Sandbox: Lymphadenopathy: Difference between revisions
No edit summary |
|||
| Line 8: | Line 8: | ||
==Classification== | ==Classification== | ||
*Lymphadenopathy may be classified according to distribution into 2 groups: | *Lymphadenopathy may be classified according to distribution into 2 groups: | ||
Revision as of 15:47, 6 May 2016
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Maria Fernanda Villarreal, M.D. [2]
Synonyms and keywords: Lymph nodes enlarged; Enlarged lymph nodes; Lymphadenitis; Swollen lymph nodes; Swollen/enlarged lymph nodes
Overview
Classification
- Lymphadenopathy may be classified according to distribution into 2 groups:
- Generalized lymphadenopathy
- Localized lymphadenopathy
Pathophysiology
- The pathogenesis of lymphadenopathy is characterized by [feature1], [feature2], and [feature3].
- On gross pathology, characteristic findings of lymphadenopathy, include:
- On microscopic histopathological analysis, characteristic findings of lymphadenopathy will depend on the aetiology.
- Common findings, include:
Non-specific reactive follicular hyperplasia (NSRFH)
- Large spaced cortical follicles
- Tingible body macrophages, normal dark/light GC pattern
Lymph node metastasis
- Foreign cell population (usually in subcapsular sinuses)
- +/-nuclear atypia
- +/-malignant architecture
Toxoplasmosis
- Large follicles
- Epithelioid cells perifollicular & intrafollicular
- Reactive GCs
- Monocytoid cell clusters
Cat-scratch disease
- PMNs in necrotic area
- "Stellate" (or serpentine) shaped micro-abscesses
- Presence of granulomas
Dermatopathic lymphadenopathy
- Melanin-laden histiocytes
- Histiocytosis
Systemic lupus erythematosus lymphadenopathy
- Blue hematoxylin bodies
- Necrosis
- No PMNs
Causes
- Common causes of lymphadenopathy, include:
- Infections (acute suppurative)
- Fungal
- Mycobacterial
- Viral
- Protozoal (e.g. toxoplasma)
- Bacterial (e.g. chlamydia, rickettsia, bartonella)
- Reactive
- Follicular hyperplasia
- Paracortical hyperplasia
- Sinus histiocytosis
- Granulomatous
- Neoplastic
- Drugs (e.g. cyclosporin, phenytoin, methotrexate)
- Lipid storage diseases
- IgG4-related sclerosing disease
Epidemiology and Demographics
- Lymphadenopathy is very common.
- The prevalence of lymphadenopathy is approximately [number or range] per 100,000 individuals worldwide.
- The estimated incidence of lymphadenopathy among children in the United States ranges from 35%- 45%.
Age
- Patients of all age groups may develop lymphadenopathy.
Gender
- Lymphadenopathy affects men and women equally.
Race
- There is no racial predilection for lymphadenopathy.
Risk Factors
- Common risk factors in the development of lymphadenopathy are [risk factor 1], [risk factor 2], [risk factor 3], and [risk factor 4].
Natural History, Complications and Prognosis
- The majority of patients with lymphadenopathy remain asymptomatic for [duration/years].
- Early clinical features include [manifestation 1], [manifestation 2], and [manifestation 3].
- If left untreated, [#%] of patients with lymphadenopathy may progress to develop [manifestation 1], [manifestation 2], and [manifestation 3].
Common complications of lymphadenopathy, include:
Mediastinal lymphadenopathy
- Superior vena cava syndrome
- Tracheal and bronchial obstruction
- Dysphagia
- Hemoptysis
- Uric acid nephropathy
- Hyperkalemia
- Hypercalcemia
- Hypocalcemia
- Hyperphosphatemia
- Renal failure
Abdominal lymphadenopathy
Superficial lymphadenopathy
- Abscess formation
- Cellulitis
- Fistulas (seen in lymphadenitis that is due to tuberculosis)
- Sepsis
Prognosis is generally [excellent/good/poor], and the [1/5/10year mortality/survival rate] of patients with lymphadenopathy is approximately [#%].
Diagnosis
Diagnostic Criteria
- The diagnosis of lymphadenopathy is made when at least [number] of the following [number] diagnostic criteria are met:
- [criterion 1]
- [criterion 2]
- [criterion 3]
- [criterion 4]
Symptoms
- Symptoms of lymphadenopathy may include the following:
- A directed history should be obtained to ascertain:
- Use of drugs causing lymphadenopathy
- Travel to endemic areas
- Occupational risk (e.g. Fishermen, slaughterhouse workers, hunters, trappers)
- High risk behavior or high risk sexual behaviors (e.g. I.V drug abuse, multiple partners)
Physical Examination
- Patients with lymphadenopathy may have a pale or normal appearance.
- Physical examination may be remarkable for:
Vitals
- Temperature
- High grade fever
- Low grade fever
- Pulse
- Rapid (e.g. acute infections)
Skin
- Rash may be present
- Color change (indicative of inflammation)
- Skin fistula draining pus may be present
- Ulcers
Head
Palpating Anterior Cervical Lymph Nodes
Lymph nodes should be examined in the following order:
- Anterior Cervical
- Posterior Cervical
- Tonsillar
- Sub-Mandibular
- Sub-Mental
- Supra-clavicular
Characteristics to be noted while palpating lymph nodes:
- Size
- Pain/ tenderness
- Increased tenderness (e.g infected lymph nodes)
- Consistency
- Matting
Gallery
-
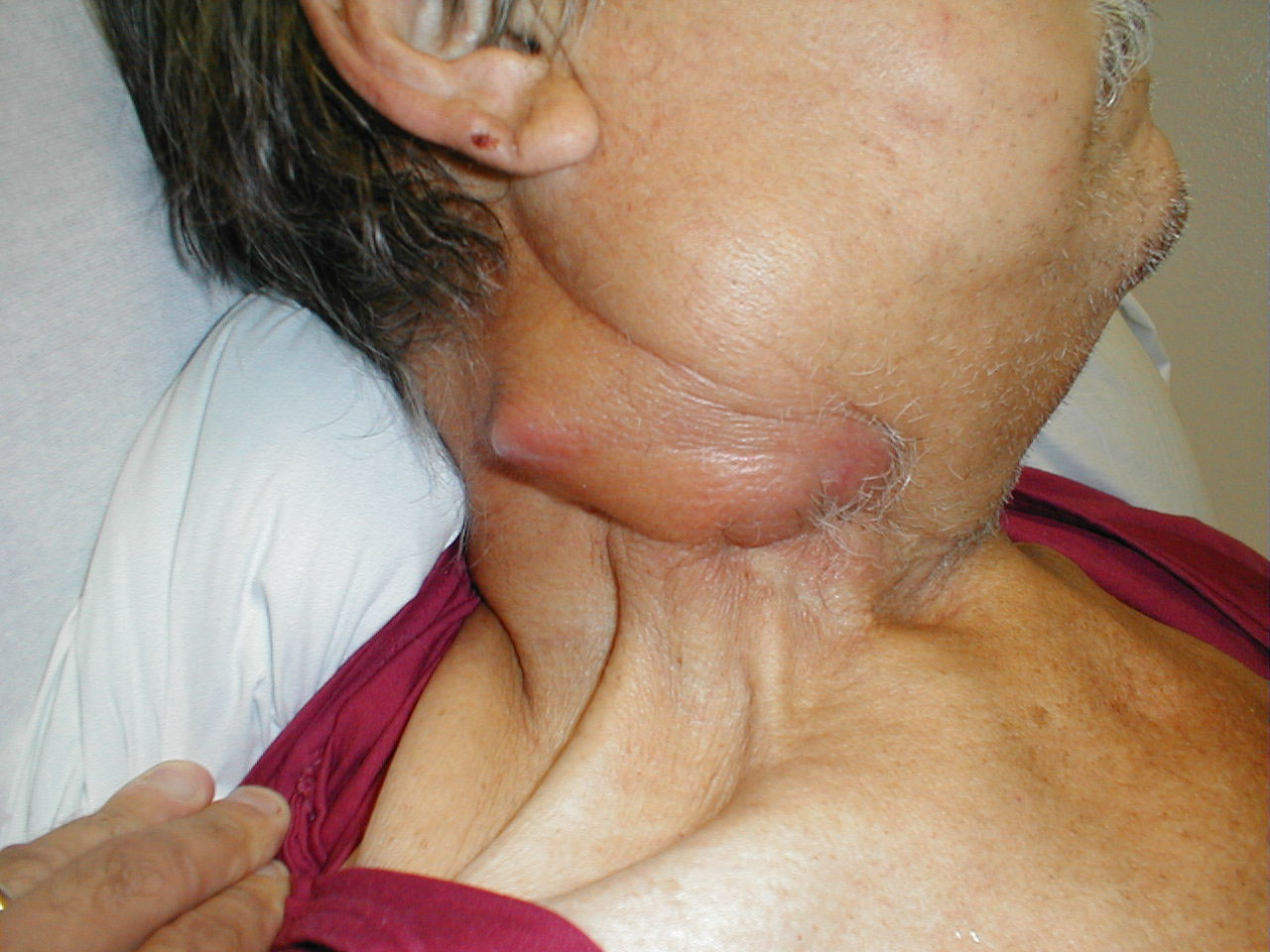
Cervical adenopathy: massive right side cervical adenopathy and facial asymmetry due to metastatic, intraoral squamous cell cancer. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
Cervical adenopathy: massive right side cervical adenopathy and facial asymmetry due to metastatic, intraoral squamous cell cancer. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.I
-
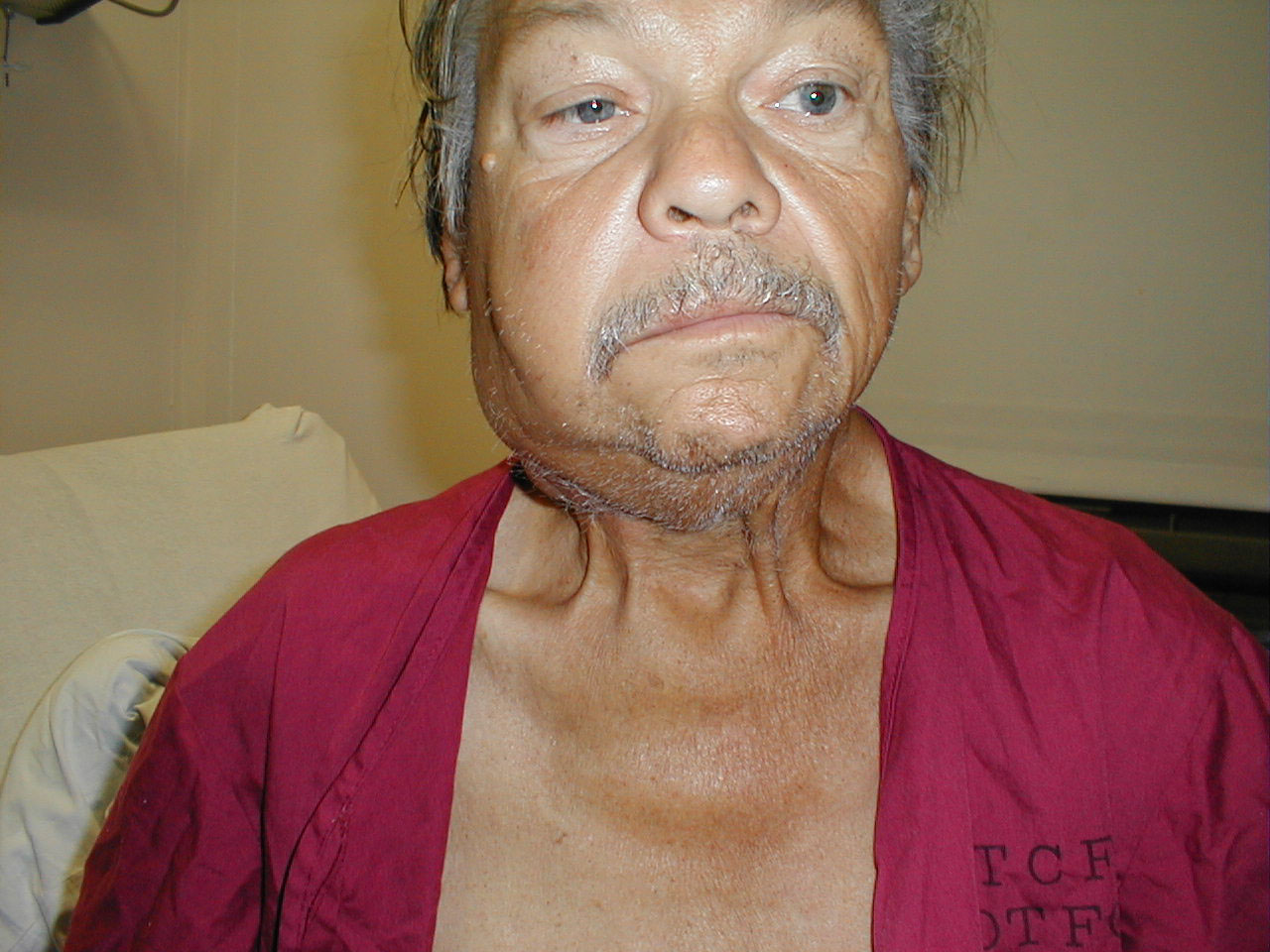
Cervical adenopathy: large right anterior cervical lymph node. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
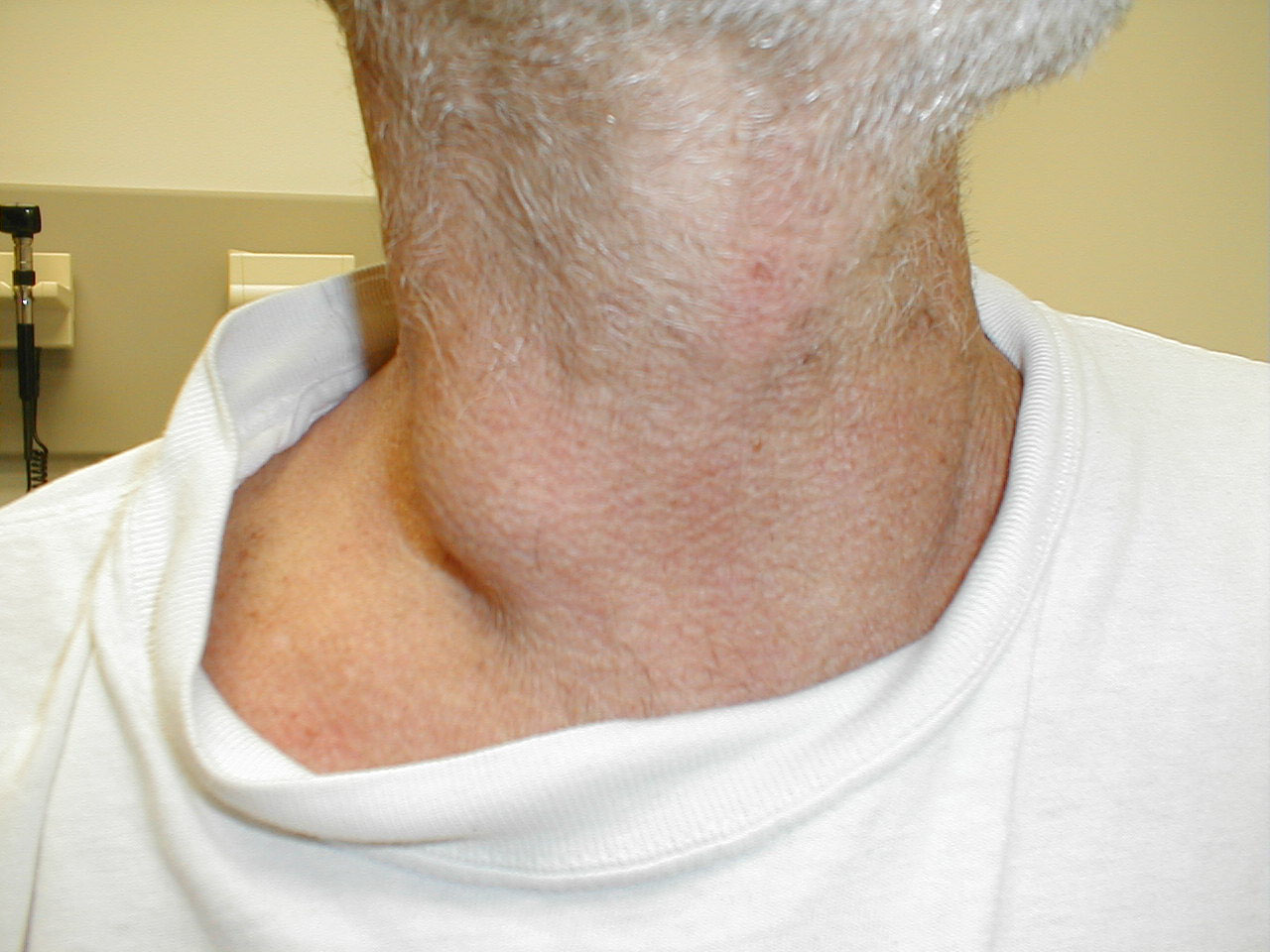
Cervical lymphadenopathy. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
-
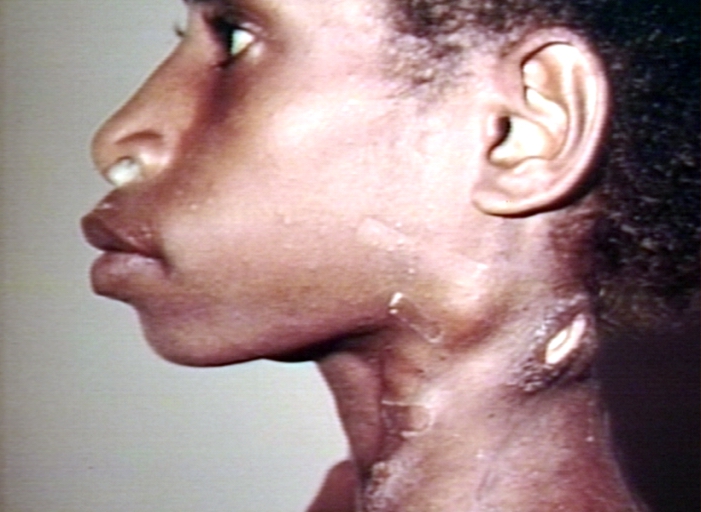
Cervical Adenopathy: multiple right sided cervical lymph nodes. Images Courtesy of Charlie Goldberg, M.D., UCSD School of Medicine and VA Medical Center, San Diego, CA.
Laboratory Findings
- There are no specific laboratory findings associated with [disease name].
- A [positive/negative] [test name] is diagnostic of [disease name].
- An [elevated/reduced] concentration of [serum/blood/urinary/CSF/other] [lab test] is diagnostic of [disease name].
- Other laboratory findings consistent with the diagnosis of [disease name] include [abnormal test 1], [abnormal test 2], and [abnormal test 3].
Imaging Findings
- There are no [imaging study] findings associated with [disease name].
- [Imaging study 1] is the imaging modality of choice for [disease name].
- On [imaging study 1], [disease name] is characterized by [finding 1], [finding 2], and [finding 3].
- [Imaging study 2] may demonstrate [finding 1], [finding 2], and [finding 3].
Other Diagnostic Studies
- [Disease name] may also be diagnosed using [diagnostic study name].
- Findings on [diagnostic study name] include [finding 1], [finding 2], and [finding 3].
Treatment
Medical Therapy
- There is no treatment for [disease name]; the mainstay of therapy is supportive care.
- The mainstay of therapy for [disease name] is [medical therapy 1] and [medical therapy 2].
- [Medical therapy 1] acts by [mechanism of action1].
- Response to [medical therapy 1] can be monitored with [test/physical finding/imaging] every [frequency/duration].
Surgery
- Surgery is the mainstay of therapy for [disease name].
- [Surgical procedure] in conjunction with [chemotherapy/radiation] is the most common approach to the treatment of [disease name].
- [Surgical procedure] can only be performed for patients with [disease stage] [disease name].
Prevention
- There are no primary preventive measures available for [disease name].
- Effective measures for the primary prevention of [disease name] include [measure1], [measure2], and [measure3].
- Once diagnosed and successfully treated, patients with [disease name] are followed-up every [duration]. Follow-up testing includes [test 1], [test 2], and [test 3].