MALT lymphoma pathophysiology
|
MALT lymphoma Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
MALT lymphoma pathophysiology On the Web |
|
American Roentgen Ray Society Images of MALT lymphoma pathophysiology |
|
Risk calculators and risk factors for MALT lymphoma pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
MALT lymphoma (MALToma) is a form of lymphoma involving the mucosa-associated lymphoid tissue (MALT), frequently of the stomach, but virtually any mucosal site can be afflicted. It is a cancer originating from B cells in the marginal zone of the MALT
Pathogenesis
MALT lymphoma (MALToma) is a form of lymphoma involving the mucosa-associated lymphoid tissue (MALT), frequently of the stomach, but virtually any mucosal site can be afflicted. It is a cancer originating from B cells in the marginal zone of the MALT
Genetics
A t(11;18)(q21;q21) chromosomal translocation, giving rise to a AP12-MLT fusion gene, is predictive of poor response to eradication therapy. [1]
Two other genetic alterations, t(1;14)(p22;q32) and t(14;18)(q32;q21), which deregulate BCL10 and MALT1-genes respectively, and seem to turn-on the same pathway as API2-MLT (i.e., that of NF-kB).

Associated Conditions
- Gastric MALT lymphoma is frequently associated with chronic inflammation as a result of the presence of Helicobacter pylori (72-98%).[2]
- Chronic immune stimulation is also suspected in the pathogenesis of non-gastric MALT lymphoma, and hence often have a history of autoimmune disorders such as:
Gross Pathology
MALT lymphoma starts in the tissues or organs outside of the lymph nodes (extranodal). MALT lymphoma develops in mucosa-associated lymphoid tissue, in the mucosa, or tissue that lines body organs or body cavities including:[3]
- Gastrointestinal tract
- The stomach is the most common location for MALT lymphoma, but they can also occur in the small bowel and colon.
- Lungs
- Eyes, including the orbit
- Skin
- Salivary glands
- Thyroid gland
- Breasts
| MALT lymphoma pathophysiology | |
 | |
|---|---|
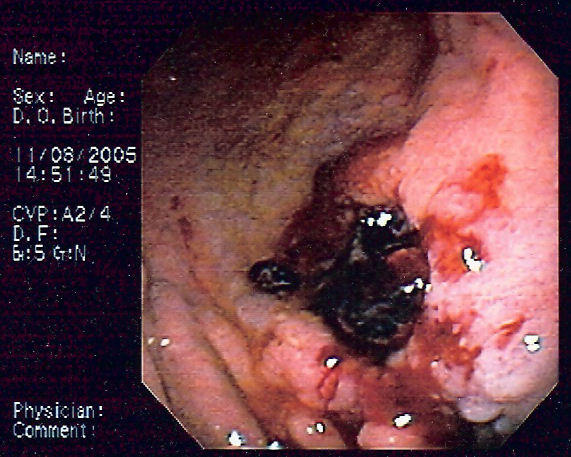
| Endoscopic image of gastric MALT lymphoma taken in body of stomach in patient who presented with upper GI hemorrhage. Appearance is similar to gastric ulcer with adherent clot. |
Microscopic pathology
Histologically, there is expansion of the marginal zone compartment with development of sheets of neoplastic small lymphoid cells.[4] The morphology of the neoplastic cells is variable with small mature lymphocytes, cells resembling centrocytes (centrocyte like cells), or marginal zone/monocytoid B cells. Plasmacytoid or plasmacytic differentiation is frequent. Lymphoid follicles are ubiquitous to MALT lymphoma but may be indistinct as they are often overrun or colonized by the neoplastic cells. Large transformed B cells are present scattered among the small cell population. If these large cells are present in clusters or sheets, a diagnosis of associated large B-cell lymphoma should be considered. A characteristic feature of MALT lymphoma is the presence of neoplastic cells within epithelial structures with associated destruction of the glandular architecture to form lymphoepithelial lesions.[5]
References
- ↑ Liu H, Ruskon-Fourmestraux A, Lavergne-Slove A, Ye H, Molina T, Bouhnik Y, Hamoudi R, Diss T, Dogan A, Megraud F, Rambaud J, Du M, Isaacson P (2001). "Resistance of t(11;18) positive gastric mucosa-associated lymphoid tissue lymphoma to Helicobacter pylori eradication therapy". Lancet. 357 (9249): 39–40. PMID 11197361.
- ↑ Parsonnet J, Hansen S, Rodriguez L, Gelb A, Warnke R, Jellum E, Orentreich N, Vogelman J, Friedman G (1994). "Helicobacter pylori infection and gastric lymphoma". N Engl J Med. 330 (18): 1267–71. PMID 8145781.
- ↑ Extranodal marginal zone of mucosa-associated lymphoid tissue (MALT lymphoma). Canadian Cancer Society 2016. http://www.cancer.ca/en/cancer-information/cancer-type/non-hodgkin-lymphoma/non-hodgkin-lymphoma/types-of-nhl/malt-lymphoma/?region=on. Accessed on January 28, 2016
- ↑ Taal, B G; Boot, H; van Heerde, P; de Jong, D; Hart, A A; Burgers, J M (1 October 1996). "Primary non-Hodgkin lymphoma of the stomach: endoscopic pattern and prognosis in low versus high grade malignancy in relation to the MALT concept". Gut. 39 (4): 556–561. doi:10.1136/gut.39.4.556.
- ↑ Janusz, edited by Jankowski, (2012). Handbook of Gastrointestinal Cancer (2 ed.). Chicester: John Wiley and Sons Ltd. pp. 243–244. ISBN 978-0-470-65624-2.