Ciprofloxacin microbiology
| Ciprofloxacin Hydrochloride |
|---|
| CIPRO®,CIPROFLOXACIN®,CILOXAN®,CETRAXAL® FDA Package Insert |
| Description |
| Clinical Pharmacology |
| Microbiology |
| Indications and Usage |
| Contraindications |
| Warnings |
| Precautions |
| Adverse Reactions |
| Overdosage |
| Clinical Studies |
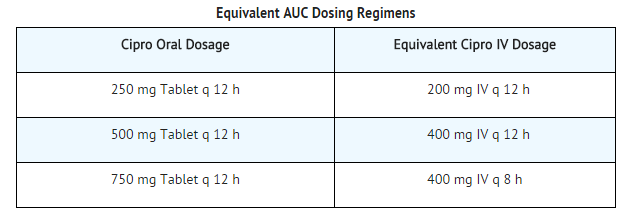
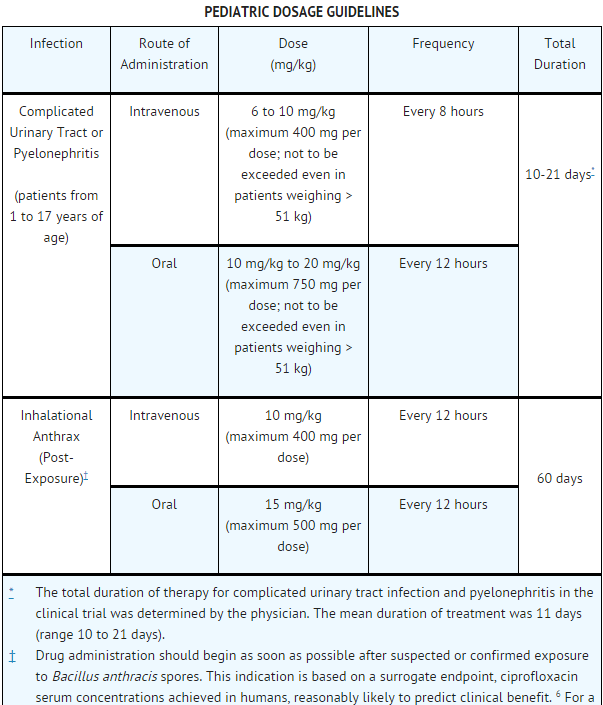
| Dosage and Administration |
| How Supplied |
| Medication Guide |
| Direction For Use |
| Labels and Packages |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1];Associate Editor(s)-in-Chief: Abdurahman Khalil, M.D. [2]
Mechanism of Action
The bactericidal action of ciprofloxacin results from inhibition of the enzymes topoisomerase II (DNA gyrase) and topoisomerase IV (both Type II topoisomerases), which are required for bacterial DNA replication, transcription, repair, and recombination.
Mechanism of Resistance
The mechanism of action of fluoroquinolones, including ciprofloxacin, is different from that of penicillins, cephalosporins, aminoglycosides, macrolides, and tetracyclines; therefore, microorganisms resistant to these classes of drugs may be susceptible to ciprofloxacin. Resistance to fluoroquinolones occurs primarily by either mutations in the DNA gyrases, decreased outer membrane permeability, or drug efflux. In vitro resistance to ciprofloxacin develops slowly by multiple step mutations. Resistance to ciprofloxacin due to spontaneous mutations occurs at a general frequency of between < 10-9 to 1x10-6.
Cross-Resistance
There is no known cross-resistance between ciprofloxacin and other classes of antimicrobials.
Ciprofloxacin has been shown to be active against most isolates of the following bacteria, both in vitro and in clinical infections as described in the INDICATIONS AND USAGE section of the package insert for CIPRO (ciprofloxacin hydrochloride) Tablets and CIPRO (ciprofloxacin*) 5% and 10% Oral Suspension.
Gram-positive bacteria Enterococcus faecalis (vancomycin-susceptible isolates only)
Staphylococcus aureus (methicillin-susceptible isolates only)
Staphylococcus epidermidis (methicillin-susceptible isolates only)
Staphylococcus saprophyticus
Streptococcus pneumoniae (penicillin-susceptible isolates only)
Streptococcus pyogenes
Gram-negative bacteria
Ciprofloxacin has been shown to be active against Bacillus anthracis both in vitro and by use of serum levels as a surrogate marker (see INDICATIONS AND USAGE and INHALATIONAL ANTHRAX – ADDITIONAL INFORMATION).
The following in vitro data are available, but their clinical significance is unknown. At least 90 percent of the following bacteria exhibit an in vitrominimum inhibitory concentration (MIC) less than or equal to the susceptible breakpoint for ciprofloxacin (≤1 mcg/mL). However, the efficacy of ciprofloxacin in treating clinical infections due to these bacteria has not been established in adequate and well-controlled clinical trials.
Gram-positive bacteria
Staphylococcus haemolyticus (methicillin-susceptible isolates only)
Staphylococcus hominis (methicillin-susceptible isolates only)
Bacillus anthracis
Gram-negative bacteria
Susceptibility Test Methods
When available, the clinical microbiology laboratory should provide the results of in vitro susceptibility test results for antimicrobial drug products used in resident hospitals to the physician as periodic reports that describe the susceptibility profile of nosocomial and community-acquired pathogens. These reports should aid the physician in selecting an antibacterial drug product for treatment.
• Dilution Techniques: Quantitative methods are used to determine antimicrobial minimum inhibitory concentrations (MICs). These MICs provide estimates of the susceptibility of bacteria to antimicrobial compounds. The MICs should be determined using a standardized test method (broth and/or agar).1, 3,4 The MIC values should be interpreted according to criteria provided in Table 1. •
Diffusion Techniques: Quantitative methods that require measurement of zone diameters can also provide reproducible estimates of the susceptibility of bacteria to antimicrobial compounds. The zone size provides an estimate of the susceptibility of bacteria to antimicrobial compounds. The zone size should be determined using a standardized test method.2, 3, 4 This procedure uses paper disks impregnated with 5 mcg ciprofloxacin to test the susceptibility of bacteria to ciprofloxacin. The disc diffusion interpretive criteria are provided in Table 1.
1. A report of “Susceptible” indicates that the antimicrobial is likely to inhibit growth of the pathogen if the antimicrobial compound reaches the concentrations at the site of infection necessary to inhibit growth of the pathogen. A report of “Intermediate” indicates that the result should be considered equivocal, and, if the microorganism is not fully susceptible to alternative, clinically feasible drugs, the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where high dosage of drug can be used. This category also provides a buffer zone that prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of “Resistant” indicates that the antimicrobial is not likely to inhibit growth of the pathogen if the antimicrobial compound reaches the concentrations usually achievable at the infection site; other therapy should be selected.
• Quality Control: Standardized susceptibility test procedures require the use of laboratory controls to monitor the accuracy and precision of supplies and reagents used in the assay, and the techniques of the individuals performing the test.1,2,3,4 Standard ciprofloxacin powder should provide the following range of MIC values noted in Table 2. For the diffusion technique using the ciprofloxacin 5 mcg disk the criteria in Table 2 should be achieved.
References
http://www.accessdata.fda.gov/drugsatfda_docs/label/2011/019537s075,020780s033lbl.pdf