Linagliptin
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Vignesh Ponnusamy, M.B.B.S. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Linagliptin is a dipeptidyl peptidase-4 (DPP-4) inhibitor that is FDA approved for the {{{indicationType}}} of type 2 diabetes mellitus. Common adverse reactions include hypoglycemia and nasopharyngitis.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Type 2 Diabetes Mellitus
- Dosing Information
- TRADJENTA tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
- The recommended dose of TRADJENTA is 5 mg once daily.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Linagliptin in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Linagliptin in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding FDA-Labeled Use of Linagliptin in pediatric patients.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Linagliptin in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Linagliptin in pediatric patients.
Contraindications
- TRADJENTA is contraindicated in patients with a history of a hypersensitivity reaction to linagliptin, such as anaphylaxis, angioedema, exfoliative skin conditions, urticaria, or bronchial hyperreactivity.
Warnings
Precautions
- Pancreatitis
- There have been postmarketing reports of acute pancreatitis, including fatal pancreatitis, in patients taking TRADJENTA. Take careful notice of potential signs and symptoms of pancreatitis. If pancreatitis is suspected, promptly discontinue TRADJENTA and initiate appropriate management. It is unknown whether patients with a history of pancreatitis are at increased risk for the development of pancreatitis while using TRADJENTA.
- Use with Medications Known to Cause Hypoglycemia
- Insulin secretagogues and insulin are known to cause hypoglycemia. The use of TRADJENTA in combination with an insulin secretagogue (e.g., sulfonylurea) was associated with a higher rate of hypoglycemia compared with placebo in a clinical trial. The use of TRADJENTA in combination with insulin in subjects with severe renal impairment was associated with a higher rate of hypoglycemia. Therefore, a lower dose of the insulin secretagogue or insulin may be required to reduce the risk of hypoglycemia when used in combination with TRADJENTA.
- Hypersensitivity Reactions
- There have been postmarketing reports of serious hypersensitivity reactions in patients treated with TRADJENTA. These reactions include anaphylaxis, angioedema, and exfoliative skin conditions. Onset of these reactions occurred within the first 3 months after initiation of treatment with TRADJENTA, with some reports occurring after the first dose. If a serious hypersensitivity reaction is suspected, discontinue TRADJENTA, assess for other potential causes for the event, and institute alternative treatment for diabetes.
- Angioedema has also been reported with other dipeptidyl peptidase-4 (DPP-4) inhibitors. Use caution in a patient with a history of angioedema to another DPP-4 inhibitor because it is unknown whether such patients will be predisposed to angioedema with TRADJENTA.
- Macrovascular Outcomes
- There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with TRADJENTA tablets or any other antidiabetic drug
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
- The safety evaluation of TRADJENTA 5 mg once daily in patients with type 2 diabetes is based on 14 placebo-controlled trials, 1 active-controlled study, and one study in patients with severe renal impairment. In the 14 placebo-controlled studies, a total of 3625 patients were randomized and treated with TRADJENTA 5 mg daily and 2176 with placebo. The mean exposure in patients treated with TRADJENTA across studies was 29.6 weeks. The maximum follow-up was 78 weeks.
- TRADJENTA 5 mg once daily was studied as monotherapy in three placebo-controlled trials of 18 and 24 weeks’ duration and in five additional placebo-controlled studies lasting ≤18 weeks. The use of TRADJENTA in combination with other antihyperglycemic agents was studied in six placebo-controlled trials: two with metformin (12 and 24 weeks’ treatment duration); one with a sulfonylurea (18 weeks’ treatment duration); one with metformin and sulfonylurea (24 weeks’ treatment duration); one with pioglitazone (24 weeks’ treatment duration); and one with insulin (primary endpoint at 24 weeks).
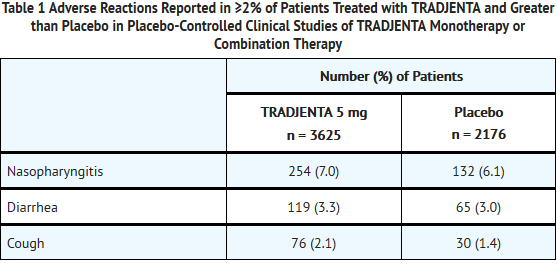
- In a pooled dataset of 14 placebo-controlled clinical trials, adverse reactions that occurred in ≥2% of patients receiving TRADJENTA (n = 3625) and more commonly than in patients given placebo (n = 2176), are shown in Table 1. The overall incidence of adverse events with TRADJENTA were similar to placebo.
- Rates for other adverse reactions for TRADJENTA 5 mg vs placebo when TRADJENTA was used in combination with specific anti-diabetic agents were: urinary tract infection (3.1% vs 0%) and hypertriglyceridemia (2.4% vs 0%) when TRADJENTA was used as add-on to sulfonylurea; hyperlipidemia (2.7% vs 0.8%) and weight increased (2.3% vs 0.8%) when TRADJENTA was used as add-on to pioglitazone; and constipation (2.1% vs 1%) when TRADJENTA was used as add-on to basal insulin therapy.
- Following 104 weeks’ treatment in a controlled study comparing TRADJENTA with glimepiride in which all patients were also receiving metformin, adverse reactions reported in ≥5% of patients treated with TRADJENTA (n = 776) and more frequently than in patients treated with a sulfonylurea (n = 775) were back pain (9.1% vs 8.4%), arthralgia (8.1% vs 6.1%), upper respiratory tract infection (8.0% vs 7.6%), headache (6.4% vs 5.2%), cough (6.1% vs 4.9%), and pain in extremity (5.3% vs 3.9%).
- Other adverse reactions reported in clinical studies with treatment of TRADJENTA were hypersensitivity (e.g., urticaria, angioedema, localized skin exfoliation, or bronchial hyperreactivity), and myalgia. In the clinical trial program, pancreatitis was reported in 15.2 cases per 10,000 patient year exposure while being treated with TRADJENTA compared with 3.7 cases per 10,000 patient year exposure while being treated with comparator (placebo and active comparator, sulfonylurea). Three additional cases of pancreatitis were reported following the last administered dose of linagliptin.
- Hypoglycemia
- In the placebo-controlled studies, 199 (6.6%) of the total 2994 patients treated with TRADJENTA 5 mg reported hypoglycemia compared to 56 patients (3.6%) of 1546 placebo-treated patients. The incidence of hypoglycemia was similar to placebo when TRADJENTA was administered as monotherapy or in combination with metformin, or with pioglitazone. When TRADJENTA was administered in combination with metformin and a sulfonylurea, 181 of 792 (22.9%) patients reported hypoglycemia compared with 39 of 263 (14.8%) patients administered placebo in combination with metformin and a sulfonylurea. Adverse reactions of hypoglycemia were based on all reports of hypoglycemia. A concurrent glucose measurement was not required or was normal in some patients. Therefore, it is not possible to conclusively determine that all these reports reflect true hypoglycemia.
- In the study of patients receiving TRADJENTA as add-on therapy to a stable dose of insulin for up to 52 weeks (n=1261), no significant difference in the incidence of investigator reported hypoglycemia, defined as all symptomatic or asymptomatic episodes with a self measured blood glucose ≤70 mg/dL, was noted between the TRADJENTA- (31.4%) and placebo- (32.9%) treated groups. During the same time period, severe hypoglycemic events, defined as requiring the assistance of another person to actively administer carbohydrate, glucagon or other resuscitative actions, were reported in 11 (1.7%) of TRADJENTA treated patients and 7 (1.1%) of placebo treated patients. Events that were considered life-threatening or required hospitalization were reported in 3 (0.5%) patients on TRADJENTA and 1 (0.2%) on placebo.
- Use in Renal Impairment
- ADJENTA was compared to placebo as add-on to pre-existing antidiabetic therapy over 52 weeks in 133 patients with severe renal impairment (estimated GFR <;<30 mL/min). For the initial 12 weeks of the study, background antidiabetic therapy was kept stable and included insulin, sulfonylurea, glinides, and pioglitazone. For the remainder of the trial, dose adjustments in antidiabetic background therapy were allowed.
- In general, the incidence of adverse events including severe hypoglycemia was similar to those reported in other TRADJENTA trials. The observed incidence of hypoglycemia was higher (TRADJENTA, 63% compared to placebo, 49%) due to an increase in asymptomatic hypoglycemic events especially during the first 12 weeks when background glycemic therapies were kept stable. Ten TRADJENTA-treated patients (15%) and 11 placebo-treated patients (17%) reported at least one episode of confirmed symptomatic hypoglycemia (accompanying finger stick glucose ≤54 mg/dL). During the same time period, severe hypoglycemic events, defined as an event requiring the assistance of another person to actively administer carbohydrate, glucagon or other resuscitative actions, were reported in 3 (4.4%) TRADJENTA-treated patients and 3 (4.6%) placebo-treated patients. Events that were considered life-threatening or required hospitalization were reported in 2 (2.9%) patients on TRADJENTA and 1 (1.5%) patient on placebo.
- Renal function as measured by mean eGFR and creatinine clearance did not change over 52 weeks’ treatment compared to placebo.
Postmarketing Experience
- Additional adverse reactions have been identified during postapproval use of TRADJENTA. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Acute pancreatitis, including fatal pancreatitis.
- Hypersensitivity reactions including anaphylaxis, angioedema, and exfoliative skin conditions.
- Rash.
Drug Interactions
- Inducers of P-glycoprotein or CYP3A4 Enzymes
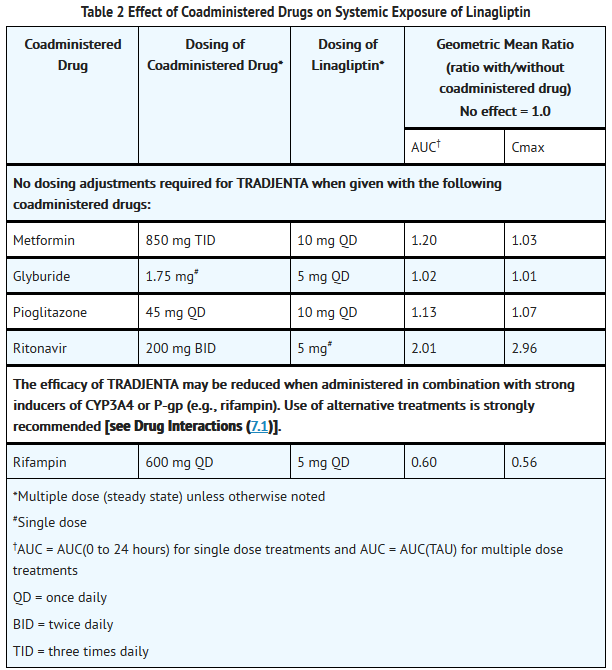
- Rifampin decreased linagliptin exposure, suggesting that the efficacy of TRADJENTA may be reduced when administered in combination with a strong P-gp or CYP3A4 inducer. Therefore, use of alternative treatments is strongly recommended when linagliptin is to be administered with a strong P-gp or CYP3A4 inducer.
Use in Specific Populations
Pregnancy
- Pregnancy Category B
- Reproduction studies have been performed in rats and rabbits. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
- Linagliptin administered during the period of organogenesis was not teratogenic at doses up to 30 mg/kg in the rat and 150 mg/kg in the rabbit, or approximately 49 and 1943 times the clinical dose based on AUC exposure. Doses of linagliptin causing maternal toxicity in the rat and the rabbit also caused developmental delays in skeletal ossification and slightly increased embryofetal loss in the rat (1000 times the clinical dose) and increased fetal resorptions and visceral and skeletal variations in the rabbit (1943 times the clinical dose).
- Linagliptin administered to female rats from gestation day 6 to lactation day 21 resulted in decreased body weight and delays in physical and behavioral development in male and female offspring at maternally toxic doses (exposures >1000 times the clinical dose). No functional, behavioral, or reproductive toxicity was observed in offspring of rats exposed to 49 times the clinical dose.
- Linagliptin crossed the placenta into the fetus following oral dosing in pregnant rats and rabbits.
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Linagliptin in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Linagliptin during labor and delivery.
Nursing Mothers
- Available animal data have shown excretion of linagliptin in milk at a milk-to-plasma ratio of 4:1. It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when TRADJENTA is administered to a nursing woman.
Pediatric Use
- Safety and effectiveness of TRADJENTA in pediatric patients under 18 years of age have not been established.
Geriatic Use
- There were 4040 type 2 diabetes patients treated with linagliptin 5 mg from 15 clinical trials of TRADJENTA; 1085 (27%) were 65 years and over, while 131 (3%) were 75 years and over. Of these patients, 2566 were enrolled in 12 double-blind placebo-controlled studies; 591 (23%) were 65 years and over, while 82 (3%) were 75 years and over. No overall differences in safety or effectiveness were observed between patients 65 years and over and younger patients. Therefore, no dose adjustment is recommended in the elderly population. While clinical studies of linagliptin have not identified differences in response between the elderly and younger patients, greater sensitivity of some older individuals cannot be ruled out.
Gender
There is no FDA guidance on the use of Linagliptin with respect to specific gender populations.
Race
There is no FDA guidance on the use of Linagliptin with respect to specific racial populations.
Renal Impairment
- No dose adjustment is recommended for patients with renal impairment.
Hepatic Impairment
- No dose adjustment is recommended for patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Linagliptin in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Linagliptin in patients who are immunocompromised.
Administration and Monitoring
Administration
- Oral
Monitoring
There is limited information regarding Monitoring of Linagliptin in the drug label.
IV Compatibility
There is limited information regarding IV Compatibility of Linagliptin in the drug label.
Overdosage
Acute Overdose
Signs and Symptoms
- During controlled clinical trials in healthy subjects, with single doses of up to 600 mg of TRADJENTA (equivalent to 120 times the recommended daily dose) there were no dose-related clinical adverse drug reactions. There is no experience with doses above 600 mg in humans.
Management
- In the event of an overdose with TRADJENTA, contact the Poison Control Center. Employ the usual supportive measures (e.g., remove unabsorbed material from the gastrointestinal tract, employ clinical monitoring, and institute supportive treatment) as dictated by the patient’s clinical status. Removal of linagliptin by hemodialysis or peritoneal dialysis is unlikely.
Chronic Overdose
There is limited information regarding Chronic Overdose of Linagliptin in the drug label.
Pharmacology

| |
Linagliptin
| |
| Systematic (IUPAC) name | |
| 8-[(3R)-3-aminopiperidin-1-yl]-7-(but-2-yn-1-yl)-3- methyl-1-[(4-methylquinazolin-2-yl)methyl]-3,7-dihydro-1H-purine-2,6-dione | |
| Identifiers | |
| CAS number | |
| ATC code | A10 |
| PubChem | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | 472.54 g/mol |
| SMILES | & |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | ? |
| Excretion | ? |
| Therapeutic considerations | |
| Licence data |
, |
| Pregnancy cat. |
B(US) |
| Legal status |
[[Prescription drug|Template:Unicode-only]](US) |
| Routes | Oral |
Mechanism of Action
- Linagliptin is an inhibitor of DPP-4, an enzyme that degrades the incretin hormones glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP). Thus, linagliptin increases the concentrations of active incretin hormones, stimulating the release of insulin in a glucose-dependent manner and decreasing the levels of glucagon in the circulation. Both incretin hormones are involved in the physiological regulation of glucose homeostasis. Incretin hormones are secreted at a low basal level throughout the day and levels rise immediately after meal intake. GLP-1 and GIP increase insulin biosynthesis and secretion from pancreatic beta-cells in the presence of normal and elevated blood glucose levels. Furthermore, GLP-1 also reduces glucagon secretion from pancreatic alpha-cells, resulting in a reduction in hepatic glucose output.
Structure
- TRADJENTA (linagliptin) tablets contain, as the active ingredient, an orally-active inhibitor of the dipeptidyl peptidase-4 (DPP-4) enzyme.
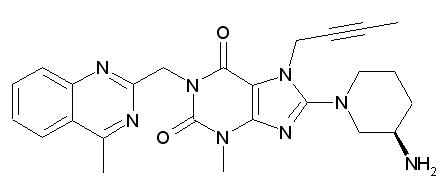
- Linagliptin is described chemically as 1H-Purine-2,6-dione, 8-[(3R)-3-amino-1-piperidinyl]-7-(2-butyn-1-yl)-3,7-dihydro-3-methyl-1-[(4-methyl-2-quinazolinyl)methyl]-
- The empirical formula is C25H28N8O2 and the molecular weight is 472.54 g/mol. The structural formula is:
- Linagliptin is a white to yellowish, not or only slightly hygroscopic solid substance. It is very slightly soluble in water (0.9 mg/mL). Linagliptin is soluble in methanol (ca. 60 mg/mL), sparingly soluble in ethanol (ca. 10 mg/mL), very slightly soluble in isopropanol (<;<1 mg/mL), and very slightly soluble in acetone (ca. 1 mg/mL).
- Each film-coated tablet of TRADJENTA contains 5 mg of linagliptin free base and the following inactive ingredients: mannitol, pregelatinized starch, corn starch, copovidone, and magnesium stearate. In addition, the film coating contains the following inactive ingredients: hypromellose, titanium dioxide, talc, polyethylene glycol, and red ferric oxide.
Pharmacodynamics
- Linagliptin binds to DPP-4 in a reversible manner and thus increases the concentrations of incretin hormones. Linagliptin glucose dependently increases insulin secretion and lowers glucagon secretion, thus resulting in better regulation of glucose homeostasis. Linagliptin binds selectively to DPP-4, and selectively inhibits DPP-4 but not DPP-8 or DPP-9 activity in vitro at concentrations approximating therapeutic exposures.
- Cardiac Electrophysiology
- In a randomized, placebo-controlled, active-comparator, 4-way crossover study, 36 healthy subjects were administered a single oral dose of linagliptin 5 mg, linagliptin 100 mg (20 times the recommended dose), moxifloxacin, and placebo. No increase in QTc was observed with either the recommended dose of 5 mg or the 100-mg dose. At the 100-mg dose, peak linagliptin plasma concentrations were approximately 38-fold higher than the peak concentrations following a 5-mg dose.
Pharmacokinetics
- The pharmacokinetics of linagliptin has been characterized in healthy subjects and patients with type 2 diabetes. After oral administration of a single 5-mg dose to healthy subjects, peak plasma concentrations of linagliptin occurred at approximately 1.5 hours post dose (Tmax); the mean plasma area under the curve (AUC) was 139 nmol*h/L and maximum concentration (Cmax) was 8.9 nmol/L.
- Plasma concentrations of linagliptin decline in at least a biphasic manner with a long terminal half-life (>100 hours), related to the saturable binding of linagliptin to DPP-4. The prolonged elimination phase does not contribute to the accumulation of the drug. The effective half-life for accumulation of linagliptin, as determined from oral administration of multiple doses of linagliptin 5 mg, is approximately 12 hours. After once-daily dosing, steady-state plasma concentrations of linagliptin 5 mg are reached by the third dose, and Cmax and AUC increased by a factor of 1.3 at steady state compared with the first dose. The intra-subject and inter-subject coefficients of variation for linagliptin AUC were small (12.6% and 28.5%, respectively). Plasma AUC of linagliptin increased in a less than dose-proportional manner in the dose range of 1 to 10 mg. The pharmacokinetics of linagliptin is similar in healthy subjects and in patients with type 2 diabetes.
- Absorption
- The absolute bioavailability of linagliptin is approximately 30%. High-fat meal reduced Cmax by 15% and increased AUC by 4%; this effect is not clinically relevant. TRADJENTA may be administered with or without food.
- Distribution
- The mean apparent volume of distribution at steady state following a single intravenous dose of linagliptin 5 mg to healthy subjects is approximately 1110 L, indicating that linagliptin extensively distributes to the tissues. Plasma protein binding of linagliptin is concentration-dependent, decreasing from about 99% at 1 nmol/L to 75%-89% at ≥30 nmol/L, reflecting saturation of binding to DPP-4 with increasing concentration of linagliptin. At high concentrations, where DPP-4 is fully saturated, 70% to 80% of linagliptin remains bound to plasma proteins and 20% to 30% is unbound in plasma. Plasma binding is not altered in patients with renal or hepatic impairment.
- Metabolism
- Following oral administration, the majority (about 90%) of linagliptin is excreted unchanged, indicating that metabolism represents a minor elimination pathway. A small fraction of absorbed linagliptin is metabolized to a pharmacologically inactive metabolite, which shows a steady-state exposure of 13.3% relative to linagliptin.
- Excretion
- Following administration of an oral [14C]-linagliptin dose to healthy subjects, approximately 85% of the administered radioactivity was eliminated via the enterohepatic system (80%) or urine (5%) within 4 days of dosing. Renal clearance at steady state was approximately 70 mL/min.
- Specific Populations
- Renal Impairment
- An open-label pharmacokinetic study evaluated the pharmacokinetics of linagliptin 5 mg in male and female patients with varying degrees of chronic renal impairment. The study included 6 healthy subjects with normal renal function (creatinine clearance [CrCl] ≥80 mL/min), 6 patients with mild renal impairment (CrCl 50 to <80 mL/min), 6 patients with moderate renal impairment (CrCl 30 to <50 mL/min), 10 patients with type 2 diabetes mellitus and severe renal impairment (CrCl <30 mL/min), and 11 patients with type 2 diabetes mellitus and normal renal function. Creatinine clearance was measured by 24-hour urinary creatinine clearance measurements or estimated from serum creatinine based on the Cockcroft-Gault formula.
- Under steady-state conditions, linagliptin exposure in patients with mild renal impairment was comparable to healthy subjects.
- In patients with moderate renal impairment under steady-state conditions, mean exposure of linagliptin increased (AUCτ,ss by 71% and Cmax by 46%) compared with healthy subjects. This increase was not associated with a prolonged accumulation half-life, terminal half-life, or an increased accumulation factor. Renal excretion of linagliptin was below 5% of the administered dose and was not affected by decreased renal function.
- Patients with type 2 diabetes mellitus and severe renal impairment showed steady-state exposure approximately 40% higher than that of patients with type 2 diabetes mellitus and normal renal function (increase in AUCτ,ss by 42% and Cmax by 35%). For both type 2 diabetes mellitus groups, renal excretion was below 7% of the administered dose.
- These findings were further supported by the results of population pharmacokinetic analyses.
- Hepatic Impairment
- In patients with mild hepatic impairment (Child-Pugh class A), steady-state exposure (AUCτ,ss) of linagliptin was approximately 25% lower and Cmax,ss was approximately 36% lower than in healthy subjects. In patients with moderate hepatic impairment (Child-Pugh class B), AUCss of linagliptin was about 14% lower and Cmax,ss was approximately 8% lower than in healthy subjects. Patients with severe hepatic impairment (Child-Pugh class C) had comparable exposure of linagliptin in terms of AUC0-24 and approximately 23% lower Cmax compared with healthy subjects. Reductions in the pharmacokinetic parameters seen in patients with hepatic impairment did not result in reductions in DPP-4 inhibition.
- Body Mass Index (BMI)/Weight
- No dose adjustment is necessary based on BMI/weight. BMI/weight had no clinically meaningful effect on the pharmacokinetics of linagliptin based on a population pharmacokinetic analysis.
- Gender
- No dose adjustment is necessary based on gender. Gender had no clinically meaningful effect on the pharmacokinetics of linagliptin based on a population pharmacokinetic analysis.
- Geriatric
- Age did not have a clinically meaningful impact on the pharmacokinetics of linagliptin based on a population pharmacokinetic analysis.
- Pediatric
- Studies characterizing the pharmacokinetics of linagliptin in pediatric patients have not yet been performed.
- Race
- No dose adjustment is necessary based on race. Race had no clinically meaningful effect on the pharmacokinetics of linagliptin based on available pharmacokinetic data, including subjects of White, Hispanic, Black, and Asian racial groups.
- Drug Interactions
- In vitro Assessment of Drug Interactions
- Linagliptin is a weak to moderate inhibitor of CYP isozyme CYP3A4, but does not inhibit other CYP isozymes and is not an inducer of CYP isozymes, including CYP1A2, 2A6, 2B6, 2C8, 2C9, 2C19, 2D6, 2E1, and 4A11.
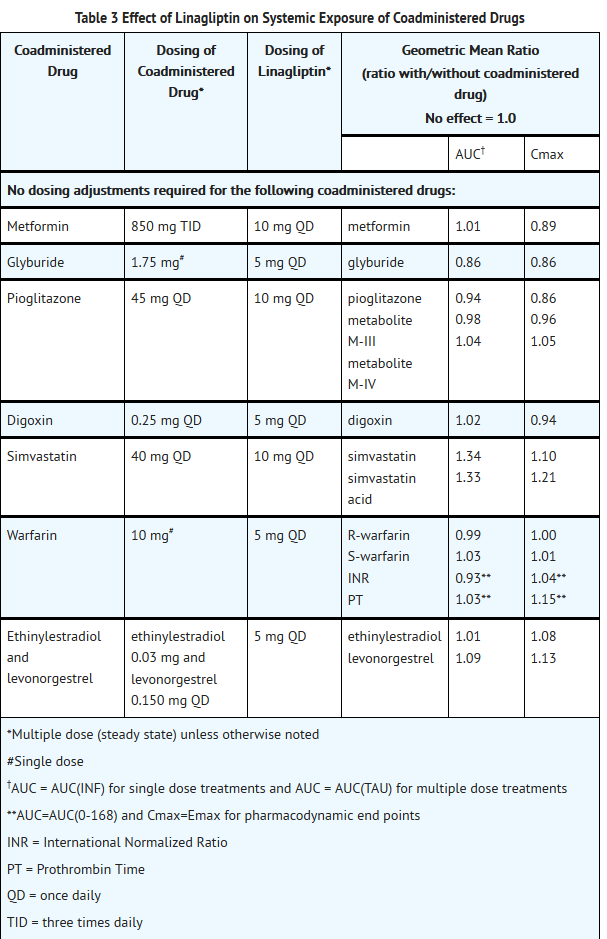
- Linagliptin is a P-glycoprotein (P-gp) substrate, and inhibits P-gp mediated transport of digoxin at high concentrations. Based on these results and in vivo drug interaction studies, linagliptin is considered unlikely to cause interactions with other P-gp substrates at therapeutic concentrations.
- In vivo Assessment of Drug Interactions
- Strong inducers of CYP3A4 or P-gp (e.g., rifampin) decrease exposure to linagliptin to subtherapeutic and likely ineffective concentrations. For patients requiring use of such drugs, an alternative to linagliptin is strongly recommended. In vivo studies indicated evidence of a low propensity for causing drug interactions with substrates of CYP3A4, CYP2C9, CYP2C8, P-gp and organic cationic transporter (OCT). No dose adjustment of TRADJENTA is recommended based on results of the described pharmacokinetic studies.
Nonclinical Toxicology
- Linagliptin did not increase the incidence of tumors in male and female rats in a 2-year study at doses of 6, 18, and 60 mg/kg. The highest dose of 60 mg/kg is approximately 418 times the clinical dose of 5 mg/day based on AUC exposure. Linagliptin did not increase the incidence of tumors in mice in a 2-year study at doses up to 80 mg/kg (males) and 25 mg/kg (females), or approximately 35- and 270-times the clinical dose based on AUC exposure. Higher doses of linagliptin in female mice (80 mg/kg) increased the incidence of lymphoma at approximately 215-times the clinical dose based on AUC exposure.
- Linagliptin was not mutagenic or clastogenic with or without metabolic activation in the Ames bacterial mutagenicity assay, a chromosomal aberration test in human lymphocytes, and an in vivo micronucleus assay.
- In fertility studies in rats, linagliptin had no adverse effects on early embryonic development, mating, fertility, or bearing live young up to the highest dose of 240 mg/kg (approximately 943-times the clinical dose based on AUC exposure).
Clinical Studies
- TRADJENTA has been studied as monotherapy and in combination with metformin, glimepiride, pioglitazone, and insulin.
- A total of 3648 patients with type 2 diabetes were randomized and exposed to linagliptin for at least 12 weeks in 10 double-blind, placebo-controlled clinical efficacy studies evaluating the effects of TRADJENTA on glycemic control. The overall ethnic/racial distribution in these studies was 69% White, 29% Asian, and 2.5% Black, and included 16% Hispanic/Latino patients. Fifty two percent of patients were male. Patients had an overall mean age of 57 years (range 20 to 91 years). In addition, an active (glimepiride)-controlled study of 104 weeks’ duration was conducted in 1551 patients with type 2 diabetes who had inadequate glycemic control on metformin, and a placebo-controlled study of 52 weeks’ duration was conducted in 133 patients with type 2 diabetes and severe chronic renal impairment (eGFR <30 mL/min).
- In patients with type 2 diabetes, treatment with TRADJENTA produced clinically significant improvements in hemoglobin A1c (A1C), fasting plasma glucose (FPG), and 2-hour post-prandial glucose (PPG) compared with placebo.
Monotherapy
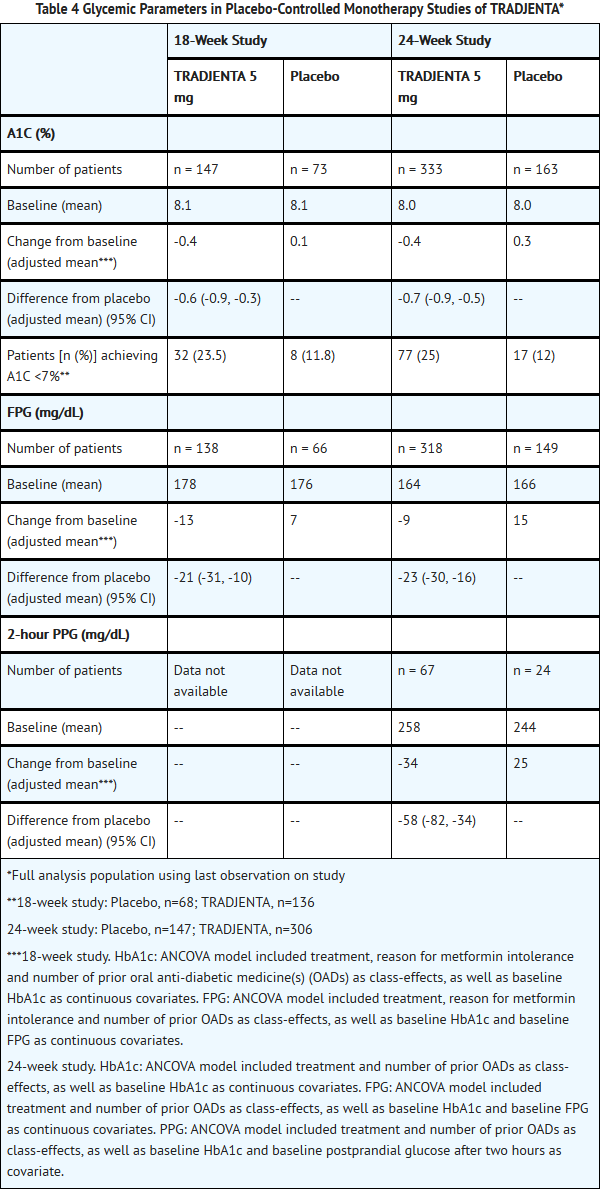
- A total of 730 patients with type 2 diabetes participated in 2 double-blind, placebo-controlled studies, one of 18 weeks’ and another of 24 weeks’ duration, to evaluate the efficacy and safety of TRADJENTA monotherapy. In both monotherapy studies, patients currently on an antihyperglycemic agent discontinued the agent and underwent a diet, exercise, and drug washout period of about 6 weeks that included an open-label placebo run-in during the last 2 weeks. Patients with inadequate glycemic control (A1C 7% to 10%) after the washout period were randomized; patients not currently on antihyperglycemic agents (off therapy for at least 8 weeks) with inadequate glycemic control (A1C 7% to 10%) were randomized after completing the 2-week, open-label, placebo run-in period. In the 18-week study, only patients ineligible for metformin were recruited. In the 18-week study, 76 patients were randomized to placebo and 151 to TRADJENTA 5 mg; in the 24-week study, 167 patients were randomized to placebo and 336 to TRADJENTA 5 mg. Patients who failed to meet specific glycemic goals during the 18-week study received rescue therapy with pioglitazone and/or insulin; metformin rescue therapy was used in the 24-week trial.
- Treatment with TRADJENTA 5 mg daily provided statistically significant improvements in A1C, FPG, and 2-hour PPG compared with placebo (Table 4). In the 18-week study, 12% of patients receiving TRADJENTA 5 mg and 18% who received placebo required rescue therapy. In the 24-week study, 10.2% of patients receiving TRADJENTA 5 mg and 20.9% of patients receiving placebo required rescue therapy. The improvement in A1C compared with placebo was not affected by gender, age, race, prior antihyperglycemic therapy, baseline BMI, or a standard index of insulin resistance (HOMA-IR). As is typical for trials of agents to treat type 2 diabetes, the mean reduction in A1C with TRADJENTA appears to be related to the degree of A1C elevation at baseline. In these 18- and 24-week studies, the changes from baseline in A1C were -0.4% and -0.4%, respectively, for those given TRADJENTA, and 0.1% and 0.3%, respectively, for those given placebo. Change from baseline in body weight did not differ significantly between the groups.
Combination Therapy
- Add-on Combination Therapy with Metformin
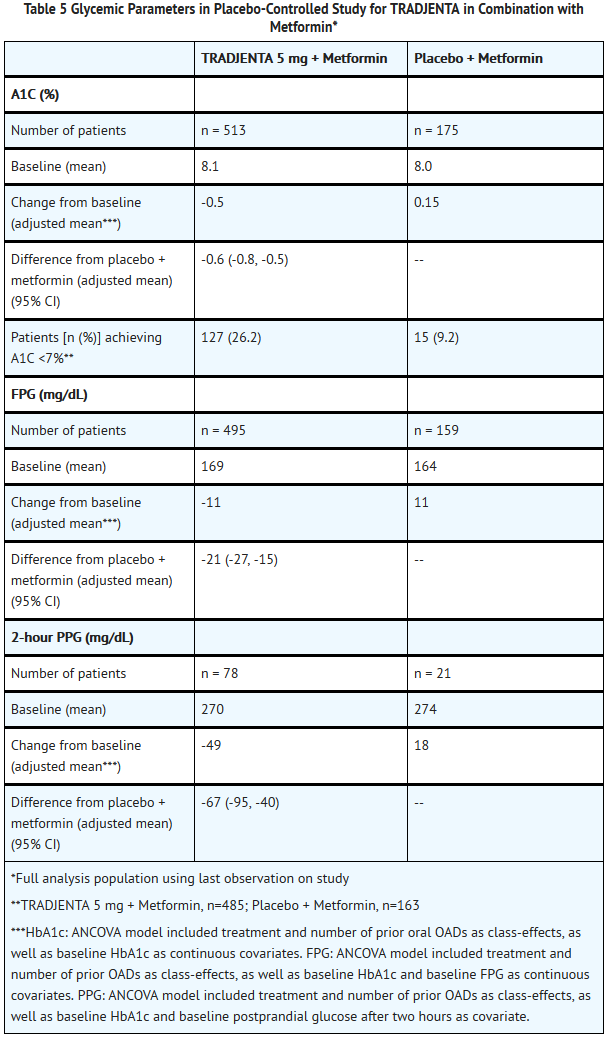
- A total of 701 patients with type 2 diabetes participated in a 24-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of TRADJENTA in combination with metformin. Patients already on metformin (n = 491) at a dose of at least 1500 mg per day were randomized after completing a 2-week, open-label, placebo run-in period. Patients on metformin and another antihyperglycemic agent (n = 207) were randomized after a run-in period of approximately 6 weeks on metformin (at a dose of at least 1500 mg per day) in monotherapy. Patients were randomized to the addition of either TRADJENTA 5 mg or placebo, administered once daily. Patients who failed to meet specific glycemic goals during the studies were treated with glimepiride rescue.
- In combination with metformin, TRADJENTA provided statistically significant improvements in A1C, FPG, and 2-hour PPG compared with placebo (Table 5). Rescue glycemic therapy was used in 7.8% of patients treated with TRADJENTA 5 mg and in 18.9% of patients treated with placebo. A similar decrease in body weight was observed for both treatment groups.
Initial Combination Therapy with Metformin
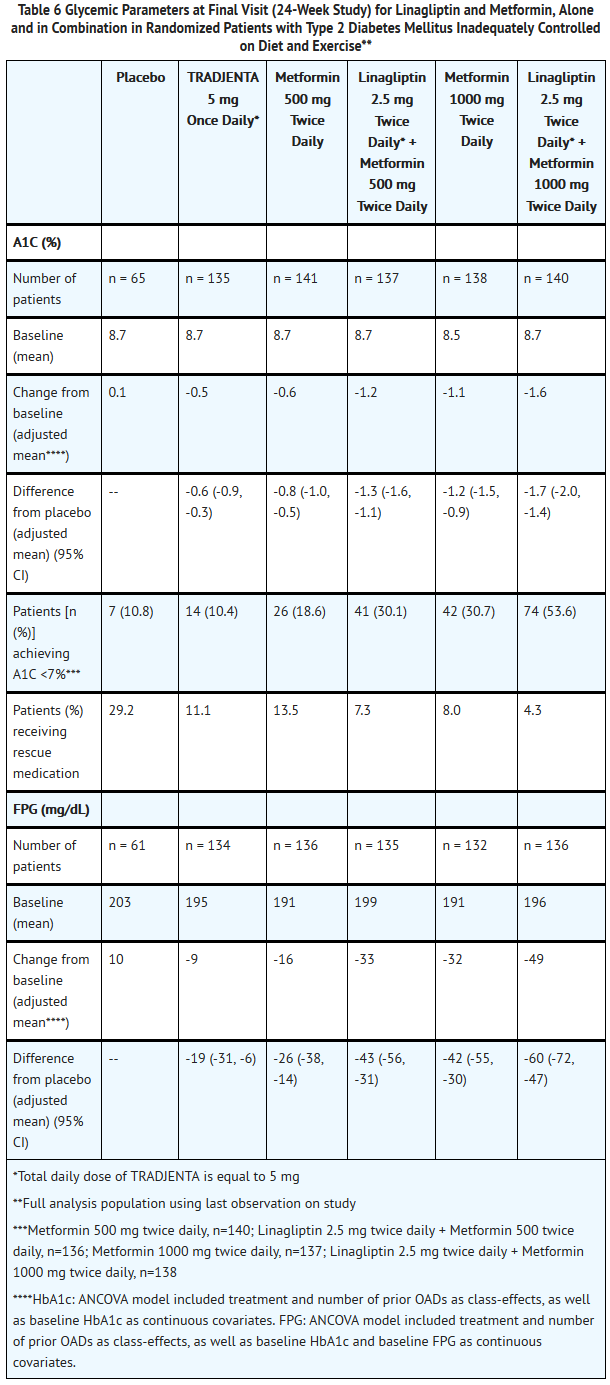
- A total of 791 patients with type 2 diabetes mellitus and inadequate glycemic control on diet and exercise participated in the 24-week, randomized, double-blind, portion of this placebo-controlled factorial study designed to assess the efficacy of TRADJENTA as initial therapy with metformin. Patients on an antihyperglycemic agent (52%) underwent a drug washout period of 4 weeks’ duration. After the washout period and after completing a 2-week single-blind placebo run-in period, patients with inadequate glycemic control (A1C ≥7.0% to ≤10.5%) were randomized. Patients with inadequate glycemic control (A1C ≥7.5% to <11.0%) not on antihyperglycemic agents at study entry (48%) immediately entered the 2-week, single-blind, placebo run-in period and then were randomized. Randomization was stratified by baseline A1C (<8.5% vs ≥8.5%) and use of a prior oral antidiabetic drug (none vs monotherapy). Patients were randomized in a 1:2:2:2:2:2 ratio to either placebo or one of 5 active-treatment arms. Approximately equal numbers of patients were randomized to receive initial therapy with 5 mg of TRADJENTA once daily, 500 mg or 1000 mg of metformin twice daily, or 2.5 mg of linagliptin twice daily in combination with 500 mg or 1000 mg of metformin twice daily. Patients who failed to meet specific glycemic goals during the study were treated with sulfonylurea, thiazolidinedione, or insulin rescue therapy.
- Initial therapy with the combination of linagliptin and metformin provided significant improvements in A1C and fasting plasma glucose (FPG) compared to placebo, to metformin alone, and to linagliptin alone (Table 6).
- The adjusted mean treatment difference in A1C from baseline to week 24 (LOCF) was -0.5% (95% CI -0.7, -0.3; p<0.0001) for linagliptin 2.5 mg/metformin 1000 mg twice daily compared to metformin 1000 twice daily; -1.1% (95% CI -1.4, -0.9; p<0.0001) for linagliptin 2.5 mg/metformin 1000 mg twice daily compared to TRADJENTA 5 mg once daily; -0.6% (95% CI -0.8, -0.4; p<0.0001) for linagliptin 2.5 mg/metformin 500 mg twice daily compared to metformin 500 mg twice daily; and -0.8% (95% CI -1.0, -0.6; p<0.0001) for linagliptin 2.5 mg/metformin 500 mg twice daily compared to TRADJENTA 5 mg once daily.
- Lipid effects were generally neutral. No meaningful change in body weight was noted in any of the 6 treatment groups.
Active-Controlled Study vs Glimepiride in Combination with Metformin
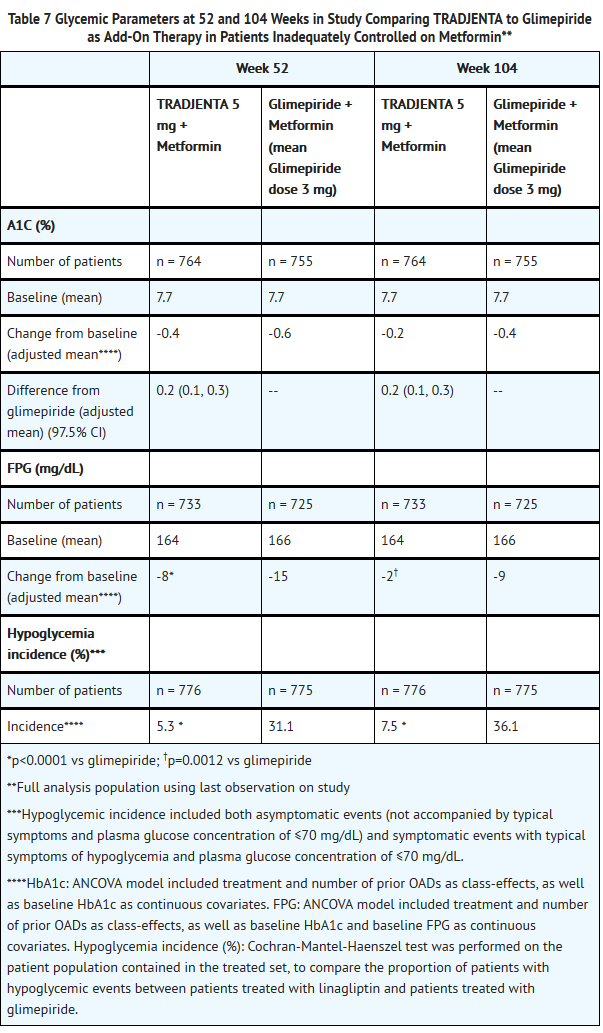
- The efficacy of TRADJENTA was evaluated in a 104-week, double-blind, glimepiride-controlled, non-inferiority study in patients with type 2 diabetes with insufficient glycemic control despite metformin therapy. Patients being treated with metformin only entered a run-in period of 2 weeks’ duration, whereas patients pretreated with metformin and one additional antihyperglycemic agent entered a run-in treatment period of 6 weeks’ duration with metformin monotherapy (dose of ≥1500 mg/day) and washout of the other agent. After an additional 2-week placebo run-in period, those with inadequate glycemic control (A1C 6.5% to 10%) were randomized 1:1 to the addition of TRADJENTA 5 mg once daily or glimepiride. Randomization was stratified by baseline HbA1c (<8.5% vs ≥8.5%), and the previous use of antidiabetic drugs (metformin alone vs metformin plus one other OAD). Patients receiving glimepiride were given an initial dose of 1 mg/day and then electively titrated over the next 12 weeks to a maximum dose of 4 mg/day as needed to optimize glycemic control. Thereafter, the glimepiride dose was to be kept constant, except for down-titration to prevent hypoglycemia.
- After 52 and 104 weeks, TRADJENTA and glimepiride both had reductions from baseline in A1C (52 weeks: -0.4% for TRADJENTA, -0.6% for glimepiride; 104 weeks: -0.2% for TRADJENTA, -0.4% for glimepiride) from a baseline mean of 7.7% (Table 7). The mean difference between groups in A1C change from baseline was 0.2% with 2-sided 97.5% confidence interval (0.1%, 0.3%) for the intent-to-treat population using last observation carried forward. These results were consistent with the completers analysis.
- Patients treated with linagliptin had a mean baseline body weight of 86 kg and were observed to have an adjusted mean decrease in body weight of 1.1 kg at 52 weeks and 1.4 kg at 104 weeks. Patients on glimepiride had a mean baseline body weight of 87 kg and were observed to have an adjusted mean increase from baseline in body weight of 1.4 kg at 52 weeks and 1.3 kg at 104 weeks (treatment difference p<0.0001 for both timepoints).
Add-On Combination Therapy with Pioglitazone
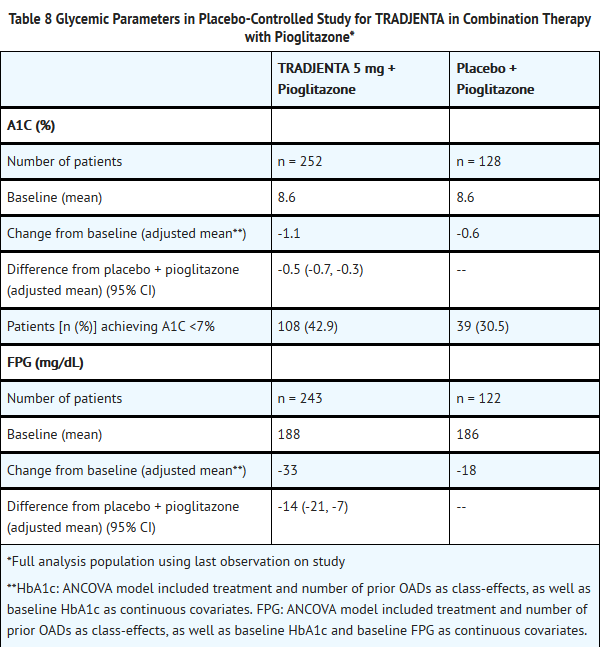
- A total of 389 patients with type 2 diabetes participated in a 24-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of TRADJENTA in combination with pioglitazone. Therapy was stopped in patients on oral antihyperglycemic therapy for a period of 6 weeks (4 weeks followed by a 2-week, open-label, placebo run-in period). Drug-naïve patients entered directly into the 2-week placebo run-in period. After the run-in period, patients were randomized to receive either TRADJENTA 5 mg or placebo, both in addition to pioglitazone 30 mg daily. Patients who failed to meet specific glycemic goals during the studies were treated with metformin rescue. Glycemic endpoints measured were A1C and FPG.
- In initial combination with pioglitazone 30 mg, TRADJENTA 5 mg provided statistically significant improvements in A1C and FPG compared to placebo with pioglitazone (Table 8). Rescue therapy was used in 7.9% of patients treated with TRADJENTA 5 mg/pioglitazone 30 mg and 14.1% of patients treated with placebo/pioglitazone 30 mg. Patient weight increased in both groups during the study with an adjusted mean change from baseline of 2.3 kg and 1.2 kg in the TRADJENTA 5 mg/pioglitazone 30 mg and placebo/pioglitazone 30 mg groups, respectively (p = 0.0141).
Add-On Combination with Sulfonylureas
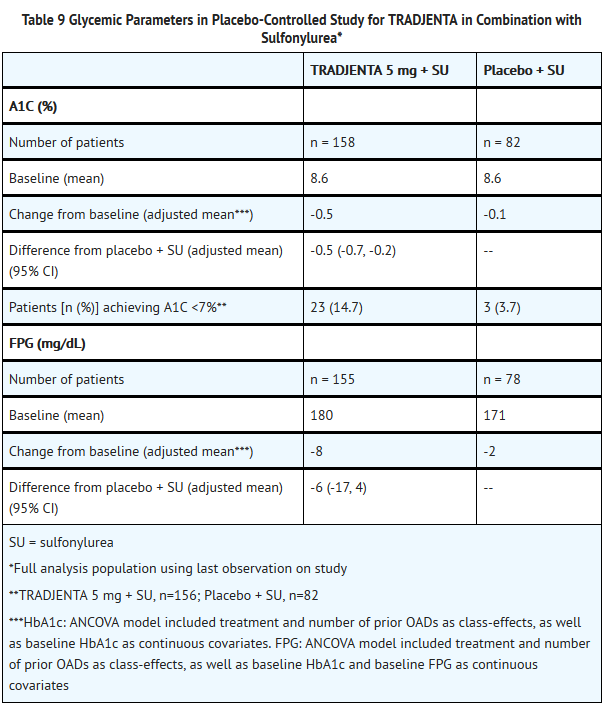
- A total of 245 patients with type 2 diabetes participated in an 18-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of TRADJENTA in combination with sulfonylurea (SU). Patients on sulfonylurea monotherapy (n = 142) were randomized after completing a 2-week, single-blind, placebo run-in period. Patients on a sulfonylurea plus one additional oral antihyperglycemic agent (n = 103) were randomized after a wash-out period of 4 weeks and a 2-week, single-blind, placebo run-in period. Patients were randomized to the addition of TRADJENTA 5 mg or to placebo, each administered once daily. Patients who failed to meet specific glycemic goals during the studies were treated with metformin rescue. Glycemic endpoints measured included A1C and FPG.
- In combination with a sulfonylurea, TRADJENTA provided statistically significant improvements in A1C compared with placebo following 18 weeks’ treatment; the improvements in FPG observed with TRADJENTA were not statistically significant compared with placebo (Table 9). Rescue therapy was used in 7.6% of patients treated with TRADJENTA 5 mg and 15.9% of patients treated with placebo. There was no significant difference between TRADJENTA and placebo in body weight.
Add-On Combination Therapy with Metformin and a Sulfonylurea
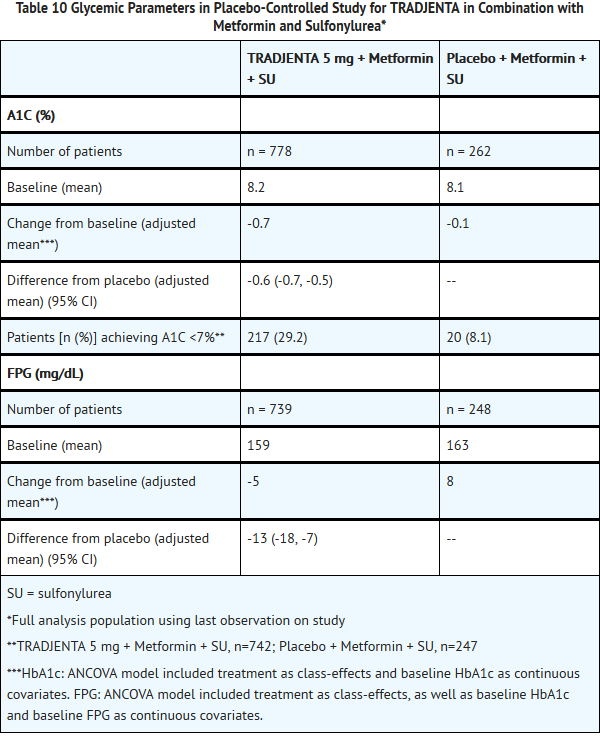
- A total of 1058 patients with type 2 diabetes participated in a 24-week, randomized, double-blind, placebo-controlled study designed to assess the efficacy of TRADJENTA in combination with a sulfonylurea and metformin. The most common sulfonylureas used by patients in the study were: glimepiride (31%), glibenclamide (26%), and gliclazide (26%, not available in the United States). Patients on a sulfonylurea and metformin were randomized to receive TRADJENTA 5 mg or placebo, each administered once daily. Patients who failed to meet specific glycemic goals during the study were treated with pioglitazone rescue. Glycemic endpoints measured included A1C and FPG.
- In combination with a sulfonylurea and metformin, TRADJENTA provided statistically significant improvements in A1C and FPG compared with placebo (Table 10). In the entire study population (patients on TRADJENTA in combination with sulfonylurea and metformin), a mean reduction from baseline relative to placebo in A1C of -0.6% and in FPG of -13 mg/dL was seen. Rescue therapy was used in 5.4% of patients treated with TRADJENTA 5 mg and in 13% of patients treated with placebo. Change from baseline in body weight did not differ significantly between the groups.
Add-On Combination Therapy with Insulin
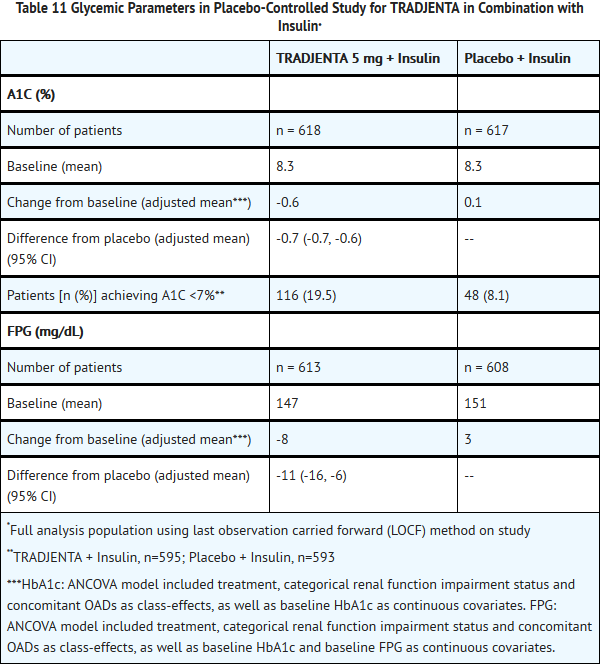
- A total of 1261 patients with type 2 diabetes inadequately controlled on basal insulin alone or basal insulin in combination with oral drugs participated in a randomized, double-blind placebo-controlled trial designed to evaluate the efficacy of TRADJENTA as add-on therapy to basal insulin over 24 weeks. Randomization was stratified by baseline HbA1c (<;<8.5% vs ≥8.5%), renal function impairment status (based on baseline eGFR), and concomitant use of oral antidiabetic drugs (none, metformin only, pioglitazone only, metformin + pioglitazone). Patients with a baseline A1C of >7% and <10% were included in the study including 709 patients with renal impairment (eGFR <90 mL/min), most of whom (n=575) were categorized as mild renal impairment (eGFR 60 to <90 mL/min). Patients entered a 2 week placebo run-in period on basal insulin (e.g., insulin glargine, insulin detemir, or NPH insulin) with or without metformin and/or pioglitazone background therapy. Following the run-in period, patients with inadequate glycemic control were randomized to the addition of either 5 mg of TRADJENTA or placebo, administered once daily. Patients were maintained on a stable dose of insulin prior to enrollment, during the run-in period, and during the first 24 weeks of treatment. Patients who failed to meet specific glycemic goals during the double-blind treatment period were rescued by increasing background insulin dose.
- TRADJENTA used in combination with insulin (with or without metformin and/or pioglitazone), provided statistically significant improvements in A1C and FPG compared to placebo (Table 11) after 24 weeks of treatment. The mean total daily insulin dose at baseline was 42 units for patients treated with TRADJENTA and 40 units for patients treated with placebo. Background baseline diabetes therapy included use of: insulin alone (16.1%), insulin combined with metformin only (75.5%), insulin combined with metformin and pioglitazone (7.4%), and insulin combined with pioglitazone only (1%). The mean change from baseline to Week 24 in the daily dose of insulin was +1.3 IU in the placebo group and +0.6 IU in the TRADJENTA group. The mean change in body weight from baseline to Week 24 was similar in the two treatment groups. The rate of hypoglycemia, defined as all symptomatic or asymptomatic episodes with a self measured blood glucose was also similar in both groups (21.4% TRADJENTA; 22.9% placebo) in the first 24 weeks of the study.
- The difference between treatment with linagliptin and placebo in terms of adjusted mean change from baseline in HbA1c after 24 weeks was comparable for patients with no renal impairment (eGFR ≥90 mL/min, n=539), with mild renal impairment (eGFR 60 to <90 mL/min, n= 565), or with moderate renal impairment (eGFR 30 to <60 mL/min, n=124).
Renal Impairment
- A total of 133 patients with type 2 diabetes participated in a 52 week, double-blind, randomized, placebo-controlled trial designed to evaluate the efficacy and safety of TRADJENTA in patients with both type 2 diabetes and severe chronic renal impairment. Participants with an estimated (based on the four variables modified diet in renal disease [MDRD] equation) GFR value of <;<30 mL/min were eligible to participate in the study. Randomization was stratified by baseline HbA1c (≤8% and >8%) and background antidiabetic therapy (insulin or any combination with insulin, SU or glinides as monotherapy and pioglitazone or any other antidiabetics excluding any other DPP-4 inhibitors). For the initial 12 weeks of the study, background antidiabetic therapy was kept stable and included insulin, sulfonylurea, glinides, and pioglitazone. For the remainder of the trial, dose adjustments in antidiabetic background therapy were allowed. At baseline in this trial, 62.5% of patients were receiving insulin alone as background diabetes therapy, and 12.5% were receiving sulfonylurea alone.
- After 12 weeks of treatment, TRADJENTA 5 mg provided statistically significant improvement in A1C compared to placebo, with an adjusted mean change of -0.6% compared to placebo (95% confidence interval -0.9, -0.3) based on the analysis using last observation carried forward (LOCF). With adjustments in antidiabetic background therapy after the initial 12 weeks, efficacy was maintained for 52 weeks, with an adjusted mean change from baseline in A1C of -0.7% compared to placebo (95% confidence interval -1.0, -0.4) based on analysis using LOCF.
How Supplied
- TRADJENTA tablets are available as light red, round, biconvex, bevel-edged, film-coated tablets containing 5 mg of linagliptin. TRADJENTA tablets are debossed with “D5” on one side and the Boehringer Ingelheim logo on the other side.
- They are supplied as follows:
- Bottles of 30 (NDC 0597-0140-30)
- Bottles of 90 (NDC 0597-0140-90)
- Cartons containing 10 blister cards of 10 tablets each (10 x 10) (NDC 0597-0140-61), institutional pack.
- If repackaging is required, dispense in a tight container as defined in USP.
- Storage
- Store at 25°C (77°F); excursions permitted to 15°-30°C (59°-86°F). Store in a safe place out of reach of children.
Storage
There is limited information regarding Linagliptin Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Linagliptin |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Linagliptin |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
Instructions
- Inform patients of the potential risks and benefits of TRADJENTA and of alternative modes of therapy. Also inform patients about the importance of adherence to dietary instructions, regular physical activity, periodic blood glucose monitoring and A1C testing, recognition and management of hypoglycemia and hyperglycemia, and assessment for diabetes complications. Advise patients to seek medical advice promptly during periods of stress such as fever, trauma, infection, or surgery, as medication requirements may change.
- Inform patients that acute pancreatitis has been reported during postmarketing use of TRADJENTA. Inform patients that persistent severe abdominal pain, sometimes radiating to the back, which may or may not be accompanied by vomiting, is the hallmark symptom of acute pancreatitis. Instruct patients to discontinue TRADJENTA promptly and contact their physician if persistent severe abdominal pain occurs.
- Inform patients that the incidence of hypoglycemia is increased when TRADJENTA is added to a sulfonylurea or insulin and that a lower dose of the sulfonylurea or insulin may be required to reduce the risk of hypoglycemia.
- Inform patients that serious allergic reactions, such as anaphylaxis, angioedema, and exfoliative skin conditions, have been reported during postmarketing use of TRADJENTA. If symptoms of allergic reactions (such as rash, skin flaking or peeling, urticaria, swelling of the skin, or swelling of the face, lips, tongue, and throat that may cause difficulty in breathing or swallowing) occur, patients must stop taking TRADJENTA and seek medical advice promptly.
- Instruct patients to take TRADJENTA only as prescribed. If a dose is missed, advise patients not to double their next dose.
- Instruct patients to read the Medication Guide before starting TRADJENTA therapy and to reread it each time the prescription is renewed. Instruct patients to inform their doctor or pharmacist if they develop any unusual symptom, or if any known symptom persists or worsens.
Laboratory Tests
- Inform patients that response to all diabetic therapies should be monitored by periodic measurements of blood glucose and A1C levels, with a goal of decreasing these levels toward the normal range. A1C monitoring is especially useful for evaluating long-term glycemic control.
Precautions with Alcohol
- Alcohol-Linagliptin interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- TRADJENTA®[1]
Look-Alike Drug Names
There is limited information regarding Linagliptin Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Page Name=Linagliptin |Pill Name=No image.jpg |Drug Name= |Pill Ingred=|+sep=; |Pill Imprint= |Pill Dosage= |Pill Color=|+sep=; |Pill Shape= |Pill Size (mm)= |Pill Scoring= |Pill Image= |Drug Author= |NDC=
}}
{{#subobject:
|Label Page=Linagliptin |Label Name=Linagliptin13.png
}}
{{#subobject:
|Label Page=Linagliptin |Label Name=Linagliptin14.png
}}
{{#subobject:
|Label Page=Linagliptin |Label Name=Linagliptin15.png
}}
{{#subobject:
|Label Page=Linagliptin |Label Name=Linagliptin16.png
}}
{{#subobject:
|Label Page=Linagliptin |Label Name=Linagliptin17.png
}}