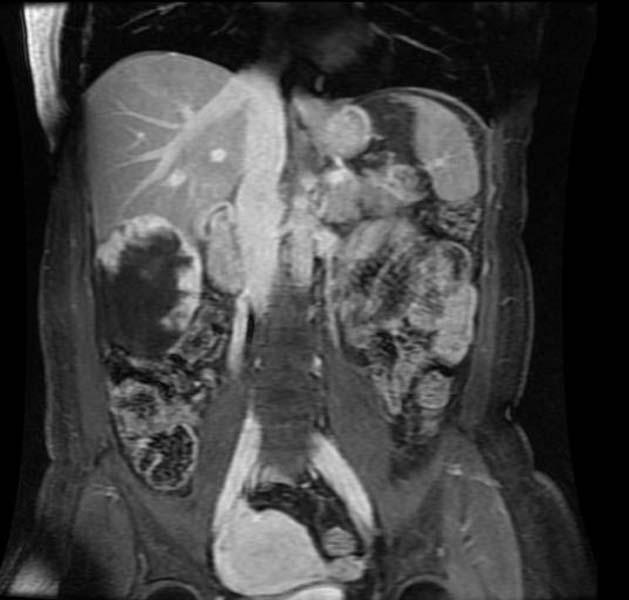
Hepatic hemangioma
| Hepatic hemangioma | |
 | |
|---|---|
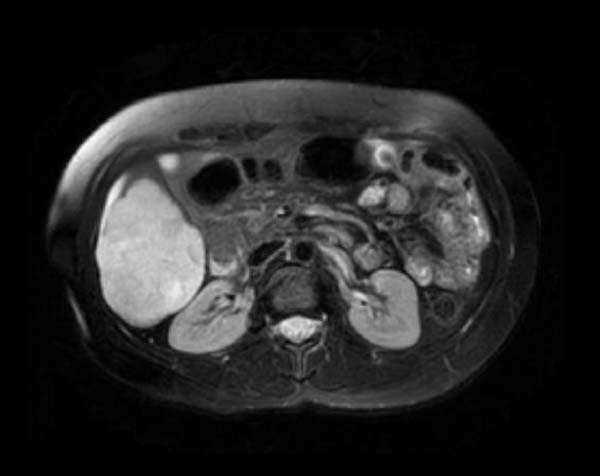
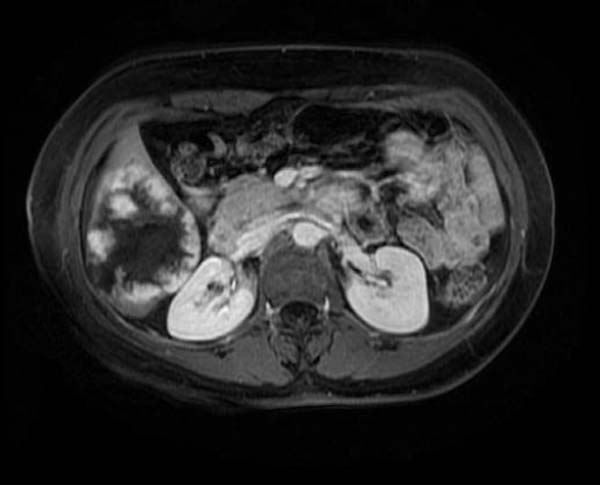
| Heptatic hemangioma. Image courtesy of RadsWiki |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Contributors: Cafer Zorkun M.D., PhD.
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [2] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Overview
- Most common primary liver tumor
- Ranges from 0.4-20% of the population
- Arise from the endothelial cells that line the blood vessels and consists of multiple, large vascular channels lined by a single layer of endothelial cells and supported by collagenous walls.
- They are frequently asymptomatic and incidentally discovered at imaging, surgery, or autopsy.
- They may be associated with focal nodular hyperplasia.
- M:F = 1:5
- May be associated with Kasabach-Merritt syndrome: Hemolytic anemia and consumptive coagulopathy
Diagnosis
Ultrasonography
- Echogenic
- Homogenous
Computed Tomography
- Noncontrast: Hypointense to liver
- Portal venous enhancement: Peripheral nodular enhancement
- Delayed enhancement: Lesion fills in the contrast
MRI
- T2 hyperintense
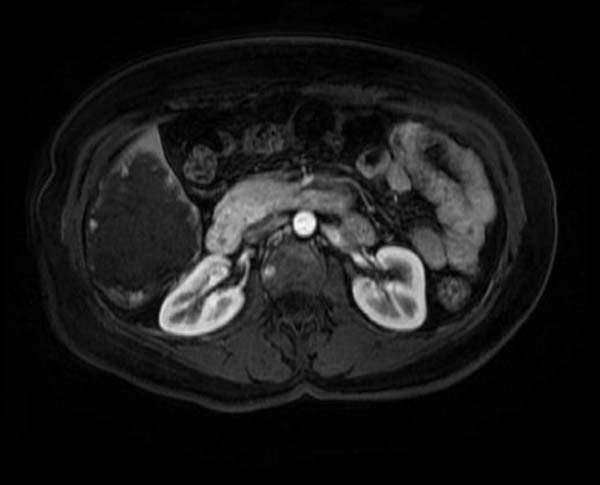
- Portal venous enhancement: Peripheral nodular enhancement
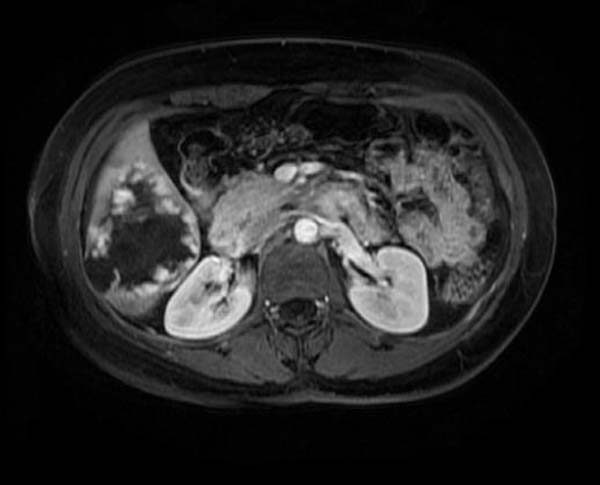
- Delayed enhancement: Lesion fills in the contrast
Scintigraphy
- Tc99-labeled red blood cells show decreased activity on early dynamic images and increased activity on delayed images (i.e. 1-2 hours).
- Only sensitive for larger lesions.
Diagnostic Findings
-
T2 FrFSE
-
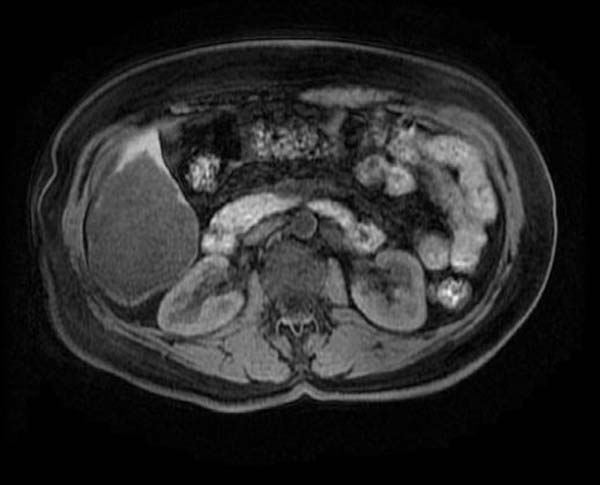
T1
-
T1 post Gad
-
T1 post Gad
-
T1 post Gad
-
T1 post Gad coronal
References
Template:Gastroenterology
Template:SIB