Entamoeba histolytica
|
Amoebiasis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Entamoeba histolytica On the Web |
|
American Roentgen Ray Society Images of Entamoeba histolytica |
| style="background:#Template:Taxobox colour;"|Entamoeba histolytica | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
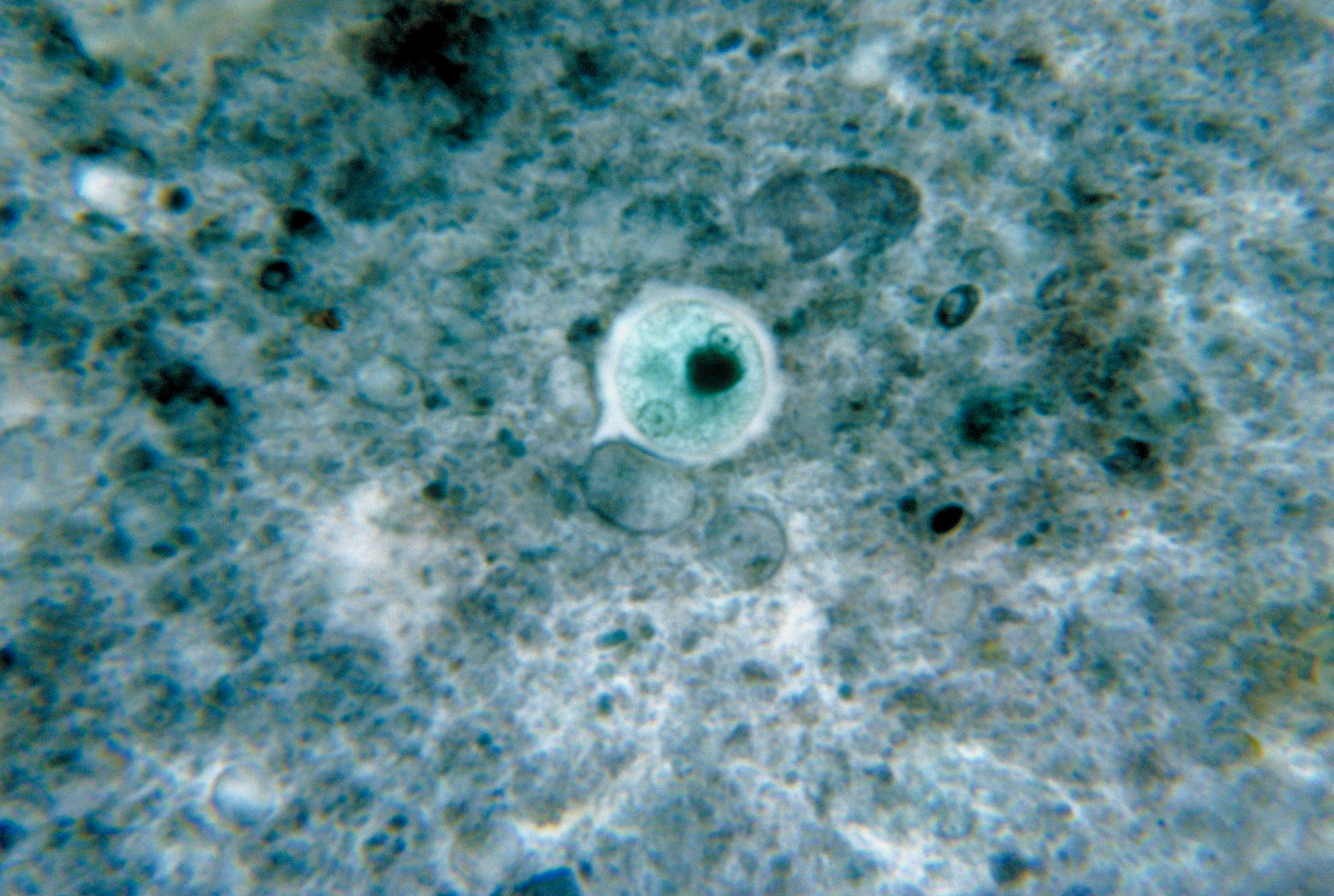 Entamoeba histolytica cyst
| ||||||||||
| style="background:#Template:Taxobox colour;" | Scientific classification | ||||||||||
|
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Jesus Rosario Hernandez, M.D. [2]
Overview
Entamoeba histolytica is a an anaerobic parasitic protozoan that is responsible for the development of amoebiasis.
Higher Order Classification
Cellular organisms; Eukaryota; Protista; Amoebozoa; Archamoebae; Entamoeba
Natural Reservoir
- Usually humans (only)
- Reports of animals as natural reservoirs of E. histolytica have been described.
Structure and Genome
- The exact number of chromosomes in E. histolytica is still unknown.
- The cysts of E. histolytica contain 4 nuclei with even distribution of chromatin between the nuclei.
- The trophozoites are spherical/oval shaped with a thin cell membrane and a single nucleus.
- E. histolytica is able to move using pseudopods.
Life Cycle
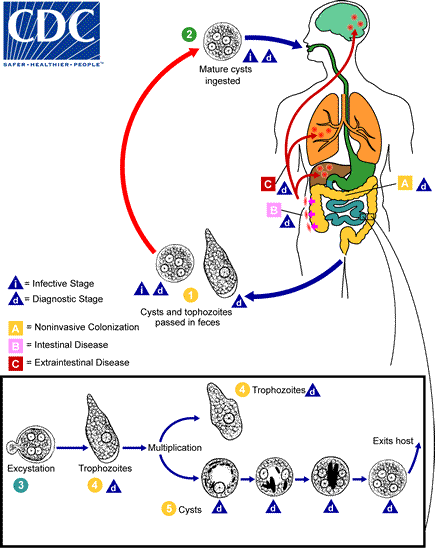
Retrieved from the Centers for Disease Control and Prevention
- Cysts and trophozoites are passed in human feces. Cysts are typically found in formed stool, whereas trophozoites are typically found in diarrheal stool.
- Infection by Entamoeba histolytica occurs by ingestion of mature cysts in fecally contaminated food, water, or hands.
- Excystation occurs in the small intestine and trophozoites are released, which migrate to the large intestine.
- The trophozoites multiply by binary fission and produce cysts, and both stages are passed in the feces.
- Because of the protection conferred by their walls, the cysts can survive days to weeks in the external environment and are responsible for transmission.
- Trophozoites passed in the stool are rapidly destroyed once outside the body, and if ingested would not survive exposure to the gastric environment.
- In many cases, the trophozoites remain confined to the intestinal lumen (A: noninvasive infection) of individuals who are asymptomatic carriers, passing cysts in their stool.
- In some patients the trophozoites invade the intestinal mucosa (B: intestinal disease), or, through the bloodstream, extraintestinal sites such as the liver, brain, and lungs (C: extraintestinal disease), with resultant pathologic manifestations.
- It has been established that the invasive and noninvasive forms represent two separate species, respectively E. histolytica and E. dispar. These two species are morphologically indistinguishable unless E. histolytica is observed with ingested red blood cells (erythrophagocystosis).
- Transmission can also occur through exposure to fecal matter during sexual contact (in which case not only cysts, but also trophozoites could prove infective).
Microbiological Characteristics
| Genus and Species | Entamoeba histolytica |
| Etiologic Agent of: | Amoebiasis; Amoebic dysentery; Extraintestinal Amoebiasis, usually Amoebic Liver Abscess = “anchovy sauce”); Amoeba Cutis; Amoebic Lung Abscess (“liver-colored sputum”) |
| Infective stage | Cyst |
| Definitive Host | Human |
| Portal of Entry | Mouth |
| Mode of Transmission | Ingestion of mature cyst through contaminated food or water |
| Habitat | Colon and Cecum |
| Pathogenic Stage | Trophozoite |
| Locomotive apparatus | Pseudopodia (“False Foot”) |
| Motility | Active, Progressive and Directional |
| Nucleus | 'Ring and dot' appearance: peripheral chromatin and central karyosome |
| Mode of Reproduction | Binary Fission |
| Pathogenesis | Lytic necrosis (it looks like “flask-shaped” holes in Gastrointestinal tract sections (GIT) |
| Type of Encystment | Protective and Reproductive |
| Lab Diagnosis | Most common is Direct Fecal Smear (DFS) and staining (but does not allow identification to species level); Enzyme immunoassay (EIA); Indirect Hemagglutination (IHA); Antigen detection – monoclonal antibody; PCR for species identification. Culture: From faecal samples - Robinson's medium, Jones' medium |
| Treatment | Metronidazole for the invasive trophozoites PLUS a luminal amoebicide for those still in the intestine (Paromomycin is the most widely used) |
| Trophozoite Stage | |
| Pathognomonic/Diagnostic Feature | Ingested RBC; distinctive nucleus |
| Cyst Stage | |
| Chromatoidal Body | 'Cigar' shaped bodies (made up of crystalline ribosomes) |
| Number of Nuclei | 1 in early stages, 4 when mature |
| Pathognomonic/Diagnostic Feature | 'Ring and dot' nucleus and chromatoid bodies |
Differential diagnosis
Entamoeba histolytica must be differentiated from other causes of viral, bacterial, and parasitic gastroentritis.
| Organism | Age predilection | Travel History | Incubation Size (cell) | Incubation Time | History and Symptoms | Diarrhea type8 | Food source | Specific consideration | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Fever | N/V | Cramping Abd Pain | Small Bowel | Large Bowel | Inflammatory | Non-inflammatory | |||||||||
| Viral | Rotavirus | <2 y | - | <102 | <48 h | + | + | - | + | + | - | Mostly in day cares, most common in winter. | |||
| Norovirus | Any age | - | 10 -103 | 24-48 h | + | + | + | + | + | - | Most common cause of gastroenteritis, abdominal tenderness, | ||||
| Adenovirus | <2 y | - | 105 -106 | 8-10 d | + | + | + | + | + | - | No seasonality | ||||
| Astrovirus | <5 y | - | 72-96 h | + | + | + | + | + | Seafood | Mostly during winter | |||||
| Bacterial | Escherichia coli | ETEC | Any age | + | 108 -1010 | 24 h | - | + | + | + | + | - | Causes travelers diarrhea, contains heat-labile toxins (LT) and heat-stable toxins (ST) | ||
| EPEC | <1 y | - | 10† | 6-12 h | - | + | + | + | + | Raw beef and chicken | - | ||||
| EIEC | Any ages | - | 10† | 24 h | + | + | + | + | + | Hamburger meat and unpasteurized milk | Similar to shigellosis, can cause bloody diarrhea | ||||
| EHEC | Any ages | - | 10 | 3-4 d | - | + | + | + | + | Undercooked or raw hamburger (ground beef) | Known as E. coli O157:H7, can cause HUS/TTP. | ||||
| EAEC | Any ages | + | 1010 | 8-18 h | - | - | + | + | + | - | May cause prolonged or persistent diarrhea in children | ||||
| Salmonella sp. | Any ages | + | 1 | 6 to 72 h | + | + | + | + | + | Meats, poultry, eggs, milk and dairy products, fish, shrimp, spices, yeast, coconut, sauces, freshly prepared salad. | Can cause salmonellosis or typhoid fever. | ||||
| Shigella sp. | Any ages | - | 10 - 200 | 8-48 h | + | + | + | + | + | Raw foods, for example, lettuce, salads (potato, tuna, shrimp, macaroni, and chicken) | Some strains produce enterotoxin and Shiga toxin similar to those produced by E. coli O157:H7 | ||||
| Campylobacter sp. | <5 y, 15-29 y | - | 104 | 2-5 d | + | + | + | + | + | Undercooked poultry products, unpasteurized milk and cheeses made from unpasteurized milk, vegetables, seafood and contaminated water. | May cause bacteremia, Guillain-Barré syndrome (GBS), hemolytic uremic syndrome (HUS) and recurrent colitis | ||||
| Yersinia enterocolitica | <10 y | - | 104 -106 | 1-11 d | + | + | + | + | + | Meats (pork, beef, lamb, etc.), oysters, fish, crabs, and raw milk. | May cause reactive arthritis; glomerulonephritis; endocarditis; erythema nodosum.
can mimic appendicitis and mesenteric lymphadenitis. | ||||
| Clostridium perfringens | Any ages | > 106 | 16 h | - | - | + | + | + | Meats (especially beef and poultry), meat-containing products (e.g., gravies and stews), and Mexican foods. | Can survive high heat, | |||||
| Vibrio cholerae | Any ages | - | 106-1010 | 24-48 h | - | + | + | + | + | Seafoods, including molluscan shellfish (oysters, mussels, and clams), crab, lobster, shrimp, squid, and finfish. | Hypotension, tachycardia, decreased skin turgor. Rice-water stools | ||||
| Parasites | Protozoa | Giardia lamblia | 2-5 y | + | 1 cyst | 1-2 we | - | - | + | + | + | Contaminated water | May cause malabsorption syndrome and severe weight loss | ||
| Entamoeba histolytica | 4-11 y | + | <10 cysts | 2-4 we | - | + | + | + | + | Contaminated water and raw foods | May cause intestinal amebiasis and amebic liver abscess | ||||
| Cryptosporidium parvum | Any ages | - | 10-100 oocysts | 7-10 d | + | + | + | + | + | Juices and milk | May cause copious diarrhea and dehydration in patients with AIDS especially with 180 > CD4 | ||||
| Cyclospora cayetanensis | Any ages | + | 10-100 oocysts | 7-10 d | - | + | + | + | + | Fresh produce, such as raspberries, basil, and several varieties of lettuce. | More common in rainy areas | ||||
| Helminths | Trichinella spp | Any ages | - | Two viable larvae (male and female) | 1-4 we | - | + | + | + | + | Undercooked meats | More common in hunters or people who eat traditionally uncooked meats | |||
| Taenia spp | Any ages | - | 1 larva or egg | 2-4 m | - | + | + | + | + | Undercooked beef and pork | Neurocysticercosis: Cysts located in the brain may be asymptomatic or seizures, increased intracranial pressure, headache. | ||||
| Diphyllobothrium latum | Any ages | - | 1 larva | 15 d | - | - | - | + | + | Raw or undercooked fish. | May cause vitamin B12 deficiency | ||||
8Small bowel diarrhea: watery, voluminous with less than 5 WBC/high power field
Large bowel diarrhea: Mucousy and/or bloody with less volume and more than 10 WBC/high power field
† It could be as high as 1000 based on patient's immunity system.
The table below summarizes the findings that differentiate inflammatory causes of chronic diarrhea[1][2][3][4][4]
| Cause | History | Laboratory findings | Diagnosis | Treatment |
|---|---|---|---|---|
| Diverticulitis |
|
|
Abdominal CT scan with oral and intravenous (IV) contrast | bowel rest, IV fluid resuscitation, and broad-spectrum antimicrobial therapy which covers anaerobic bacteria and gram-negative rods |
| Ulcerative colitis |
|
|
Endoscopy | Induction of remission with mesalamine and corticosteroids followed by the administration of sulfasalazine and 6-Mercaptopurine depending on the severity of the disease. |
| Entamoeba histolytica |
|
cysts shed with the stool | detects ameba DNA in feces | Amebic dysentery
Luminal amebicides for E. histolytica in the colon:
For amebic liver abscess:
|
Gallery
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
-
Entamoeba histolytica. From Public Health Image Library (PHIL). [5]
References
- ↑ Konvolinka CW (1994). "Acute diverticulitis under age forty". Am J Surg. 167 (6): 562–5. PMID 8209928.
- ↑ Silverberg MS, Satsangi J, Ahmad T, Arnott ID, Bernstein CN, Brant SR; et al. (2005). "Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a Working Party of the 2005 Montreal World Congress of Gastroenterology". Can J Gastroenterol. 19 Suppl A: 5A–36A. PMID 16151544.
- ↑ Satsangi J, Silverberg MS, Vermeire S, Colombel JF (2006). "The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications". Gut. 55 (6): 749–53. doi:10.1136/gut.2005.082909. PMC 1856208. PMID 16698746.
- ↑ 4.0 4.1 Haque R, Huston CD, Hughes M, Houpt E, Petri WA (2003). "Amebiasis". N Engl J Med. 348 (16): 1565–73. doi:10.1056/NEJMra022710. PMID 12700377.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 "Public Health Image Library (PHIL)".
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/5/5d/Entamoeba_histolytica01.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/1/11/Entamoeba_histolytica02.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/8/8d/Entamoeba_histolytica03.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/e/ec/Entamoeba_histolytica04.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/7/74/Entamoeba_histolytica05.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/d/d9/Entamoeba_histolytica06.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/b/bc/Entamoeba_histolytica07.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/2/24/Entamoeba_histolytica08.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/e/e0/Entamoeba_histolytica09.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/0/0b/Entamoeba_histolytica11.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/e/e9/Entamoeba_histolytica12.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/2/2b/Entamoeba_histolytica13.jpeg)
![Entamoeba histolytica. From Public Health Image Library (PHIL). [5]](/images/1/10/Entamoeba_histolytica14.jpeg)