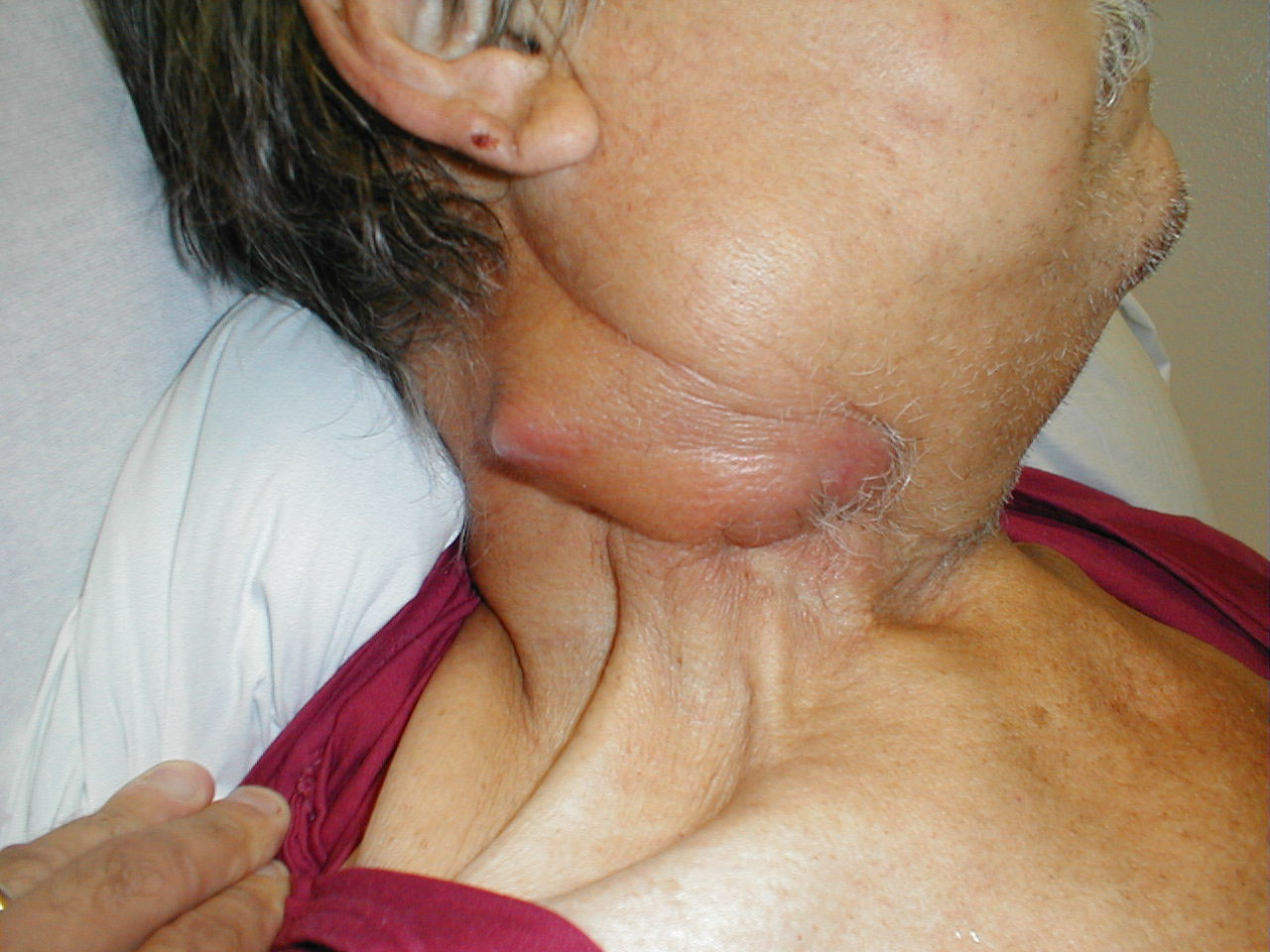
Cervical adenopathy: massive right side cervical adenopathy and facial asymmetry due to metastatic, intraoral squamous cell cancer. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
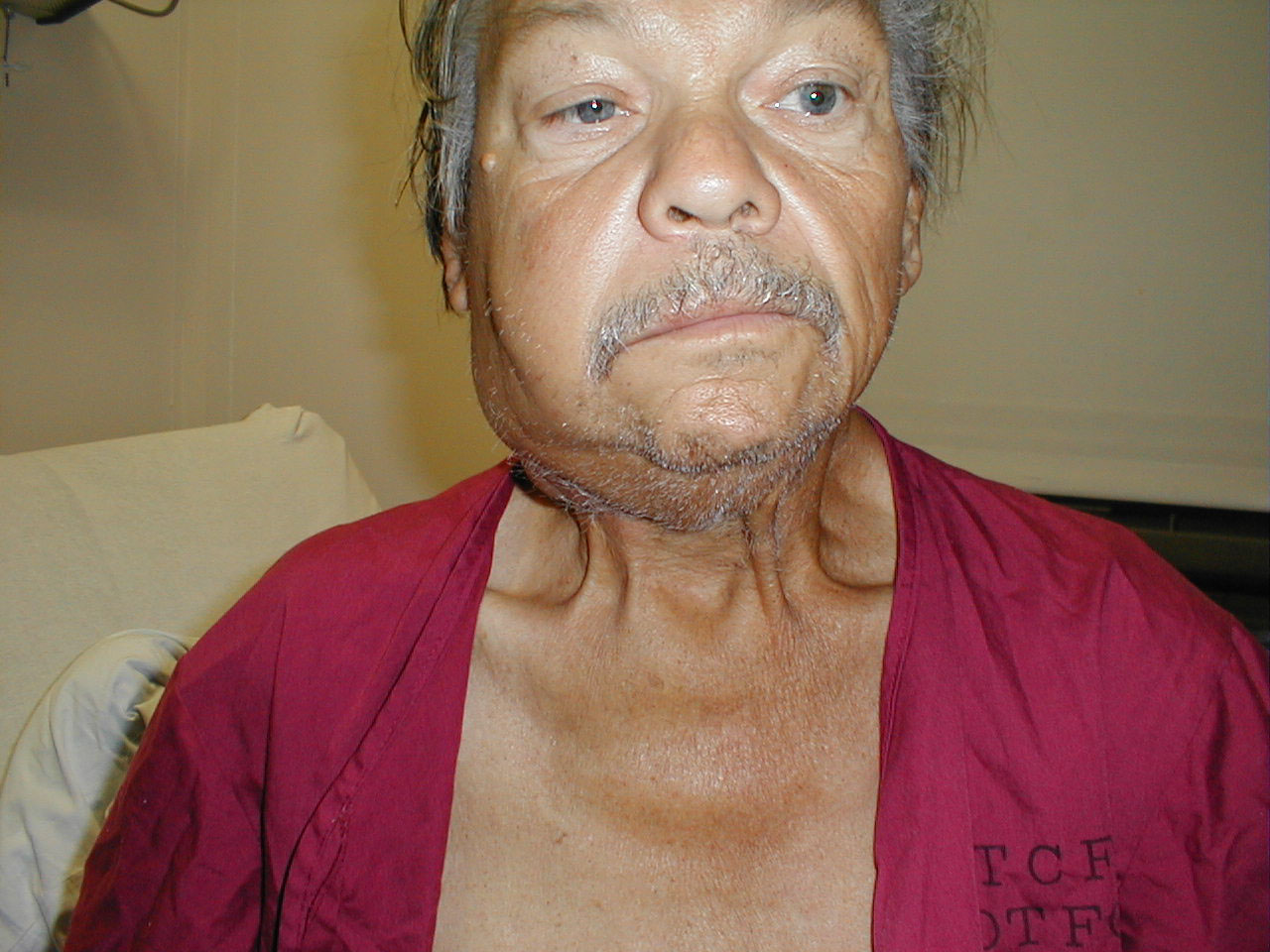
Cervical adenopathy: massive right side cervical adenopathy and facial asymmetry due to metastatic, intraoral squamous cell cancer. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
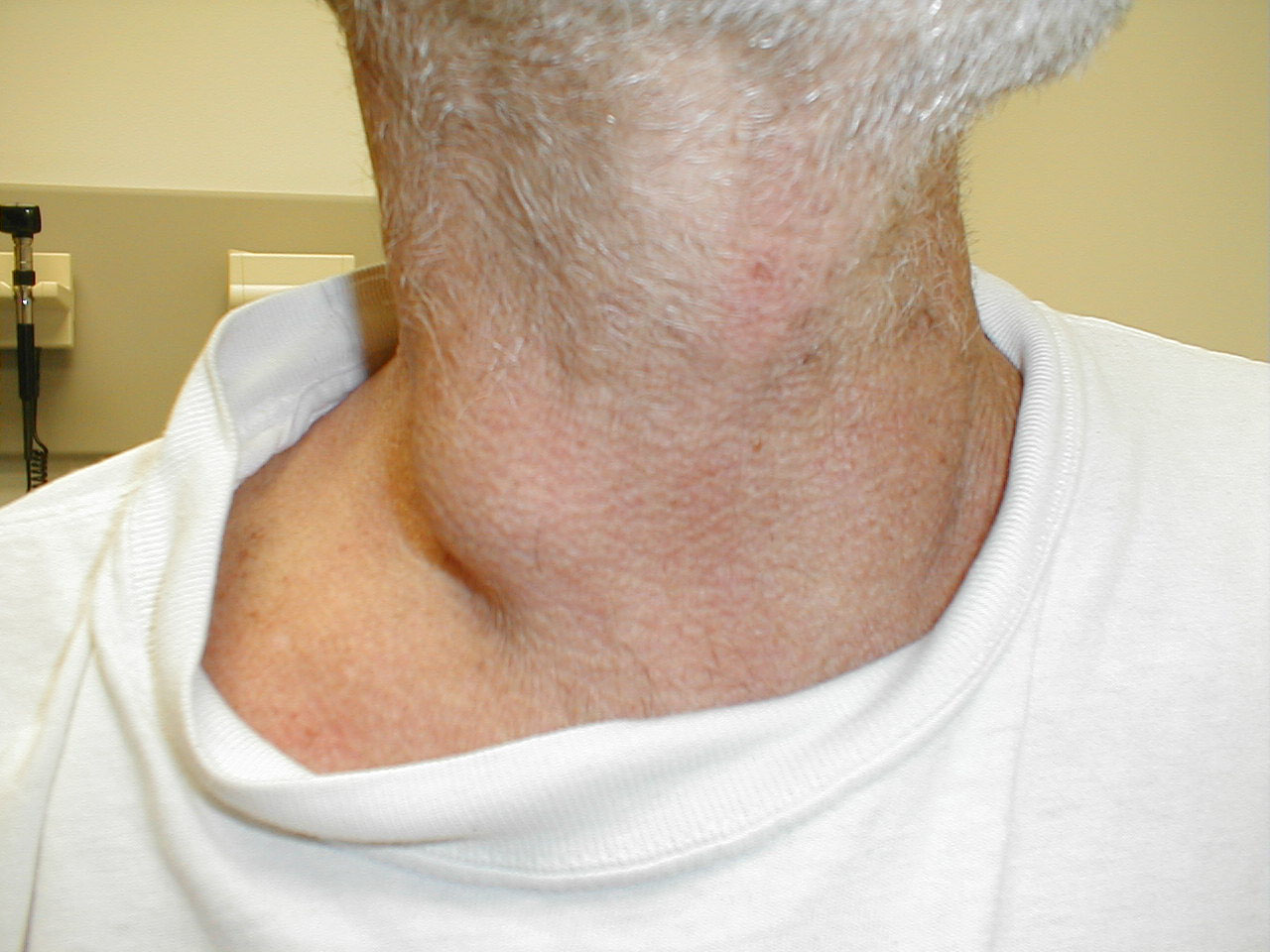
Cervical adenopathy: large right anterior cervical lymph node. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
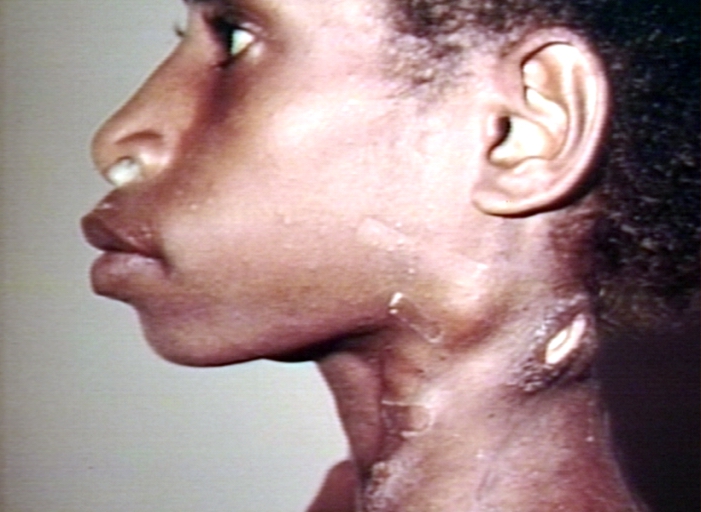
Cervical lymphadenopathy. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
Cervical Adenopathy: multiple right sided cervical lymph nodes. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
Laboratory Findings
Complete Blood Count
- Elevated lactate dehydrogenase (LDH)
- Mild neutropenia
- Leukocytosis
- Elevated markers of inflammation and acute phase reactants (e.g. ESR, C-reactive protein, ferritin)
Imaging Findings
Ultrasonography
- Increased lymph node size
CT
- The upper limit in size of a normal node varies with location.
PET/CT
- On PET/CT, lymphadenopathy can be further assessed via quantitation of FDG uptake, which is a surrogate of metabolic activity. Infectious, inflammatory, and neoplastic processes will show high FDG avidity on PET/CT. PET/CT is particularly useful for assessing response of lymph nodes to systemic chemotherapy.
MRI
- MRI is the most anatomically precise test for assessing lymphadenopathy. MRI is particularly useful for intraabdominal lymphadenopathy, which cannot be readily palpated via physical examination. MRI is more expensive than CT scan, so CT is preferred in general unless the clinical need for MRI arises.
Treatment
- There is no treatment for lymphadenopathy; the mainstay of therapy is treating the underlying condition.[1]
- Infectious lymphadenopathy responds well to prompt treatment with antibiotics, and usually leads to a complete recovery. However, it may take months, for swelling to disappear. The amount of time to recovery depends on the cause.[2]
- Neoplastic (malignant) lymphadenopathy usually responds well to systemic chemotherapy.
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 Mohseni S, Shojaiefard A, Khorgami Z, Alinejad S, Ghorbani A, Ghafouri A (2014). "Peripheral lymphadenopathy: approach and diagnostic tools". Iran J Med Sci. 39 (2 Suppl): 158–70. PMC 3993046. PMID 24753638.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 Lymph node enlargment. Wikipedia. https://en.wikipedia.org/wiki/Lymph_node Accessed on May 9, 2016
- ↑ Deschenes J, Seamone CD, Baines MG (1992). "Acquired ocular syphilis: diagnosis and treatment". Ann Ophthalmol. 24 (4): 134–8. PMID 1590633.
- ↑ 4.0 4.1 Lymph node enlargment. Radiopedia. http://radiopaedia.org/articles/lymph-node-enlargement Accessed on May 9, 2016
- ↑ van den Brekel MW, Castelijns JA (January 2000). "Imaging of lymph nodes in the neck". Semin Roentgenol. 35 (1): 42–53. PMID 10670052.
- ↑ Sumi M, Ohki M, Nakamura T (April 2001). "Comparison of sonography and CT for differentiating benign from malignant cervical lymph nodes in patients with squamous cell carcinoma of the head and neck". AJR Am J Roentgenol. 176 (4): 1019–24. doi:10.2214/ajr.176.4.1761019. PMID 11264102.