Lanthanum carbonate
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Rabin Bista, M.B.B.S. [2]; Turky Alkathery, M.D. [3]
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Lanthanum carbonate is a phosphate binder that is FDA approved for the treatment of high serum phosphate in patients with end stage renal disease (ESRD). Common adverse reactions include nausea,vomiting, diarrhea, and abdominal pain.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Indications
- Lanthanum carbonate is a phosphate binder indicated to reduce serum phosphate in patients with end stage renal disease (ESRD).
- Management of elevated serum phosphorus levels in end stage renal disease patients usually includes all of the following: reduction in dietary intake of phosphate, removal of phosphate by dialysis and reduction of intestinal phosphate absorption with phosphate binders.
Dosage
- Divide the daily dose of lanthanum carbonate and take with or immediately after food. The recommended initial total daily dose of lanthanum carbonate is 1500 mg. Titrate the dose every 2-3 weeks until an acceptable serum phosphate level is reached. Monitor serum phosphate levels as needed during dose titration and on a regular basis thereafter.
- In clinical studies of ESRD patients, lanthanum carbonate doses up to 4500 mg were evaluated. Most patients required a total daily dose between 1500 mg and 3000 mg to reduce plasma phosphate levels to less than 6.0 mg/dL. Doses were generally titrated in increments of 750 mg/day.
- Chew tablets completely before swallowing. To aid in chewing, tablets may be crushed. Do not swallow intact tablets.
- Consider potential drug interactions when prescribing lanthanum carbonate
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
- There is limited information regarding Off-Label Guideline-Supported Use of Lanthanum in adult patients.
Non–Guideline-Supported Use
- There is limited information regarding Off-Label Non–Guideline-Supported Use of Lanthanum in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
- Safety and effectiveness in pediatric patients have not been established.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
- There is limited information regarding Off-Label Guideline-Supported Use of Lanthanum in pediatric patients.
Non–Guideline-Supported Use
- There is limited information regarding Off-Label Non–Guideline-Supported Use of Lanthanum in pediatric patients.
Contraindications
Warnings
Gastrointestinal Adverse Effects
- There have been reports of serious cases of gastrointestinal obstruction, ileus, and fecal impaction reported in association with lanthanum, some requiring surgery or hospitalization.
- Risk factors for gastrointestinal obstruction identified from post-marketing reports include alteration in gastrointestinal anatomy (e.g., history of gastrointestinal surgery, colon cancer), hypomotility disorders (e.g., constipation, ileus, diabetes) and concomitant medications (e.g., calcium channel blockers). Some cases were reported in patients with no history of gastrointestinal disease.
- Advise patients to chew the tablet thoroughly to reduce the risk of adverse gastrointestinal events.
- Patients with acute peptic ulcer, ulcerative colitis, Crohn's disease or bowel obstructionwere not included in lanthanum carbonate clinical studies.
Diagnostic Tests
- Lanthanum carbonate has radio-opaque properties and therefore may give the appearance typical of an imaging agent during abdominal X-ray procedures.
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
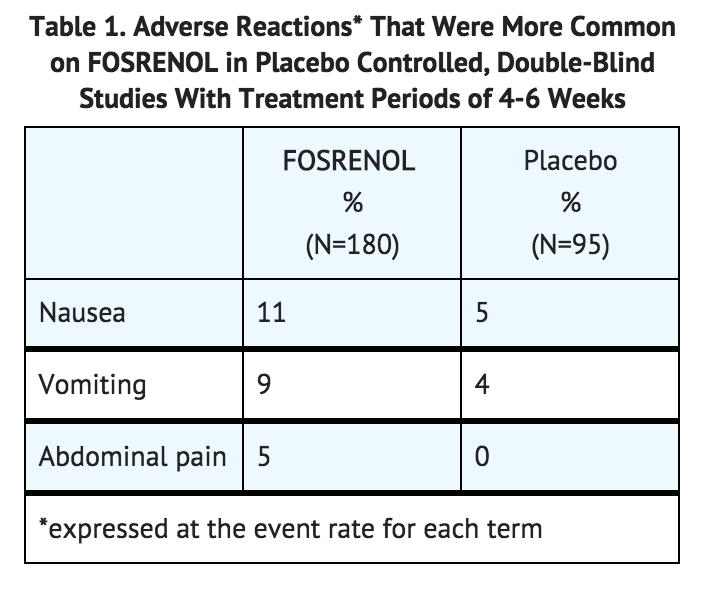
- In double-blind, placebo-controlled studies where a total of 180 and 95 ESRD patients were randomized to lanthanum carbonate and placebo, respectively, for 4-6 weeks of treatment, the most common reactions that were more frequent (>5% difference) in the lanthanum carbonate group were nausea, vomiting, and abdominal pain (Table 1).
- In an open-label long-term 2 year extension study in 93 patients who had transitioned from other studies, resulting in a total of up to 6 years treatment, mean baseline values and changes in transaminases were similar to those observed in the earlier comparative studies, with little change during treatment.
- The safety of lanthanum carbonate was studied in two long-term, open-labeled clinical trials, which included 1215 patients treated with lanthanum carbonate and 944 with alternative therapy. Fourteen percent (14%) of lanthanum carbonate treated patients discontinued treatment due to adverse events. Gastrointestinal adverse reactions, such as nausea, diarrhea and vomiting were the most common types of event leading to discontinuation.
Postmarketing Experience
- The following adverse reactions have been identified during post-approval use of lanthanum carbonate: constipation, dyspepsia, allergic skin reactions, hypophosphatemia, and tooth injury.
Drug Interactions
- Lanthanum has the potential to bind to drugs with anionic (e.g., carboxyl, carbonyl, and hydroxyl) groups. lanthanum carbonate may decrease the bioavailability of tetracyclines or fluoroquinolones via this mechanism.
- There are no empirical data on avoiding drug interactions between lanthanum carbonate and most concomitant drugs. When administering an oral medication where a reduction in the bioavailability of that medication would have a clinically significant effect on its safety or efficacy, administer the drug at least one hour before or three hours after lanthanum carbonate. Monitor blood levels of the concomitant drugs that have a narrow therapeutic range.
Drugs Binding to Antacids
- There is a potential for lanthanum carbonate to interact with compounds which bind to cationic antacids (i.e. aluminium-, magnesium-, or calcium-based). Therefore, do not administer such compounds within 2 hours of dosing with lanthanum carbonate. Examples of relevant classes of compounds where antacids have been demonstrated to reduce bioavailability include antibiotics (such as quinolones, ampicillin and tetracyclines), thyroid hormones, ACE-inhibitors, statin lipid regulators and anti-malarials.
Quinolone Antibiotics
- Co-administration of lanthanum carbonate with quinolone antibiotics may reduce the extent of their absorption. The bioavailability of oral ciprofloxacin was decreased by approximately 50% when taken with lanthanum carbonate in a single dose study in healthy volunteers. Administer oral quinolone antibiotics at least 1 hour before or 4 hours after lanthanum carbonate. When oral quinolones are given for short courses, consider eliminating the doses of lanthanum carbonate that would be normally scheduled near the time of quinolone intake to improve quinolone absorption.
Levothyroxine
- The bioavailability of levothyroxine was decreased by approximately 40% when taken together with lanthanum carbonate. Administer thyroid hormone replacement therapy at least 2 hours before or 2 hours after dosing with lanthanum carbonate and monitor thyroid stimulating hormone (TSH) levels
Use in Specific Populations
Pregnancy
- No adequate and well-controlled studies have been conducted in pregnant women. The effect of lanthanum carbonate on the absorption of vitamins and other nutrients has not been studied in pregnant women. Lanthanum carbonate is not recommended for use during pregnancy.
- Studies in pregnant rabbits showed that oral administration of lanthanum carbonate at 1500 mg/kg/day (5 times the maximum recommended daily human dose (MRHD) of 5725 mg, on a mg/m2 basis, assuming a 60 kg patient) was associated with increased post-implantation loss, reduced fetal weights, and delayed fetal ossification
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Lanthanum carbonate in women who are pregnant.
Labor and Delivery
- No lanthanum carbonate treatment-related effects on labor and delivery were seen in animal studies. The effects of lanthanum carbonate on labor and delivery in humans is unknown.
Nursing Mothers
- It is not known whether lanthanum carbonate is excreted in human milk. As many drugs are excreted in human milk, consider the possibility of infant exposure when lanthanum carbonate is administered to a nursing woman.
Pediatric Use
- The safety and efficacy of lanthanum carbonate in pediatric patients have not been established. While growth abnormalities were not identified in long-term animal studies, lanthanum was deposited into developing bone including growth plate. The consequences of such deposition in developing bone in pediatric patients are unknown. Therefore, the use of lanthanum carbonate in this population is not recommended.
Geriatic Use
- Of the total number of patients in clinical studies of lanthanum carbonate, 32% (538) were ≥65, while 9.3% (159) were ≥75. No overall differences in safety or effectiveness were observed between patients ≥65 years of age and younger patients.
Gender
There is no FDA guidance on the use of Lanthanum carbonate with respect to specific gender populations.
Race
There is no FDA guidance on the use of Lanthanum carbonate with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Lanthanum carbonate in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Lanthanum carbonate in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Lanthanum carbonate in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Lanthanum carbonate in patients who are immunocompromised.
Administration and Monitoring
Administration
- Oral.
Monitoring
There is limited information regarding Lanthanum carbonate Monitoring in the drug label.
IV Compatibility
- There is limited information regarding IV Compatibility of Lanthanum.
Overdosage
- The symptoms associated with overdose are adverse reactions such as headache, nausea and vomiting. In clinical trials, daily doses up to 6000 mg/day of lanthanum carbonate were well tolerated in healthy adults when administered with food, with the exception of GI symptoms. Given the topical activity of lanthanum in the gut, and the excretion in feces of the majority of the dose, supportive therapy is recommended for overdosage. Lanthanum carbonate was not acutely toxic in animals by the oral route. No deaths and no adverse effects occurred in mice, rats or dogs after single oral doses of 2000 mg/kg (1.7, 3.4, and 11.3 times the MRHD, respectively, on a mg/m2 basis).
Pharmacology
| Template:Chembox header2 | Lanthanum carbonate | |
|---|---|
| Identifiers | |
3D model (JSmol)
|
|
| ChEMBL | |
| ChemSpider | |
| ECHA InfoCard | Lua error in Module:Wikidata at line 879: attempt to index field 'wikibase' (a nil value). Lua error in Module:Wikidata at line 879: attempt to index field 'wikibase' (a nil value). |
PubChem CID
|
|
| |
| |
| Properties | |
| La2(CO3)3 | |
| Molar mass | 457.838 g/mol |
| Related compounds | |
| Template:Chembox header2 | Except where noted otherwise, data are given for materials in their standard state (at 25 °C, 100 kPa) Infobox disclaimer and references | |
Mechanism of Action
Lanthanum carbonate is a phosphate binder that reduces absorption of phosphate by forming insoluble lanthanum phosphate complexes that pass through the gastrointestinal (GI) tract unabsorbed. Both serum phosphate and calcium phosphate product are reduced as a consequence of the reduced dietary phosphate absorption.
Structure
There is limited information regarding Lanthanum carbonate Structure in the drug label.
Pharmacodynamics
- In vitro studies have shown that lanthanum effectively binds phosphate in the physiologically relevant pH range of 3 to 7. In simulated gastric fluid, lanthanum binds approximately 97% of the available phosphate at pH 3-5 and 67% at pH 7, when lanthanum is present in a two-fold molar excess to phosphate. Bile acids have not been shown to affect the phosphate binding affinity of lanthanum. In order to bind dietary phosphate efficiently, lanthanum carbonate must be administered with or immediately after food.
- In five Phase I pharmacodynamic studies comparing the reduction from baseline of urinary phosphorus excretion in healthy volunteers (N=143 taking lanthanum carbonate), it was shown that the mean intestinal phosphate binding capacity of lanthanum ranged from 235 to 468 mg phosphorus/day when lanthanum was administered at a dose of 3 g per day with food. By comparison, in one study with an untreated control group (n=10) and another study with a placebo group (n=3), the corresponding mean changes from baseline were 3 mg phosphorus/day and 87 mg phosphorus/day, respectively.
Pharmacokinetics
- Absorption and Distribution - Following single or multiple dose oral administration of lanthanum carbonate to healthy subjects, the concentration of lanthanum in plasma was very low (bioavailability <0.002%). Following oral administration in patients, the mean lanthanum Cmax was 1.0 ng/mL. During long-term administration (52 weeks) in ESRD patients, the mean lanthanum concentration in plasma was approximately 0.6 ng/mL. There was minimal increase in plasma lanthanum concentrations with increasing doses within the therapeutic dose range. The timing of food intake relative to lanthanum administration (during and 30 minutes after food intake) has a negligible effect on the systemic level of lanthanum.
- In vitro, lanthanum is highly bound (>99%) to human plasma proteins, including human serum albumin, α1-acid glycoprotein, and transferrin. Binding to erythrocytes in vivo is negligible in rats.
- In animal studies, lanthanum concentrations in several tissues, particularly gastrointestinal tract, mesenteric lymph nodes, bone and liver, increased over time to levels several orders of magnitude higher than those in plasma. The level of lanthanum in the liver was higher in renally impaired rats due to higher intestinal absorption. Lanthanum was found in the lysosomes and the biliary canal consistent with transcellular transport. Steady state tissue concentrations in bone and liver were achieved in dogs between 4 and 26 weeks. Relatively high levels of lanthanum remained in these tissues for longer than 6 months after cessation of dosing in dogs. There is no evidence from animal studies that lanthanum crosses the blood-brain barrier.
- In 105 bone biopsies from patients treated with lanthanum carbonate for up to 4.5 years, rising levels of lanthanum were noted over time. Estimates of elimination half-life from bone ranged from 2.0 to 3.6 years. Steady state bone concentrations were not reached during the period studied.
- Metabolism and Elimination - Lanthanum is not metabolized. Lanthanum was cleared from plasma of patients undergoing dialysis with an elimination half-life of 53 hours following discontinuation of therapy.
- No information is available regarding the mass balance of lanthanum in humans after oral administration. In rats and dogs, the mean recovery of lanthanum after an oral dose was about 99% and 94% respectively and was essentially all from feces. Biliary excretion is the predominant route of elimination for circulating lanthanum in rats. In healthy volunteers administered intravenous lanthanum as the soluble chloride salt (120 μg), renal clearance was less than 2% of total plasma clearance. Quantifiable amounts of lanthanum were not measured in the dialysate of treated ESRD patients.
Drug Interactions
- Lanthanum carbonate has a low potential for systemic drug-drug interactions because of the very low bioavailability of lanthanum and because it is not a substrate or inhibitor of major cytochrome P450 enzyme groups involved in drug metabolism (CYP1A2, CYP2C9/10, CYP2C19, CYP2D6 and CYP3A4/5).
- Lanthanum carbonate does not alter gastric pH. Therefore, Lanthanum carbonate drug interactions based on altered gastric pH are not expected.
- In an in vitro investigation, lanthanum did not form insoluble complexes when mixed in simulated gastric fluid with warfarin, digoxin, furosemide, phenytoin, metoprolol and enalapril. Clinical studies have shown that Lanthanum carbonate (three doses of 1000 mg on the day prior to exposure and one dose of 1000 mg on the day of co-administration) administered 30 minutes earlier did not alter the pharmacokinetics of oral warfarin (10 mg), digoxin (0.5 mg), or metoprolol (100 mg). Potential pharmacodynamic interactions between lanthanum and these drugs (e.g., bleeding time or prothrombin time) were not evaluated. None of the drug interaction studies were done with the maximum recommended therapeutic dose of lanthanum carbonate. No drug interaction studies assessed the effects of drugs on phosphate binding by lanthanum carbonate.
Ciprofloxacin
- In a randomized, two-way crossover study in healthy volunteers examining the interaction potential of a single oral dose of ciprofloxacin (750 mg) alone and with lanthanum carbonate (1 g TID), the maximum plasma concentration of ciprofloxacin was reduced by 56% and the area under the ciprofloxacin plasma concentration-time curve was reduced by 54%. The 24-h urinary recovery of ciprofloxacin was reduced 52% by Lanthanum carbonate.
Levothyroxine
- In a single-dose crossover study of levothyroxine (1 mg) with or without simultaneous administration of a single dose of anthanum carbonate (500 mg) in six euthyroid normal healthy volunteers, the area under the serum T4 concentration-time curve was decreased by 40%.
Fat Soluble Vitamins
- Lanthanum carbonate appears not to affect the availability of fat soluble vitamins (A, D, E and K) or other nutrient.
Citrate
- Citrate did not increase the absorption of lanthanum.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- Oral administration of lanthanum carbonate to rats for up to 104 weeks, at doses up to 1500 mg of the salt per kg/day [2.5 times the MRHD of 5725 mg, on a mg/m2 basis, assuming a 60-kg patient] revealed no evidence of carcinogenic potential. In the mouse, oral administration of lanthanum carbonate for up to 99 weeks, at a dose of 1500 mg/kg/day (1.3 times the MRHD) was associated with an increased incidence of glandular stomach adenomas in male mice.
- Lanthanum carbonate tested negative for mutagenic activity in an in vitro Ames assay using Salmonella typhimurium and Escherichia coli strains and in vitro HGPRT gene mutation and chromosomal aberration assays in Chinese hamster ovary cells. Lanthanum carbonate also tested negative in an oral mouse micronucleus assay at doses up to 2000 mg/kg (1.7 times the MRHD), and in micronucleus and unscheduled DNA synthesis assays in rats given IV lanthanum chloride at doses up to 0.1 mg/kg, a dose that produced plasma lanthanum concentrations >2000 times the peak human plasma concentration.
- Lanthanum carbonate, at doses up to 2000 mg/kg/day (3.4 times the MRHD), did not affect fertility or mating performance of male or female rats.
Animal Toxicology and/or Pharmacology
Developmental Toxicity
- In pregnant rats, oral administration of lanthanum carbonate at doses as high as 2000 mg/kg/day (3.4 times the MRHD) resulted in no evidence of harm to the fetus. In pregnant rabbits, oral administration of lanthanum carbonate at 1500 mg/kg/day (5 times the MRHD) was associated with a reduction in maternal body weight gain and food consumption, increased post-implantation loss, reduced fetal weights, and delayed fetal ossification. Lanthanum carbonate administered to rats from implantation through lactation at 2000 mg/kg/day (3.4 times the MRHD) caused delayed eye opening, reduction in body weight gain, and delayed sexual development (preputial separation and vaginal opening) of the offspring.
Clinical Studies
- The effectiveness of lanthanum carbonate in reducing serum phosphorus in ESRD patients was demonstrated in one short-term, placebo-controlled, double-blind dose-ranging study, two placebo-controlled randomized withdrawal studies and two long-term, active-controlled, open-label studies in both hemodialysis and peritoneal dialysis (PD) patients.
Double-Blind Placebo-Controlled Studies
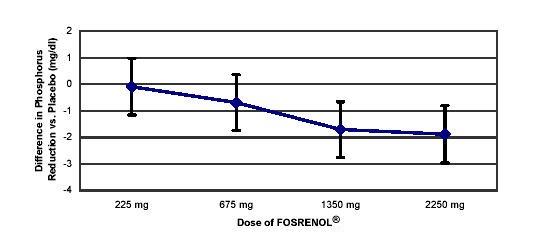
- One hundred and forty-four patients with chronic renal failure undergoing hemodialysis and with elevated phosphate levels were randomized to double-blind treatment at a fixed dose of lanthanum carbonate of 225 mg (n=27), 675 mg (n=29), 1350 mg (n=30) or 2250 mg (n=26) or placebo (n=32) in divided doses with meals. Fifty-five percent of subjects were male, 71% black, 25% white and 4% of other races. The mean age was 56 years and the duration of dialysis ranged from 0.5 to 15.3 years. Steady-state effects were achieved after two weeks. The effect after six weeks of treatment is shown in Figure 1.
- Figure 1. Difference in Phosphate Reduction in the lanthanum carbonate and Placebo Group in a 6-Week, Dose-Ranging, Double-Blind Study in ESRD Patients (with 95% Confidence Intervals)
Open-Label Active-Controlled Studies
- Two long-term open-label studies were conducted, involving a total of 2028 patients with ESRD undergoing hemodialysis. Patients were randomized to receive lanthanum carbonate or alternative phosphate binders for up to six months in one study and two years in the other. The daily lanthanum carbonate doses, divided and taken with meals, ranged from 375 mg to 3000 mg. Doses were titrated to reduce serum phosphate levels to a target level. The daily doses of the alternative therapy were based on current prescribing information or those commonly utilized. Both treatment groups had similar reductions in serum phosphate of about 1.8 mg/dL. Maintenance of reduction was observed for up to three years in patients treated with lanthanum carbonate in long-term, open-label extensions.
- No effects of lanthanum carbonate on serum levels of 25-dihydroxy vitamin D3, vitamin A, vitamin B12, vitamin E and vitamin K were observed in patients who were monitored for 6 months.
- Paired bone biopsies (at baseline and at one or two years) in 69 patients randomized to either lanthanum carbonate or calcium carbonate in one study and 99 patients randomized to either lanthanum carbonate or alternative therapy in a second study showed no differences in the development of mineralization defects between the groups.
- Vital status was known for over 2000 patients, 97% of those participating in the clinical program during and after receiving treatment. The adjusted yearly mortality rate (rate/years of observation) for patients treated with lanthanum carbonate or alternative therapy was 6.6%.
How Supplied
- Lanthanum carbonate is supplied as a chewable tablet in three dosage strengths for oral administration: 500 mg tablets, 750 mg tablets, and 1000 mg tablets. Each chewable tablet is white to off-white round, flat with a bevelled edge, and embossed on one side with 'S405' and the dosage strength corresponding to the content of elemental lanthanum.
- 500 mg Patient Pack (2 bottles of 45 tablets, NDC 54092-252-45, per each patient pack) NDC 54092-252-90.
- 750 mg Patient Pack (6 bottles of 15 tablets, NDC 54092-253-15, per each patient pack) NDC 54092-253-90.
- 1000 mg Patient Pack (9 bottles of 10 tablets, NDC 54092-254-10, per each patient pack) NDC 54092-254-90.
Storage
- Storage - Store at 25°C (77°F): excursions permitted to 15-30°C (59-86°F).
- Protect from moisture.
Images
Drug Images
{{#ask: Page Name::Lanthanum carbonate |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel



{{#ask: Label Page::Lanthanum carbonate |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
- Advise patients to take FOSRENOL tablets with or immediately after food and to chew or to crush tablets completely before swallowing.
- Advise patients who are taking an oral medication where a reduction in the bioavailability of that medication would have a clinically significant effect on its safety or efficacy to separate the dosing of FOSRENOL from the affected drug by several hours.
- Notify your physician that you are taking FOSRENOL prior to an abdominal x-ray.
Precautions with Alcohol
Alcohol-Lanthanum interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- FOSRENOL ®[1]
Look-Alike Drug Names
- There is limited information regarding Look-Alike Drug Names.
Price
References
The contents of this FDA label are provided by the National Library of Medicine.