Pituitary apoplexy pathophysiology
|
Pituitary apoplexy Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Pituitary apoplexy pathophysiology On the Web |
|
American Roentgen Ray Society Images of Pituitary apoplexy pathophysiology |
|
Risk calculators and risk factors for Pituitary apoplexy pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Akshun Kalia M.B.B.S.[2]
Overview
Pituitary apoplexy is an acute clinical syndrome caused by hemorrhage and necrosis in the pituitary gland. Most commonly, pituitary apoplexy is associated with pituitary adenoma. The pituitary adenoma predisposes the patient to an increased risk of bleeding within the pituitary gland. The pituitary adenoma has fenestrated endothelium surrounded by a variable number of smooth muscle cells, which are not found in the normal pituitary gland.Gene involved in the pathogenesis of pituitary apoplexy include a mutation in AIP gene, which is located on chromosome 11q13.2. On gross pathology, pituitary apoplexy presents with hemorrhage with or without necrosis. Electron microscopic shows evidence of abnormal fenestration of tumor vessels (pituitary adenoma) with fragmented basal membranes that may predispose the patient to hemorrhage.
Pathophysiology
Pituitary apoplexy is caused by bleeding into the pituitary gland. Most often, pituitary apoplexy is seen with a pituitary adenoma. Pituitary adenoma predisposes the patient to an increased risk of bleeding within the pituitary gland.[1][2][3][4][5][6][7][8]
- In addition, these pituitary adenomas have decreased blood supply and angiogenesis.
- Pituitary adenoma has fenestrated endothelium surrounded by a variable number of smooth muscle cells, which are not found in the normal pituitary gland.
- VEGF mRNA may be increased in pituitary tumors, especially in non-functioning pituitary adenomas, which could be related to an abnormal vascularization.
- Enlarging pituitary adenomas may outgrow their blood supply, making them susceptible to bleeding and infarction.
- The bleeding may lead to increase in intrasellar pressure. The increased intrasellar pressure may compress the adjoining structures and lead to the clinical symptoms of pituitary apoplexy.
- An enlarged pituitary tumor may become impacted at the diaphragmatic notch, leading to compression of the hypophyseal stalk and its vascular supply.
- This may render the anterior pituitary gland and its tumor with reduced blood supply causing ischemia and subsequent necrosis.
- Reperfusion after infarction may lead to hemorrhage within the pituitary gland or adenoma.
Genetics
- Gene involved in the pathogenesis of pituitary apoplexy include a mutation in AIP gene, which is located on chromosome 11q13.2.
- The most common mutation site in the AIP gene is p.R304 locus.
- Mutated AIP loses its activity as a tumor suppressor gene and leads to increased proliferation.
- The penetration of AIP positive carriers is 12-30%.
Associated Conditions
Pituitary apoplexy is seen with 0.6 to 10% of pituitary adenomas.
Gross Pathology
- The predominant finding is hemorrhage with or without necrosis.
- Pale, necrotic material is particularly found when there is a long interval between the acute clinical event and surgery.
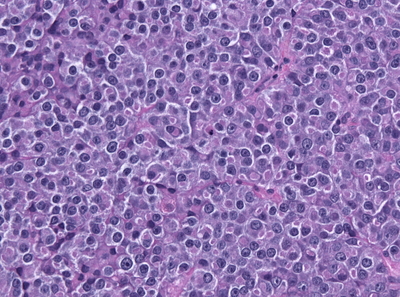
Microscopic Pathology
Electron microscopic shows evidence of abnormal fenestration of tumor vessels (pituitary adenoma) with fragmented basal membranes that may predispose the patient to hemorrhage.
References
- ↑ Nielsen EH, Lindholm J, Bjerre P, Christiansen JS, Hagen C, Juul S, Jørgensen J, Kruse A, Laurberg P (2006). "Frequent occurrence of pituitary apoplexy in patients with non-functioning pituitary adenoma". Clin. Endocrinol. (Oxf). 64 (3): 319–22. doi:10.1111/j.1365-2265.2006.02463.x. PMID 16487443.
- ↑ Chacko AG, Chacko G, Seshadri MS, Chandy MJ (2002). "Hemorrhagic necrosis of pituitary adenomas". Neurol India. 50 (4): 490–3. PMID 12577104.
- ↑ Zayour DH, Selman WR, Arafah BM (2004). "Extreme elevation of intrasellar pressure in patients with pituitary tumor apoplexy: relation to pituitary function". J Clin Endocrinol Metab. 89 (11): 5649–54. doi:10.1210/jc.2004-0884. PMID 15531524.
- ↑ Oldfield EH, Merrill MJ (2015). "Apoplexy of pituitary adenomas: the perfect storm". J Neurosurg. 122 (6): 1444–9. doi:10.3171/2014.10.JNS141720. PMID 25859802.
- ↑ Schechter J (1972). "Ultrastructural changes in the capillary bed of human pituitary tumors". Am J Pathol. 67 (1): 109–26. PMC 2032586. PMID 5055626.
- ↑ Schechter J, Goldsmith P, Wilson C, Weiner R (1988). "Morphological evidence for the presence of arteries in human prolactinomas". J Clin Endocrinol Metab. 67 (4): 713–9. doi:10.1210/jcem-67-4-713. PMID 3417848.
- ↑ Nawar RN, AbdelMannan D, Selman WR, Arafah BM (2008). "Pituitary tumor apoplexy: a review". J Intensive Care Med. 23 (2): 75–90. doi:10.1177/0885066607312992. PMID 18372348.
- ↑ Findling JW, Tyrrell JB, Aron DC, Fitzgerald PA, Wilson CB, Forsham PH (1981). "Silent pituitary apoplexy: subclinical infarction of an adrenocorticotropin-producing pituitary adenoma". J. Clin. Endocrinol. Metab. 52 (1): 95–7. doi:10.1210/jcem-52-1-95. PMID 6256408.