Antisynthetase syndrome: Difference between revisions
| Line 94: | Line 94: | ||
==Risk Factors== | ==Risk Factors== | ||
There are several environmental exposures associated with antisynthetase syndrome. These include ultraviolet radiation, stress, muscle overexertion, collage implants, infections such as retroviruses and streptococci bacteria, and certain drugs and chemicals. https://www.niehs.nih.gov/research/clinical/bethesda/participants/studies/erftas/index.cfm | There are several environmental exposures associated with antisynthetase syndrome. These include ultraviolet radiation, stress, muscle overexertion, collage implants, infections such as retroviruses and streptococci bacteria, and certain drugs and chemicals.<ref name=“NIH”>{{cite web|url= https://www.niehs.nih.gov/research/clinical/bethesda/participants/studies/erftas/index.cfm}} </ref> | ||
==Natural History, Complications and Prognosis== | ==Natural History, Complications and Prognosis== | ||
Latest revision as of 18:43, 11 August 2022
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-In-Chief: M. Hassan, M.B.B.S
Synonyms and keywords:
Overview
Antisynthetase syndrome, an uncommon autoimmune disorder, is characterized by antibodies against aminoacyl-transfer ribonucleic acid synthetases, with various combinations of three cardinal manifestations of interstitial lung disease (ILD), polymyositis, and arthritis. Other features of antisynthetase syndrome may include pyrexia of unknown origin, mechanic's hand (hyperkeratotic skin changes along the lateral surfaces of the digits) and Raynaud's phenomenon.[1][2]
So far, nine different anti-aminoacyl t-RNA synthetase (ARS) antibodies have been identified to play a role in the development of antisynthetase syndrome.[1]
Historical Perspective
In 1990, Marguerie et al and coworkers first described antisynthetase syndrome as a triad of polymyositis, interstitial lung disease (ILD), and the presence of myositis-specific autoantibodies to aminoacyl-transfer ribonucleic acid synthetases.[3]
Classification
Antisynthetase syndrome may be classified in accordance with the type of antibodies that are present. Some of the identified antibodies include Anti-Jo-1, Anti PL-12, Anti-Pl-7, Anti-OJ, Anti-KS, Anti-EJ, Anti-Ha, and Anti-Zo.[4]
Pathophysiology
Antisynthetase syndrome is characterized by the presence of myositis-specific anti-synthetase antibodies.[5]
| Anti-ARS antibodies | Antigen | Clinical features |
|---|---|---|
| Anti-Jo-1 | Histidyl-tRNA synthetase |
|
| Anti PL-12 | Alanyl-tRNA synthetase, Alanyl-tRNA |
|
| Anti-PL-7 | Glycyl-tRNA synthetase |
|
| Anti-OJ | Isoleucyl-tRNA synthetase | |
| Anti-KS | Asparaginyl-tRNA synthetase | |
| Anti-EJ | Glycyl-tRNA synthetase |
|
| Anti-Ha | Tyrosyl-tRNA synthetase | |
| Anti-Zo | Phenylalanyl-tRNA synthetase |
Causes
The exact cause of antisynthetase syndrome is not fully understood.
Differentiating Antisynthetase syndrome from other Diseases
Antisynthetase syndrome may be misdiagnosed as idiopathic interstitial lung disease (ILD) or inflammatory myopathy, as a result of rarity, lack of awareness of the disease, as well as due to the lack of available testing for anti-ARS antibodies.[1]
Epidemiology and Demographics
Age
The mean age at onset of antisynthetase syndrome in adults varies from 43 to 60 years.[5]
Gender
Antisynthetase syndrome is 2–3 times more common in women than in men.[5]
Race
Antisynthetase syndrome usually affects individuals of the black American ethnicity race.[1]
Risk Factors
There are several environmental exposures associated with antisynthetase syndrome. These include ultraviolet radiation, stress, muscle overexertion, collage implants, infections such as retroviruses and streptococci bacteria, and certain drugs and chemicals.[6]
Natural History, Complications and Prognosis
Main causes of death in antisynthetase syndrome is anti-Jo-1-positive patients included interstitial lung disease, neoplasm, infectious diseases including pneumonia, severe myositis and cardiovascular disorders.
The cumulative ten-year survival rate in patients with antisynthetase syndrome was estimated as 76.8%.[7]
| Poor prognostic factors associated with Antisynthetase syndrome [1] |
|---|
| 1) Anti-Ro 52 |
| 2) Rapidly progressive interstitial lung disease |
| 3) Pulmonary hypertension |
| 4) Malignancy |
| 5) Male sex |
| 6) Reduced diffusing capacity of lung for carbon monoxide |
| 7) Elevated serum ferritin |
| 8) Black American ethnicity |
Diagnosis
Diagnostic Criteria
In 2010, Connors et al proposed a formal criteria for the diagnosis of antisynthetase syndrome. This criteria proposed that all patients must have a presence of an anti-aminoacyl tRNA synthetase antibody in addition to one or more of the following clinical features: mechanic’s hands, Raynaud’s phenomenon, myositis, interstitial lung disease (ILD), arthritis, and/or unexplained fever.
In 2011, Solomon et al proposed alternative criteria, which is more strict. This criteria requires the presence of anti-aminoacyl tRNA synthetase antibody plus two major or one major and two minor criteria.
Major criteria includes: Interstitial Lung Disease (not attributable to another cause), and Polymyositis or dermatomyositis.
Minor criteria includes: arthritis, Raynaud’s phenomenon, and mechanic’s hands.[4]
| Connors et al (2010) criteria |
|---|
| Required: Presence of an anti-aminoacyl tRNA synthetase antibody |
| PLUS one or more of the following clinical features:
1) Raynaud’s phenomenon 2) Arthritis 3) Interstitial lung disease 4) Fever (not attributable to another cause) 5) Mechanic’s hands (thickened and cracked skin on hands, particularly at fingertips) |
| Solomon et al (2011) criteria |
|---|
| Required: Presence of anti-aminoacyl tRNA synthetase antibody |
| PLUS two major or one major and two minor criteria:
1) Interstitial Lung Disease (not attributable to another cause) 2) Polymyositis or dermatomyositis
1) Arthritis 2) Raynaud’s phenomenon 3) Mechanic’s hands |
Symptoms
Symptoms seen at the diagnosis of antisynthetase syndrome include the following:[1]
| Symptoms of antisynthetase syndrome |
|---|
| 1) Fever |
| 2) Weight loss |
| 3) Anorexia |
| 4) Dyspnea |
| 5) Dry cough |
| 6) Arthralgia |
| 7) Joint swelling |
| 8) Proximal muscle weakness |
| 9) Myalgia |
| 10) Raynaud's phenomenon |
Physical Examination
Physical exam findings play an important role in diagnosis of antisynthetase syndrome as the findings may be classified into major and minor criteria. Clinical findings on examination includes:[1]
| Clinical findings |
|---|
| 1) Polyarthritis |
| 2) Mechanics hands (hyperkeratotic lesions on the radial and palmar aspects of the hands and fingers with fissuring and scaling of the skin) |
| 3) Calcinosis cutis |
| 4) Malar rash |
| 5) Cutaneous ulcers |
| 6) Crackles on chest auscultation |
Laboratory Findings
Suggested lab findings based on the systems are as follows:[8]
| Domains | Suggested investigations |
|---|---|
| Bloodwork | CBC, creatinine, CK, LDH, aldolase, AST, ALT, ANA, ENA, RF, ACPA, MSAs and MAAs |
| Muscle | MMT8 and consider: MRI pelvic/thighs and shoulder girdle muscles, EMG, and Muscle biopsy |
| Joint | TJC, SJC |
| Lung | CXR, HRCT, PFT, 6MWT, echocardiogram for PAH if isolated decrease in DLCO,
Referral to respirology for co-management if ILD |
| Skin | General assessment and consider documentation with CDASI
Referral to dermatologists |
| Raynaud’s phenomenon | Conservative and pharmacological management review |
| Overall disease activity and damage assessment | Consider MDAAT, MDI |
| TJC: tender joint count; SJC: swollen joint count; PAH: pulmonary artery hypertension; MMT8: manual muscle testing 8
MRI: magnetic resonance imaging; EMG: electromyography; CXR: chest X-ray; HRCT: high-resolution computed tomography; PFT: pulmonary function test; 6MWT: 6-minute walk test; DLCO: diffusing capacity of lung for carbon monoxide; ILD: interstitial lung disease; CDASI: cutaneous dermatomyositis disease area and severity index; CBC: complete blood count; CK: creatine kinase; LDH: lactate dehydrogenase; AST: aspartate aminotransferase; ALT: alanine transaminase; ANA: antinuclear antibody; ENA: extractable nuclear antigens; RF: rheumatoid factor; ACPA: anti-citrullinated protein antibody; MSA: myositis-specific antibody; MAA: myositis-associated antibody; MDAAT: Myositis Disease Activity Assessment Tool; MDI: myositis damage index | |
Imaging Findings
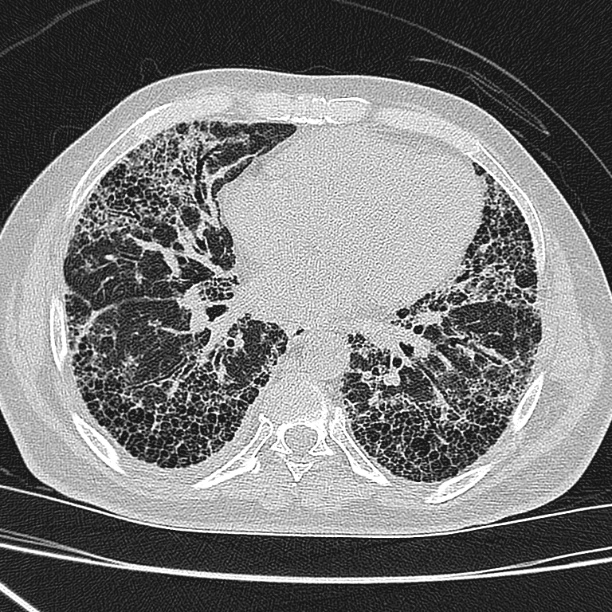
As antisynthetase syndrome is associated with interstitial lung disease, and therefore, high resolution computed tomography (HRCT) plays an important role in its work up, as well as to monitor the disease activity. Radiographic features seen on HRCT at the initial diagnosis include traction bronchiectasis, ground glass opacities and reticulation.[4]
Other Diagnostic Studies
Pertinent diagnostic studies can be found under the laboratory findings.
Treatment
Medical Therapy
Various immunosuppressive agents, such as azathioprine, mycophenolate mofetil, and/or tacrolimus, are used in the treatment of antisynthetase syndrome. Additionally, corticosteroids may be added for management of the myositis and pulmonary manifestations of anti-synthetase syndrome. The choice of immunosuppressive agent is dependent on the practitioner and is based on the potential risks of therapy as no agent is superior to the other.
Prednisone and azathioprine or mycophenolate mofetil may be used in patients with anti-synthetase syndrome related interstitial lung disease (ILD). In addition to that, tacrolimus may be added for rapid disease control in more severe cases of ILD.
In patients with severe progressive or refractory ILD, rituximab may be added; while cyclophosphamide is reserved for those with acute respiratory distress syndrome.
The physician must also been on the lookout for other co-morbid conditions associated with antisynthetase syndrome i.e. pulmonary hypertension and screening for malignancies.[4]
| Therapies for Anti-synthetase Syndrome-ILD | ||||
|---|---|---|---|---|
| Drug | Clinical Use | Monitoring | Adverse effects* | Suggested Starting Dose |
| Corticosteroids | First-line therapy | Glucose, weight, blood pressure | Hypertension, weight gain, hyperglycemia | 1 mg/kg/day |
| Azathioprine | Most common second-line agent | CBC, renal/liver function | Leukopenia, hepatic injury, pancreatitis | 1 mg/kg/day |
| Mycophenolate mofetil | Second-line agent in addition to corticosteroids | CBC | Diarrhea, cytopenias | 500 mg twice daily |
| Rituximab | Rescue therapy, added to standard immunosuppression | CBC | Infection, neutropenia, infusion reaction | ** |
| Cyclophosphamide | Rescue therapy (e.g. ARDS) | CBC, urinalysis, renal function | Malignancy, cytopenias, hemorrhagic cystitis, sterility | 1–2 mg/kg/day by mouth or 500–1000 mg IV every 4 weeks** |
| Tacrolimus | Add-on therapy | Renal function, blood pressure, electrolytes, CBC, drug level | Renal failure, hypertension, hyperglycemia | 1 mg twice daily |
| IVIG | Add-on therapy | Immunoglobulin G levels | Infusion reaction, infection from donor | ** |
| ILD = Interstitial lung disease; ARDS = acute respiratory distress syndrome; IVIG = intravenous immunoglobulin G; mg = milligram; kg = kilogram
*all except IVIG increase the risk of opportunistic infection **rheumatology consult strongly advised | ||||
Surgery
Surgical intervention is not recommended for the management of antisynthetase syndrome.
Prevention
There are no primary preventive measures available for antisynthetase syndrome.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Maturu VN, Lakshman A, Bal A, Dhir V, Sharma A, Garg M; et al. (2016). "Antisynthetase syndrome: An under-recognized cause of interstitial lung disease". Lung India. 33 (1): 20–6. doi:10.4103/0970-2113.173055. PMC 4748659. PMID 26933302.
- ↑ Robinson D, Scholz B (2020). "The antisynthetase syndrome". Proc (Bayl Univ Med Cent). 33 (3): 401–403. doi:10.1080/08998280.2020.1764818. PMC 7340408 Check
|pmc=value (help). PMID 32675964 Check|pmid=value (help). - ↑ Devi HG, Pasha MM, Padmaja MS, Halappa S (2016). "Antisynthetase Syndrome: A Rare Cause for ILD". J Clin Diagn Res. 10 (3): OD08–9. doi:10.7860/JCDR/2016/16872.7361. PMC 4843302. PMID 27134916.
- ↑ 4.0 4.1 4.2 4.3 Witt LJ, Curran JJ, Strek ME (2016). "The Diagnosis and Treatment of Antisynthetase Syndrome". Clin Pulm Med. 23 (5): 218–226. doi:10.1097/CPM.0000000000000171. PMC 5006392. PMID 27594777.
- ↑ 5.0 5.1 5.2 Cojocaru M, Cojocaru IM, Chicos B (2016). "New Insights into Antisynthetase Syndrome". Maedica (Bucur). 11 (2): 130–135. PMC 5394574. PMID 28461832.
- ↑ https://www.niehs.nih.gov/research/clinical/bethesda/participants/studies/erftas/index.cfm. Missing or empty
|title=(help) - ↑ https://www.sciencedirect.com/science/article/abs/pii/S0049017220303085. Missing or empty
|title=(help) - ↑ Huang K, Aggarwal R (2020). "Antisynthetase syndrome: A distinct disease spectrum". J Scleroderma Relat Disord. 5 (3): 178–191. doi:10.1177/2397198320902667. PMC 8922626 Check
|pmc=value (help). PMID 35382516 Check|pmid=value (help).