Pulmonary nodule CT: Difference between revisions
Jump to navigation
Jump to search
No edit summary |
|||
| Line 6: | Line 6: | ||
==CT== | ==CT== | ||
'''Calcification''' | |||
===Nodules | *Calcification patterns are commonly seen in granulomatous disease and hamartomas | ||
==== | *Characteristic calcification patterns of pulmonary nodule, include: | ||
:*Diffuse | |||
* If less than 8 mm, use guidelines | :*Central | ||
:*Laminated | |||
:*Popcorn | |||
'''Size''' | |||
*Different size ranges of pulmonary nodule, include: | |||
:* Nodules less than 4mm | |||
:* Nodules between 4mm and 7mm | |||
:* Nodules between 8mm and 20mm | |||
:* Nodules more than 20mm | |||
'''Growth''' | |||
*The growth pattern of the pulmonary nodule plays an important role in the management strategy.<ref name="pmid22156993">{{cite journal |vauthors=Ko JP, Berman EJ, Kaur M, Babb JS, Bomsztyk E, Greenberg AK, Naidich DP, Rusinek H |title=Pulmonary Nodules: growth rate assessment in patients by using serial CT and three-dimensional volumetry |journal=Radiology |volume=262 |issue=2 |pages=662–71 |year=2012 |pmid=22156993 |pmc=3267080 |doi=10.1148/radiol.11100878 |url=}}</ref> | |||
*Nodule growth should be evaluated on a individual basis and based on the risk assessment score | |||
* A 4x growth is associated with a 50% risk of malignancy<ref name="pmid22156993">{{cite journal |vauthors=Ko JP, Berman EJ, Kaur M, Babb JS, Bomsztyk E, Greenberg AK, Naidich DP, Rusinek H |title=Pulmonary Nodules: growth rate assessment in patients by using serial CT and three-dimensional volumetry |journal=Radiology |volume=262 |issue=2 |pages=662–71 |year=2012 |pmid=22156993 |pmc=3267080 |doi=10.1148/radiol.11100878 |url=}}</ref> | |||
'''Shape''' | |||
*Polygonal | |||
*Circular | |||
*Spherical | |||
'''Margins''' | |||
*Lobulated or scalloped margins | |||
:*Intermediate malignancy probability | |||
*Smooth margins | |||
*:Associated with nodule benignancy | |||
'''Attenuation''' | |||
*Different types of attenuation for pulmonary nodule, include: | |||
*Solid pulmonary nodules | |||
:*Malignancy rate of only 7% | |||
*Calcified pulmonary nodules | |||
*Partly solid pulmonary nodules | |||
:*Malignancy rate of 63% | |||
*Ground glass pulmonary nodules | |||
:*Malignancy rate of 18% | |||
'''Contrast enhancement''' | |||
* Contrast enhancement of pulmonary nodules may be useful to determine benign or malignant features | |||
* Benign pulmonary nodules usually have a contrast enhancement less than 15 HU | |||
On CT, radiological signs of pulmonary nodule, include: | |||
*'''Corona radiata sign''': highly associated with malignancy | |||
*'''Air bronchogram sign''': non-specific sign | |||
*'''Halo sign''': zone of ground-glass attenuation surrounding a pulmonary nodule or mass on CT images. | |||
==CT Surveillance== | |||
According to the [[American College of Chest Physicians]] (ACCP) for the CT surveillance of pulmonary nodules, recommends the following:<ref name="pmid23649456">{{cite journal| author=Gould MK, Donington J, Lynch WR, Mazzone PJ, Midthun DE, Naidich DP et al.| title=Evaluation of individuals with pulmonary nodules: when is it lung cancer? Diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines. | journal=Chest | year= 2013 | volume= 143 | issue= 5 Suppl | pages= e93S-120S | pmid=23649456 | doi=10.1378/chest.12-2351 | pmc=PMC3749714 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=23649456 }} </ref> | |||
* If less than 8 mm, use guidelines by the Fleischner society (see table below). | |||
* For nodules greater than 8 mm in diameter, assess the patients risk of complications from thoracic surgery: | * For nodules greater than 8 mm in diameter, assess the patients risk of complications from thoracic surgery: | ||
** If low to moderate risk for complications of surgery, assess probability of cancer by a validated calculation. The model developed at the Mayo Clinic has been the most extensively validated<ref name="pmid9129544">{{cite journal| author=Swensen SJ, Silverstein MD, Ilstrup DM, Schleck CD, Edell ES| title=The probability of malignancy in solitary pulmonary nodules. Application to small radiologically indeterminate nodules. | journal=Arch Intern Med | year= 1997 | volume= 157 | issue= 8 | pages= 849-55 | pmid=9129544 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=9129544 }} </ref>. An open-source version is [https://openrules.ocpu.io/home/www/pulmnodule.html available online]. | ** If low to moderate risk for complications of surgery, assess probability of cancer by a validated calculation. The model developed at the Mayo Clinic has been the most extensively validated<ref name="pmid9129544">{{cite journal| author=Swensen SJ, Silverstein MD, Ilstrup DM, Schleck CD, Edell ES| title=The probability of malignancy in solitary pulmonary nodules. Application to small radiologically indeterminate nodules. | journal=Arch Intern Med | year= 1997 | volume= 157 | issue= 8 | pages= 849-55 | pmid=9129544 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=9129544 }} </ref>. An open-source version is [https://openrules.ocpu.io/home/www/pulmnodule.html available online]. | ||
| Line 20: | Line 69: | ||
|+ Fleischner society guidelines for follow-up and management of nodules <8 mm Detected Incidentally at non-screening CT<ref name="pmid16244247">{{cite journal| author=MacMahon H, Austin JH, Gamsu G, Herold CJ, Jett JR, Naidich DP et al.| title=Guidelines for management of small pulmonary nodules detected on CT scans: a statement from the Fleischner Society. | journal=Radiology | year= 2005 | volume= 237 | issue= 2 | pages= 395-400 | pmid=16244247 | doi=10.1148/radiol.2372041887 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=16244247 }} </ref> | |+ Fleischner society guidelines for follow-up and management of nodules <8 mm Detected Incidentally at non-screening CT<ref name="pmid16244247">{{cite journal| author=MacMahon H, Austin JH, Gamsu G, Herold CJ, Jett JR, Naidich DP et al.| title=Guidelines for management of small pulmonary nodules detected on CT scans: a statement from the Fleischner Society. | journal=Radiology | year= 2005 | volume= 237 | issue= 2 | pages= 395-400 | pmid=16244247 | doi=10.1148/radiol.2372041887 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=16244247 }} </ref> | ||
! Nodule Size (mm) | ! Nodule Size (mm) | ||
! | ! Low risk patients† | ||
! | ! High risk patients‡ | ||
|- | |- | ||
| <= 4 | | <= 4 | ||
| Line 42: | Line 91: | ||
|} | |} | ||
==== | ==Gallery== | ||
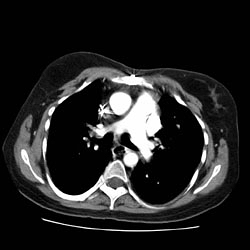
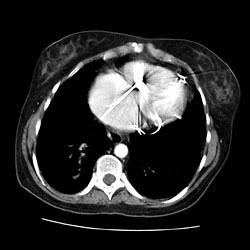
[[Image:Pulmonary AVM as nodule 2.jpg|thumb|center|Thorax CT]] | [[Image:Pulmonary AVM as nodule 2.jpg|thumb|center|Thorax CT]] | ||
| Line 69: | Line 115: | ||
</gallery> | </gallery> | ||
</div> | </div> | ||
Revision as of 16:23, 18 March 2016
|
Pulmonary Nodule Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Pulmonary nodule CT On the Web |
|
American Roentgen Ray Society Images of Pulmonary nodule CT |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Maria Fernanda Villarreal, M.D. [2]
Overview
CT
Calcification
- Calcification patterns are commonly seen in granulomatous disease and hamartomas
- Characteristic calcification patterns of pulmonary nodule, include:
- Diffuse
- Central
- Laminated
- Popcorn
Size
- Different size ranges of pulmonary nodule, include:
- Nodules less than 4mm
- Nodules between 4mm and 7mm
- Nodules between 8mm and 20mm
- Nodules more than 20mm
Growth
- The growth pattern of the pulmonary nodule plays an important role in the management strategy.[1]
- Nodule growth should be evaluated on a individual basis and based on the risk assessment score
- A 4x growth is associated with a 50% risk of malignancy[1]
Shape
- Polygonal
- Circular
- Spherical
Margins
- Lobulated or scalloped margins
- Intermediate malignancy probability
- Smooth margins
- Associated with nodule benignancy
Attenuation
- Different types of attenuation for pulmonary nodule, include:
- Solid pulmonary nodules
- Malignancy rate of only 7%
- Calcified pulmonary nodules
- Partly solid pulmonary nodules
- Malignancy rate of 63%
- Ground glass pulmonary nodules
- Malignancy rate of 18%
Contrast enhancement
- Contrast enhancement of pulmonary nodules may be useful to determine benign or malignant features
- Benign pulmonary nodules usually have a contrast enhancement less than 15 HU
On CT, radiological signs of pulmonary nodule, include:
- Corona radiata sign: highly associated with malignancy
- Air bronchogram sign: non-specific sign
- Halo sign: zone of ground-glass attenuation surrounding a pulmonary nodule or mass on CT images.
CT Surveillance
According to the American College of Chest Physicians (ACCP) for the CT surveillance of pulmonary nodules, recommends the following:[2]
- If less than 8 mm, use guidelines by the Fleischner society (see table below).
- For nodules greater than 8 mm in diameter, assess the patients risk of complications from thoracic surgery:
- If low to moderate risk for complications of surgery, assess probability of cancer by a validated calculation. The model developed at the Mayo Clinic has been the most extensively validated[3]. An open-source version is available online.
- If high risk for complications of surgery, assess probability of cancer by a validated calculation. If low to moderate risk of cancer follow up with CT scan surveillance. If moderate to high risk of cancer obtain non-surgical biopsy.
| Nodule Size (mm) | Low risk patients† | High risk patients‡ |
|---|---|---|
| <= 4 | No follow-up needed. | Follow-up at 12 months. If no change, no further imaging needed. |
| >4 - 6 | Follow-up at 12 months. If no change, no further imaging needed. | Initial follow-up CT at 6 -12 months and then at 18 - 24 months if no change. |
| >6 - 8 | Initial follow-up CT at 6 -12 months and then at 18 - 24 months if no change. | Initial follow-up CT at 3 - 6 months and then at 9 -12 and 24 months if no change. |
| >8 | Follow-up CTs at around 3, 9, and 24 months. Dynamic contrast enhanced CT, PET, and/or biopsy. | Same at for low risk patients. |
| † Low risk patients: Minimal or absent history of smoking and of other known risk factors. ‡ High risk patients: History of smoking or of other known risk factors. | ||
Gallery

References
- ↑ 1.0 1.1 Ko JP, Berman EJ, Kaur M, Babb JS, Bomsztyk E, Greenberg AK, Naidich DP, Rusinek H (2012). "Pulmonary Nodules: growth rate assessment in patients by using serial CT and three-dimensional volumetry". Radiology. 262 (2): 662–71. doi:10.1148/radiol.11100878. PMC 3267080. PMID 22156993.
- ↑ Gould MK, Donington J, Lynch WR, Mazzone PJ, Midthun DE, Naidich DP; et al. (2013). "Evaluation of individuals with pulmonary nodules: when is it lung cancer? Diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines". Chest. 143 (5 Suppl): e93S–120S. doi:10.1378/chest.12-2351. PMC 3749714. PMID 23649456.
- ↑ Swensen SJ, Silverstein MD, Ilstrup DM, Schleck CD, Edell ES (1997). "The probability of malignancy in solitary pulmonary nodules. Application to small radiologically indeterminate nodules". Arch Intern Med. 157 (8): 849–55. PMID 9129544.
- ↑ MacMahon H, Austin JH, Gamsu G, Herold CJ, Jett JR, Naidich DP; et al. (2005). "Guidelines for management of small pulmonary nodules detected on CT scans: a statement from the Fleischner Society". Radiology. 237 (2): 395–400. doi:10.1148/radiol.2372041887. PMID 16244247.