Peak flow meter

|
WikiDoc Resources for Peak flow meter |
|
Articles |
|---|
|
Most recent articles on Peak flow meter Most cited articles on Peak flow meter |
|
Media |
|
Powerpoint slides on Peak flow meter |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Peak flow meter at Clinical Trials.gov Trial results on Peak flow meter Clinical Trials on Peak flow meter at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Peak flow meter NICE Guidance on Peak flow meter
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Peak flow meter Discussion groups on Peak flow meter Patient Handouts on Peak flow meter Directions to Hospitals Treating Peak flow meter Risk calculators and risk factors for Peak flow meter
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Peak flow meter |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
A peak flow meter is a small, hand-held device used to manage asthma by monitoring airflow through the bronchi and thus the degree of restriction in the airways.
Function
The peak flow meter measures the patient's maximum ability to expel air from the lungs, or peak expiratory flow rate (PEFR or PEF). Peak flow readings are higher when patients are well, and lower when the airways are constricted. From changes in recorded values, patients and doctors may determine lung functionality, severity of asthma symptoms, and treatment options.
The measurement of peak expiratory flow was pioneered by Dr. Basil Martin Wright, who produced the first meter specifically designed to measure this index of lung function. Since the original design of instrument was introduced in the late 1950s, and the subsequent development of a more portable, lower cost version (the 'Mini-Wright' peak flow meter), other designs and copies have become available across the world.
Measurement of PEFR requires training to correctly use a meter and the normal expected value depends on a patient's sex, age and height. It is classically reduced in obstructive lung disorders such as asthma.
Scales
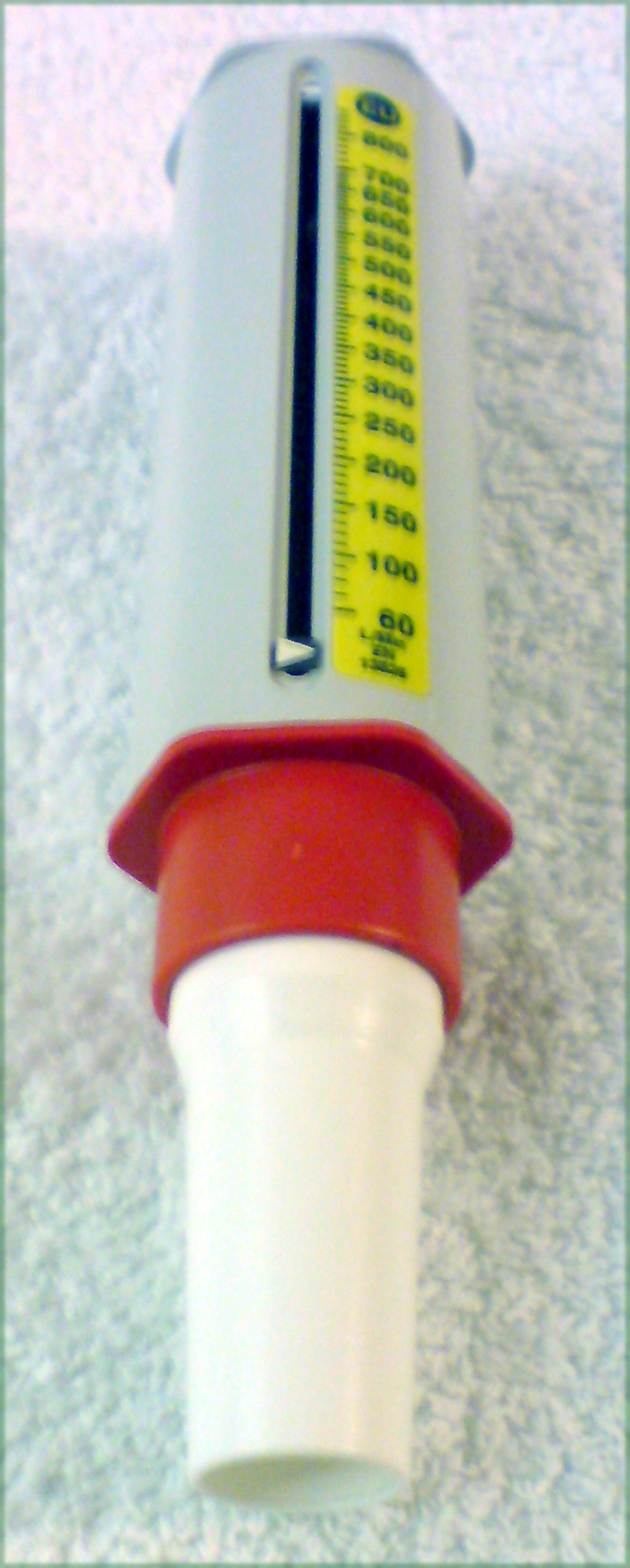
There are a number of non-equivalent scales used in the measurement of Peak Flow.[1]
Graphs or tables are available of predicted normal values based on a person's gender, age and height. It should be noted that there is a wide natural variation in results from healthy test subjects.
- Wright scale[2][3]
- EN 13826 or EU scale[4]
- A.T.S. (American Thoracic Society) scale
In 2004 the UK switched from the original Wright scale to the newer, more accurate European scale. Limited information on converting between the scales exists.[5]
Measurement
The best of three readings is used as the recorded value of the Peak Expiratory Flow Rate. It may be plotted out on graph paper charts together with a record of symptoms or using peak flow charting software.[6] This allows patients to self-monitor and pass information back to their doctor or nurse.[7]
Peak flow readings are often classified into 3 zones of measurement according to the American Lung Association[8]; green, yellow, and red. The color system is based on the colors of street traffic lights. Doctors and health practitioners can develop an asthma management plan based on the green-yellow-red zones.
The Green Zone means 80 to 100 percent of the usual or normal peak flow readings are clear. A peak flow reading in the green zone indicates that the asthma is under good control.
The Yellow Zone means 50 to 80 percent of the usual or normal peak flow readings indicate caution. It may mean respiratory airways are narrowing and additional medication may be required.
The Red Zone means less than 50 percent of the usual or normal peak flow readings indicate a medical emergency. Severe airway narrowing may be occurring and immediate action needs to be taken. This would usually involve contacting a doctor or hospital.
Related Chapters
References
- ↑ Martin R. Miller (2004). "Peak expiratory flow meter scale changes: implications for patients and health professionals" (PDF). The Airways Journal. 2 (2): 80. Unknown parameter
|month=ignored (help) - ↑ Nunn A, Gregg I (1989). "New regression equations for predicting peak expiratory flow in adults". BMJ. 298 (6680): 1068–70. PMID 2497892. - Predicted peak expiratory flow in normal adults using Wright-scale
- ↑ Godfrey S, Kamburoff PL, Naim JL (1970). "Spirometry, lung volumes and airway resistance in normal children ages 5 to 18". Br J Dis Chest. 64: 15–24. - Predicted peak expiratory flow in normal children using Wright-scale
- ↑ Clement Clarke International (2004). "Predictive Normal Values (Nomogram, EU scale)". Clement Clarke International. - Downloadable PDF charts for adults and children using EU scale
- ↑ Clement Clarke International (2004). "Mini-Wright Peak Flow Meter - Wright to EU (EN13826) converter" (EXE macromedia flash). Clement Clarke International.
- ↑ Template:Cite website
- ↑ Scottish Intercollegiate Guidelines Network & The British Thoracic Society (2003). "British Guideline on the Management of Asthma - Annex 8: Personal Asthma Action Plan" (PDF). Thorax. 58: Suppl I. - for recording chart of PEFR readings
- ↑ Template:Cite website