Dysplastic nevus natural history, complications and prognosis
|
Dysplastic nevus Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Dysplastic nevus natural history, complications and prognosis On the Web |
|
American Roentgen Ray Society Images of Dysplastic nevus natural history, complications and prognosis |
|
FDA on Dysplastic nevus natural history, complications and prognosis |
|
CDC on Dysplastic nevus natural history, complications and prognosis |
|
Dysplastic nevus natural history, complications and prognosis in the news |
|
Blogs on Dysplastic nevus natural history, complications and prognosis |
|
Risk calculators and risk factors for Dysplastic nevus natural history, complications and prognosis |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] ; Associate Editor(s)-in-Chief: Aditya Ganti M.B.B.S. [2]
Overview
If left untreated, dysplastic nevus progression occurs horizontally (radial growth plate) and vertically (vertical growth plate) and is then followed by dermal invasion and distant metastasis. Dysplastic nevus is an aggressive tumor characterized by early metastasis. Common sites of metastasis include bones, brain, kidneys, lungs, liver and skin (secondary distant site). Complications of dysplastic nevus are usually related to the site of metastasis. The 5-year relative survival of patients with dysplastic nevus is approximately 93%. Features associated with worse prognosis are tumor thickness (Breslow thickness), depth related to skin structures (Clark level), type of melanoma, presence of ulceration, presence of lymphatic/perineural invasion, location of lesion, presence of satellite lesions, and the presence of regional or distant metastasis.
Natural History
- If left untreated, melanocytes first proliferate randomly with an aberrant growth within an existing nevus.
- More advanced stages are characterized by a radial growth phase with intraepidermal growth and penetration into the papillary dermis.
- Final stages demonstrate a vertical growth phase with dermal invasion and widening of the papillary dermis before cancerous cells finally metastasize to other parts of the skin and other organs.
Complications
Complications of Dysplastic nevus are usually due to distant metastasis. Common sites of metastasis are shown below:
Prognosis
Determinants of Prognosis
- Tumor thickness in millimeters (Breslow's depth)
- Depth related to skin structures (Clark level)
- Type of melanoma
- Presence of ulceration
- Presence of lymphatic/perineural invasion
- Presence of tumor infiltrating lymphocytes (if present, prognosis is better)
- Location of lesion
- Presence of satellite lesions
- Presence of regional or distant metastasis
Micro-metastasis vs. Macro-metastasis
- Extent of malignancy within a node is also important; micro-metastases in which malignancy is only microscopic have a more favorable prognosis than macro-metastases.
- In some cases, micro-metastases may only be detected by special staining, and if malignancy is only detectable polymerase chain reaction (PCR), the prognosis is better.
- Macro-metastases in which malignancy is clinically apparent (in some cases cancer completely replaces a node) have a far worse prognosis, and if nodes are matted or if there is extra-capsular extension, the prognosis is still worse.
5-Year Survival
- When stratified by age, the 5-year relative survival of patients with melanoma was 92.7% and 88.2% for patients <65 and ≥ 65 years of age respectively.[3]
- When there is distant metastasis, the cancer is generally considered incurable. The five year survival rate is less than 10%.[4]
- The survival of patients with melanoma varies with the stage of the disease. Shown below is a table depicting the 5-year relative survival by the stage of melanoma:[3]
| Stage | 5-year relative survival (%), 2004-2010 |
|---|---|
| All stages | 91.3% |
| Localized | 98.1% |
| Regional | 62.6% |
| Distant | 16.1% |
| Unstaged | 78.4% |
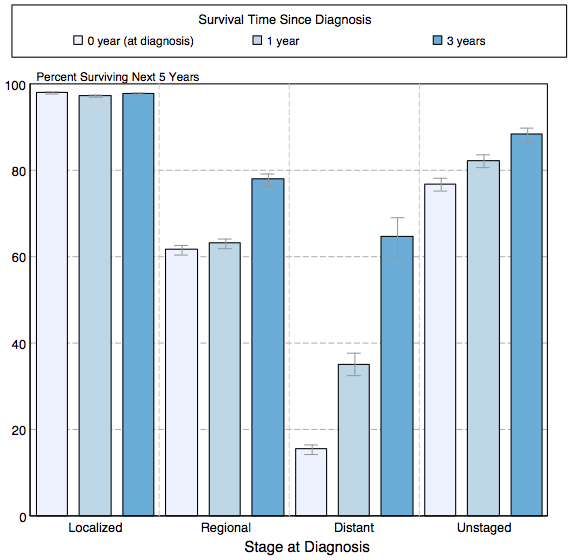
- Shown below is an image depicting the 5-year conditional relative survival (probability of surviving in the next 5-years given the cohort has already survived 0, 1, 3 years) between 1998 and 2010 of melanoma by stage at diagnosis according to SEER. These graphs are adapted from SEER: The Surveillance, Epidemiology, and End Results Program of the National Cancer Institute.[3]
References
- ↑ Brant JM (November 2013). "Breathlessness with pulmonary metastases: a multimodal approach". J Adv Pract Oncol. 4 (6): 415–22. PMC 4093448. PMID 25032021.
- ↑ Homsi J, Kashani-Sabet M, Messina J, Daud A (2005). "Cutaneous melanoma: prognostic factors". Cancer Control. 12 (4): 223–9. PMID 16258493.Full text (PDF)
- ↑ 3.0 3.1 3.2 3.3 Howlader N, Noone AM, Krapcho M, Garshell J, Miller D, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z,Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (eds). SEER Cancer Statistics Review, 1975-2011, National Cancer Institute. Bethesda, MD, http://seer.cancer.gov/csr/1975_2011/, based on November 2013 SEER data submission, posted to the SEER web site, April 2014.
- ↑ Balch C, Buzaid A, Soong S, Atkins M, Cascinelli N, Coit D, Fleming I, Gershenwald J, Houghton A, Kirkwood J, McMasters K, Mihm M, Morton D, Reintgen D, Ross M, Sober A, Thompson J, Thompson J (2001). "Final version of the American Joint Committee on Cancer staging system for cutaneous melanoma". J Clin Oncol. 19 (16): 3635–48. PMID 11504745.Full text