Cough resident survival guide: Difference between revisions
Jump to navigation
Jump to search
Sara Haddadi (talk | contribs) |
Sara Haddadi (talk | contribs) |
||
| Line 211: | Line 211: | ||
{{Family tree | | | | | | | | | | | | | | | B01 | | | | | | | | | | | | | | | | | | | | | | | | |B01= '''Chronic Cough'''}} | {{Family tree | | | | | | | | | | | | | | | B01 | | | | | | | | | | | | | | | | | | | | | | | | |B01= '''Chronic Cough'''}} | ||
{{Family tree | | | | | | |,|-|-|-|-|-|v|-|-|^|-|-|-|v|-|-|-|-|.| | | | | | | | | | | | | | | | | | | | }} | {{Family tree | | | | | | |,|-|-|-|-|-|v|-|-|^|-|-|-|v|-|-|-|-|.| | | | | | | | | | | | | | | | | | | | }} | ||
{{Family tree | | | | | | C01 | | | | C02 | | | | | C03 | | | C04 | | | | | |C01= first-generation antihistamine/decongestant<br> ❑Partial or complete resolution of cough after one to two weeks shows '''upper airway cough syndrome''' as the cause<br> ❑persistent symptoms: begin a topical nasal steroid<br> ❑symptoms still persist: sinus imaging for sinusitis| C02= '''ASTHMA-INDUCED CHRONIC COUGH'''<br> inhaled corticosteroids and beta agonists<br> ❑No response or cannot take inhaled medication: Oral consideration corticosteroids for five to 10 days*<br> ❑Consider adding a leukotriene inhibitor before an oral corticosteroid|C03= | {{Family tree | | | | | | C01 | | | | C02 | | | | | C03 | | | C04 | | | | | |C01=1'''UPPER AIRWAY COUGH SYNDROME–INDUCED CHRONIC COUGH'''<br>first-generation antihistamine/decongestant<br> ❑Partial or complete resolution of cough after one to two weeks shows '''upper airway cough syndrome''' as the cause<br> ❑persistent symptoms: begin a topical nasal steroid<br> ❑symptoms still persist: sinus imaging for sinusitis| C02= 2'''ASTHMA-INDUCED CHRONIC COUGH'''<br> inhaled corticosteroids and beta agonists<br> ❑No response or cannot take inhaled medication: Oral consideration corticosteroids for five to 10 days*<br> ❑Consider adding a leukotriene inhibitor before an oral corticosteroid|C03= 3'''NONASTHMATIC EOSINOPHILIC BRONCHITIS-INDUCED CHRONIC COUGH'''<br>inhaled corticosteroids for 4 weeks|C04= 4'''GERD-INDUCED CHRONIC COUGH'''<br>Any patient who responds only partially or not at all to the therapies discussed in 1-3 should be empirically treated for GERD.}} | ||
{{familytree/end}} | {{familytree/end}} | ||
Revision as of 05:45, 27 October 2020
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sara Haddadi, M.D.[2]
| Cough Resident Survival Guide |
|---|
| Overview |
| Causes |
| FIRE |
| Diagnosis |
| Treatment |
| Do's |
| Don'ts |
Overview
Causes
Common Causes
- Allergic Rhinitis
- Asthma
- Bronchiectasis
- Gastroesophageal Reflux Disease (GERD)
- Post-nasal drip
- Medications' side effect
- Bronchitis
- Laryngopharyngeal reflux
- Respiratory tract infection
- Lung cancer
- Nonasthmatic eosinophilic bronchitis
Diagnosis
Shown below is an algorithm summarizing the evaluation of acute cough according to the American College of Chest Physicians guidelines.[1]
| Acute Cough | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| History and physical
examination, ask about environmental and occupational factors and travel exposures ± investigations | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Life-threatening diagnosis | Non-life-threatening diagnosis | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Pneumonia, severe
exacerbation of asthma or COPD, PE, heart failure, other serious disease | Infections | Exacerbation of pre-existing condition | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| LRTI | URTI | Asthma | Bronchiectasis | UACS | COPD | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Evaluate and treat first | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Acute Bronchitis | Pertussis | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Consider TB in
endemic areas or high risk | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
- Shown below is an alogrithm describing the evaluation of subacute cough in adults according to the American College of Chest Physicians guidelines.
| Subacute Cough | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| History and Physical Exam Ask about red flags,
environmental and occupational factors, travel exposures | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Postinfectious or life-threatening diagnosis | New onset or exacerbation of pre-existing condition | Not postinfectious* | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Pneumonia, severe exacerbation of asthma or COPD, PE, heart failure, other serious disease | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Pertusis | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| COPD | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| UACS | Asthma | Bronchitis | GERD | Bronchiectasis | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| {{{ }}} | Postinfectious | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| TB | NAEB | AECB/COPD | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
- Not postinfectious: Work up same as chronic cough
- Shown below is an algorithm describing the evaluation of chronic cough in adults according to the American College of Chest Physicians guidelines.
| Chronic Cough | |||||||||||||||||||||||||||||||||||||||||||||||||||
| History, Physical exam and CXR | |||||||||||||||||||||||||||||||||||||||||||||||||||
| Life-threatening condition | Consider 4 most common causes: 1)Upper Airway Cough Syndrome (UACS), secondary to rhinosinus diseases, 2)Asthma, 3)Non-asthmatic Eosinophilic Bronchitis 4)Gastroesophageal Reflux Disease (GERD) | Smoking, ACEI, Sitagliptin | |||||||||||||||||||||||||||||||||||||||||||||||||
| Treat based on the cause | Discontinue for at least 4week | ||||||||||||||||||||||||||||||||||||||||||||||||||
| Follow up 4-6 weeks if inadequate response | Initial treatments for each condition | Further investigation if No response to treatment* | Consider 4 most common causes of cough if No response at4-6 week follow up | ||||||||||||||||||||||||||||||||||||||||||||||||
| Follow up 4-6 weeks if inadequate response to optimal treatment | |||||||||||||||||||||||||||||||||||||||||||||||||||
Consider the following further investigations if no response to treatment*:
- 24h esophageal pH / Impedance monitoring
- Endoscopic and/or videofluoroscopic swallow evaluation
- Barium esophagram / Modified barium swallow
- Sinus Imaging• HRCT
- Bronchoscopy• Cardiac Work-up (ECG, Holter Monitoring, Echo)
- Environmental / Occupational Assessment
- Consider uncommon causes
Treatment
Shown below is an algorithm summarizing the treatment of Cough according to the American College of Chest Physicians guidelines.
 | |||||||||||||||||||
| Acute Cough | |||||||||||||||||||
| determine if the cause of the cough is one of the life-threatening conditions below and treat accordingly ❑Pneumonia ❑severe exacerbation of asthma or COPD ❑ PE ❑heart failure ❑ other serious condittons | Cough due to the common cold: a first-generation antihistamine plus a decongestant ❑ naproxen (Naprosyn) favorably affects cough ❑ Newer-generation nonsedating antihistamines are not effective | ||||||||||||||||||
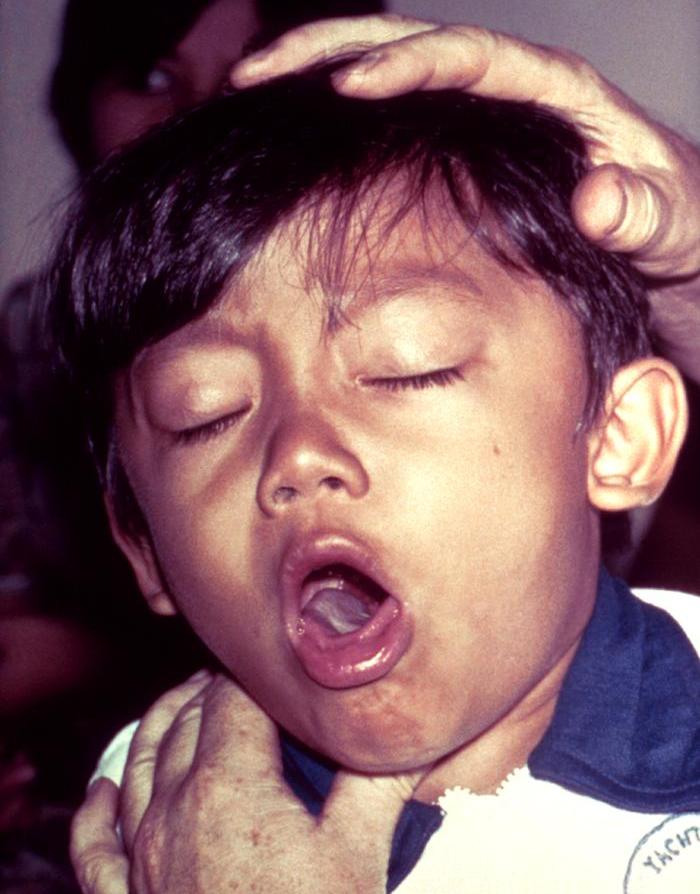 | |||||||||||||||||||
| Subacute Cough | |||||||||||||||||||
| confirmed whooping cough by culture positive nasopharyngeal swab: macrolide antibiotics plus isolation for 5 days beginning first day of treatment | Cough not caused by Bordetella pertussis: inhaled ipratropium (Atrovent) ❑if cough persists: inhaled corticosteroids ❑severe cough:30 to 40 mg of prednisone per day for a brief period) ❑When other treatments fail: codeine or dextromethorphan (Delsym) | ||||||||||||||||||
Do's
- The content in this section is in bullet points.
Don'ts
- The content in this section is in bullet points.
References
- ↑ Irwin RS, French CL, Chang AB, Altman KW, CHEST Expert Cough Panel* (2018). "Classification of Cough as a Symptom in Adults and Management Algorithms: CHEST Guideline and Expert Panel Report". Chest. 153 (1): 196–209. doi:10.1016/j.chest.2017.10.016. PMC 6689094 Check
|pmc=value (help). PMID 29080708.